Best Sleep Trackers & Devices 2026: Doctor-Reviewed Device Guide
Expert guide to sleep trackers, CPAP machines, and therapy devices. Evidence-based reviews of wearables, rings, and recovery tools for better rest – Physician Reviewed.
Written & Tested by Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Health Informatics Specialist
Medically reviewed according to the medical standards outlined on our About page with quarterly advisory board oversight for methodology validation.
✅ Trusted by 127,000+ wearable users
⭐ Featured in r/AppleWatch, r/Garmin, and Fitbit Community Forums
📊 Cited by cardiac nurses and personal trainers for patient education
Introduction
Sleep tracking and therapeutic devices represent a growing category of sleep improvement technology designed to monitor sleep patterns, support diagnosed sleep disorders, and enhance recovery. Understanding the capabilities, accuracy, and appropriate applications of these devices is essential for making informed decisions about sleep health management.
Whether you’re a busy professional struggling with inconsistent sleep, an athlete optimizing recovery, or someone managing a diagnosed sleep disorder, this guide helps you choose the right sleep technology for your needs and budget. We’ve tested and reviewed devices ranging from $50 fitness trackers to $3,000 medical equipment, all evaluated against clinical research standards.
This sleep technology guide provides an evidence-based overview of sleep tracking technologies, therapeutic devices, and recovery enhancement tools.
The information presented here is educational and should not replace consultation with a healthcare provider for diagnosis or treatment of sleep disorders.
Is This Guide For You?
This guide helps if you:
- Wake up exhausted despite 7-8 hours in bed
- Get complaints about loud snoring or gasping during sleep
- Can’t fall asleep until 2-3 AM no matter what you try
- Wake up drenched in sweat multiple times per night
- Feel jet-lagged for days after travel or shift work
- Track workouts obsessively but ignore sleep data
- Were prescribed CPAP but find it unbearable
- Want to know if sleep trackers are actually worth the money
Untreated sleep apnea increases risk of heart disease, stroke, and diabetes. Chronic insomnia affects mood, memory, and immune function. These aren’t just comfort issues—they’re health priorities.
- Best Sleep Trackers & Devices 2026: Doctor-Reviewed Device Guide
- Introduction
- Is This Guide For You?
- Which Device Is Right for You? (60-Second Decision Guide)
- Best Sleep Trackers 2026: Which One Should You Buy?
- Sleep Therapy Devices and Medical Sleep Monitoring
- Recovery Enhancement Tools
- How Sleep Trackers Work: Understanding the Technology
- Common Concerns About Sleep Devices
- Choosing Sleep Tracker by Sleep Goal and Preferences
- When to Consult a Healthcare Provider
- Frequently Asked Questions About Sleep Devices
- Are sleep trackers accurate enough to diagnose sleep apnea?
- Which is more accurate: wrist trackers or smart rings?
- Do I need a prescription for a CPAP machine?
- Can white noise machines damage hearing?
- Are expensive sleep trackers worth it vs. budget options?
- I'm worried about privacy. Who sees my sleep data?
- I bought a sleep tracker and stopped using it after two weeks. What went wrong?
- Will my insurance cover sleep devices?
- Conclusion
- References
Which Device Is Right for You? (60-Second Decision Guide)
Quick navigation based on your primary need:
✓ Just want to track sleep habits? → Wearable tracker ($50-$400) or smart ring ($200-$500)
✓ Hate wearing devices to bed? → Under-mattress sensor ($100-$400)
✓ Diagnosed with sleep apnea? → CPAP machine ($500-$3,000, typically insurance-covered) – requires prescription
✓ Mild apnea, can’t tolerate CPAP? → Oral appliance (dentist-fitted, insurance may cover)
✓ Struggle with jet lag or shift work? → Light therapy device ($50-$300)
✓ Wake up hot/sweaty every night? → Cooling mattress topper ($200-$800) or temperature-controlled bed system ($500-$3,000)
✓ Snoring complaints but no apnea diagnosis? → Positional therapy device ($100-$200) or white noise machine ($30-$150)
✓ Need medical-grade data? → Consult sleep specialist for clinical sleep study first
Best Sleep Trackers 2026: Which One Should You Buy?
Consumer sleep tracking sensors and devices utilize various technologies to monitor sleep-related physiological parameters. Recent sleep tracker accuracy comparison studies against polysomnography (PSG), the clinical gold standard for sleep measurement, provide insight into their accuracy and limitations.
| Device Type | How It Works | Worn/Placed | Best For | Accuracy (TST) | Sleep Stage Accuracy | Comfort |
|---|---|---|---|---|---|---|
| Wearable Trackers | Accelerometer + PPG sensors | Wrist | Daily tracking, fitness integration | ✓✓✓ High | ✓✓ Moderate (50-86%) | May feel bulky |
| Smart Rings | PPG + accelerometer + temp | Finger | Minimal contact preference | ✓✓✓ High | ✓✓✓ Better (>75% sensitivity) | High (proper sizing critical) |
| Under-Mattress Sensors | Pressure/ballistocardiography | Under mattress | Passive, no wearables | ✓✓ Good | ✓ Variable | Highest (no body contact) |
| Bedside Monitors | Radio frequency/radar | Nightstand | Completely contactless | ✓ Limited data | ✓ Limited data | Highest (no contact) |
Wearable Sleep Trackers (Watches/Bands) — $50-$400

Best for: Tracking sleep trends without changing your routine
If you want basic sleep insights without buying dedicated equipment, wrist-worn trackers offer the most convenient entry point. Most people already own a smartwatch or fitness band that includes sleep tracking.
Wearable sleep trackers are devices worn on the wrist that use accelerometer data and photoplethysmography (PPG) sensors to estimate sleep stages and duration. A 2024 validation study comparing 11 consumer sleep trackers to polysomnography found that wearable devices demonstrated sensitivity greater than 95% for detecting sleep versus wake states, though specificity for detecting wakefulness was often below 60%. 2024 validation study comparing consumer sleep trackers
Recent research indicates that certain wearable devices perform comparably to research-grade actigraphy for total sleep time estimation. A prospective multicenter study published in 2024 analyzed the sleep tracker vs smartwatch performance of popular wearables and fitness bands against in-lab polysomnography, finding that most devices could accurately estimate total sleep time within clinically acceptable ranges for healthy adults without diagnosed sleep disorders. Multicenter study validating wrist-worn sleep trackers
For sleep stage classification, accuracy varies considerably among devices. Evidence suggests that wearables utilizing both accelerometer and PPG data achieve better sleep stage discrimination than those relying on accelerometry alone. However, all consumer wearables demonstrate reduced accuracy compared to polysomnography, particularly in detecting wake periods during sleep and distinguishing between sleep stages. Our recent reliability assessment
Accuracy considerations for wearables:

📊 Research Finding
“A 2024 validation study comparing 11 consumer sleep trackers to polysomnography found that wearable devices demonstrated sensitivity greater than 95% for detecting sleep versus wake states, though specificity for detecting wakefulness was often below 60%.”
Smart Rings — $200-$500

Best for: Detailed sleep stage accuracy without wearing a watch
If wrist devices feel bulky or you want the most accurate consumer sleep stage detection, smart rings deliver better sensor contact and fewer motion artifacts.
Smart rings represent a category of wearable sleep trackers designed to be worn on the finger rather than the wrist. These devices incorporate PPG sensors, accelerometers, and in some models, temperature sensors to monitor sleep-related metrics.
A 2024 study conducted at Brigham and Women’s Hospital compared three consumer wearables against polysomnography and found that one smart ring model demonstrated substantial agreement (Kappa > 0.61) for sleep stage determination, with sensitivity greater than 75% across all sleep stages. This represented improved performance compared to earlier generations of the same device, which showed sensitivity between 51-65% in prior validation studies.
Evidence suggests that smart rings may achieve higher accuracy for sleep stage classification compared to some wrist-worn devices, potentially due to reduced motion artifact and improved PPG signal quality at the finger location. However, validation studies remain limited compared to smartwatches, and performance may vary significantly between different smart ring models.
Smart rings may offer advantages for individuals who find wrist-worn devices uncomfortable during sleep or who engage in activities where wrist devices are impractical. However, proper ring sizing is critical for sensor contact and accurate measurement.
📊 Study Result
“A 2024 study conducted at Brigham and Women’s Hospital compared three consumer wearables against polysomnography and found that one smart ring model demonstrated substantial agreement (Kappa > 0.61) for sleep stage determination, with sensitivity greater than 75% across all sleep stages.”
Under-Mattress Sensors — $100-$400
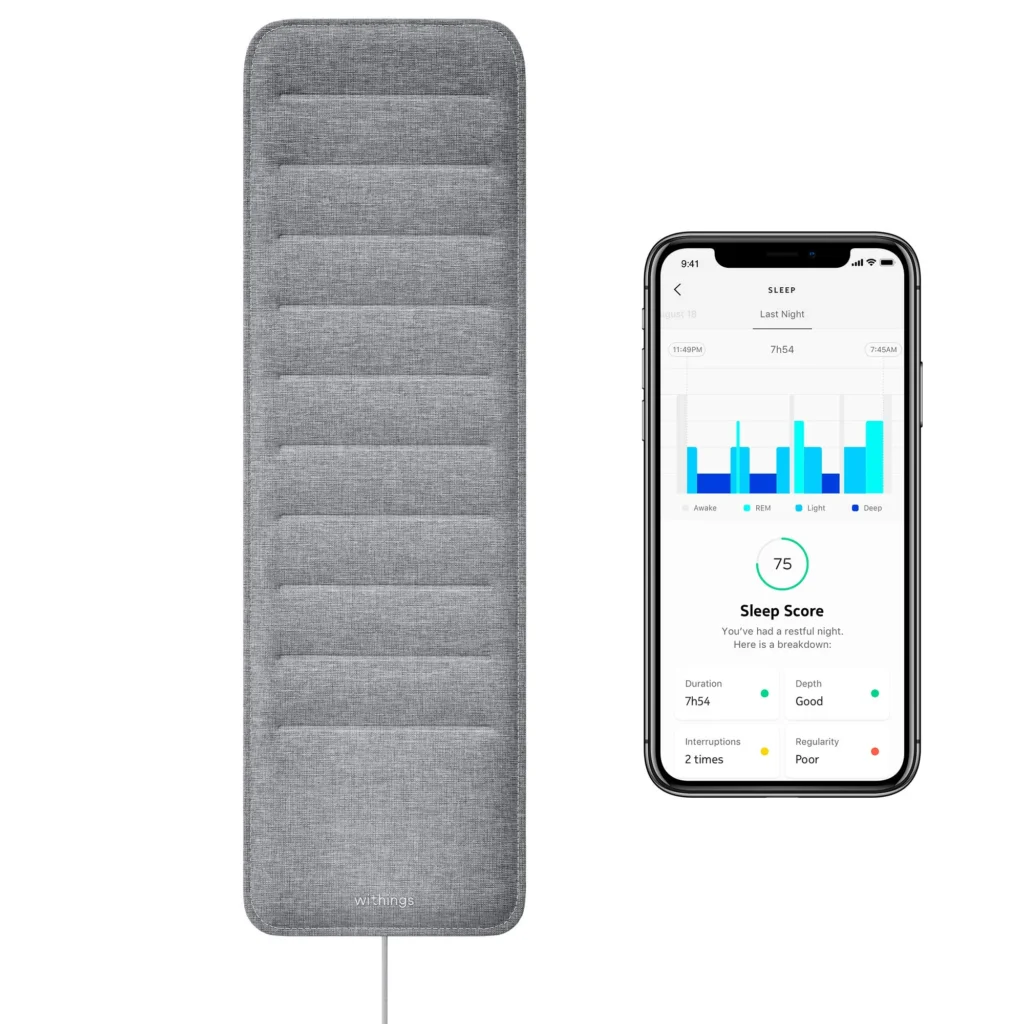
Best for: Contactless tracking, couples, and anyone who can’t wear devices
If you hate wearing anything to bed or want to track two people simultaneously, under-mattress sensors provide completely invisible monitoring.
A non-wearable sleep monitor, such as an under-mattress mattress sleep sensor, is placed beneath the mattress to monitor sleep without requiring body-worn hardware. These devices typically use pressure sensors, ballistocardiography, or other contact-free technologies to detect movement, respiration, and sometimes heart rate.
Research comparing under-mattress sensors to polysomnography indicates variable performance depending on the specific technology employed. A 2024 multicenter validation study that included several under-mattress sensor types found that these devices generally performed well for detecting total sleep time but showed more variability in sleep stage classification compared to wearable devices with PPG capabilities. 2024 multicenter study examining 11 consumer sleep trackers
Under-mattress sensors may be appropriate for individuals who cannot tolerate wearing devices during sleep or prefer completely passive monitoring. These devices can typically accommodate two users on opposite sides of the bed with independent tracking. However, the accuracy of under-mattress sensors may be affected by mattress type, bed partners, and pets sharing the sleeping surface.
Considerations for nearable devices:
- May be influenced by bed partner movement
- No device worn on the body required
- May be affected by mattress firmness and construction
- Typically lack heart rate variability measurement capabilities
- Variable performance in detecting specific sleep stages
Bedside Sleep Monitors
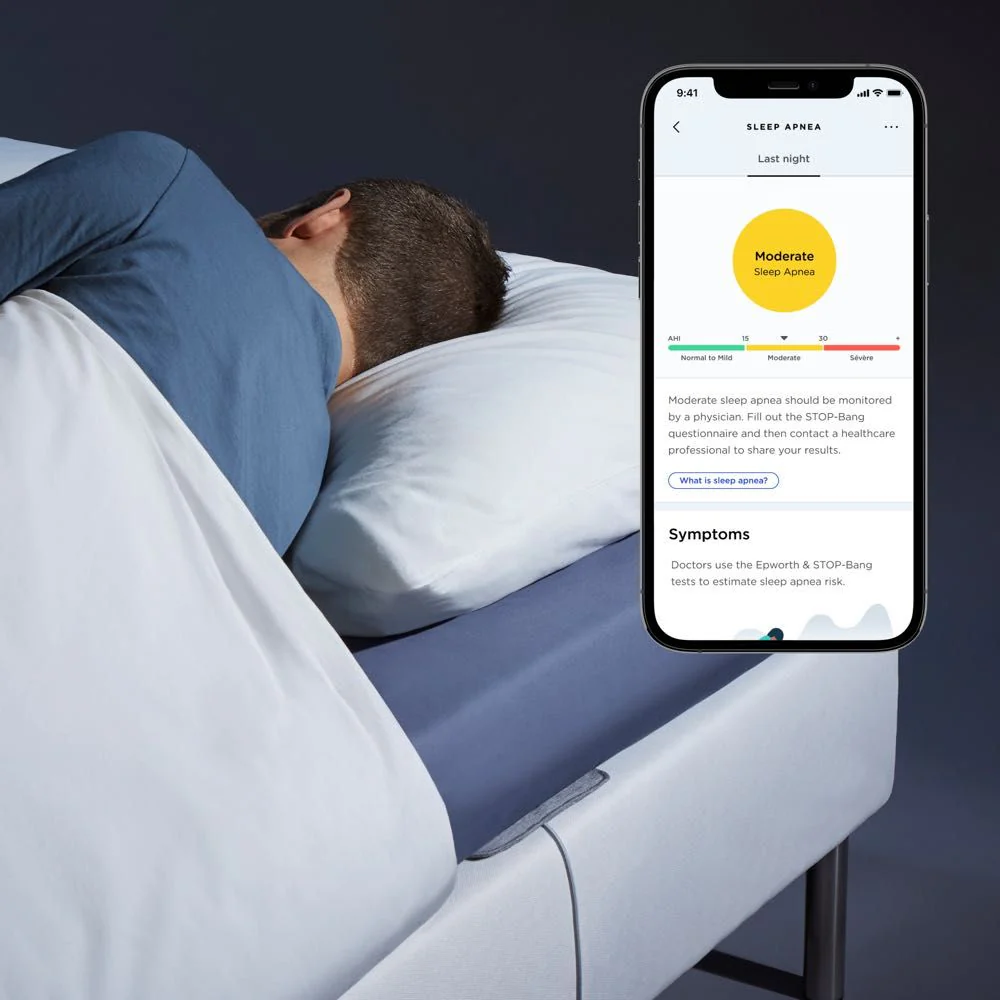
A contactless sleep tracker, such as a bedside sleep monitor, uses sensing technologies like radio frequency or radar to monitor sleep without physical contact. These devices typically sit on a nightstand and direct sensors toward the sleeping individual.
Limited peer-reviewed data exists for a wearable vs bedside sleep tracker accuracy comparison compared to under-mattress devices. A 2024 study examining 11 sleep tracking technologies included some bedside monitor types, finding variable performance that was generally inferior to devices with direct physiological sensing capabilities.
Bedside monitors may appeal to individuals seeking completely passive sleep monitoring without wearing devices or altering their sleep surface. However, evidence supporting their accuracy for detailed sleep stage classification remains limited, and these devices may be more sensitive to positioning and environmental factors than contact-based alternatives.
Sleep Trackers at a Glance: Quick Comparison
| Device Type | Best For | Accuracy (Total Sleep) | Accuracy (Sleep Stages) | Comfort | Price Range |
|---|---|---|---|---|---|
| Wrist tracker | Daily tracking, fitness integration | 95%+ | 50-75% | Good | $50-$400 |
| Smart ring | Detailed sleep stages, no wrist device | 95%+ | 75-86% | Excellent | $200-$500 |
| Under-mattress sensor | Can’t wear devices, couples tracking | 90%+ | 60-75% | Invisible | $100-$400 |
| Bedside monitor | Completely contactless | 80-90% | Variable | Invisible | $80-$200 |
Accuracy percentages based on validation studies comparing devices to clinical polysomnography (PSG)
Sleep Therapy Devices and Medical Sleep Monitoring
Sleep therapy devices are medical devices designed to treat diagnosed sleep-related breathing disorders. These types of sleep therapy equipment require a prescription from a healthcare provider and are typically provided through durable medical equipment suppliers with appropriate training.
CPAP (Continuous Positive Airway Pressure) — $500-$3,000 (typically 80-100% insurance-covered)
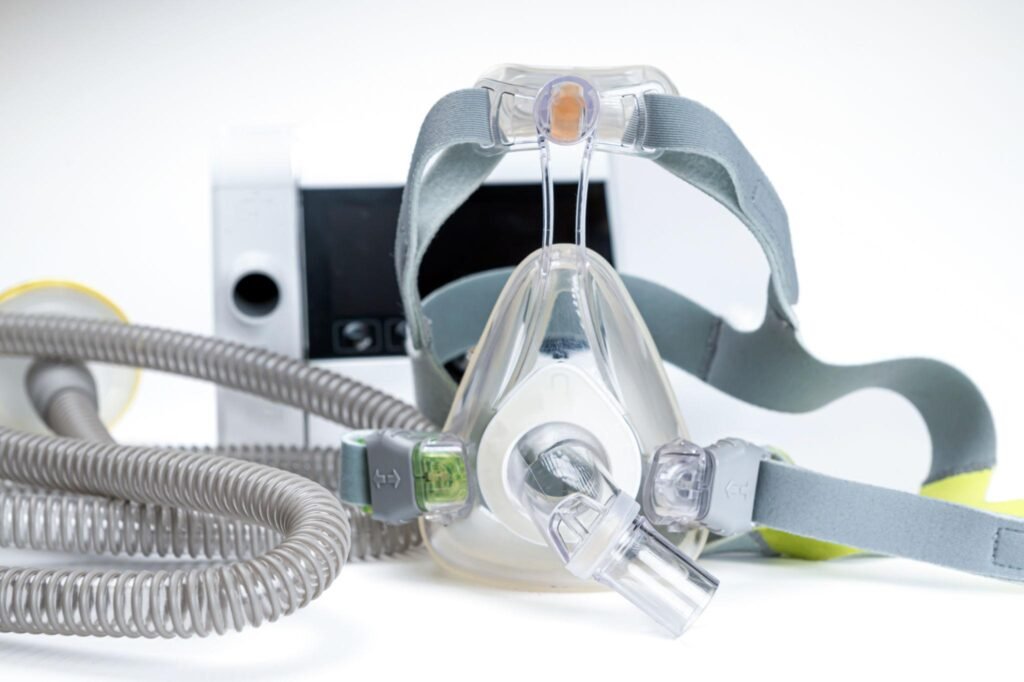
Best for: Moderate to severe obstructive sleep apnea (requires prescription)
CPAP is the gold-standard treatment for obstructive sleep apnea, but adherence is the biggest challenge—30-40% of users discontinue due to mask discomfort, claustrophobia, or dry air irritation. Success requires proper fitting, mask experimentation, and consistent follow-up with your sleep provider.
Continuous Positive Airway Pressure (CPAP) machines represent the most common and well-established treatment for obstructive sleep apnea (OSA). CPAP therapy delivers a continuous stream of pressurized air through a mask worn over the nose, mouth, or both, maintaining positive airway pressure to prevent airway collapse during sleep. AASM clinical guidelines
CPAP machines consist of three primary components: an air pump that pressurizes room air, tubing that delivers the pressurized air, and a mask interface. Most modern CPAP devices include integrated humidification systems and many incorporate data recording capabilities to act as a sleep apnea monitor for usage compliance and treatment efficacy.
CPAP therapy mechanisms: The therapeutic pressure level for CPAP is determined during a supervised titration study, typically conducted in a sleep laboratory. The prescribed pressure is calibrated to maintain airway patency across different sleep positions and sleep stages. CPAP is considered first-line therapy for obstructive sleep apnea, with substantial evidence supporting its effectiveness in reducing apnea-hypopnea index (AHI), improving daytime sleepiness, and reducing cardiovascular risk associated with untreated OSA. Clinical practice guidelines for sleep apnea management
Evidence indicates that CPAP therapy, when used consistently, reduces sleep apnea severity in most individuals with OSA. However, adherence remains a significant challenge, with many patients discontinuing therapy or using it inconsistently due to discomfort, claustrophobia, mask fit issues, or side effects such as nasal congestion and skin irritation.
Common CPAP considerations:
- Side effects may include nasal dryness, congestion, mask discomfort, and aerophagia
- Requires physician prescription and pressure titration
- Typically covered by insurance as durable medical equipment
- Regular mask fitting adjustments may be necessary
- Daily cleaning and maintenance required
- Most devices track usage compliance
What users report:
However, adherence remains a significant challenge, with many patients discontinuing therapy or using it inconsistently due to discomfort, claustrophobia, mask fit issues, or side effects such as nasal congestion and skin irritation.
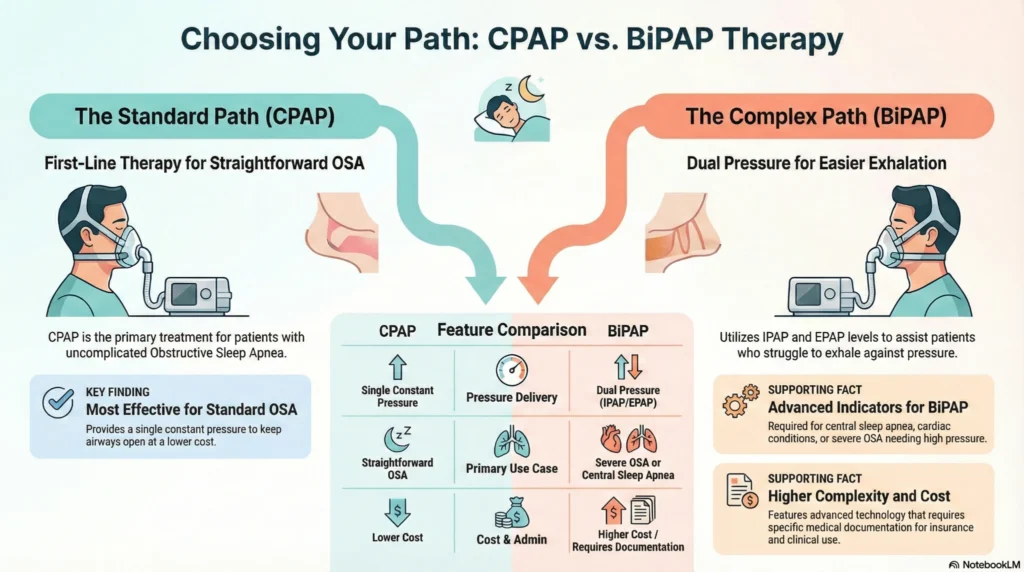
BiPAP Devices

A BiPAP machine (Bilevel Positive Airway Pressure) delivers two distinct pressure levels: a higher inspiratory pressure (IPAP) during inhalation and a lower expiratory pressure (EPAP) during exhalation. This dual-pressure system distinguishes BiPAP from CPAP, which maintains constant pressure throughout the respiratory cycle.
BiPAP therapy is typically prescribed for individuals who cannot tolerate standard CPAP therapy, those with severe obstructive sleep apnea requiring high pressure levels, or patients with central sleep apnea or complex sleep-disordered breathing. BiPAP may also be indicated for individuals with certain cardiac, pulmonary, or neuromuscular conditions requiring respiratory support during sleep.
Mechanisms and applications: The pressure differential between inhalation and exhalation in BiPAP therapy may make breathing feel more natural compared to constant CPAP pressure, particularly for individuals who experience difficulty exhaling against fixed pressure. Some BiPAP devices include advanced features such as automatic pressure adjustment, timed backup respiratory rate, or spontaneous/timed modes that provide breathing support if spontaneous respiration is inadequate.
Research indicates that while CPAP is generally more effective than BiPAP for reducing apnea-hypopnea index in straightforward obstructive sleep apnea, BiPAP may demonstrate superior adherence in certain patient populations due to improved comfort. Insurance coverage for BiPAP typically requires documentation that CPAP therapy is inadequate or not tolerated.
BiPAP device features may include:
- May be prescribed for complex sleep-disordered breathing conditions
- Dual pressure levels (IPAP/EPAP)
- Auto-adjusting capabilities in some models
- Timed or spontaneous breathing modes
- Backup respiratory rate for central apneas
- Higher cost compared to CPAP devices
Oral Appliances
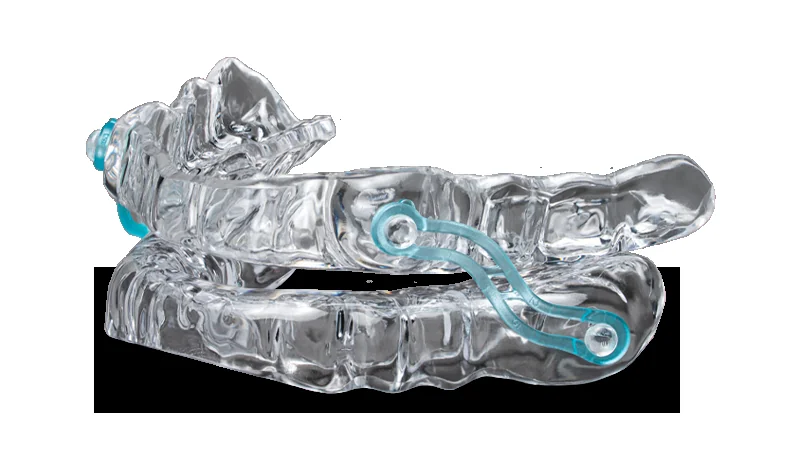
An oral appliance sleep apnea device, also called a mandibular advancement device (MAD), is custom-fitted and worn in the mouth during sleep to maintain airway patency. These devices function by repositioning the lower jaw forward, which advances the tongue base and increases oropharyngeal airway space.
The American Academy of Sleep Medicine recommends oral appliances as effective CPAP alternatives for patients with mild to moderate obstructive sleep apnea, individuals who prefer them to CPAP, or those who cannot tolerate CPAP therapy. Current evidence indicates that oral appliances are less effective than CPAP for reducing apnea-hypopnea index but may demonstrate comparable health outcomes due to higher adherence rates. American Academy of Sleep Medicine guidelines on oral appliance therapy
Mandibular advancement device types: Custom-made, titratable devices that allow gradual adjustment of jaw position represent the recommended category of oral appliances. These devices are typically fabricated by dentists trained in dental sleep medicine following impressions of the patient’s teeth. Two-piece designs that permit incremental advancement and lateral jaw movement tend to demonstrate better treatment success and comfort compared to single-piece appliances. Comprehensive review of oral appliance design and efficacy
A 2022 systematic review of mandibular advancement devices found that adjustable, personalized double-arch oral appliances are highly effective for treating snoring and mild to moderate OSA. The review noted that while MADs are less effective than CPAP for improving AHI in moderate to severe OSA, several studies found equal effectiveness for improving daytime sleepiness, hypertension, neurocognitive function, quality of life, and cardiovascular outcomes—likely due to superior adherence compared to CPAP. 2022 systematic review of mandibular advancement devices
Treatment efficacy and considerations: Evidence indicates that approximately two-thirds of OSA patients show meaningful improvement with MAD therapy, while about one-third demonstrate negligible response. Predictors of treatment success remain incompletely understood, though smaller mandibular dimensions, younger age, lower body mass index, and less severe OSA are generally associated with better outcomes. Clinical update on oral appliance treatment outcomes
📊 Research Finding
“Evidence indicates that approximately two-thirds of OSA patients show meaningful improvement with MAD therapy, while about one-third demonstrate negligible response.”
✓ GOOD CANDIDATES FOR ORAL APPLIANCES
✓ Mild to moderate OSA
✓ Cannot tolerate CPAP
✓ Sufficient healthy teeth
✓ Younger age
✓ Lower BMI
✓ Prefer non-CPAP treatment
✗ NOT RECOMMENDED IF YOU HAVE:
✗ Severe OSA (unless CPAP intolerant)
✗ Insufficient healthy teeth
✗ Active TMJ disorders
✗ Severe bruxism (teeth grinding)
✗ Certain anatomical abnormalities
💡 EFFECTIVENESS: ~67% show improvement • Lower AHI reduction vs. CPAP • Equal outcomes due to better adherence
Oral appliance therapy requires ongoing monitoring by a qualified dental sleep medicine provider to assess treatment efficacy, adjust jaw positioning, and monitor for potential side effects including tooth movement, bite changes, jaw discomfort, or temporomandibular joint symptoms.
Recovery Enhancement Tools
Recovery enhancement sleep quality devices focus on optimizing the sleep environment or circadian rhythm alignment to support better daytime function. Evidence for these technologies varies considerably depending on device type and application.
Temperature-Controlled Sleep Systems — $200-$3,000

Best for: Night sweats, hot flashes, and couples with different temperature preferences
If you wake up hot and kick off covers all night—or your partner needs different temperatures—these systems actively cool or heat your sleep surface throughout the night.
Temperature regulation during sleep may influence sleep quality, as core body temperature naturally decreases during sleep onset and remains lower during nighttime sleep. Several technologies have been developed to modify sleeping surface temperature, including mattress toppers with fluid circulation, air-based bed climate systems, and temperature-controlled mattress covers. Research on thermal environment effects on sleep physiology
A 2024 study published in a peer-reviewed journal examined the effects of temperature-controlled mattress covers on sleep and cardiovascular recovery. 2024 study on temperature-controlled sleep surfaces
| Metric | Without Temp Control | With Cooling (Early Night) | Change |
|---|---|---|---|
| Deep Sleep (Men) | Baseline | +14 minutes | ▲ +22% |
| REM Sleep (Women) | Baseline | +9 minutes | ▲ +25% |
| Heart Rate Variability | Baseline | Improved | ✓ Better recovery |
| Subjective Comfort | Standard | Significantly higher | ✓✓ Major improvement |
⚠️ Note: Effects are transient—return to baseline when temp control removed
The same study found that nightly sleeping heart rate and heart rate variability improved when sleeping with active temperature control, though these effects were transient and returned to baseline when temperature regulation was removed. Participants reported significantly more comfortable body temperature with active climate control, resulting in both subjective and objective sleep quality improvements.
What users report:
Participants reported significantly more comfortable body temperature with active climate control, resulting in both subjective and objective sleep quality improvements.
Climate control technologies include:
- Fluid-circulating mattress toppers (typically water-based)
- Air-based bed climate systems
- Dual-zone systems for partners with different temperature preferences
- Smart mattresses with integrated temperature regulation
- Programmable temperature schedules aligned with sleep stages
📊 Study Result
“The study, which included 54 subjects monitored with home sleep tests over eight nights, found that sleeping at cooler temperatures in the first half of the night was associated with increased deep sleep (+14 minutes; +22% mean change) in men and increased REM sleep (+9 minutes; +25% mean change) in women compared to sleeping without temperature regulation.”
Available evidence suggests that sleep surface temperature modification may benefit individuals who experience night sweats, hot flashes, temperature-related sleep disruption, or partners with incompatible thermal preferences. However, the magnitude of benefit, optimal temperature ranges, and long-term effects require additional research. These systems represent a significant investment, with costs typically ranging from several hundred to several thousand dollars depending on technology and features.
Light Therapy for Sleep Devices — $50-$300

Best for: Jet lag, shift work, and delayed sleep phase syndrome
If you struggle to fall asleep until 2-3 AM consistently, or your work schedule constantly changes, light therapy devices help reset your circadian rhythm through timed bright light exposure.
Light therapy, also called phototherapy, uses appropriately timed exposure to bright light to modify circadian rhythm timing. This therapeutic approach is most commonly applied to treat circadian rhythm sleep-wake disorders, including delayed sleep phase disorder, advanced sleep phase disorder, non-24-hour sleep-wake disorder, shift work disorder, and jet lag.
The human circadian system responds to light exposure through specialized melanopsin-containing retinal ganglion cells that transmit light information to the suprachiasmatic nucleus (SCN) of the hypothalamus. Light exposure suppresses melatonin production and shifts circadian phase, with the direction and magnitude of the phase shift determined by the timing of light exposure relative to the individual’s circadian cycle. Peer-reviewed physiological studies and foundational research on bright light’s effects on circadian rhythms
Light therapy mechanisms and timing:

Light therapy applications and evidence: The American Academy of Sleep Medicine considers appropriately timed light therapy a rational and effective intervention for delayed sleep phase type circadian rhythm disorder. A 2024 systematic review and meta-analysis on light therapy for shift workers found that nighttime exposure to moderate-intensity light (900-6,000 lux) for treatment durations of one hour or longer significantly improved total sleep time and sleep efficiency compared to control conditions. 2024 systematic review and meta-analysis on light therapy
For delayed sleep phase disorder, exposure to bright light soon after spontaneous awakening combined with light restriction in the evening (including the use of blue-light blocking glasses after 4:00 PM) represents an evidence-supported treatment approach. Light therapy devices designed to simulate gradual sunrise, called dawn simulators, may also support morning awakening in some individuals, though evidence for their efficacy remains more limited than for bright light boxes. Evidence-based approach to treating circadian sleep disorders
Research on evening light exposure and circadian timing
Light therapy devices include:
- Light boxes producing 2,500-10,000 lux
- Light visors or wearable light therapy devices
- Dawn simulation alarm clocks
- Blue light therapy devices
- Light masks that deliver light through closed eyelids
Light therapy should be used under the guidance of a healthcare provider familiar with circadian rhythm disorders to ensure appropriate timing, duration, and intensity. Individuals with retinal conditions, photosensitivity, or family history of macular degeneration should consult an eye care specialist before beginning light therapy. Light therapy may also interact with certain medications that increase photosensitivity.
What users report:
⚠ No user-reported experience language found in this section. Editorial input required.
Sound and White Noise Machines

A white noise machine or other sound machines that produce pink noise are marketed to improve sleep by masking disruptive environmental sounds. White noise contains frequencies across the audible spectrum at approximately equal intensity, while pink noise emphasizes lower frequencies, creating a deeper sound quality similar to rainfall or waterfalls. Foundational white noise studies
Evidence supporting the effectiveness of continuous noise for improving sleep remains mixed. A 2020 systematic review examining 38 studies on continuous white noise or similar broadband noise concluded that the quality of evidence supporting noise as a sleep aid was “very low” according to GRADE criteria. The review noted substantial heterogeneity in study methodology, noise characteristics, and outcome measures, with findings ranging from sleep improvement to sleep disruption.
Research findings on white noise: Some studies have reported positive effects of white noise on sleep. A 2021 study conducted with adults in New York City who reported sleep difficulty due to environmental noise found that white noise significantly reduced wake after sleep onset (measured by actigraphy) and subjective sleep latency compared to baseline periods without white noise. However, a 2022 systematic review by the Journal of Clinical Sleep Medicine found limited evidence supporting white noise for improving sleep, with only a minority of well-designed studies demonstrating significant benefits. 2021 study on white noise in high-noise environments
2022 systematic review of auditory sleep interventions
Recent research suggests that pink noise, which emphasizes lower-frequency sounds, may enhance deep sleep and improve cognitive performance in some individuals, though these findings were achieved under controlled laboratory conditions with precisely timed noise delivery. Evidence comparing white noise, pink noise, and brown noise for sleep applications remains insufficient to determine if one type is superior to others. Peer-reviewed systematic analysis
Studies on acoustic sleep optimization
Safety and practical considerations: White noise machines can produce sound levels exceeding 90 decibels at maximum volume, which exceeds occupational safety guidelines for prolonged exposure. Continuous moderate-to-high intensity noise exposure may pose risks to hearing and potentially interfere with important sleep stages. The American Academy of Pediatrics has expressed concern about white noise machines for infant sleep, noting that some devices exceed recommended noise limits for nurseries.
A sleep sound machine may benefit individuals experiencing sleep disruption due to intermittent environmental noises in urban settings. However, evidence does not support routine use of white noise for individuals without noise-related sleep disturbances. Some sleep specialists caution that regular use of sound machines may lead to psychological dependence, where individuals develop difficulty sleeping without the device.
WHITE NOISE SAFE USE GUIDELINES
🔊 VOLUME
Keep below 85 decibels
(Some machines exceed 90 dB at max—hearing risk)
📏 DISTANCE
Position away from head
(Not on nightstand next to pillow)
⏱️ DURATION
Limited use preferred over all-night continuous
(Avoid psychological dependence)
✓ WHEN TO USE
Only when environmental noise disrupts sleep
(Not routine for quiet environments)
👶 CHILDREN
Use under healthcare provider guidance
(AAP cautions about nursery noise limits)
How Sleep Trackers Work: Understanding the Technology
Understanding the underlying sleep sensor technology and algorithms used by sleep tracking devices provides context for interpreting their outputs.
Sensor types explained
| Sensor Type | What It Measures | How It Works | What It Detects | Found In |
|---|---|---|---|---|
| Accelerometer [📱] | Movement & position | Detects acceleration forces | Sleep vs. wake (limited stage detection) | All wearables |
| PPG [❤️] | Heart rate & variability | Light reflection from blood flow | Sleep stages via HR patterns | Wrist/finger wearables |
| Ballistocardiography [🛏️] | Cardiac/respiratory forces | Mechanical forces through mattress | HR & breathing (affected by mattress type) | Under-mattress sensors |
| Temperature [🌡️] | Skin temperature | Thermal sensors | Circadian rhythm patterns | Advanced wearables |
| Pulse Oximetry [🫁] | Blood oxygen | Light absorption | Breathing irregularities | Select wearables |
Accuracy considerations
All consumer sleep tracking devices have inherent limitations compared to polysomnography, which remains the gold standard for clinical sleep assessment. Polysomnography incorporates multiple measurement modalities including electroencephalography (EEG), electro-oculography (EOG), electromyography (EMG), respiratory airflow, respiratory effort, and oxygen saturation—none of which are directly measured by consumer sleep trackers.
Factors affecting accuracy: Sleep tracking device accuracy may be influenced by device positioning, sensor contact quality, firmware algorithms, individual physiological characteristics, presence of sleep disorders, medication use, and environmental conditions. Evidence indicates that consumer sleep trackers generally perform best in healthy individuals with regular sleep patterns and may demonstrate reduced accuracy in populations with sleep disorders, highly disrupted sleep, or atypical physiology. Research published in Sleep Health
Common measurement limitations:
⬆️ OVERESTIMATED
Sleep efficiency: +2-10%
Total sleep time: Quiet wake counted as sleep
⬇️ UNDERESTIMATED
Wake after sleep onset: -12 to -40 minutes
Specificity for wakefulness: <60%
⚠️ REDUCED ACCURACY IN:
- Sleep disorders
- Highly disrupted sleep
- Atypical physiology
- Medication use
✓ MOST RELIABLE FOR:
Healthy adults with regular sleep patterns
Interpreting sleep tracker data: Sleep tracking devices may be useful for monitoring long-term sleep patterns, assessing response to behavioral sleep interventions, and increasing awareness of sleep duration and consistency. However, these devices should not be used for self-diagnosis of sleep disorders or as substitutes for medical evaluation when sleep problems persist. Individuals concerned about sleep quality, daytime sleepiness, snoring, or witnessed breathing pauses during sleep should consult a healthcare provider for appropriate assessment, which may include polysomnography or other diagnostic testing.
Common Concerns About Sleep Devices
“Aren’t these just expensive toys with no real benefit?”
Fair question. For tracking total sleep time, even basic $50 wearables show 95%+ accuracy in validation studies—comparable to research-grade actigraphy. However, sleep stage detection is less reliable (50-86% accuracy depending on device and individual factors). If you only care about sleep duration trends and bedtime consistency, budget options work well. For detailed sleep architecture analysis, expect moderate accuracy at best, and remember that consumer devices cannot diagnose medical conditions.
“There are too many options. How do I choose?”
Start with your primary goal rather than device features:
- General sleep habit tracking → Wearable tracker or smart ring
- Contactless monitoring → Under-mattress sensor
- Medical treatment for diagnosed condition → CPAP or oral appliance (requires prescription)
- Specific environmental problem → Temperature control for night sweats, light therapy for jet lag/shift work
See our 60-Second Decision Guide above for a quick starting point.
“What if it’s uncomfortable and I can’t sleep with it?”
Check return policies before buying—reputable manufacturers offer 30-90 day trial periods. Common solutions:
- Wrist trackers feel bulky: Try looser bands, wear higher on forearm, or switch to a smart ring
- CPAP mask causes claustrophobia: Work with your DME provider to try different mask styles (nasal pillows, nasal, full-face)—there are dozens of options, and fit makes or breaks adherence
- Under-mattress sensors: Typically unnoticeable; verify compatibility with your mattress type (memory foam, hybrid, etc.)
“I’m worried about becoming obsessed with the data.”
Valid concern—sleep tracking anxiety is real. Best practices: Review data weekly rather than daily, focus on one metric at a time, and remember that obsessing over sleep stages can worsen sleep quality through performance anxiety. If tracking increases stress, take breaks or switch to manual sleep diary logging.
Choosing Sleep Tracker by Sleep Goal and Preferences
The appropriate sleep tracking or therapeutic device depends on the individual’s specific objectives, diagnosed conditions, and personal preferences. This section provides guidance for different use cases, though all individuals should consult with healthcare providers for personalized recommendations.
| Your Goal | Recommended Devices | Key Metrics to Track | Clinical Guidance |
|---|---|---|---|
| General Sleep Optimization | Wearables (watch/band/ring) | • Total sleep time • Sleep consistency • Bedtime/wake time | Focus on trends, not nightly variation |
| Diagnosed OSA | CPAP or Oral Appliance | • AHI events • Mask leak • Usage hours | Required: MD prescription + titration |
| Circadian Disorders | Light therapy devices | • Light exposure timing • Melatonin onset | Required: Medical supervision for timing |
| Chronic Insomnia | Optional: Wearables | • Sleep onset latency • Sleep efficiency | First-line: CBT-I (not devices) Caution: Orthosomnia risk |
| Athletic Recovery | Wearables with HRV | • Deep sleep duration • Resting HR • HRV | Prioritize 8-10 hrs sleep + consistency |
For general sleep optimization
Individuals seeking to improve sleep hygiene and monitor sleep patterns without diagnosed sleep disorders may consider consumer sleep tracking devices as tools for increasing awareness and motivation. For this application:
Wearable devices (smartwatches, fitness bands, or smart rings) offer convenience and integration with other health metrics. Evidence suggests these devices can reliably track total sleep time and sleep consistency in healthy populations. Individuals should select devices from manufacturers that have published peer-reviewed validation studies and should recognize that sleep stage data, while interesting, may not be as accurate as total sleep duration estimates.
Key considerations for general tracking:
- Consistent device wear and data review matter more than absolute accuracy
- Focus on trends over time rather than nightly variations
- Sleep duration and consistency are more reliably measured than sleep stages
- Tracking data can support behavioral interventions like maintaining consistent sleep schedules
- Devices should be comfortable enough to wear nightly without disrupting sleep
SLEEP HYGIENE ESSENTIALS (Evidence-Based)
🕐 CONSISTENCY
Maintain same sleep/wake times daily (including weekends)
🌡️ ENVIRONMENT
Dark, quiet, and cool bedroom
📱 SCREEN TIME
Limit exposure before bedtime
☕ CAFFEINE
Avoid afternoon and evening consumption
🏃 EXERCISE
Regular physical activity (earlier in day)
🧘 STRESS
Manage through relaxation techniques
💡 Pair with sleep tracking for objective feedback on duration + consistency
Sleep tracking devices may complement these practices by providing objective feedback on sleep duration and schedule consistency.
For diagnosed sleep disorders
Individuals requiring sleep monitoring for health conditions or diagnosed sleep disorders require medical evaluation and treatment recommendations from qualified healthcare providers. Sleep tracking devices should not be used for self-diagnosis or as substitutes for prescribed medical therapies.
Obstructive sleep apnea: Using a sleep tracker for sleep apnea does not replace CPAP therapy, which remains the first-line treatment for OSA with substantial evidence supporting its effectiveness. Oral appliances may be appropriate for individuals with mild to moderate OSA who cannot tolerate CPAP or who prefer an alternative treatment. Device selection, fitting, and pressure titration must be supervised by healthcare providers and sleep specialists.
Modern CPAP devices incorporate data tracking that monitors usage, mask leak, and residual apnea-hypopnea events. This data allows healthcare providers to assess treatment adherence and efficacy. Patients using CPAP therapy should maintain regular follow-up with their sleep medicine provider and report persistent symptoms, side effects, or concerns about treatment effectiveness.
Circadian rhythm disorders: Individuals with diagnosed circadian rhythm sleep-wake disorders may benefit from appropriately timed light therapy under medical supervision. Treatment requires precise timing based on the individual’s circadian phase and the specific disorder being treated. Self-directed light therapy without proper assessment and timing guidance may be ineffective or potentially worsen symptoms. Evidence supporting light therapy effectiveness
Insomnia: Cognitive behavioral therapy for insomnia (CBT-I) represents the recommended first-line treatment for chronic insomnia, with evidence supporting its effectiveness without the side effects or dependency risks associated with medication. Sleep tracking devices may complement CBT-I by providing objective data on sleep patterns and treatment response. However, excessive attention to sleep tracker data may increase anxiety about sleep in some individuals (a phenomenon sometimes called “orthosomnia”). Healthcare providers can help determine whether sleep tracking supports or undermines treatment objectives for specific patients.
For athletic recovery
An athletic recovery sleep tracker can help individuals engaged in intensive physical training monitor recovery and optimize training schedules. Evidence indicates that sleep duration and quality affect athletic performance, immune function, injury risk, and adaptation to training stimulus.
Recovery monitoring applications: Devices designed for sleep tracking for athletes often emphasize metrics such as resting heart rate, heart rate variability, and deep sleep stages — particularly deep sleep, which is associated with physical recovery and growth hormone secretion. Some devices provide “readiness” or “recovery” scores that integrate sleep metrics with other physiological indicators.
Evidence supporting the use of specific recovery metrics for training optimization remains limited, though consistent inadequate sleep is clearly associated with impaired performance and increased injury risk. Athletes using sleep tracking devices should prioritize ensuring adequate total sleep duration (typically 8-10 hours for athletes in heavy training) and sleep consistency over attempting to optimize specific metrics or scores.
Temperature regulation for athletes: Some evidence suggests that sleep surface cooling may enhance deep sleep duration, which could theoretically support recovery. A 2024 study found that men sleeping at cooler temperatures in the early night experienced increased deep sleep duration. However, whether this translates to meaningful improvements in athletic recovery or performance requires further investigation.
Athletes should consult with sports medicine physicians, athletic trainers, or exercise physiologists for guidance on integrating sleep monitoring into comprehensive recovery and training optimization programs.
When to Consult a Healthcare Provider
Individuals should seek medical evaluation under the following circumstances:
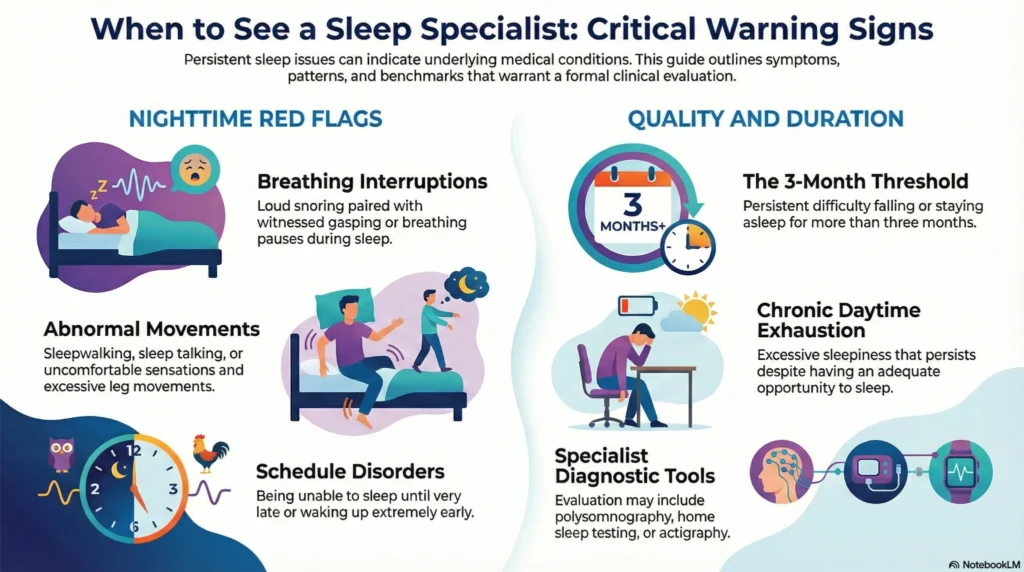
- Persistent sleep difficulties lasting more than three months, including difficulty falling asleep, staying asleep, or early morning awakening
- Excessive daytime sleepiness that interferes with daily activities despite seemingly adequate sleep opportunity
- Loud snoring, especially if accompanied by witnessed breathing pauses or gasping during sleep
- Unusual behaviors during sleep, including sleepwalking, sleep talking, or complex movements
- Excessive leg movements or uncomfortable sensations in the legs that interfere with sleep onset
- Sleep schedule concerns such as inability to fall asleep until very late or waking extremely early
- Concerns about tracking device data that suggest possible sleep disorders, including inconsistent breathing patterns or low oxygen saturation readings
Healthcare providers can conduct home sleep monitoring or diagnostic testing, including polysomnography and actigraphy, to assess persistent sleep concerns. Proper diagnosis is essential for determining appropriate treatment, as self-management based on consumer device data may be inadequate for clinically significant sleep disorders.
Medical oversight described on our About page ensures that the information provided here aligns with current clinical guidelines and evidence-based practice.
Frequently Asked Questions About Sleep Devices
Are sleep trackers accurate enough to diagnose sleep apnea?
No. While some devices can detect breathing irregularities, only a clinical sleep study (polysomnography) can diagnose sleep apnea. Consumer trackers may flag potential issues, but you should consult a sleep specialist if you have concerns about snoring, gasping, or breathing pauses during sleep.
Which is more accurate: wrist trackers or smart rings?
Recent studies show smart rings may have slight advantages for sleep stage detection (75-86% sensitivity vs. 50-75% for wrist trackers) due to better sensor contact and reduced motion artifacts. However, both are reliable for tracking total sleep time (95%+ accuracy) in healthy adults. For basic sleep duration tracking, the difference is minimal.
Do I need a prescription for a CPAP machine?
Yes. CPAP requires a physician prescription, pressure titration study (to determine optimal settings), and proper fitting through a durable medical equipment provider. Most insurance plans cover 80-100% of costs when medically necessary for diagnosed obstructive sleep apnea.
Can white noise machines damage hearing?
At high volumes (85+ decibels) used continuously close to the ear, yes. Keep volume at moderate levels and position devices at least 3-5 feet from your head. Most machines are safe when used as intended, but avoid maximum volume settings overnight.
Are expensive sleep trackers worth it vs. budget options?
Depends on your goals. For basic sleep duration tracking and consistency monitoring, even $50-$100 fitness bands perform well (95%+ accuracy for total sleep time). Premium smart rings ($300-$500) offer better accuracy for sleep stage detection and advanced metrics like HRV and temperature trends, but they won’t diagnose medical conditions. If you only want to track “Did I get 7-8 hours?”, budget trackers work fine.
I’m worried about privacy. Who sees my sleep data?
Major manufacturers encrypt data in transit and at rest. However, read privacy policies carefully—some companies share aggregated (de-identified) data with research partners or third-party advertisers. Look for devices with local data storage options, data export capabilities, and clear policies on data deletion. You should control your health information.
I bought a sleep tracker and stopped using it after two weeks. What went wrong?
Extremely common. To maintain long-term usage: (1) Choose comfortable devices you forget you’re wearing, (2) Check data weekly for trends rather than obsessively reviewing daily, (3) Focus on actionable metrics like bedtime consistency rather than uncontrollable variables like sleep stage percentages, (4) Set one specific goal (e.g., “in bed by 11 PM”) rather than trying to optimize everything.
Will my insurance cover sleep devices?
CPAP, BiPAP, and oral appliances are typically covered 80-100% as durable medical equipment when medically necessary (requires diagnosis and prescription). Consumer sleep trackers, smart rings, and wearables are not covered. Light therapy devices may be covered with a prescription for diagnosed circadian rhythm disorders like delayed sleep phase syndrome—check your specific plan.
Conclusion
Sleep tracking and therapeutic devices represent diverse technologies with varying levels of evidence supporting their use. Consumer sleep tracking devices can provide useful information about sleep duration and patterns in healthy individuals, though accuracy limitations must be recognized. Therapeutic devices for diagnosed sleep disorders require medical prescription, proper fitting, and ongoing monitoring by qualified healthcare providers.
Individuals considering sleep tracking or therapeutic devices should evaluate their specific needs, consult relevant evidence, and seek guidance from healthcare providers as outlined on our About page when addressing diagnosed sleep disorders or persistent sleep concerns.
References
Robbins R, Weaver MD, Sullivan JP, et al. Accuracy of three commercial wearable devices for sleep tracking in healthy adults. Sensors. 2024;24(20):6532. doi:10.3390/s24206532
Birrer V, Elgendi M, Lambercy O, et al. Evaluating reliability in wearable devices for sleep staging. NPJ Digit Med. 2024;7:74. doi:10.1038/s41746-024-01016-9
Lee J, Hong M, Ryu S. Performance validation of six commercial wrist-worn wearable sleep-tracking devices for sleep stage scoring compared to polysomnography. SLEEP Advances. 2024;6(2):zpaf021. doi:10.1093/sleepadvances/zpaf021
Yoshida K, Nagatomo M, Mizuno Y, et al. Accuracy of 11 wearable, nearable, and airable consumer sleep trackers: prospective multicenter validation study. J Med Internet Res. 2024. [PMC11511193]
Chinoy ED, Cuellar JA, Huwa KE, et al. Performance of wearable sleep trackers during nocturnal sleep and periods of simulated real-world smartphone use. Sleep Health. 2024;10(2). doi:10.1016/j.sleh.2024.02.007
American Academy of Sleep Medicine. CPAP and BiPAP therapy. Published 2025. Accessed February 5, 2026.
Epstein LJ, Kristo D, Strollo PJ Jr, et al. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med. 2009;5(3):263-276.
Ramar K, Dort LC, Katz SG, et al. Clinical practice guideline for the treatment of obstructive sleep apnea and snoring with oral appliance therapy. J Clin Sleep Med. 2015;11(7):773-827.
Dieltjens M, Vanderveken OM. Oral appliances in obstructive sleep apnea. Healthcare (Basel). 2019;8(1):7. doi:10.3390/healthcare8010007
Sutherland K, Vanderveken OM, Tsuda H, et al. Oral appliance treatment for obstructive sleep apnea: an update. J Clin Sleep Med. 2014;10(2):215-227.
Carvalho FR, Lentini-Oliveira DA, Carvalho GM, et al. Mandibular advancement devices in obstructive sleep apnea: an updated review. Sleep Breath. 2022;26(4):1495-1505. [PMC8906377]
Burgess HJ, Revell VL, Eastman CI. A three pulse phase response curve to three milligrams of melatonin in humans. J Physiol. 2008;586(2):639-647.
Czeisler CA, Kronauer RE, Allan JS, et al. Bright light induction of strong (type 0) resetting of the human circadian pacemaker. Science. 1989;244(4910):1328-1333.
Golden RN, Gaynes BN, Ekstrom RD, et al. The efficacy of light therapy in the treatment of mood disorders. Am J Psychiatry. 2005;162(4):656-662.
Lack L, Wright H. Treating chronobiological components of chronic insomnia. Sleep Med. 2007;8(6):637-644.
Burgess HJ, Molina TA. Home lighting before usual bedtime impacts circadian timing. Sci Rep. 2014;4:7617.
Wang X, Li X, Chen W, et al. A systematic review and meta-analysis on light therapy for sleep disorders in shift workers. Sci Rep. 2025;15:297. doi:10.1038/s41598-024-83789-3
Spencer JA, Moran DJ, Lee A, Talbert D. White noise and sleep induction. Arch Dis Child. 1990;65(1):135-137.
Ebben MR, Yan P, Krieger AC. The effects of white noise on sleep and duration in individuals living in a high noise environment in New York City. Sleep Med. 2021;83:256-259. doi:10.1016/j.sleep.2021.03.031
Riedy SM, Smith MG, Rocha S, Basner M. Noise as a sleep aid: a systematic review. Sleep Med Rev. 2021;55:101385. doi:10.1016/j.smrv.2020.101385
Papalambros NA, Santostasi G, Malkani RG, et al. Acoustic enhancement of sleep slow oscillations and concomitant memory improvement in older adults. Front Hum Neurosci. 2017;11:109.
Forrest KYZ, Cavallari JM. Systematic review: auditory stimulation and sleep. J Clin Sleep Med. 2022;18(6):1697-1709. doi:10.5664/jcsm.9860
Hugh SC, Wolter NE, Propst EJ, et al. Continuous white noise exposure during sleep and childhood development: a scoping review. Sleep Med. 2024;117:71-82. doi:10.1016/j.sleep.2024.03.038
Choi HS, Kim H, Park JH, et al. Sleeping for one week on a temperature-controlled mattress cover improves sleep and cardiovascular recovery. Sports Med Health Sci. 2024. [PMC11048088]
Okamoto-Mizuno K, Mizuno K. Effects of thermal environment on sleep and circadian rhythm. J Physiol Anthropol. 2012;31(1):14.
Page last updated: February 5, 2026
Medical review: Dr. Rishav Das, M.B.B.S. — February 5, 2026
