Track Body Weight & Composition Beyond the Scale
Move beyond body weight tracking to understand fat, muscle, and health. Compare DEXA and BIA methods, and learn when tracking serves your goals.
Written by Dr. Rishav Das, M.B.B.S., Wellness Device Data Analyst
See About page for credentials
Medically reviewed according to the standards outlined on our About page
Introduction
Are You Tracking the Wrong Number?
You’re eating right and exercising consistently, but the scale isn’t moving—or worse, it’s going up. Before you get discouraged, consider this: your weight might be stable while you’re losing fat and gaining muscle. The scale doesn’t tell you this story.
Body composition—the proportion of fat, muscle, bone, and water in your body—reveals what the scale can’t. Two people at the same weight can look completely different and have vastly different health risks depending on their muscle, fat, and bone composition. Understanding these differences helps you:
- See real progress when the scale stays the same
- Know whether your training program is working
- Make informed decisions about your health
- Stop second-guessing your fitness routine
Whether you’re a 30-something professional tracking fitness progress, a 50+ adult monitoring age-related muscle loss, or an athlete optimizing performance, this guide helps you understand body composition tracking—what works, what doesn’t, and whether you actually need it.
Educational Purpose: This content is designed to help you understand body composition metrics and make informed decisions about whether and how to track them. It is not a substitute for professional medical or nutritional guidance.
When to Consult a Healthcare Provider:
- When body composition changes occur unexpectedly
- Before starting any significant body composition change program
- If you have a history of disordered eating
- When tracking causes anxiety, obsession, or negative self-perception
- For interpretation of body composition results in medical context
Quick Comparison: Body Composition Measurement Methods
| Method | Accuracy | Cost | Time | Best For |
|---|---|---|---|---|
| DEXA Scan | ±1–3% body fat | $50–150 per scan | 10–20 min | Clinical needs, baseline measurement, athletes needing precision |
| BIA Smart Scale (Multi-frequency) | ±5–8% body fat | $100–150 one-time | 30 seconds | Home tracking trends, resistance training progress |
| BIA Smart Scale (Basic) | ±5–8% body fat | $30–80 one-time | 30 seconds | Budget-friendly trend tracking |
| Skinfold Calipers | ±3–5% (trained user) | $5–30 one-time | 5–10 min | DIY tracking, portable measurements |
| Measuring Tape | ±4–6% (equations) | $2 one-time | 2 minutes | Free visceral fat monitoring, simple tracking |
| Bod Pod | ±2–4% body fat | $50–100 per test | 10 minutes | Alternative to DEXA, research purposes |
Key Insight: You don’t need perfect accuracy—you need consistent measurements that show whether you’re moving in the right direction. Think of it like a home thermometer: not lab-precise, but good enough to know if you have a fever.
- Track Body Weight & Composition Beyond the Scale
- Introduction
- Quick Comparison: Body Composition Measurement Methods
- What You'll Gain from Understanding Body Composition
- Understanding Body Composition
- Body Composition Measurement Methods
- Overview of Measurement Technologies
- DEXA Scans for Body Composition: Accuracy, Cost & Where to Get One
- BIA Smart Scales: How Accurate Are They Really?
- Body Composition Testing Options Compared: Bod Pod, Skinfold Calipers, and More
- How to Choose the Best Body Composition Measurement Method for Your Goals
- Our Top Recommendations by Use Case
- What Do Smart Scales Actually Measure? Understanding Body Composition Metrics
- When Body Composition Tracking Is Helpful
- Using Body Composition Tracking in a Healthy Way
- How to Choose the Best Body Composition Scale or Device
- Key Metrics That Don't Require Special Devices
- Summary and Recommendations
- References
- About the Medical Reviewer:
What You’ll Gain from Understanding Body Composition
See Real Progress the Scale Can’t Show:
Discover you’re building muscle even when weight stays the same. Celebrate wins that traditional metrics would hide.
Train Smarter, Not Harder:
Stop guessing whether your program is working. Know within weeks whether you’re gaining muscle, losing fat, or maintaining effectively.
Save Time and Frustration:
Identify what’s working in weeks, not months. Avoid wasting effort on approaches that aren’t delivering results.
Make Informed Decisions:
Choose nutrition and training strategies based on data, not guesswork. Understand how your body responds to different approaches.
Peace of Mind:
Know exactly what’s happening in your body. Replace anxiety about the scale with confidence in your progress.
This guide helps you understand:
- When body composition tracking helps vs. when it’s unnecessary
- Which measurement methods actually work (and which are marketing hype)
- Whether you need expensive devices or free methods are sufficient
- How to track effectively without developing unhealthy patterns
Understanding Body Composition
Components of Body Composition
Body composition is typically divided into two or more compartments depending on the analysis model used:
| Component | Description | Typical % of Body Weight | Health Significance |
| Body Fat (Adipose Tissue) | Energy storage, hormone production, insulation | 10–35% (varies by sex/age) | Essential for hormone function; excess associated with metabolic disease |
| Skeletal Muscle Mass | Voluntary muscle tissue | 30–40% | Metabolic activity, strength, mobility; declines with age (sarcopenia) |
| Bone Mineral Content | Skeletal system density | 3–5% | Structural support; low density increases fracture risk |
| Body Water | Intracellular and extracellular fluid | 50–60% | Hydration status; affected by sodium, hormones, inflammation |
| Organs & Other Tissues | Non-muscle lean tissue | ~10–15% | Essential physiological functions |
Key Research Support:
Age-related changes in body composition well-documented (Kyle et al., 2001, European Journal of Clinical Nutrition)
Body composition models validated through four-compartment reference methods (Wang et al., 1992, American Journal of Clinical Nutrition)
Why Weight Alone Is Misleading
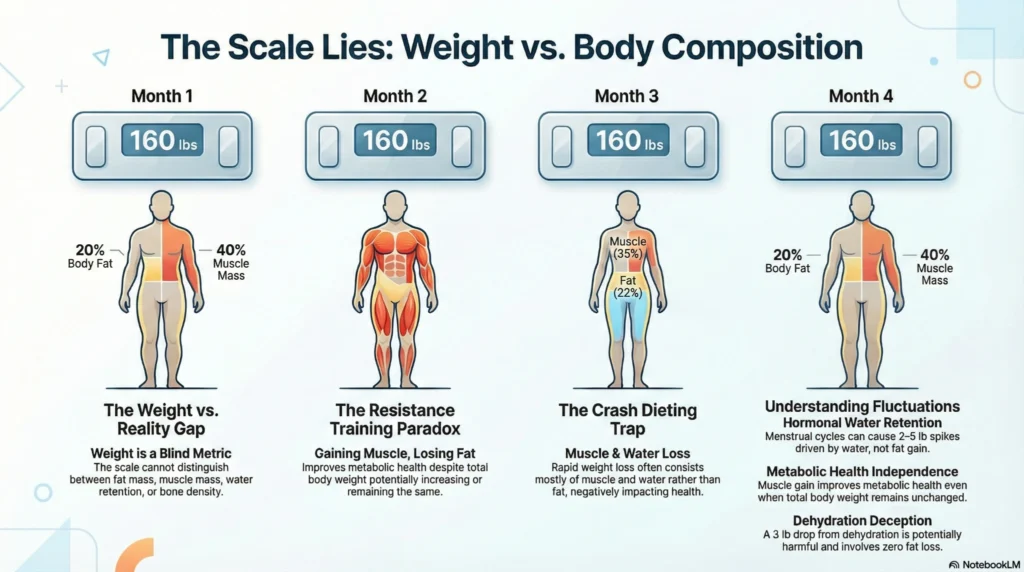
Weight does not distinguish between fat mass, muscle mass, water retention, or bone density. Body composition analysis addresses these limitations:
| Scenario | Weight Change | Body Composition Reality | Health Implication |
| Starting resistance training | +3 lbs | +5 lbs muscle, -2 lbs fat | Improved metabolic health despite weight gain |
| Crash dieting | -15 lbs | -5 lbs fat, -8 lbs muscle, -2 lbs water | Loss of metabolically active tissue |
| Menstrual cycle (female) | +2–5 lbs | Water retention, no fat change | Temporary, hormonally driven |
| Dehydration | -3 lbs | Water loss only | No fat loss; potentially harmful |
Evidence: Resistance training increases lean mass while reducing fat mass, improving metabolic health independent of weight changes (Westcott, 2012, Current Sports Medicine Reports).
Body Composition Across Age and Sex
Body composition varies significantly by biological sex and changes predictably with aging:
By Sex (Adults 20–40 years):
| Metric | Males | Females | Biological Reason |
| Essential body fat | 2–5% | 10–13% | Reproductive function, hormone production |
| Typical body fat range | 8–24% | 21–35% | Sex hormone influence on fat distribution |
| Skeletal muscle mass | 38–42% of body weight | 30–36% of body weight | Testosterone effects on muscle development |
By Age (General Population):
| Age Range | Body Fat Trend | Muscle Mass Trend | Clinical Concern |
| 18–30 | Baseline established | Peak muscle mass | Reference for later comparison |
| 30–50 | Gradual increase (0.5–1% per decade) | Begins declining (~1% per year) | Sarcopenia onset without intervention |
| 50–70 | Accelerated increase | Accelerated decline (1–2% per year) | Metabolic syndrome risk, mobility loss |
| 70+ | May stabilize or decrease | Significant loss (sarcopenia) | Falls risk, frailty, mortality predictor |
Research Basis:
Sex differences in body composition persist across lifespan (Wells, 2007, International Journal of Obesity)
Age-related sarcopenia: 3–8% muscle mass loss per decade after age 30 (Volpi et al., 2004, Journal of Gerontology)
Healthy Body Fat Ranges
Body fat percentage ranges are defined by health outcomes, not aesthetic preferences. These ranges are associated with optimal metabolic and cardiovascular function:
American Council on Exercise Body Fat Categories:
| Category | Males | Females | Notes |
| Essential Fat | 2–5% | 10–13% | Minimum for physiological function; below this is dangerous |
| Athletes | 6–13% | 14–20% | Sport-dependent; may not be sustainable year-round |
| Fitness | 14–17% | 21–24% | Associated with good health and appearance |
| Average | 18–24% | 25–31% | Typical for general population; health neutral |
| Obese | 25%+ | 32%+ | Associated with increased cardiometabolic risk |
Important Qualifications:
- Health risks emerge at both extremes (too low or too high)
- These are statistical associations, not prescriptive targets
- Individual health status matters more than a specific percentage
- Athletes often function optimally at lower ranges temporarily
Health Risks at Body Fat Extremes
Risks of Body Fat Below Essential Range:
| System | Potential Consequence | Population at Risk |
| Reproductive | Menstrual irregularities, amenorrhea (females); reduced testosterone (males) | Female athletes, restrictive dieters |
| Immune | Increased infection susceptibility, impaired healing | Chronic dieters, eating disorder patients |
| Metabolic | Reduced metabolic rate, cold intolerance | Extreme low-calorie dieters |
| Bone Health | Accelerated bone loss, stress fractures | Athletes with Female Athlete Triad |
| Psychological | Body dysmorphia, obsessive behaviors | Eating disorder patients |
Clinical Evidence: Body fat below 12% in females and below 5% in males may impair hormone production and immune function (Gallagher et al., 1998, American Journal of Clinical Nutrition).
Risks of Elevated Body Fat:
| Condition | Associated Body Fat Range | Evidence Level |
| Insulin resistance | Males >25%, Females >32% | Strong (multiple large cohorts) |
| Metabolic syndrome | Males >25%, Females >32% | Strong (prospective studies) |
| Cardiovascular disease | Elevated visceral fat specifically | Strong (meta-analyses) |
| Sleep apnea | BMI >30, body fat >30% | Moderate (observational) |
| Osteoarthritis | Weight-bearing joints affected | Moderate (large studies) |
Important Context: Body fat percentage alone does not diagnose disease. Clinical evaluation considers multiple factors including visceral fat distribution, metabolic markers (glucose, lipids, blood pressure), and family history.
Evidence: Visceral fat accumulation, even at “normal” body fat percentages, increases metabolic disease risk (Goossens, 2017, Diabetologia). This is why body composition analysis provides more information than weight or body fat percentage alone.
Normal Weight Obesity Phenomenon
Some individuals have body weight within “normal” BMI range (18.5–24.9) but elevated body fat percentage and metabolic dysfunction. This is termed “normal weight obesity” or “metabolically obese, normal weight.”
Characteristics:
- BMI 18.5–24.9 (normal range)
- Body fat percentage >30% (females) or >20% (males)
- Elevated visceral adiposity
- Metabolic dysfunction (insulin resistance, dyslipidemia)
Clinical Significance: Individuals with normal weight obesity may have similar or greater metabolic risk than those classified as overweight by BMI alone (Oliveros et al., 2014, Progress in Cardiovascular Diseases).
Why This Matters: Weight-based screening misses this population. Body composition assessment can identify metabolic risk in individuals who would otherwise be considered healthy based on weight alone.
Body Composition Measurement Methods

Overview of Measurement Technologies
Different body composition methods vary in accuracy, accessibility, and cost. Understanding these differences helps determine which method, if any, is appropriate for your needs.
| Method | Typical Error Range | Cost | Accessibility | Best Use Case |
| DEXA Scan | ±1–3% body fat | $50–150 per scan | Medical facilities, research centers | Clinical assessment, research standard |
| Hydrostatic Weighing | ±2–3% body fat | $40–75 per test | Research labs, university facilities | Athletic assessment, validation studies |
| Bod Pod (ADP) | ±2–4% body fat | $50–100 per test | Research centers, some gyms | Athletic testing, periodic assessment |
| Clinical BIA | ±3–5% body fat | $75–200 per test | Medical offices, specialized clinics | Medical monitoring, clinical populations |
| Consumer BIA Scales | ±5–8% body fat | $30–200 (one-time purchase) | Home use | Trend tracking (not absolute accuracy) |
| Skinfold Calipers | ±3–5% body fat (when properly done) | $5–30 (one-time purchase) | Home use with training | Low-cost tracking; technique-dependent |
Important Context: Error ranges represent measurement precision, not accuracy. A device can be precise (consistent) without being accurate (correct). Consumer devices often show consistent but biased readings.
DEXA Scans for Body Composition: Accuracy, Cost & Where to Get One
DEXA uses two X-ray energies to differentiate bone, fat, and lean tissue. It is the reference standard for body composition research.
How It Works:
- Two X-ray beams pass through the body
- Different tissues absorb X-rays differently
- Software calculates fat mass, lean mass, and bone mineral density
- Regional analysis available (trunk, limbs, visceral fat estimation)
Accuracy Characteristics:
- Typical precision: ±1–3% body fat across repeated scans
- Regional variation: Trunk fat less precise than total body fat
- Highly sensitive to hydration status (water counted as lean mass)
- Bone density measurement ±1–2%
Research Support: DEXA shows high agreement with four-compartment models (Wang et al., 1992, American Journal of Clinical Nutrition) and is widely used as the reference standard in body composition research.
Clinical Applications:
- Sarcopenia diagnosis in older adults
- Bone density assessment (osteoporosis screening)
- Body composition changes in clinical populations
- Athletic performance optimization
Practical Considerations:
- Cost: $50–150 per scan (varies by facility and insurance)
- Radiation exposure: Minimal (0.001–0.01 mSv, equivalent to 1–10 hours of natural background radiation)
- Time: 10–20 minutes per scan
- Requires lying still on scanning table
- Results affected by recent food/fluid intake, exercise, menstrual cycle
When DEXA Is Appropriate:
- Clinical need for accurate body composition (sarcopenia screening, bone health assessment)
- Baseline measurement before significant body composition change program
- Validation of other measurement methods
- Research purposes
When DEXA Is Unnecessary:
- General fitness tracking (consumer methods sufficient for trends)
- Frequent monitoring (cost prohibitive, unnecessary radiation exposure)
- Weight loss motivation (simpler methods adequate)
BIA Smart Scales: How Accurate Are They Really?
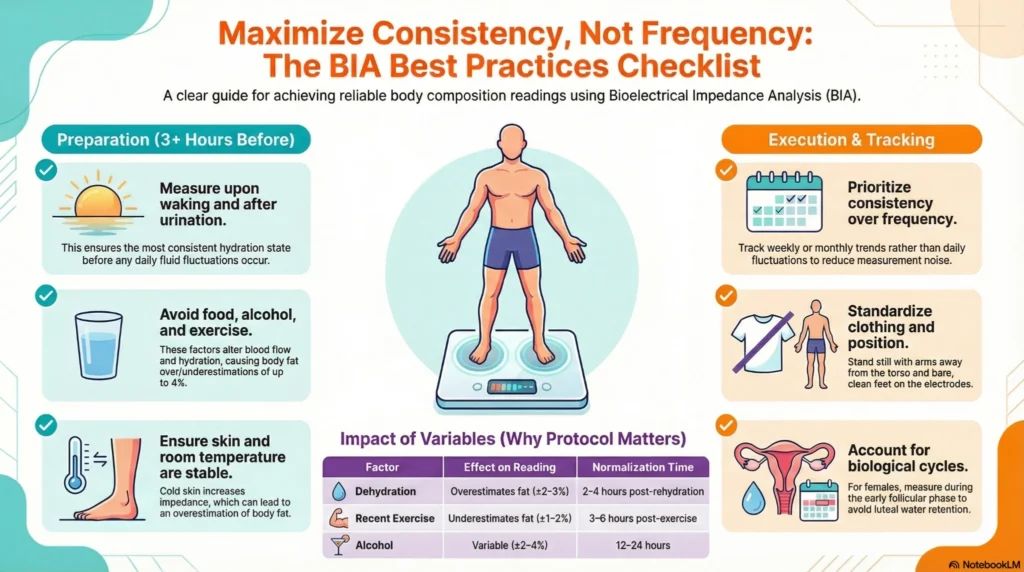
BIA measures body composition by passing a weak electrical current through the body. Fat tissue resists electrical flow; lean tissue conducts it. The device calculates body composition from this resistance.
How It Works:
- Electrodes placed on body (feet, hands, or both)
- Weak alternating current (50 kHz typical for consumer devices) applied
- Device measures electrical impedance (resistance and reactance)
- Algorithm estimates body composition based on impedance values, plus user inputs (age, sex, height, weight)
Clinical vs. Consumer BIA:
| Feature | Clinical BIA | Consumer BIA |
| Frequencies | Multiple (5–500 kHz) | Single (50 kHz typical) |
| Electrode placement | 4–8 point (hands and feet) | 2–4 point (feet only or feet and hands) |
| Validation | Clinical studies published | Often minimal validation |
| Typical accuracy | ±3–5% body fat | ±5–8% body fat |
| Additional metrics | Intracellular/extracellular water, phase angle | Often includes unvalidated metrics |
Factors Affecting BIA Accuracy:
- Hydration status (dehydration overestimates body fat, overhydration underestimates)
- Recent food intake (affects hydration and blood flow)
- Exercise timing (alters fluid distribution and skin temperature)
- Menstrual cycle phase (hormonal fluid retention affects readings)
- Skin temperature (cold skin increases impedance)
- Device calibration and algorithm quality
Research Evidence:
- Multi-frequency BIA shows moderate correlation with DEXA (r = 0.7–0.9) in validation studies (Marra et al., 2019, Nutrition)
- Consumer single-frequency BIA shows weaker correlation (r = 0.5–0.7) and systematic bias (Nickerson et al., 2020, International Journal of Exercise Science)
- BIA is more useful for tracking changes over time than estimating absolute body fat percentage
When BIA Is Appropriate:
- Trend tracking over weeks/months (not day-to-day changes)
- General fitness monitoring
- Supplement to other health metrics (weight, waist circumference, how you feel)
- Cost-effective repeated measurements
When BIA Is Problematic:
- Conditions affecting hydration (kidney disease, heart failure, pregnancy)
- Day-to-day monitoring (too affected by fluid shifts)
- Clinical decision-making (accuracy insufficient for diagnosis)
- Individuals with implanted medical devices (pacemakers, ICDs)
Best Practices for Consumer BIA:
- Compare measurements under similar conditions only
- Measure at same time of day (morning upon waking recommended)
- Avoid measurements after exercise, large meals, dehydration, or alcohol consumption
- Track trends, not absolute numbers
- Use same device consistently
💡 Common Concern: “But aren’t home scales inaccurate?”
Yes, they have ±5–8% error—but that’s fine for tracking trends. You don’t need perfect accuracy; you need consistent measurements that show whether you’re moving in the right direction. Think of it like a home thermometer: not lab-precise, but good enough to know if you have a fever.
Example: If your scale reads 22% body fat but you’re actually 25%, it doesn’t matter for progress tracking. What matters is that next month it reads 20% (showing you lost ~2% body fat), even if your true measurement is 23%. The trend is accurate even when the absolute number isn’t.
Body Composition Testing Options Compared: Bod Pod, Skinfold Calipers, and More
Hydrostatic (Underwater) Weighing:
How it works: Participants submerge in water tank; body density calculated from underwater weight. Body fat estimated from density using established equations.
- Accuracy: ±2–3% body fat
- Advantages: Well-validated reference method, minimal assumptions about body water
- Limitations: Requires specialized equipment, uncomfortable for some, technique-dependent (requires exhaling fully underwater)
- Accessibility: Research labs, some university facilities
Bod Pod (Air Displacement Plethysmography):
How it works: Measures body volume by air displacement in sealed chamber. Body density and composition calculated.
- Accuracy: ±2–4% body fat
- Advantages: Similar principle to hydrostatic weighing without water immersion, relatively quick
- Limitations: Expensive equipment, clothing/body hair affects readings, less validated than DEXA or hydrostatic weighing
- Accessibility: Research centers, some specialized fitness facilities
Skinfold Calipers:
How it works: Pinches skin and subcutaneous fat at standardized body sites. Thickness measured with calipers. Body density estimated from skinfold sum using equations (e.g., Jackson-Pollock 3-site or 7-site).
- Accuracy: ±3–5% body fat when performed by trained technician; ±5–10% with self-measurement
- Advantages: Inexpensive, portable, no equipment needed beyond calipers
- Limitations: Highly technique-dependent, requires training, difficult to measure yourself accurately, assumes subcutaneous fat represents total body fat proportionally (not true for all individuals)
- Accessibility: Calipers available for $5–30; training required for accuracy
3D Body Scanners:
How it works: Infrared depth sensors or structured light creates 3D body model. Body volume and regional measurements calculated. Body composition estimated from body shape using algorithms.
- Accuracy: Body volume precise (±1–2%), but body fat estimates ±4–6% (algorithm-dependent)
- Advantages: Quick, non-invasive, provides body measurements (circumferences, volumes)
- Limitations: Body fat estimation relies on assumptions about body shape-composition relationships; less validated than DEXA or BIA
- Accessibility: Some gyms, research centers; emerging consumer devices
Circumference Measurements + Equations:
How it works: Measures circumferences (waist, hip, neck, limbs) using measuring tape. Body fat estimated using regression equations (e.g., U.S. Navy or YMCA equations).
- Accessibility: Home use with $2 measuring tape
- Accuracy: ±4–6% body fat (equation-dependent)
- Advantages: No equipment beyond measuring tape, free, measures visceral adiposity proxy (waist circumference)
- Limitations: Estimates rely on population-averaged equations, does not measure muscle mass directly
How to Choose the Best Body Composition Measurement Method for Your Goals
Selection depends on goals, access, and budget:
| Goal | Recommended Method | Rationale |
| Clinical diagnosis or medical monitoring | DEXA, clinical BIA | Accuracy necessary for medical decisions |
| Athletic performance optimization | DEXA (baseline), then BIA or skinfolds (tracking) | Baseline accuracy, then consistent tracking |
| General fitness and trend tracking | Consumer BIA scale or waist circumference | Cost-effective, accessible, sufficient for trends |
| No tracking necessary | Scale weight + how clothes fit + how you feel | Simplicity, avoids fixation on metrics |
| History of disordered eating | No tracking; focus on health behaviors and how you feel | Metrics may trigger unhealthy patterns |
Evidence Against Over-Tracking: Frequent body composition monitoring may promote body dissatisfaction and disordered eating patterns in vulnerable individuals (Pacanowski et al., 2015, Obesity). For many people, periodic professional assessment or simple metrics (weight, waist circumference, clothing fit) are sufficient.
Our Top Recommendations by Use Case
Based on accuracy research and practical considerations, here’s guidance for different goals:
Best for Most People: Mid-Range BIA Scale
Who it’s for: Anyone tracking fitness progress, weight loss with muscle preservation, or general health monitoring
What to look for:
- Multi-frequency BIA (more accurate than single-frequency)
- Hand-and-foot electrodes (8-point measurement)
- Price range: $100–150
- App allows data export
- No subscription required for basic features
Why this works: Provides adequate accuracy (±5–8%) for tracking trends at reasonable cost. Perfect for seeing whether resistance training is building muscle or whether fat loss is progressing.
Best for Budget-Conscious: Measuring Tape + Basic Scale
Who it’s for: Those wanting simple health monitoring without device investment
What you need:
- Flexible measuring tape ($2)
- Regular bathroom scale (you likely already own)
- Our free tracking template [download link]
How to use:
- Measure waist circumference monthly
- Track weight weekly
- Note how clothes fit
- Monitor strength/performance improvements
Why this works: Waist circumference predicts cardiometabolic disease as well as expensive devices. Free, validated, and sufficient for most health goals.
Best for Serious Athletes: DEXA + Home Tracking Combo
Who it’s for: Competitive athletes, bodybuilders, those with specific body composition targets
Approach:
- Baseline DEXA scan at training cycle start ($50–150)
- Mid-range BIA scale for weekly trend tracking ($100–150)
- Follow-up DEXA every 3–6 months
Why this works: DEXA provides accurate baseline and progress verification. BIA scale catches trends between DEXA scans without repeated expense.
Best for Clinical Needs: Professional Testing Only
Who it’s for: Sarcopenia screening (50+ adults), eating disorder recovery, chronic disease management
Approach:
- DEXA or clinical BIA as recommended by healthcare provider
- Frequency determined by medical need
- No home device needed
Why this works: Clinical decisions require clinical accuracy. Home devices insufficient for medical diagnosis or monitoring.
Decision Flowchart: Find Your Match
1. What’s your primary goal?
- Track fitness progress → Mid-range BIA scale
- Monitor health simply → Measuring tape + basic scale
- Athletic performance optimization → DEXA + BIA combo
- Clinical monitoring → Professional testing only
2. What’s your budget?
- Under $10 → Measuring tape method
- $30–80 → Basic BIA scale (adequate for trends)
- $100–150 → Multi-frequency BIA scale (better accuracy)
- $150+ per quarter → Periodic DEXA scans
3. How often will you track?
- Quarterly → Professional testing option
- Daily/several times per week → You may benefit from therapy (see “When Tracking Becomes Counterproductive”)
- Weekly → Consumer BIA scale appropriate
- Monthly → Measuring tape sufficient
What Do Smart Scales Actually Measure? Understanding Body Composition Metrics
Consumer body composition devices (smart scales, fitness trackers with body composition features) use bioelectrical impedance analysis (BIA). Understanding what these devices actually measure helps set appropriate expectations.
Core Metrics: What They Mean
Body Fat Percentage:
- Definition: Percentage of total body weight composed of fat mass
- How measured: BIA estimates from electrical impedance and user inputs (age, sex, height, weight)
- Typical consumer device accuracy: ±5–8% body fat
- Useful for: Tracking directional trends (increasing, decreasing, stable) over weeks/months
- Not reliable for: Day-to-day changes, absolute accuracy, clinical diagnosis
Muscle Mass / Lean Body Mass:
- Definition: Weight of muscle tissue (muscle mass) or all non-fat tissue (lean body mass = muscle + bone + organs + water)
- How measured: Total weight minus estimated fat mass
- Important distinction: Most devices report lean body mass, not skeletal muscle specifically
- Typical accuracy: ±3–5 lbs (±1–2 kg)
- Useful for: Tracking muscle gain or loss over time (e.g., during resistance training)
- Limitations: Includes water weight, affected by hydration status
Body Water Percentage:
- Definition: Percentage of total body weight composed of water (intracellular and extracellular)
- How measured: Estimated from BIA impedance values
- Typical range: 50–65% of body weight (varies by age, sex, lean mass)
- Useful for: Athletes monitoring hydration; general awareness
- Limitations: Single-frequency BIA cannot distinguish intracellular vs. extracellular water; affected by recent fluid intake, sodium intake, hormones
Bone Mass:
- Clinical use: DEXA is required for bone health assessment; consumer BIA bone estimates not clinically validated
- Definition: Estimated mineral content of skeleton
- How measured: Calculated from algorithms using lean mass estimate (BIA does not directly measure bone)
- Typical consumer device accuracy: ±0.5–1 lb bone mass estimate
- Important caveat: Consumer BIA estimates bone mass from lean mass, not actual bone measurement
- Not equivalent to: DEXA bone mineral density (BMD) measurement for osteoporosis screening
Metrics with Limited Utility
Many consumer devices report additional metrics with questionable validity:
“Metabolic Age” or “Body Age”:
- Marketing construct, not medically defined metric
- Compares your body composition to population averages for different ages
- Not validated in research; no clinical meaning
- May be motivating for some users but has no health assessment value
“Visceral Fat Level” or “Visceral Fat Rating”:
- Attempts to estimate abdominal fat around organs
- Consumer BIA cannot directly measure visceral fat (requires imaging like CT or MRI)
- Estimates based on total body fat and demographics, not actual measurement
- Waist circumference is a more validated proxy for visceral adiposity (Ross et al., 2020, Nature Reviews Endocrinology)
Basal Metabolic Rate (BMR) or Resting Metabolic Rate (RMR):
- Calculated estimate, not measured value
- Uses equations (e.g., Mifflin-St Jeor) based on age, sex, weight, and estimated lean mass
- Actual BMR varies by genetics, thyroid function, muscle metabolic activity
- Error range: ±10–20% from true BMR
- Indirect calorimetry (clinical test) required for accurate BMR measurement
“Protein Percentage” or “Mineral Percentage”:
- Not directly measured by consumer BIA
- Estimated from lean mass using population averages
- No validation studies supporting these specific metrics
- Not clinically useful
“Segmental Body Composition” (arm, leg, trunk):
- May be useful for tracking asymmetry or regional changes in athletes; less meaningful for general population
- Some devices claim to measure body composition by body region
- Multi-frequency, multi-electrode BIA can provide regional estimates with moderate accuracy
- Consumer devices with fewer electrodes provide less reliable regional estimates
Metrics Actually Useful for Tracking
Focus on these core metrics:
- Scale weight (most accurate measurement on any device)
- Body fat percentage trend (directional changes over weeks/months, not absolute number)
- Lean/muscle mass trend (tracking resistance training progress)
- Waist circumference measured manually (visceral fat proxy, free, well-validated)
Ignore or deprioritize:
- Protein/mineral percentages (not validated)
- Metabolic age, body age (marketing)
- Visceral fat level from BIA (use waist circumference instead)
- BMR calculations (useful as rough estimate only)
- Segmental measurements unless using clinical multi-frequency BIA
- Bone mass from BIA (DEXA needed for clinical bone assessment)
When Body Composition Tracking Is Helpful
Body composition tracking can support health and fitness goals when used appropriately and with realistic expectations.
Beneficial Use Cases
Resistance Training Progress:
- Goal: Verify muscle mass gain, track strength-to-weight ratio
- Appropriate method: Consumer BIA scale for trends, periodic DEXA or clinical BIA for validation
- Tracking frequency: Weekly to bi-weekly
- What to look for: Gradual increase in lean mass estimate (0.5–2 lbs per month for trained individuals is realistic)
- Evidence: Resistance training increases muscle mass measurably over 8–12 weeks (Peterson et al., 2010, Medicine & Science in Sports & Exercise)
Weight Loss with Muscle Preservation:
- Goal: Ensure weight loss comes primarily from fat, not muscle
- Appropriate method: Consumer BIA scale or skinfold measurements
- Tracking frequency: Every 2–4 weeks
- What to look for: Decreasing body fat percentage with stable or slowly declining lean mass (some lean mass loss is normal during caloric deficit)
- Evidence: Caloric restriction combined with resistance exercise better preserves lean mass than diet alone (Heymsfield et al., 2011, Obesity Reviews)
Clinical Monitoring (with Healthcare Provider Guidance):
- Goal: Track body composition changes in medical contexts (cancer cachexia, chronic disease, eating disorder recovery)
- Appropriate method: DEXA or clinical BIA, as recommended by healthcare team
- Tracking frequency: As directed by healthcare provider
- Important: Home tracking not appropriate substitute for clinical monitoring in these populations
Athletic Training Periodization:
- Goal: Optimize body composition for sport performance across training cycles
- Appropriate method: Clinical BIA or DEXA at key training phases (off-season, pre-competition, in-season)
- Tracking frequency: Quarterly or at phase transitions, not daily/weekly
- Evidence: Athletes in weight-class or aesthetic sports benefit from periodic body composition assessment to guide training and nutrition (Nana et al., 2014, European Journal of Clinical Nutrition)
Sarcopenia Risk Assessment (Older Adults):
- Evidence: Early identification of sarcopenia enables intervention with resistance training and nutrition to prevent frailty and falls (Landi et al., 2013, BMJ Open)
- Goal: Identify age-related muscle loss early to guide intervention
- Appropriate method: DEXA with appendicular lean mass calculation; clinical BIA
- Tracking frequency: Annually after age 50, or as recommended by healthcare provider
Real-World Scenarios: What Body Composition Tracking Revealed
Scenario 1: The “Scale Isn’t Moving” Mystery
Sarah, 34, resistance training 4x/week, eating in caloric deficit
What happened: Scale stayed at 165 lbs for 6 weeks despite consistent training and nutrition.
What body composition showed: Lost 8 lbs of fat, gained 5 lbs of muscle, net weight change of -3 lbs (masked by normal weight fluctuations).
Impact: Prevented Sarah from abandoning a program that was actually working extremely well. She continued training with confidence instead of second-guessing her entire approach.
Scenario 2: The “I Don’t Need Expensive Devices” Discovery
James, 42, wanted to monitor health simply
What happened: Considered buying $150 smart scale, decided to try measuring tape method first.
What he learned: Waist circumference decreased from 38″ to 34″ over 6 months. Weight dropped from 210 to 195 lbs. Clothes fit better, energy improved.
Impact: Saved $150 and achieved health goals with $2 measuring tape. Realized he didn’t need technology to track what mattered.
Scenario 3: The “Recomp” Validation
Mike, 28, powerlifter beginning cut phase
What happened: Used home BIA scale weekly + DEXA scan at start and end of 12-week cut.
What he learned: BIA showed stable muscle mass, declining body fat. DEXA confirmed: preserved 94% of lean mass while losing 18 lbs of fat.
Impact: Training and nutrition strategy validated. Knew his approach preserved strength while cutting weight for competition.
Scenario 4: The “I Should Have Stopped Sooner” Warning
Emma, 26, tracking daily, multiple times per day
What happened: Began weighing herself 3–5 times daily, adjusting food and exercise based on fluctuations.
Result: Developed anxiety around measurements, menstrual cycle irregularities, chronic fatigue.
Resolution: Stopped tracking entirely, worked with therapist. Focused on intuitive eating and how body felt. Health improved dramatically.
Lesson: Technology isn’t the problem—relationship with metrics is. Daily fluctuations are normal water shifts, not real body composition changes.
When Body Composition Tracking Adds Value
Tracking is most useful when:
- Tracking enhances motivation without causing anxiety or obsession
- There is a specific, measurable goal (gain muscle, reduce body fat, monitor clinical condition)
- Tracking method is consistent (same device, same conditions, same time of day)
- Trends are evaluated over weeks/months, not day-to-day
- Results are combined with other indicators (performance, how you feel, clinical markers)
Important Context: For most people pursuing general health and fitness, simple metrics like scale weight, waist circumference, exercise performance, and how clothes fit are sufficient indicators of progress. Body composition tracking is optional and not necessary for health.
Using Body Composition Tracking in a Healthy Way
Body composition tracking supports health goals when used appropriately. Here’s how to ensure tracking enhances rather than harms your well-being:
Signs You’re Tracking Well:
- Measurements are one data point among many (performance, energy, how you feel)
- You track trends over weeks/months, not day-to-day changes
- You can skip measurements without anxiety
- Tracking motivates healthy behaviors without obsession
- Your goals are health-focused rather than appearance-focused
- You adjust goals based on how your body responds
If You Notice These Patterns, Adjust Your Approach:
While body composition tracking can support health goals, it can also become problematic. Recognizing when tracking is unhelpful or harmful is critical for psychological and physical health.
Red Flags: Unhealthy Tracking Patterns
Obsessive Measurement:
- Weighing multiple times per day
- Daily body composition measurements with emotional response to normal fluctuations
- Inability to skip measurements without anxiety
- Measurements dictating mood and food choices
Distorted Body Perception:
- Dissatisfaction despite objective health markers improving
- Fixation on achieving body composition targets not aligned with health (e.g., pursuing essential fat levels)
- Comparing measurements to unrealistic standards (professional athletes, fitness models)
- Ignoring clinical advice when it conflicts with body composition goals
Behavioral Red Flags:
- Restricting food or overexercising based on daily measurement fluctuations
- Basing self-worth on body composition metrics
- Social withdrawal or avoidance of activities due to body composition concerns
- Ignoring hunger, fatigue, or other body signals to achieve measurement goals
Physical Warning Signs:
- Cold intolerance (metabolic adaptation to low energy availability)
- Menstrual irregularities or loss of period (females)
- Chronic fatigue despite adequate sleep
- Persistent mood changes (irritability, depression, anxiety)
- Frequent injuries or illness (immune suppression)
Populations for Whom Tracking Is Not Appropriate
Children and Adolescents:
- Body composition tracking may promote body dissatisfaction and disordered eating in developing individuals
- Growth and development priorities outweigh body composition optimization
- Healthcare providers should handle all body composition assessment in this population
- Evidence: Body composition tracking in adolescents associated with increased eating disorder risk (Neumark-Sztainer et al., 2006, International Journal of Eating Disorders)
Individuals with History of Eating Disorders:
- Tracking may trigger relapse or maintain disordered patterns
- Focus on intuitive eating, health behaviors, and psychological recovery more appropriate
- Clinical teams may use body composition assessment when medically necessary, but self-tracking typically contraindicated
- Alternative focus: How body feels, what body can do (strength, endurance, energy), health markers
Pregnant and Postpartum Individuals:
- Body composition changes during pregnancy and postpartum are normal and necessary
- Tracking may promote unrealistic expectations and postpartum body dissatisfaction
- Healthcare providers monitor appropriate weight gain; self-tracking adds no value
- Focus instead: Adequate nutrition for fetal development and breastfeeding, recovery, energy levels
Individuals with Body Dysmorphic Disorder (BDD):
- Clinical treatment (therapy, potentially medication) addresses root cause; self-monitoring counterproductive
- Tracking reinforces obsessive focus on appearance
- Metrics do not address underlying distorted perception
When to Stop Tracking and Seek Support
Consider stopping body composition tracking and consulting a healthcare provider or mental health professional if:
- Tracking causes significant anxiety or distress
- You find yourself thinking about measurements frequently throughout the day
- Measurements influence self-worth or mood substantially
- You restrict food or overexercise in response to measurements
- Physical warning signs appear (fatigue, menstrual changes, frequent injury/illness)
- Friends or family express concern about your tracking or eating behaviors
Resources:
Mental Health America: mhanational.org
National Eating Disorders Association (NEDA): 1-800-931-2237, nationaleatingdisorders.org
National Association of Anorexia Nervosa and Associated Disorders (ANAD): 1-888-375-7767, anad.org
Healthy Relationship with Body Composition Metrics
Signs of Healthy Tracking:
- Measurements are one data point among many (performance, energy, how you feel)
- Day-to-day fluctuations do not cause emotional response
- You can skip measurements without anxiety
- Tracking motivates healthy behaviors without obsession
- Goals are health-focused rather than appearance-focused
- You adjust goals based on how your body responds and how you feel
Evidence-Based Perspective: Body composition is associated with health outcomes at population level, but individual health depends on many factors including cardiovascular fitness, strength, metabolic health markers, mental health, social connections, and sleep quality. Optimizing one metric at the expense of overall well-being is counterproductive.
😰 Common Concern: “Will tracking make me obsessed?”
Healthy tracking means measuring weekly or monthly, not daily. If you measure at consistent intervals (e.g., Monday mornings before breakfast) and evaluate trends over 4–8 weeks, tracking provides useful information without obsession.
Red flag signs to watch for:
- Measuring multiple times per day
- Emotional reactions to normal fluctuations
- Inability to skip measurements without anxiety
- Basing self-worth on numbers
If these patterns emerge, tracking has become counterproductive. See “When to Stop Tracking and Seek Support” section for guidance.
How to Choose the Best Body Composition Scale or Device
If you decide that body composition tracking aligns with your goals and you can engage with metrics in a healthy way, selecting an appropriate device requires critical evaluation.
Evaluating Consumer Body Composition Devices
When assessing devices, look for:
Accuracy and Validation:
- States typical error range (e.g., ±3–5% body fat) rather than claiming “clinical accuracy” or “99% accurate”
- References validation studies comparing device to reference method (DEXA, hydrostatic weighing)
- Transparency about variables affecting accuracy (hydration, device placement, skin temperature)
Measurement Technology:
- Clearly describes measurement method (bioelectrical impedance, if BIA, states frequency used)
- Multi-frequency BIA generally more accurate than single-frequency
- Hand-and-foot electrode placement (8-point) more accurate than foot-only (4-point)
Core vs. Extraneous Metrics:
- Focuses on validated metrics: weight, body fat %, lean/muscle mass
- Body water % may be useful for athletes or those monitoring hydration
- Skepticism warranted for: metabolic age, body age, visceral fat “level” from foot-only BIA, segmental analysis from basic devices
App and Data Quality:
- Provides clear trend charts over time
- Allows data export (CSV, PDF)
- Does not require subscription for basic functionality
- Transparent about how data is calculated
Price Appropriateness:
- Anything above $200 for consumer BIA is likely overpriced (not adding proportional accuracy)
- Basic BIA scale: $30–80 (single frequency, foot-only electrodes)
- Advanced BIA scale: $100–150 (multi-frequency, hand-and-foot electrodes)
💰 Common Concern: “Is it worth the cost?”
Basic BIA scales start at $30—about the same as 2 months of gym membership. If you work out regularly, knowing whether your efforts are building muscle or just burning calories is worth far more than $30.
Cost comparison over 1 year:
- Basic BIA scale: $50 (one-time) = $4.17/month
- Mid-range BIA scale: $120 (one-time) = $10/month
- Quarterly DEXA scans: $200–600/year = $17–50/month
- Personal trainer (who may misguide you without data): $200–400/month
For context: Americans spend an average of $155/month on dining out. If body composition tracking helps you train smarter and reach goals faster, the ROI is substantial.
Smart Scale Buying Checklist
Before purchasing, verify:
✓ Technology Transparency
- States measurement method clearly (bioelectrical impedance)
- Specifies frequency used (multi-frequency better than single-frequency)
- Describes electrode configuration (8-point hand-and-foot > 4-point foot-only)
✓ Realistic Claims
- States accuracy range as ±3–8% body fat (not “99% accurate” or “clinical-grade”)
- References validation studies comparing device to DEXA or hydrostatic weighing
- Acknowledges limitations (hydration effects, etc.)
✓ Core Metrics Focus
- Prioritizes validated metrics: weight, body fat %, lean mass
- Body water % may be useful
- Skeptical of: metabolic age, visceral fat “level” from foot-only BIA, 15+ metrics
✓ App Quality
- Provides trend charts over time (not just current reading)
- Allows data export (CSV or PDF format)
- No subscription required for basic functionality
- Privacy policy transparent about data usage
✓ Fair Pricing
- Basic single-frequency, foot-only: $30–80
- Multi-frequency with hand sensors: $100–150
- Anything above $200 likely overpriced (diminishing returns on accuracy)
✓ User Experience
- Consistent readings when measured repeatedly under same conditions
- Positive reviews regarding reliability (not wildly fluctuating numbers)
- Responsive customer support
- No MLM (multi-level marketing) distribution
Deal-Breakers (Avoid These):
Implies diagnostic capability or disease prevention
Claims of “lab-grade” or “medical-grade” accuracy
Vague language like “advanced sensors” without technical specs
Requires subscription for basic features
Cannot export your own data
Red Flags to Avoid
Unrealistic Claims:
- “Lab-grade accuracy” or “medical-grade accuracy” (consumer devices do not meet clinical standards)
- “99% accurate” (BIA inherently has ±3–8% error even under controlled conditions)
- Claims to measure 15+ body composition metrics (most are estimates from estimates, not validated measurements)
Lack of Transparency:
- Does not state measurement method or error range
- No validation studies cited
- Vague language like “advanced sensors” without technical specification
- No information about variables affecting accuracy
Poor User Experience:
- App requires subscription for basic features
- Cannot export your own data
- Frequent connectivity issues reported in reviews
- Inconsistent readings across repeated measurements under same conditions
Suspicious Business Practices:
- Aggressive upselling or claims device prevents disease
- Device only available through multi-level marketing (MLM)
- Health claims that imply diagnostic capability
Device Evaluation Checklist
Before purchasing:
✓ Realistic accuracy claims (±3–8% body fat stated)
✓ Validation study referenced
✓ Core metrics focused (weight, body fat, muscle mass)
✓ BIA measurement method clearly described
✗ Claims “clinical accuracy” or “>95% accurate”
✗ Offers >10 body composition metrics
✗ No validation studies or methodology information
✗ Requires ongoing subscription for basic functionality
Questions to Ask Before Purchasing
Self-Assessment:
- Do I actually need body composition tracking, or is weight + waist circumference sufficient?
- Will I use this device consistently with proper protocol (same time of day, fasted, consistent conditions)?
- Do I have a healthy relationship with body metrics, or could this device trigger unhealthy patterns?
- What will I do with the information? (If no clear answer, device may not be necessary)
Device Assessment:
- Is the price reasonable for the features offered?
- Is the stated accuracy range realistic and acceptable for my purposes?
- Has this device been validated against a reference method in published studies?
- Do user reviews mention consistent readings, or are there complaints about wildly varying numbers?
Bottom Line: No consumer device provides clinical-grade accuracy. If truly accurate body composition assessment is important for a medical reason or elite athletic training, periodic professional testing (DEXA, clinical BIA) is more appropriate than investing in expensive consumer equipment.
Professional Testing as an Alternative
Instead of purchasing a device:
Periodic Professional Testing:
- Get baseline DEXA scan or clinical BIA ($50–150)
- Use simple metrics for ongoing tracking (scale weight, waist circumference, how clothes fit, performance)
- Return for professional testing every 3–6 months if desired
- Cost: $200–600 per year (comparable to mid-range home device, but far more accurate)
Advantages:
- Reduced risk of obsessive tracking
- Higher accuracy when it matters (baseline, progress checks)
- No daily/weekly fixation on numbers
- Professional interpretation of results
Key Metrics That Don’t Require Special Devices
Many meaningful body composition indicators require no technology beyond a measuring tape and scale.
Waist Circumference
Waist circumference is a validated indicator of visceral adiposity (abdominal fat around organs) and metabolic disease risk.
How to Measure:
- Use flexible, non-stretch measuring tape
- Locate top of hip bone (iliac crest)
- Wrap tape horizontally around abdomen at this level
- Tape should be snug but not compressing skin
- Measure at end of normal exhalation
- Record to nearest 0.5 cm or 0.25 inch
Health Risk Thresholds (Adults):
| Sex | Increased Risk | Substantially Increased Risk |
| Males | ≥94 cm (37 inches) | ≥102 cm (40 inches) |
| Females | ≥80 cm (31.5 inches) | ≥88 cm (34.5 inches) |
Thresholds based on Caucasian populations. Lower thresholds (Male ≥90 cm, Female ≥80 cm) recommended for Asian populations.
Evidence: Waist circumference predicts cardiometabolic disease independent of BMI. It is a stronger predictor of metabolic risk than body weight alone (Ross et al., 2020, Nature Reviews Endocrinology).
Advantages:
- Free (requires only measuring tape)
- Well-validated against metabolic disease outcomes
- More direct measure of visceral fat than BIA estimates
- Easy to perform accurately at home
Tracking Recommendation:
- Decreasing waist circumference indicates reducing visceral adiposity regardless of scale weight changes
- Measure monthly, same time of day (morning upon waking recommended)
- Track trend over 3–6 months, not week-to-week fluctuations
Waist-to-Hip Ratio
Waist-to-hip ratio (WHR) assesses fat distribution pattern. Higher WHR indicates central (abdominal) fat accumulation, which carries greater metabolic risk than peripheral (hip/thigh) fat.
How to Calculate:
- Measure waist circumference (as described above)
- Measure hip circumference at widest point of buttocks
- Divide waist by hip measurement
Health Risk Thresholds:
| Sex | Low Risk | Moderate Risk | High Risk |
| Males | <0.90 | 0.90–0.99 | ≥1.00 |
| Females | <0.80 | 0.80–0.84 | ≥0.85 |
Clinical Use: WHR used in some research settings but waist circumference alone is simpler and equally predictive in clinical practice.
How Clothes Fit
Clothing fit is a practical, non-numerical indicator of body composition changes.
What It Indicates:
- Looser clothing suggests fat loss and/or muscle mass loss
- Tighter clothing suggests fat gain and/or muscle mass gain
- Clothing fitting differently in specific areas (e.g., pants looser in waist but tighter in thighs) may indicate regional body composition changes
Advantages:
- No measurement required
- Immediate feedback
- Subjectively meaningful (reflects real-world body size changes)
Limitations:
- Not quantitative
- Clothing brands and styles vary
- Cannot distinguish fat from muscle changes
Best Use: Supplement to other metrics. If weight is stable but clothing fits differently, body composition is changing.
Strength and Performance Metrics
Physical capability often correlates with favorable body composition, particularly muscle mass.
Useful Performance Indicators:
- Resistance training progress (weight lifted for given repetitions)
- Bodyweight exercise performance (pull-ups, push-ups, etc.)
- Walking, running, or cycling endurance
- Balance and mobility tests (especially for older adults)
Why This Matters: Functional capacity is a health outcome in itself. If strength and endurance improve, muscle mass is likely maintained or increased regardless of scale weight.
Evidence: Muscle mass is associated with mortality risk in older adults, but strength and physical function are even stronger predictors (Srikanthan & Karlamangla, 2011, Journal of Clinical Endocrinology & Metabolism).
When Simple Methods Are Sufficient
For many health goals, body composition technology is unnecessary:
| Goal | Sufficient Metrics |
| General health maintenance | Scale weight monthly + annual physical exam |
| Fat loss for health | Scale weight weekly + waist circumference monthly |
| Muscle gain verification | Strength performance (weight lifted) + how clothes fit |
| Health risk screening | Waist circumference + blood pressure, glucose, and lipids (clinical tests) |
| Avoiding body metric fixation | No tracking; focus on health behaviors, how you feel, what you can do |
Summary and Recommendations
Body composition tracking can provide useful information when used appropriately, but it is not necessary for most people pursuing general health and fitness.
Key Takeaways:
- Body composition provides more information than weight alone. Two individuals at the same weight may have very different body compositions and health risks.
- No consumer device is clinically accurate. Consumer bioelectrical impedance scales have ±5–8% body fat error. They are useful for tracking trends over time, not for precise measurements.
- DEXA is the reference standard for accurate body composition assessment, but it is expensive and unnecessary for most people. Use it for baseline or validation if needed, not for frequent tracking.
- Waist circumference is a validated, free alternative. It predicts cardiometabolic disease independent of body weight and requires only a measuring tape.
- Tracking can become counterproductive. If tracking causes anxiety, obsession, or unhealthy behaviors, stop tracking and consult a healthcare provider or mental health professional.
- Body composition is one health indicator among many. Metabolic health markers (blood pressure, glucose, lipids), cardiovascular fitness, strength, mental health, and quality of life are equally or more important.
- For most people, simple metrics are sufficient: scale weight, waist circumference, how clothes fit, and how you feel provide adequate feedback without requiring body composition technology.
When Professional Body Composition Assessment Is Indicated:
- Clinical need (sarcopenia screening, eating disorder recovery, chronic disease management)
- Baseline before significant body recomposition program (athletes, intensive training)
- Validation of consumer device accuracy
- Medical decision-making (not general curiosity)
When Consumer Devices May Be Helpful:
- Resistance training progress tracking
- Verifying fat loss with muscle preservation during weight loss
- Motivation when used in psychologically healthy way
- Supplement to (not replacement for) health behaviors and clinical markers
When Tracking Should Be Avoided:
- History of eating disorders or body dysmorphia
- Tracking causes anxiety, obsession, or mood changes
- Children and adolescents (healthcare provider should monitor)
- Pregnant or postpartum individuals
- When simpler methods (weight, waist circumference, performance) are adequate
Final Perspective: Body composition metrics can inform health and fitness decisions, but they are tools, not goals. Optimal health depends on nutrition, physical activity, sleep, stress management, social connection, and psychological well-being—not a specific body fat percentage. Use body composition information when it genuinely serves your health, and ignore it when it does not.
References
American Council on Exercise. (n.d.). Percent body fat norms for standard adults. ACE Fitness.
Fiatarone, M. A., et al. (1994). Exercise training and nutritional supplementation for physical frailty in very elderly people. New England Journal of Medicine, 330(25), 1769–1775.
Gallagher, D., et al. (1998). Appendicular skeletal muscle mass: effects of age, gender, and ethnicity. American Journal of Clinical Nutrition, 67(4), 673–681.
Goossens, G. H. (2017). The metabolic phenotype in obesity: fat mass, body fat distribution, and adipose tissue function. Diabetologia, 60(10), 1645–1654.
Heymsfield, S. B., et al. (2011). Weight loss composition is one-fourth fat-free mass: a critical review and critique of this widely cited rule. Obesity Reviews, 12(5), e329–e339.
Kaji, H. (2013). Linkage between muscle and bone: common catabolic signals resulting in osteoporosis and sarcopenia. Clinical Calcium, 23(11), 1607–1614.
Kyle, U. G., et al. (2001). Age-related differences in fat-free mass, skeletal muscle, body cell mass and fat mass between 18 and 94 years. European Journal of Clinical Nutrition, 55(8), 663–672.
Landi, F., et al. (2013). Sarcopenia as a risk factor for falls in elderly individuals: results from the ilSIRENTE study. BMJ Open, 3(2), e002762.
Marra, M., et al. (2019). Assessment of body composition in health and disease using bioelectrical impedance analysis (BIA) and dual energy X-ray absorptiometry (DXA): a critical overview. Nutrition, 62, 51–59.
Nana, A., et al. (2014). Importance of standardized DXA protocol for assessing physique changes in athletes. European Journal of Clinical Nutrition, 68(11), 1204–1211.
Neumark-Sztainer, D., et al. (2006). Obesity, disordered eating, and eating disorders in a longitudinal study of adolescents: how do dieters fare 5 years later? International Journal of Eating Disorders, 39(8), 629–639.
Nickerson, B. S., et al. (2020). Validity of four commercially available bioelectrical impedance scales for body composition assessment. International Journal of Exercise Science, 13(4), 1396–1405.
Oliveros, E., et al. (2014). The concept of normal weight obesity. Progress in Cardiovascular Diseases, 56(4), 426–433.
Pacanowski, C. R., et al. (2015). Self-weighing: Helpful or harmful for psychological well-being? A review of the literature. Obesity, 23(8), 1512–1518.
Peterson, M. D., et al. (2010). Resistance exercise for muscular strength in older adults: a meta-analysis. Medicine & Science in Sports & Exercise, 42(3), 426–434.
Romero-Corral, A., et al. (2008). Accuracy of body mass index in diagnosing obesity in the adult general population. International Journal of Obesity, 32(6), 959–966.
Ross, R., et al. (2020). Waist circumference as a vital sign in clinical practice: a Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity. Nature Reviews Endocrinology, 16(3), 177–189.
Srikanthan, P., & Karlamangla, A. S. (2011). Relative muscle mass is inversely associated with insulin resistance and prediabetes. Findings from the Third National Health and Nutrition Examination Survey. Journal of Clinical Endocrinology & Metabolism, 96(9), 2898–2903.
Volpi, E., et al. (2004). Muscle tissue changes with aging. Current Opinion in Clinical Nutrition & Metabolic Care, 7(4), 405–410.
Wang, Z. M., et al. (1992). The five-level model: a new approach to organizing body-composition research. American Journal of Clinical Nutrition, 56(1), 19–28.
Wells, J. C. (2007). Sexual dimorphism of body composition. Best Practice & Research Clinical Endocrinology & Metabolism, 21(3), 415–430.
Westcott, W. L. (2012). Resistance training is medicine: effects of strength training on health. Current Sports Medicine Reports, 11(4), 209–216.
About the Medical Reviewer:
Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Dr. Das serves as the lead medical reviewer for Wearable Wellness Guide. He specializes in translating clinical validation research on consumer wellness devices into consumer-friendly analysis. His role includes developing evidence-based testing protocols, evaluating sensor accuracy and measurement reliability, and ensuring all health-related content is medically sound.
Credentials: M.B.B.S. (Grant Government Medical College, Mumbai, 2024) | Post-Graduate Certificate in Health Informatics (Columbia University, 2025) | Specialization in Immunology (Imperial College London, 2025) | Post-Graduate Diploma in Neuroscience (Johns Hopkins University, 2025) | Medical License: Medical Council of India (MCI) and Maharashtra Medical Council (MMC) – License No: PR/7466/2024
Full credentials and scope of review authority on About page
Medical Disclaimer: The information on this page is for educational purposes and should not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis, treatment, or medical device recommendations tailored to your individual health needs.





