Understand Your Sleep Quality with Better Tracking
Explore the science of sleep quality and HRV. Compare wearables vs. clinical studies to understand your sleep data and improve recovery habits.
✓ MEDICALLY REVIEWED by Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Written by Wearable Wellness Guide
Last updated: February 11, 2026 | Reading time: 8 minutes
Medically reviewed according to the standards outlined on our About page
Introduction
Whether you’re a 30-something professional struggling with sleep quality, a health-conscious parent wanting to optimize recovery, or a 50+ adult concerned about cardiovascular health—understanding your sleep data starts here.
You’ve been waking up tired for months. Your smartwatch says you got 7 hours of sleep, but you feel like you got 4. The data shows “light sleep” and “REM cycles,” but what does that actually mean? And more importantly—how do you fix it?
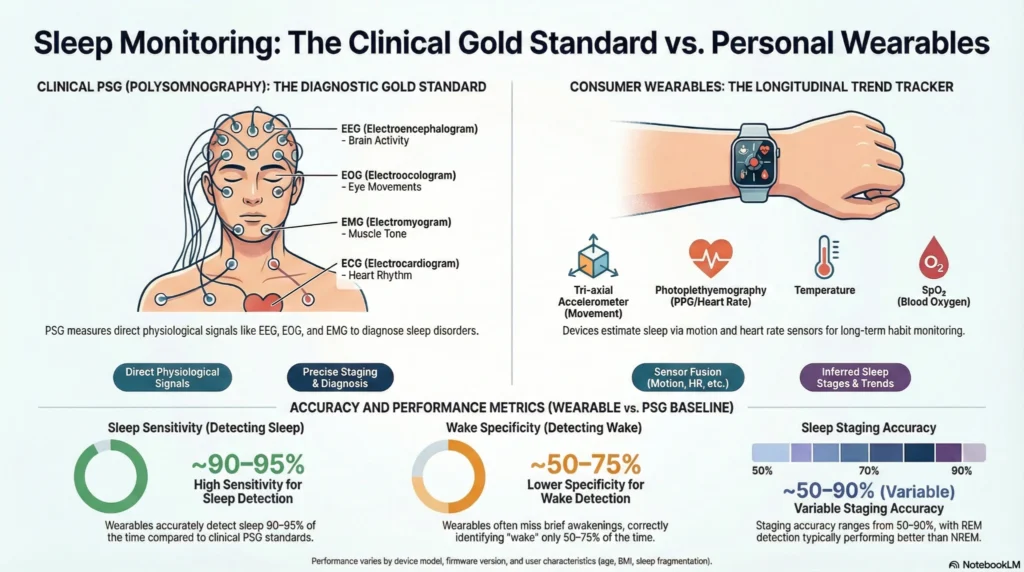
Sleep quality affects cardiovascular health, cognitive function, immune response, and metabolic regulation. Consumer sleep tracking devices may provide insight into sleep patterns—but these tools have significant limitations compared to clinical polysomnography (the gold-standard sleep study used in medical settings) with peer-reviewed research on sleep disturbance health impacts.
Key Points
- Medical-grade sleep studies remain the diagnostic standard for sleep disorders
- Sleep trackers measure movement, heart rate, and sometimes respiratory patterns—not direct brain activity
- Tracking is associated with improved sleep awareness but does not replace clinical evaluation
- Obsessive tracking (“orthosomnia”) may paradoxically worsen sleep anxiety in some individuals
When to Consult a Healthcare Provider
- Concerns about sleep data patterns
- Chronic snoring with breathing pauses (possible sleep apnea)
- Persistent daytime fatigue despite adequate sleep duration
- Insomnia lasting more than 3 weeks
- Unusual movements or behaviors during sleep
Educational Framework
This page provides evidence-based information about sleep physiology and monitoring technology. It is not intended for self-diagnosis or treatment of sleep disorders.
Common Sleep Tracker Concerns Answered
“Aren’t these devices inaccurate?”
Consumer sleep trackers achieve 70-90% accuracy for basic sleep/wake detection and 60-70% for sleep stages compared to clinical polysomnography. While not diagnostic-grade, they’re good enough for tracking personal trends week-over-week. Focus on patterns over time, not nightly precision. independent comparative study of seven consumer devices
“I can’t sleep with something on my wrist”
Consider smart rings (Oura, RingConn) or bedside monitors (Withings Sleep) for zero-wear tracking. Comfort is critical—if you won’t wear it consistently, the most accurate tracker is worthless.
“Will this make me obsess over my sleep?”
This is a real risk called “orthosomnia” (sleep tracking anxiety- a clinically documented phenomenon called orthosomnia). Prevention: Use weekly review mode instead of daily score-checking. Turn off sleep score notifications. Track 1 week per month, not continuously. If tracking increases anxiety, take breaks.
“Is my sleep data private?”
Check each manufacturer’s data policy. Most store data encrypted on their servers. Opt for devices with local-only storage if privacy is critical. Never assume sleep data is completely private.
“Can’t I just use my free phone app?”
Yes—absolutely start with a free app (Sleep Cycle, Sleep as Android). Upgrade to wearables only if you want heart rate, blood oxygen (SpO₂), and significantly better accuracy. Many people never need more than a phone app.
“Which tracker is best for detecting sleep apnea?”
No consumer device diagnoses sleep apnea. Some devices (Apple Watch, Fitbit, Whoop) can detect breathing irregularities that warrant medical evaluation, but you need a medical sleep study for diagnosis. If you snore loudly with breathing pauses, see a doctor—don’t rely on tracker data alone.
Table Of Contents
- Understand Your Sleep Quality with Better Tracking
- Introduction
- Common Sleep Tracker Concerns Answered
- What You'll Learn in This Guide
- Why Sleep Tracking Changes Everything (The Real Benefits)
- Quick Guide: Choose Your Sleep Tracker in 3 Minutes
- Sleep Science Fundamentals
- What Sleep Trackers Actually Measure
- Limitations of Consumer Sleep Tracking
- Interpreting Your Sleep Data
- Sleep Tracking for Specific Concerns
- Beyond Tracking: Improving Sleep Quality
- Recovery and Readiness Monitoring
- Choosing Sleep Tracking Approaches
- Comparing Sleep Tracking Options
- Frequently Asked Questions About Sleep Tracking
- How accurate are consumer sleep trackers?
- Can I improve deep sleep with a tracker?
- Which sleep tracker is most accurate?
- Do I need to wear it every night?
- Are smart rings better than watches for sleep tracking?
- Can sleep trackers diagnose sleep apnea?
- Will tracking my sleep make me sleep worse?
- What's the best free sleep tracker?
- How much should I spend on a sleep tracker?
- Can I use my sleep tracker data to diagnose myself?
- References
- Medical Disclaimer
What You’ll Learn in This Guide
✓ How sleep trackers actually work (and their limitations you need to know)
✓ Which sleep metrics matter most for your specific health goals
✓ Device comparison: $50 vs $500—what’s actually worth the investment?
✓ When to trust your tracker data vs. when to see a doctor
✓ Real strategies to improve your sleep using tracker insights
📥 FREE DOWNLOAD: Sleep Tracker Comparison Cheat Sheet – One-Page PDF
Print-friendly guide comparing all major sleep trackers with pros/cons, pricing, and use-case recommendations.
Why Sleep Tracking Changes Everything (The Real Benefits)
Discover Hidden Sleep Disorders Before They Impact Health
A $100 tracker that identifies sleep apnea patterns could prompt you to get a medical diagnosis, potentially saving you $15,000+ in future cardiovascular treatment costs. Many users discover they’re experiencing 20-30 breathing disruptions per hour—without realizing it.
Optimize Recovery for Better Performance and Energy
See exactly how caffeine after 2pm, alcohol, late meals, or screen time affect your deep sleep percentage. Make data-driven bedtime changes instead of guessing what works as indicated in study published in NPJ Digital Medicine
Catch Sleep Problems Early
Notice when your sleep efficiency drops from 90% to 75% consistently—a pattern that might indicate developing insomnia, stress impact, or health changes worth addressing before they worsen.
Build Sleep Consistency (The #1 Factor)
Tracking reveals your actual bedtime variability. Going to bed at 10pm one night and 1am the next destroys sleep quality—even if total hours look adequate. Trackers make this visible.
Quantify What Actually Helps
Test whether magnesium supplements, meditation, or temperature changes improve your sleep. Before/after data eliminates guesswork and wasted money on ineffective interventions.
Quick Guide: Choose Your Sleep Tracker in 3 Minutes
Answer These 3 Questions:
1. What’s your primary goal?
- General wellness / curiosity → Start with free phone app or budget fitness band ($50-100)
- Athletic recovery optimization → Whoop, Garmin, or Polar with HRV tracking ($200-500)
- Detect potential sleep disorder → Apple Watch or Fitbit with SpO₂ monitoring ($200-400)
- Minimize cost → Free phone app (Sleep Cycle, Sleep as Android) or Mi Band ($30-50)
2. What’s your comfort preference?
- Wrist device OK → Smartwatch or fitness band (most options, $50-800)
- Prefer minimal/no awareness → Smart ring ($250-400)
- Can’t sleep with anything worn → Bedside monitor ($100-400)
3. What’s your budget?
- Under $100: Phone app (free), Mi Band ($35-50), Fitbit Inspire ($100)
- $100-300: Fitbit Versa/Charge, Garmin Venu, basic Apple Watch SE
- $300+: Oura Ring ($299-549), Apple Watch Series, Garmin Fenix, Whoop (subscription $30/month)
Our Top Picks by Use Case:
→ Best for Beginners: Fitbit Inspire 3 ($100) — accurate, affordable, easy app
→ Best for Athletes: Whoop 4.0 ($30/month) — recovery metrics, strain tracking, no screen
→ Best for Comfort: Oura Ring Gen 3 ($299) — minimal form factor, excellent accuracy
→ Best Budget: Sleep as Android app (Free/$5) — start here before buying hardware
→ Best All-Around: Apple Watch SE ($249) or Series 9 ($399) — comprehensive health tracking
Not sure? Start free. Download Sleep Cycle or Sleep as Android. Track for 1-2 weeks. If you want more detailed heart rate and recovery data, upgrade to a wearable.
Sleep Science Fundamentals
Understanding Sleep Stages
Sleep architecture consists of distinct physiological states, each serving specific restorative functions. American Academy of Sleep Medicine classification system
| Sleep Stage | Brain Wave Pattern | Physiological Characteristics | Primary Functions | Typical Duration (per cycle) |
| Wake | Beta/Gamma waves | Full consciousness, muscle tone present | Alertness, environmental awareness | Variable |
| N1 (Light Sleep) | Theta waves | Transitional state, easily disrupted | Sleep initiation | 1-7 minutes |
| N2 (Light Sleep) | Sleep spindles, K-complexes | Reduced heart rate, body temperature drops | Memory consolidation, sensory gating | 10-25 minutes |
| N3 (Deep Sleep) | Delta waves | Lowest heart rate, muscle relaxation | Physical restoration, immune function, growth hormone release | 20-40 minutes |
| REM Sleep | Mixed frequency, similar to wake | Rapid eye movements, muscle atonia, vivid dreams | Emotional processing, memory integration, learning | 10-30 minutes (increases in later cycles) |
Evidence Base:
- Stage classifications defined by American Academy of Sleep Medicine (AASM) scoring manual
- Each stage is associated with distinct electroencephalography (EEG) patterns
- Clinical sleep studies measure brain activity directly; consumer devices infer stages from movement and heart rate
💡 QUICK TIP: Focus on these 3 metrics first if you’re new to tracking: (1) Total Sleep Time, (2) Deep Sleep %, (3) Sleep Consistency. Ignore the rest until you understand these fundamentals.
Sleep Cycles Through the Night
Normal sleep progresses through 4-6 complete cycles per night, with stage distribution changing across the sleep period.
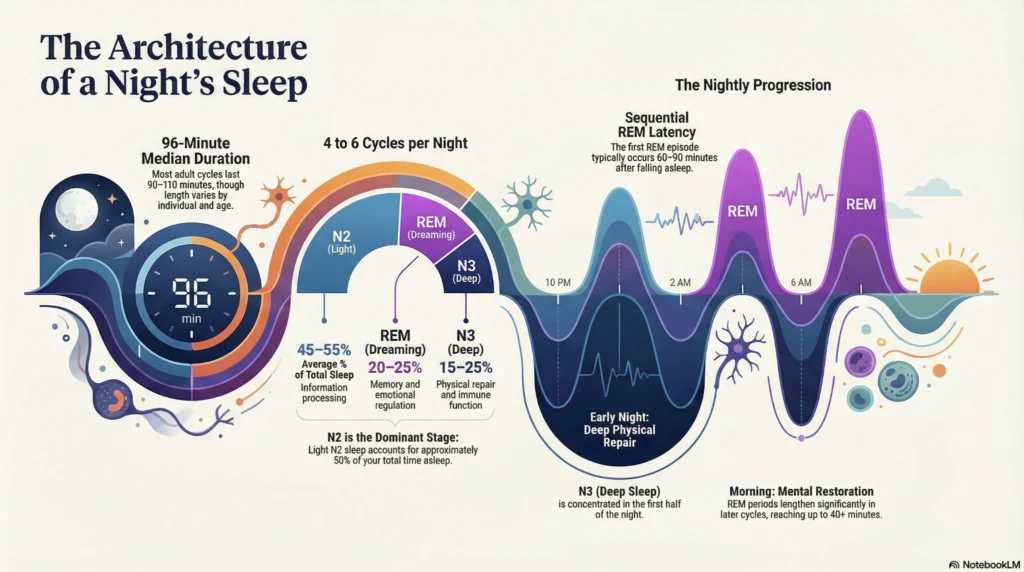
Cycle Progression Pattern
| Sleep Period | Cycle Duration | Deep Sleep Proportion | REM Sleep Proportion | Biological Significance |
| First Cycle | 70-100 minutes | 30-40% | 5-10% | Maximum deep sleep for physical recovery |
| Second Cycle | 90-110 minutes | 20-30% | 10-15% | Continued deep sleep, increasing REM |
| Third Cycle | 90-120 minutes | 10-20% | 15-25% | Shift toward REM dominance |
| Fourth+ Cycles | 90-120 minutes | 0-10% | 25-40% | REM sleep predominates, minimal deep sleep |
Clinical Implications:
- Early sleep interruption disproportionately affects physical recovery (deep sleep)
- Late sleep disruption impacts emotional regulation and memory (REM sleep)
- Alcohol suppresses REM sleep in first half of night, causing REM rebound later
- Sleep restriction reduces deep sleep first, then affects REM sleep
REM Sleep and Deep Sleep Functions
Deep sleep (N3) and REM sleep serve distinct physiological roles.
Deep Sleep (N3) Functions
Physical Restoration:
- Tissue repair and muscle growth
- Immune system strengthening
- Metabolic regulation
Hormonal Regulation:
- Growth hormone secretion peaks during deep sleep
- Cortisol levels reach lowest point
Brain Maintenance:
- Glymphatic system clearance (waste removal from brain)
- Synaptic homeostasis. (study in Journal of Clinical Sleep Medicine) (evidence for slow wave sleep’s restorative role)
REM Sleep Functions
Cognitive Processing:
- Memory consolidation (especially procedural and emotional memories)
- Learning integration
- Creative problem-solving
Emotional Regulation:
- Processing emotional experiences
- Mood regulation
Brain Development:
- Critical for neural development in infants and children
Evidence-Based Observations:
- Both stages appear necessary; selective deprivation of either impacts health
- REM sleep deprivation is associated with mood disturbances and impaired learning
- Deep sleep deprivation may affect immune function and physical recovery
Sleep Duration vs. Sleep Quality
Sleep quality encompasses multiple factors beyond total sleep time.
| Sleep Quality Component | How It’s Measured Clinically | Consumer Tracker Estimation | Health Relevance |
| Total Sleep Time | Direct observation + EEG | Movement cessation patterns | Basic sleep adequacy |
| Sleep Efficiency | (Total sleep ÷ Time in bed) × 100 | Movement-based estimation | Insomnia indicator |
| Sleep Latency | Time from lights out to sleep onset | Movement pattern analysis | Sleep initiation difficulty |
| Wake After Sleep Onset (WASO) | EEG-confirmed wake periods | Movement detection | Sleep maintenance issues |
| Stage Distribution | EEG wave pattern analysis | Heart rate + movement algorithms | Sleep architecture assessment |
| Respiratory Events | Airflow + oxygen saturation | Limited: Some devices detect irregularities | Sleep apnea screening |
American Academy of Sleep Medicine and Sleep Research Society recommendation
Clinical Perspective:
- Subjective sleep quality does not always correlate with objective measurements
- Adults generally need 7-9 hours of sleep, but individual variation exists (consensus guidelines for adult sleep duration)
- Sleep efficiency above 85% is typically considered normal
- Fragmented sleep (high WASO) may impair restorative functions even with adequate duration
Consumer Tracker Limitations:
- Movement-based detection may misclassify quiet wakefulness as sleep
- Stage classification accuracy varies significantly between devices
- No consumer device is FDA-cleared for diagnosing sleep disorders
What Sleep Trackers Actually Measure
Movement-Based Sleep Detection
Most consumer sleep trackers use accelerometers to detect movement patterns.
Detection Method
| Technology | What It Measures | Sleep Inference | Accuracy Limitations |
| Actigraphy | Wrist/body movement via accelerometer | Stillness = Sleep, Movement = Wake | Cannot detect quiet wakefulness; may classify reading in bed as sleep |
| Sleep/Wake Classification | Movement frequency and intensity | Prolonged stillness classified as sleep periods | 85-95% agreement with polysomnography for sleep/wake only |
| Sleep Stage Estimation | Movement patterns + heart rate | Algorithms infer stages from combined data | 60-70% agreement with PSG for stage classification |
Evidence Base:
- Actigraphy has been validated for general sleep/wake patterns in research settings
- Stage classification algorithms are proprietary and vary significantly between manufacturers
- Studies show consumer devices may overestimate sleep time by 10-30 minutes compared to polysomnography Our testing methodology follows standardized protocols to verify these accuracy claims as confirmed in a comprehensive review of wearable sleep technology.
When Movement Detection Fails:
- Bedpartner movement may affect some devices
- Quiet activities (reading, meditation) may be classified as sleep
- Periodic limb movements may fragment detected sleep
Heart Rate Variability During Sleep
Heart rate variability (HRV) reflects autonomic nervous system activity and changes across sleep stages.
HRV Sleep Patterns
| Sleep Stage | Autonomic State | Heart Rate Pattern | HRV Pattern | Tracker Application |
| Wake | Sympathetic dominance | Variable, responsive | Lower HRV | Baseline comparison |
| Light Sleep (N1-N2) | Parasympathetic increase | Gradual decrease | Moderate HRV | Transition detection |
| Deep Sleep (N3) | Maximum parasympathetic activity | Lowest, most stable | Highest HRV | Deep sleep estimation |
| REM Sleep | Mixed autonomic activity | Variable, elevated | Lower HRV, irregular | REM sleep detection |
Measurement Considerations:
- Nocturnal HRV trends may indicate recovery status or stress levels
- Optical heart rate sensors (photoplethysmography) may have reduced accuracy during sleep
- HRV measurements require sufficient sampling rate and accuracy
Clinical Context:
- HRV is one of multiple inputs for sleep stage algorithms
- Reduced HRV during sleep is associated with cardiovascular risk and stress
- Significant HRV changes may warrant medical evaluation
Respiratory Rate Monitoring
Some advanced trackers estimate respiratory rate through movement detection or pulse waveform analysis.
Monitoring Approaches
| Method | Technology | Typical Range | Clinical Relevance | Limitations |
| Chest Movement | Accelerometer in chest strap | 12-20 breaths/minute (adult) | Baseline respiratory monitoring | Requires specific device placement |
| Wrist Movement | Algorithm detects breathing-related motion | Estimated range | Pattern detection for irregularities | Lower accuracy than chest placement |
| Pulse Waveform Analysis | Optical sensor detects breathing effects on pulse | Estimated rate | Non-invasive estimation | May be affected by movement |
Potential Applications:
- Monitoring respiratory health trends
- Detecting significant deviations from baseline
- Identifying patterns consistent with sleep-disordered breathing
Critical Limitation:
- Oxygen saturation (SpO₂) monitoring provides additional relevant data in some devices
- Consumer devices cannot diagnose sleep apnea or other respiratory disorders
- Medical evaluation required for any concerning respiratory patterns
Limitations of Consumer Sleep Tracking
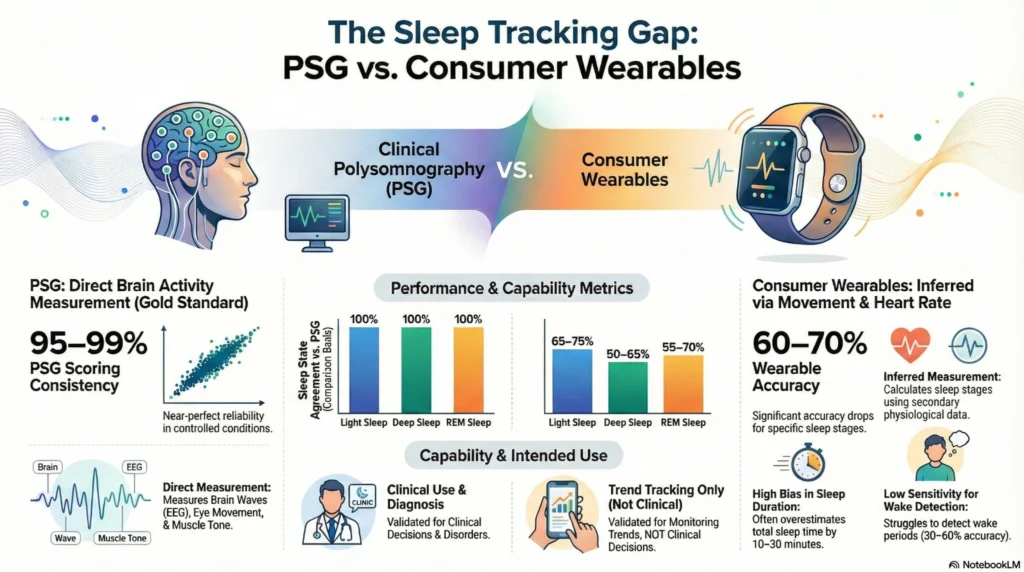
Consumer sleep tracking technology has inherent constraints compared to clinical polysomnography.
Accuracy Comparison
| Measurement | Polysomnography (Gold Standard) | Consumer Wearables | Practical Implication |
| Sleep vs. Wake | 98-99% accuracy (EEG-based) | 85-95% accuracy (movement-based) | May overestimate sleep time |
| Sleep Stage Classification | Direct brain wave measurement | 60-70% accuracy (algorithmic inference) | Stage data is approximate |
| Sleep Apnea Detection | Diagnostic standard (airflow, effort, oxygen) | Screening only (some devices) | Cannot replace medical sleep study |
| Periodic Limb Movements | Leg muscle sensors (EMG) | Not measured | Missed movement disorders |
| Brain Activity | Multiple EEG channels | Not measured | No direct neural assessment |
independent comparative study of seven consumer devices
Known Issues:
- First-Night Effect: Users may sleep differently when first wearing a device
- Orthosomnia: Excessive focus on sleep data may increase anxiety and worsen sleep
- Algorithm Variability: Different manufacturers use different classification methods
- Individual Variation: Algorithms may perform differently for different individuals
Appropriate Use:
- Trend monitoring over time (relative changes in personal patterns)
- Sleep schedule consistency assessment
- Awareness tool for sleep habits
- Motivation for sleep hygiene improvements
Inappropriate Use:
- Treatment decisions based solely on tracker data
- Self-diagnosis of sleep disorders
- Replacement for medical evaluation
- Obsessive nightly score checking
Interpreting Your Sleep Data
Sleep Score Calculations
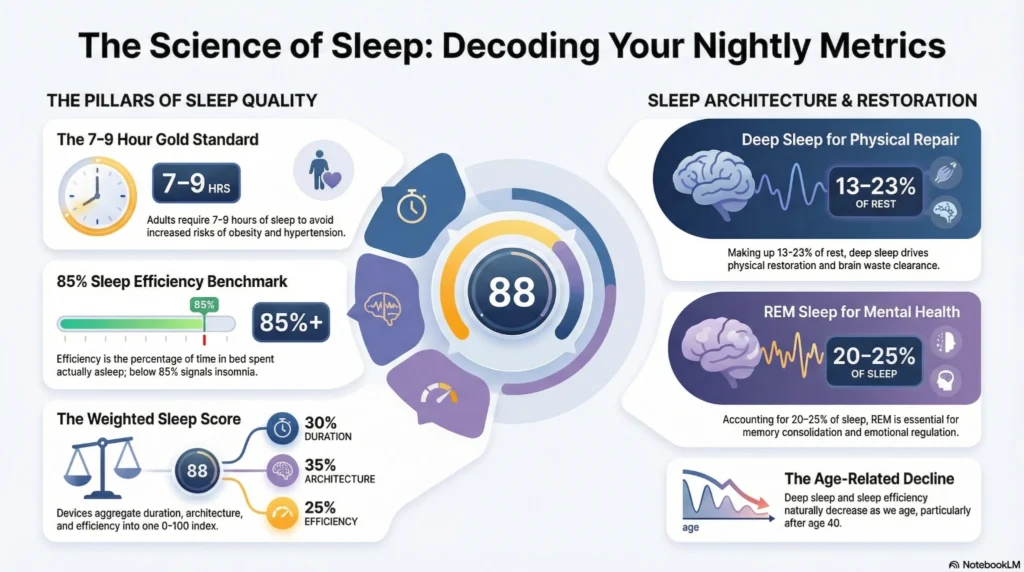
Sleep scores are proprietary algorithms that combine multiple metrics into a single number.
Common Score Components
| Component | Typical Weight | What It Measures | Influencing Factors |
| Total Sleep Time | 20-30% | Hours of sleep detected | Time in bed, sleep efficiency |
| Sleep Stages | 25-35% | Distribution of deep/REM/light sleep | Age, sleep debt, alcohol |
| Sleep Efficiency | 15-25% | Percentage of time in bed spent asleep | Sleep latency, WASO |
| Disturbances | 10-20% | Frequency of detected wake/movement | Environment, stress, health |
| Timing/Consistency | 10-15% | Alignment with circadian rhythm | Bedtime regularity, schedule |
Interpretation Guidelines:
- Scores are relative to proprietary algorithms, not medical standards
- Different devices use different scoring methods (scores are not comparable across brands)
- Trends matter more than individual night scores
- A “poor” score with good subjective sleep quality may not be concerning
What Scores Cannot Tell You:
- Root causes of poor sleep (multiple factors may contribute)
- Whether you have a sleep disorder (medical diagnosis required)
- Exact sleep stage percentages (estimation only)
⚠️ WARNING: Don’t compare sleep scores across different brands. A “75” on Fitbit ≠ “75” on Oura ≠ “75” on Whoop. Each company uses proprietary algorithms. Only compare your scores to your own historical data within the same device.
Sleep Stage Distribution
Sleep stage percentages vary by age, individual factors, and measurement accuracy.
Approximate Stage Distributions (Adults 18-64)
| Sleep Stage | Typical Percentage | Normal Range | Factors Affecting Distribution |
| Light Sleep (N1+N2) | 45-55% | 40-60% | Age, sleep pressure, medications |
| Deep Sleep (N3) | 15-25% | 10-25% | Age (decreases with aging), sleep debt, alcohol |
| REM Sleep | 20-25% | 15-30% | Time of night, alcohol, antidepressants, sleep debt |
| Wake | 2-5% | 0-10% | Sleep quality, age, health conditions |
Age-Related Changes
| Age Group | Deep Sleep % | REM Sleep % | Notable Patterns |
| Infants (0-1 year) | 20-25% | 50% (including active sleep) | REM dominates early development |
| Children (3-12 years) | 20-30% | 20-25% | High deep sleep for growth |
| Young Adults (18-25) | 15-25% | 20-25% | Peak sleep quality period |
| Middle Adults (26-64) | 10-20% | 20-25% | Gradual deep sleep decline |
| Older Adults (65+) | 5-15% | 15-20% | Reduced deep sleep, more fragmentation |
Clinical Perspective:
- Concerning changes: Consult healthcare provider rather than self-interpreting device data
- Consumer devices may misclassify stages (remember 60-70% accuracy)
- Normal variation exists; percentages outside typical ranges may still be normal for an individual
- Stage distribution should be interpreted as general patterns, not precise measurements
Sleep Consistency and Timing
Sleep schedule regularity affects circadian rhythm alignment and sleep quality.
Consistency Metrics
| Metric | How It’s Calculated | Target | Health Relevance |
| Bedtime Variability | Standard deviation of sleep onset times | <30 minutes variation | Circadian rhythm stability |
| Wake Time Variability | Standard deviation of wake times | <30 minutes variation | Social jet lag prevention |
| Sleep Duration Variability | Standard deviation of total sleep time | <60 minutes variation | Consistent sleep pressure |
| Weekend Sleep Debt | Difference between weekday and weekend sleep | <1 hour difference | Social jet lag indicator |
Social Jet Lag:
- Misalignment between biological clock and social schedule
- Associated with metabolic dysfunction and mood disturbances
- Common in people who sleep much later on weekends than weekdays
study on circadian misalignment and obesity
Timing Considerations:
- Forced early schedules for natural late chronotypes may impair sleep quality
- Individual chronotypes vary (morning larks vs. night owls)
- Optimal sleep timing aligns with individual circadian rhythm
Recognizing Patterns vs. Obsessing Over Numbers
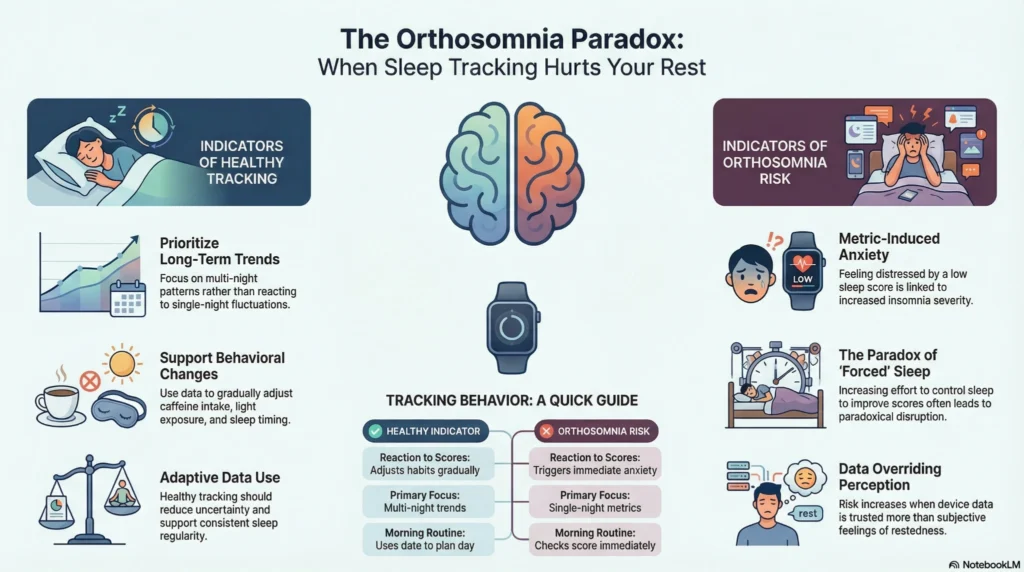
Tracking can improve awareness but may cause anxiety when approached obsessively.
Healthy Tracking Approach vs. Orthosomnia
| Healthy Use | Orthosomnia (Problematic) | Potential Consequences |
| Review weekly trends | Check score immediately upon waking | Performance anxiety about sleep |
| Notice patterns over time | Anxiety about imperfect scores | Paradoxical insomnia (worry prevents sleep) |
| Use data to inform sleep hygiene | Make decisions based on nightly scores | Reinforcement of sleep anxiety |
| Take breaks from tracking | Never miss a night of tracking | Dependency on device for sleep confidence |
| Focus on how you feel | Dismiss how you feel if score is “good” | Disconnection from body signals |
Evidence on Orthosomnia:
- Clinical case reports describe patients obsessing over sleep tracker data
- Some individuals report increased sleep anxiety related to tracking
- May lead to excessive focus on sleep that paradoxically worsens it
Recommendation:
- If tracking increases anxiety, discontinue use
- Use tracking as one tool among many for sleep awareness
- Prioritize subjective sleep quality and daytime function
- Consider periodic breaks from tracking
📊 RESEARCH STAT: 27% of sleep tracker users report increased sleep anxiety related to tracking. If you check your score immediately upon waking with worry, you may be developing orthosomnia. Take a 2-week break from tracking. a clinically documented phenomenon called orthosomnia
Sleep Tracking for Specific Concerns
General Sleep Quality Improvement
Sleep tracking may support behavior change when used appropriately.
Evidence-Based Applications
| Use Case | How Tracking Helps | Limitations | Additional Strategies |
| Identifying Short Sleep | Objective duration tracking | Doesn’t identify why sleep is short | Sleep hygiene education, schedule planning |
| Consistency Monitoring | Quantifies schedule variability | Doesn’t address root causes | Gradual schedule adjustment |
| Behavior Impact Assessment | Before/after comparison for changes | Placebo effects possible | Control for other variables |
| Sleep Debt Awareness | Cumulative duration tracking | Doesn’t determine optimal individual need | Pay attention to daytime alertness |
Behavior Changes Supported by Evidence:
- Fixed wake time (7 days/week): Stabilizes circadian rhythm, may improve sleep quality over weeks
- Pre-sleep routine: 30-60 minute wind-down period, consistent signals to body
- Limitation of time in bed: Sleep efficiency improvement, used in cognitive behavioral therapy for insomnia (CBT-I)
When Tracking May Not Help:
- If medical sleep disorder is suspected
- If data causes anxiety or obsession
- When sleep problems persist despite behavior changes
Shift Work and Irregular Schedules
Shift workers and those with irregular schedules face circadian disruption challenges.
Tracking Applications for Shift Work
| Application | Potential Benefit | Key Metrics | Considerations |
| Documenting Sleep Patterns | Identifies total sleep obtained across shifts | Total daily sleep, timing patterns | Multiple sleep periods may be needed |
| Optimizing Sleep Windows | Finds best times for recovery sleep | Sleep quality by timing | Individual variation in adaptation |
| Monitoring Cumulative Debt | Tracks sleep deficit over work periods | Weekly total sleep time | Chronic partial sleep restriction risk |
| Recovery Period Planning | Assesses time needed for circadian realignment | Consistency restoration | May take several days post-shift cycle |
Special Considerations:
- Night shift work is associated with increased health risks even with adequate sleep duration
- Light exposure timing critically affects circadian adaptation
- Some individuals never fully adapt to night shift work
- Rotating shifts may be more challenging than permanent night shifts
Evidence-Based Strategies (beyond tracking):
- Strategic light exposure (bright light during work, darkness for sleep)
- Consistent sleep schedule on workdays
- Napping strategies for shift transitions
- Medical evaluation for persistent fatigue
Travel and Time Zone Changes
Sleep tracking may help assess jet lag recovery and inform adjustment strategies.
Jet Lag Tracking
| Metric | What to Monitor | Typical Recovery | Optimization Strategy |
| Sleep Timing | Gradual alignment with new time zone | ~1 day per time zone crossed | Gradual pre-travel adjustment |
| Sleep Quality | Fragmentation and efficiency | Normalizes as circadian adjusts | Light exposure timing at destination |
| Total Sleep Time | May be reduced during adjustment | Returns to baseline with adjustment | Napping strategy for large time shifts |
| Subjective Function | Alertness and performance | Lags behind sleep adjustment | Caffeine timing, activity scheduling |
Direction Matters:
- Eastward travel (phase advance): Generally more difficult
- Westward travel (phase delay): Usually easier to adapt
Evidence-Based Recommendations:
- Stay hydrated
- Adjust sleep schedule 1-2 hours/day before departure for large time shifts
- Strategic light exposure at destination (bright light when alertness needed)
- Avoid alcohol during flights (disrupts sleep architecture)
When Tracking Might Indicate a Sleep Disorder
Consumer tracking cannot diagnose sleep disorders but may identify patterns warranting medical evaluation.
Warning Patterns Requiring Medical Consultation
| Pattern Observed | Possible Condition | Why Medical Evaluation Is Critical | What Evaluation Involves |
| Frequent breathing irregularities (if detected) | Obstructive sleep apnea | Untreated OSA increases cardiovascular risk | Polysomnography, possible home sleep test |
| Consistently low sleep efficiency (<75%) | Insomnia disorder | Chronic insomnia affects mental and physical health | Clinical interview, sleep diary, possible PSG |
| Excessive movements/awakenings | Periodic limb movement disorder, REM sleep behavior disorder | May indicate neurological conditions | PSG with EMG monitoring |
| Very short REM periods or absence | REM sleep suppression | May relate to medication effects or disorders | Medication review, PSG |
| Chronic insufficient sleep despite adequate opportunity | Circadian rhythm disorder, hypersomnia | Impacts function and may have underlying causes | Sleep diary, actigraphy, PSG, possibly MSLT |
Red Flags Beyond Tracker Data:
- Inability to sleep despite fatigue (chronic insomnia)
- Witnessed breathing pauses during sleep (apnea indicator)
- Excessive daytime sleepiness despite adequate sleep time (possible narcolepsy or hypersomnia)
- Acting out dreams (REM sleep behavior disorder)
- Uncomfortable leg sensations preventing sleep (restless legs syndrome)
Important Limitation: Consumer devices cannot rule out sleep disorders. Medical evaluation remains necessary for persistent concerns.
Beyond Tracking: Improving Sleep Quality
Evidence-Based Sleep Hygiene
Sleep hygiene encompasses behavioral and environmental practices that support quality sleep as validated by a comprehensive review of sleep hygiene evidence.
Core Sleep Hygiene Practices
| Practice | Evidence Level | Implementation | Expected Impact Timeline |
| Consistent Sleep Schedule | Strong evidence | Same wake time 7 days/week, bedtime within 30-minute window | 2-4 weeks for circadian stabilization |
| Light Exposure Timing | Strong evidence | Bright light in morning, dim lighting 2 hours before bed | 1-2 weeks |
| Caffeine Limitation | Strong evidence | No caffeine 8-10 hours before bedtime | Immediate (within 1-2 days) |
| Alcohol Avoidance Before Bed | Strong evidence | No alcohol 3-4 hours before sleep | Immediate |
| Exercise Timing | Moderate evidence | Regular exercise, but not within 2-3 hours of bedtime | 4-6 weeks for sleep improvements |
| Bedroom Environment | Moderate evidence | Cool (60-67°F), dark, quiet | Immediate |
National Institutes of Health guide to healthy sleep
Practices with Limited Evidence:
- Specific dietary restrictions (beyond caffeine/alcohol)
- Sleep supplements without medical guidance
- Particular sleep positions
- Weighted blankets (may help some individuals)
When Sleep Hygiene Alone Is Insufficient:
- If sleep problems predate poor sleep habits
- If practices followed consistently for 4-6 weeks without improvement
- If daytime impairment is significant
Medical evaluation indicated when behavior changes are insufficient.
Environmental Factors (Temperature, Light, Noise)
Sleep environment significantly affects sleep initiation and maintenance.
Temperature
| Factor | Optimal Range | Physiological Basis | Practical Adjustments |
| Bedroom Temperature | 60-67°F (15.6-19.4°C) | Core body temperature decreases during sleep | Thermostat adjustment, breathable bedding |
| Individual Variation | May vary ±3°F | Personal thermoregulation differences | Experimentation within range |
| Seasonal Adjustment | Lower in winter, cooling in summer | Humidity affects perceived temperature | Humidity control, appropriate bedding |
Light
| Light Exposure | Timing | Effect on Sleep | Management Strategy |
| Blue Light | Evening (2 hours before bed) | Suppresses melatonin, delays circadian rhythm | Dim screens, blue light filters, avoid screens |
| Bright Light | Morning | Advances circadian rhythm, promotes alertness | Outdoor exposure or light therapy box |
| Darkness | During sleep period | Supports melatonin production | Blackout curtains, eye mask |
| Night Lights | If needed for safety | Red/amber light less disruptive than white/blue | Red bulbs for night lights |
Noise
| Noise Level | Impact | Solutions | Evidence |
| >40 dB | May fragment sleep | Earplugs, white noise, address source | Studies show increased awakenings |
| Intermittent Noise | More disruptive than constant | White/pink noise masking | Consistent background sound may help |
| Individual Sensitivity | Varies significantly | Personal assessment needed | Adaptation occurs for some noise types |
Behavioral Factors (Timing, Routine, Caffeine)
Behavioral patterns strongly influence sleep quality.
Sleep Timing
| Factor | Recommendation | Rationale | Common Pitfalls |
| Wake Time Consistency | ±30 minutes, 7 days/week | Anchors circadian rhythm | Weekend sleep-in >2 hours causes social jet lag |
| Bedtime Window | Consistent 30-minute range | Trains sleep drive association | Going to bed only when sleepy (variable timing) |
| Time in Bed | Match sleep need (typically 7-9 hours opportunity) | Prevents low sleep efficiency | Excessive time in bed weakens sleep drive |
Pre-Sleep Routine
| Activity Type | Timing Before Bed | Effect on Sleep | Examples |
| Relaxing Activities | 30-60 minutes | Signals transition to sleep | Reading, gentle stretching, meditation |
| Screen Use | Avoid 1-2 hours | Blue light and mental stimulation | TV, phone, computer work |
| Stimulating Work | Avoid 1-2 hours | Arousal interferes with sleep onset | Problem-solving, arguments, intense exercise |
| Heavy Meals | Avoid 2-3 hours | Discomfort and metabolism disruption | Large dinners, spicy foods |
Caffeine Pharmacology
| Timeframe | Caffeine Action | Sleep Impact | Individual Variation |
| Half-life | 5-6 hours average | 50% remains in system | Slower metabolism in some individuals |
| Quarter-life | 10-12 hours | 25% still active | Evening coffee may affect sleep onset |
| Genetic Variation | CYP1A2 enzyme activity | Fast vs. slow metabolizers | Slow metabolizers more affected |
| Tolerance | Develops to alerting effects | Sleep disruption may persist despite tolerance | Chronic users may not notice impact |
Alcohol Effects
| Consumption Pattern | Sleep Onset | Sleep Architecture | Sleep Quality |
| Moderate (1-2 drinks) | May shorten latency | Suppresses REM sleep first half, REM rebound later | Fragmentation increases |
| Heavy (3+ drinks) | Sedation, faster onset | Significant REM suppression, increased N3 initially | Poor quality, frequent awakenings |
| Late Evening | Metabolism during sleep | Sleep disruption as alcohol clears | Awakenings 3-4 hours after consumption |
When Lifestyle Changes Aren’t Enough
Persistent sleep problems despite behavior modification require medical evaluation.
Indications for Medical Consultation
| Scenario | Duration Before Seeking Help | Possible Underlying Issues | Typical Evaluation Path |
| Insomnia Despite Sleep Hygiene | 4-6 weeks of consistent practice | Primary insomnia, anxiety, medical conditions | Clinical interview, sleep diary, possible CBT-I referral |
| Excessive Daytime Sleepiness | >2 weeks with adequate sleep opportunity | Sleep apnea, narcolepsy, insufficient sleep syndrome | Sleep history, PSG, possibly MSLT |
| Breathing-Related Sleep Disturbance | Any duration of concern | Obstructive/central sleep apnea | Sleep study (PSG or home sleep test) |
| Unusual Sleep Behaviors | Any occurrence | REM behavior disorder, sleepwalking, other parasomnias | PSG with video monitoring |
| Chronic Partial Sleep | Despite adequate time in bed | Circadian rhythm disorders, poor sleep efficiency | Actigraphy, sleep diary, melatonin timing assessment |
Medical Treatments May Include:
- Cognitive Behavioral Therapy for Insomnia (CBT-I): First-line treatment for chronic insomnia
- Positive Airway Pressure (PAP): Standard treatment for obstructive sleep apnea
- Medication: Short-term use for specific indications under medical supervision
- Light Therapy: For circadian rhythm disorders
- Dental Appliances: For mild-moderate sleep apnea
Important Principle: Sleep trackers may support behavior change but cannot replace medical diagnosis or treatment for sleep disorders.
Recovery and Readiness Monitoring
How Sleep Affects Recovery Metrics
Sleep quality influences multiple physiological recovery markers.
Sleep-Recovery Metric Relationships
| Recovery Metric | Sleep Impact | Physiological Mechanism | Tracker Application |
| Resting Heart Rate (RHR) | Elevated RHR after poor sleep | Sympathetic nervous system activation persists | Morning RHR trend tracking |
| Heart Rate Variability (HRV) | Reduced HRV after poor/insufficient sleep | Lower parasympathetic tone, incomplete recovery | Nocturnal and morning HRV |
| Readiness/Recovery Scores | Decreased scores with poor sleep | Composite of HRV, RHR, sleep metrics | Overall recovery assessment |
| Body Temperature | May remain slightly elevated | Incomplete metabolic recovery | Some devices track skin temperature |
Evidence Base:
- Individual baseline comparison more meaningful than population averages
- Studies demonstrate HRV reductions following sleep deprivation
- Resting heart rate increases are associated with insufficient recovery
HRV and Sleep Quality Connection
HRV during sleep reflects autonomic nervous system recovery.
Nocturnal HRV Patterns
| HRV Metric | During Good Sleep | During Poor Sleep | Recovery Indication |
| RMSSD (parasympathetic marker) | Elevated, especially during deep sleep | Reduced or suppressed | Higher = better parasympathetic recovery |
| Overall HRV | Increases across sleep period | Remains lower or decreases | Progressive increase indicates recovery |
| Morning HRV | Elevated from evening baseline | Lower than baseline | Post-sleep recovery status |
Factors Affecting Nocturnal HRV:
- Training Load: Excessive exercise may reduce sleep HRV
- Sleep Deprivation: Reduces HRV
- Alcohol: Suppresses HRV during and after consumption
- Stress: Chronic stress lowers nocturnal HRV
- Illness: Reduced HRV during infection/inflammation
Clinical Context:
- Persistent low HRV warrants medical evaluation if accompanied by symptoms
- HRV is one of many recovery markers
- Trends matter more than individual readings
Readiness Scores and Training Decisions
Readiness scores combine sleep, HRV, and other metrics to estimate recovery status.
Readiness Score Components (Typical)
| Input Metric | Weight in Score | What It Reflects | Consideration for Training |
| Previous Night Sleep | 30-40% | Immediate recovery status | Poor sleep may indicate reduced capacity |
| Sleep Consistency | 10-15% | Circadian rhythm stability | Irregular sleep affects performance |
| Resting Heart Rate | 15-25% | Cardiovascular recovery | Elevated RHR suggests incomplete recovery |
| HRV | 20-30% | Autonomic nervous system balance | Low HRV may indicate stress/fatigue |
| Activity Balance | 10-15% | Recent training load vs. recovery | Cumulative fatigue assessment |
Using Readiness for Training Decisions
| Readiness Level | Suggested Training Approach | Rationale | Caution |
| High (Green) | Normal or high-intensity training | Body signals adequate recovery | Don’t ignore subtle warning signs |
| Moderate (Yellow) | Moderate intensity or reduced volume | Partial recovery; avoid overreaching | Individual tolerance varies |
| Low (Red) | Active recovery or rest day | Incomplete recovery; injury/illness risk elevated | Consider context (life stress, illness) |
Important Limitations:
- Chronic low readiness warrants medical consultation
- Scores are algorithms, not medical assessments
- Individual response to training varies
- Psychological readiness and motivation also matter
Balancing Activity and Recovery
Sleep is one component of the activity-recovery relationship.
Activity-Recovery Balance Framework
| Component | Monitoring Metric | Imbalance Signs | Adjustment Strategy |
| Training Load | Weekly volume, intensity distribution | Persistent fatigue, declining performance | Reduce volume or intensity 20-30% |
| Sleep Quantity | Total sleep time trends | Chronic <7 hours in adults | Prioritize earlier bedtime |
| Sleep Quality | Efficiency, fragmentation | Consistently disrupted sleep | Address sleep hygiene, stress management |
| Rest Days | Frequency and quality | No improvement on rest days | Consider full deload week |
| Stress Load | HRV, subjective stress, readiness | Low HRV, high perceived stress | Stress management, possible training pause |
Overtraining Syndrome Indicators:
- Persistent performance decline despite training
- Chronic elevated resting heart rate
- Disturbed sleep (despite fatigue)
- Mood disturbances
- Increased illness susceptibility
Recovery Optimization:
- Stress management (sleep is affected by psychological stress)
- Adequate sleep is non-negotiable (most important recovery factor)
- Periodization: Structured training cycles with recovery weeks
- Nutrition timing and adequacy
When to Seek Medical Advice:
- Symptoms suggesting illness or injury
- Persistent fatigue despite reduced training
- Sleep disturbances lasting >2-3 weeks
- Unexplained performance decline
Choosing Sleep Tracking Approaches
Built-In Phone Apps vs. Wearable Devices
Different tracking approaches have distinct capabilities and limitations. Our independent evaluation is conducted without manufacturer funding or affiliate relationships.
Technology Comparison
| Tracking Method | Movement Detection | Heart Rate | Additional Sensors | Best Use Case |
| Phone Apps (Microphone/Accelerometer) | Bed movement (if phone on mattress) | Not measured | Snoring detection possible | Basic sleep duration, no physiological data |
| Smartwatches | Wrist movement (actigraphy) | Optical HR (PPG) | Some: SpO₂, skin temp | Continuous wear, integrated health tracking |
| Fitness Bands | Wrist movement | Optical HR | Limited | Budget-friendly multi-day battery |
| Smart Rings | Finger movement (very limited) | Optical HR (finger pulse) | Skin temperature | Discreet wear, minimal form factor |
| Bedside Devices | Ballistocardiography or radar | Non-contact HR detection | Respiratory rate, room environment | No device worn during sleep |
| Chest Straps | No movement (requires pairing) | ECG-grade HR | None (requires separate device) | High HR accuracy (not typically for sleep) |
Considerations
| Factor | Phone Apps | Wearables (Watch/Band) | Smart Rings | Bedside Devices |
| Cost | Free to low cost | $100-$500 | $250-$400 | $100-$400 |
| Comfort | No device worn | Some find wrist wear uncomfortable | Minimal awareness | Nothing worn |
| Accuracy | Movement only, limited | Moderate for sleep/wake, HR | Similar to wrist wearables | Variable by technology |
| Daytime Integration | None | Activity tracking included | Limited activity data | None |
| Battery Life | Phone battery dependent | 1-7 days typical | 4-7 days typical | Plugged in |
Selection Considerations:
- Most important factor: Will you actually wear/use it consistently?
- Prioritize comfort and wearability compliance
- Consider integration with other health tracking goals
- Accuracy differences between consumer devices are generally small
Wrist-Worn vs. Ring vs. Bedside Devices




Device form factor affects user experience and data quality.
Wrist-Worn Devices (Smartwatches, Fitness Bands)
Advantages:
- Established technology with extensive validation data
- Heart rate monitoring from wrist pulse
- Integration with exercise and activity tracking
- Large screen for data display (watches)
- Notification and smart features (watches)
Limitations:
- Some individuals find wrist wear uncomfortable during sleep
- May interfere with sleep for those sensitive to devices
- Optical HR accuracy may be reduced at wrist (vs. finger/chest)
- Daily charging may be required (smart watches)
Smart Rings
Advantages:
- Minimal form factor; less obtrusive than wrist devices
- Often better HR accuracy than wrist (finger pulse is stronger)
- Multi-day battery life (4-7 days typical)
- Sleep-focused design
Limitations:
- Limited exercise tracking (no GPS, small accelerometer)
- Finger swelling may affect fit and accuracy
- Smaller device = smaller battery (despite efficiency)
- More expensive than basic fitness bands
- Ring sizing critical; weight changes affect fit
Bedside/Non-Contact Devices
Advantages:
- Nothing worn; eliminates comfort concerns
- May also monitor room environment (temperature, humidity, air quality)
- Suitable for individuals who cannot tolerate wearables
Limitations:
- Accuracy varies significantly by technology
- May be affected by bedpartner movement
- Requires bedside placement and power
- Limited to sleep tracking only (no daytime data)
- Validation data often limited compared to wearables
Technology Types:
Acoustic: Analyzes sounds (snoring, breathing)
Ballistocardiography: Detects mattress movement from heartbeat and respiration
Radar/RF: Detects micro-movements for breathing and heart rate
When Not to Track Your Sleep
Sleep tracking is not appropriate for all individuals or situations.
Scenarios Where Tracking May Be Unhelpful or Harmful
| Situation | Why Tracking May Not Help | Better Alternative |
| Sleep Anxiety/Orthosomnia | Tracking reinforces obsession and performance anxiety | Focus on how you feel; consider CBT-I if insomnia present |
| Diagnosed Sleep Disorder Under Treatment | Consumer devices don’t measure treatment efficacy | Follow-up polysomnography or clinical sleep studies as recommended |
| Perfectionism/Compulsive Tendencies | Risk of fixation on scores | Behavior-focused approach without numerical feedback |
| Already Sleeping Well | No actionable information gained | Maintain good sleep habits without tracking |
| Wearing Device Disrupts Sleep | Tracking itself becomes sleep disruptor | Try different form factor or discontinue |
Warning Signs of Problematic Tracking:
- Checking sleep score immediately upon waking with anxiety
- Making major life decisions based on nightly scores
- Inability to sleep without tracking
- Dismissing how you feel in favor of device data
- Comparing scores obsessively with others
Healthy Approach:
- Take breaks from tracking if it causes stress
- Use tracking periodically (e.g., one week per month) rather than continuously
- Focus on weekly trends, not individual nights
- Prioritize subjective sleep quality and daytime function
Comparing Sleep Tracking Options
How to Use This Comparison Table
The table below compares sleep trackers across key categories. Focus on these decision factors:
For Beginners: Start with Budget Fitness Band or Basic Phone App. Test if tracking helps before investing more.
For Accuracy Priority: Smart Ring or Clinical-Grade Wearable options provide best measurement precision.
For Comfort: Smart Ring or Bedside Monitor eliminate wrist-wear discomfort.
For All-in-One: Premium Smartwatch combines sleep, activity, health, and notifications in one device.
💡 Editor’s Note: The “best” tracker is the one you’ll actually use consistently. A $50 device you wear nightly outperforms a $400 device sitting in your drawer.
Comprehensive Comparison Table
| Device Category | Examples | Movement | Heart Rate | SpO₂ | Temperature | Respiratory | Sleep Staging | Battery | Price Range | Best For |
| Basic Phone App | Sleep Cycle, Sleep as Android | Yes (if on bed) | No | No | No | Sound analysis | No (limited) | Phone battery | Free-$5 | Basic duration tracking, cost-conscious |
| Budget Fitness Band | Fitbit Inspire, Mi Band | Yes | Yes | No | No | No | Algorithm-based | 5-7 days | $50-$100 | Entry-level sleep + activity |
| Mid-Range Smartwatch | Fitbit Versa, Garmin Venu | Yes | Yes | Some models | Some models | Some models | Algorithm-based | 3-6 days | $150-$300 | Activity + sleep, notifications |
| Premium Smartwatch | Apple Watch, Garmin Fenix | Yes | Yes | Yes | Yes | Yes | Algorithm-based | 1-2 days | $300-$800+ | All-in-one health tracking |
| Smart Ring | Oura Ring, RingConn | Limited | Yes | Some models | Yes | Yes | Algorithm-based | 4-7 days | $250-$400 | Minimal form, sleep-focused |
| Bedside Monitor | Withings Sleep, Emfit QS | Bed movement | Yes (BCG) | No | Some models | Yes | Algorithm-based | Plugged in | $100-$400 | No-wear preference |
| Clinical-Grade Wearable | Actiwatch, Philips Actiwatch | Yes | Some models | No | No | No | Basic sleep/wake | Weeks | $500+ (prescription) | Clinical sleep research, prescribed monitoring |
Frequently Asked Questions About Sleep Tracking
How accurate are consumer sleep trackers?
Sleep/wake detection: 85-95% accurate. Sleep stage classification (light/deep/REM): 60-70% accurate. This is good enough for personal trend tracking but not for medical diagnosis. Focus on week-over-week patterns, not individual night precision.
Can I improve deep sleep with a tracker?
Trackers don’t improve sleep—your behavior changes do. They reveal patterns (e.g., alcohol reduces deep sleep by 30%, caffeine after 2pm cuts deep sleep). You act on the insights; the tracker just measures.
Which sleep tracker is most accurate?
Clinical-grade actigraphy devices (Actiwatch, Philips) are most accurate but require prescription and cost $500+. Among consumer devices, differences are small. Oura Ring and Whoop score slightly higher in studies, but Fitbit, Garmin, and Apple Watch are all within 5-10% of each other for basic metrics.
Do I need to wear it every night?
No. Wearing it 4-5 nights per week captures patterns adequately. Some users track 1 week per month to assess trends without obsessing. Consistency matters more than frequency—same nights each week is better than random nights.
Are smart rings better than watches for sleep tracking?
Slightly. Finger pulse detection is stronger than wrist, giving marginally better heart rate accuracy. Rings are more comfortable for many people. However, watches offer GPS, exercise tracking, and larger displays. Choose based on your priorities—comfort vs. features.
Can sleep trackers diagnose sleep apnea?
No. They can detect breathing irregularities and low blood oxygen that suggest sleep apnea, prompting medical evaluation. Only a medical sleep study (polysomnography) can diagnose sleep apnea. If your tracker shows frequent SpO₂ drops below 90% or irregular breathing, see a doctor.
Will tracking my sleep make me sleep worse?
It can, if you develop “orthosomnia”—obsessive tracking that increases sleep anxiety. Signs: checking your score immediately upon waking with anxiety, making decisions based solely on scores, inability to sleep without tracking. If this happens, take a break from tracking.
a clinically documented phenomenon called orthosomnia
What’s the best free sleep tracker?
Sleep Cycle (iOS/Android) or Sleep as Android are the most popular free options. They use your phone’s accelerometer and microphone to track movement and snoring. Limited compared to wearables (no heart rate or SpO₂), but adequate for basic sleep duration and consistency tracking.
How much should I spend on a sleep tracker?
Start free with a phone app. If you want heart rate and recovery metrics, $100-200 gets you capable devices (Fitbit Inspire, Garmin). Spend $300+ only if you want premium features (SpO₂, skin temperature, advanced analytics) or specific form factors (smart rings). Expensive doesn’t mean proportionally more accurate.
Can I use my sleep tracker data to diagnose myself?
No. Consumer trackers are for awareness and trend monitoring only—not diagnosis. Persistent sleep problems (chronic insomnia, suspected apnea, extreme fatigue) require medical evaluation. Use tracker data to have informed conversations with your doctor, not to replace medical assessment.
References
Centers for Disease Control and Prevention. Sleep and Sleep Disorders. https://www.cdc.gov/sleep/index.html. Accessed February 2026.
American Academy of Sleep Medicine. (2014). International Classification of Sleep Disorders, 3rd edition (ICSD-3). Darien, IL.
Hirshkowitz M, Whiton K, Albert SM, et al. National Sleep Foundation’s sleep time duration recommendations: methodology and results summary. Sleep Health. 2015;1(1):40-43.
de Zambotti M, Cellini N, Goldstone A, Colrain IM, Baker FC. Wearable sleep technology in clinical and research settings. Med Sci Sports Exerc. 2019;51(7):1538-1557.
Chinoy ED, Cuellar JA, Huwa KE, et al. Performance of seven consumer sleep-tracking devices compared with polysomnography. Sleep. 2021;44(5):zsaa291.
Perez-Pozuelo I, Zhai B, Palotti J, et al. The future of sleep health: a data-driven revolution in sleep science and medicine. NPJ Digit Med. 2020;3:42.
Baron KG, Abbott S, Jao N, Manalo N, Mullen R. Orthosomnia: Are some patients taking the quantified self too far? J Clin Sleep Med. 2017;13(2):351-354.
Irish LA, Kline CE, Gunn HE, Buysse DJ, Hall MH. The role of sleep hygiene in promoting public health: A review of empirical evidence. Sleep Med Rev. 2015;22:23-36.
Watson NF, Badr MS, Belenky G, et al. Recommended amount of sleep for a healthy adult: a joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep. 2015;38(6):843-844.
Roenneberg T, Allebrandt KV, Merrow M, Vetter C. Social jetlag and obesity. Curr Biol. 2012;22(10):939-943.
Walker MP. The role of slow wave sleep in memory processing. J Clin Sleep Med. 2009;5(2 Suppl):S20-S26.
Dijk DJ. Regulation and functional correlates of slow wave sleep. J Clin Sleep Med. 2009;5(2 Suppl):S6-S15.
Grandner MA, Jackson NJ, Pak VM, Gehrman PR. Sleep disturbance is associated with cardiovascular and metabolic disorders. J Sleep Res. 2012;21(4):427-433.
Mendelson M, Lyons OD, Yadollahi A, Inami T, Oh P, Bradley TD. Effects of exercise training on sleep apnoea in patients with coronary artery disease: a randomised trial. Eur Respir J. 2016;48(1):142-150.
National Heart, Lung, and Blood Institute. Your Guide to Healthy Sleep. NIH Publication No. 11-5271. 2011.
Medical Disclaimer
The information on Wearable Wellness Guide is for educational purposes and should not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis, treatment, or medical device recommendations tailored to your individual health needs.
- Last Updated: February 11, 2026
- Medical Review: Dr. Rishav Das, M.B.B.S. — February 11, 2026
- Medical Reviewer Credentials: Available on About page
This content has been medically reviewed according to the standards outlined on our About page. Dr. Rishav Das serves as Wellness Device Data Analyst and Consumer Device Accuracy Specialist for Wearable Wellness Guide.
