How to Choose the Best Heart Monitor: Match Devices to Your Health Goals
Find the right heart monitor for your health goals. Our 2026 physician-reviewed guide compares ECG smartwatches, chest straps, and BP monitors for clinical accuracy.
Written and medically reviewed by Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Specializing in clinical validation translation for wearables
Medical Review & Testing Standards
This guide reflects current clinical guidelines for heart health monitoring. All device categories and accuracy standards have been reviewed by Dr. Rishav Das, who evaluates each technology type against peer-reviewed research and FDA standards.
Introduction
From fitness enthusiasts tracking training intensity to individuals managing diagnosed heart conditions, heart monitoring devices serve vastly different purposes—and not all technologies are appropriate for every use case. This guide explains the distinct categories of heart monitoring devices, how each technology works, and which types align with specific health goals.
Who this guide is for: Whether you’re a 40-year-old athlete optimizing training zones, a 55-year-old managing blood pressure after your doctor’s recommendation, or a 65-year-old screening for atrial fibrillation, this guide translates medical-grade information into practical device choices. We explain medical terminology clearly—no cardiology degree required.
About device costs: Heart monitors range from $50 budget fitness bands to $1,000+ medical-grade systems. This guide helps you avoid wasting $50-150 on inaccurate devices while also identifying when a $400 smartwatch provides better value than pursuing a $1,000 medical device. Most readers find their ideal device in the $80-400 range.
What You’ll Learn
-
The 5 main categories of heart monitoring devices and their clinical purposes
-
How optical sensors, ECG electrodes, and Oscilometric technology differ
-
Which device types are appropriate for fitness tracking vs. medical monitoring
-
Realistic accuracy expectations for consumer vs. medical-grade devices
-
Key features to prioritize based on your specific health needs
⚡ QUICK NAVIGATION
(Skip ahead if you already know what you need)
Already decided on device type?
- Fitness tracking → Jump to chest straps & smartwatches comparison ↓
- Diagnosed AFib or irregular heartbeat → Jump to FDA-cleared ECG devices ↓
- Blood pressure monitoring → Jump to BP monitor recommendations ↓
- Sleep apnea screening → Jump to continuous SpO₂ devices ↓
Comparing specific brands?
Who This Guide Is For
-
Fitness enthusiasts seeking accurate heart rate data during exercise
-
Individuals with diagnosed cardiovascular conditions (hypertension, arrhythmia, heart failure)
-
People monitoring sleep quality and nighttime heart rate patterns
-
Those interested in ECG screening for atrial fibrillation detection
-
Anyone choosing between smartwatches, chest straps, or dedicated medical monitors
🏆 Top Picks by Primary Goal
If you only remember three things:
Best for Fitness & Training:
Polar H10 Chest Strap ($90) — Medical-grade accuracy (±1 bpm), works with all apps, no wrist-based limitations. Ideal for runners, cyclists, HIIT training.
Best FDA-Cleared ECG:
Apple Watch Series 10 ($399+) — FDA-cleared AFib detection, ECG in 30 seconds, continuous background rhythm monitoring. Requires iPhone.
Best Blood Pressure Monitor:
Omron Evolv ($80-100) — Upper arm design (more accurate than wrist), clinically validated, connects to smartphone, one-touch operation.
[See detailed comparison and alternatives below ↓]
⚠️ When to Seek Care
EMERGENCY (Call 911):
-
Heart rate >180 bpm or <40 bpm (awake)
-
Blood pressure >180/120 mmHg
-
SpO₂ ≤85% at rest
-
Chest pain, severe shortness of breath, fainting
NON-EMERGENCY (See physician):
-
Irregular rhythms, BP >140/90 consistently
-
SpO₂ <90% during sleep
-
Unexplained resting HR change >20 bpm
Consumer devices detect patterns—NOT diagnose. Physician review required.
To understand more about why you should proceed with acquiring a Wearable for heart health monitoring, check our
Comprehensive heart health monitoring guide.
5 Types of Heart Monitors: Which Device Is Best for Your Health Goals?
Heart monitoring technology spans five distinct categories, each designed for different measurement types and clinical purposes. Understanding these categories helps you choose devices that match your specific monitoring needs.
Best Smartwatches for Heart Rate Monitoring: Accuracy & Limitations Explained
Technology:
Functioning as a continuous heart rate monitor, PPG sensors measure blood volume changes in capillaries beneath the skin using LED light reflection.

What They Measure:
-
Continuous heart rate (24/7 tracking)
-
Heart rate during exercise (real-time zones)
-
Resting heart rate trends (daily averages)
-
Heart rate variability (HRV) in some models
-
Irregular rhythm notifications (not diagnostic)
Best For:
-
Use as a heart monitor for exercise training and general fitness tracking.
-
Daily heart rate trend monitoring
-
Sleep heart rate analysis
-
Detecting potential irregular rhythms for further medical evaluation
Medical Limitations:
-
Not FDA-cleared for diagnosing arrhythmias
-
Accuracy decreases during high-intensity exercise
-
Cannot replace prescribed medical monitoring
-
Limited clinical validation for specific populations (dark skin tones, tattoos)
Example Devices:
Apple Watch (Series 4+), Garmin Forerunner series, Fitbit Charge/Sense, Samsung Galaxy Watch
Limitations:
Tested under controlled conditions; results may differ by skin tone, movement, placement, and firmware. Clinical review of commercial wearable heart rate accuracy
⚠️ When to Upgrade to Medical-Grade:
If you have diagnosed atrial fibrillation, heart failure, or other cardiovascular conditions requiring clinical-grade monitoring, consult your cardiologist about FDA-cleared alternatives. See medical-grade ECG devices below.
FDA-Cleared ECG Devices for Atrial Fibrillation: Apple Watch vs KardiaMobile
Technology:
Electrocardiogram (ECG/EKG) sensors measure electrical activity of the heart using conductive electrodes. FDA-cleared devices must demonstrate clinical accuracy equivalent to medical equipment.
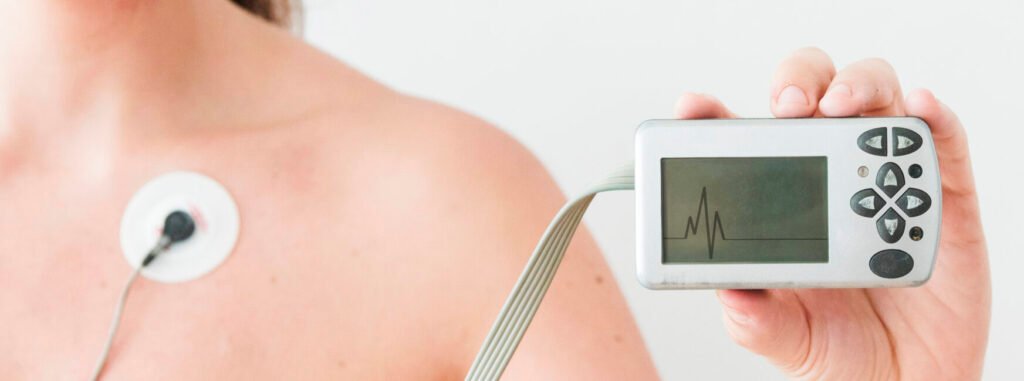
What They Measure:
-
Single-lead or multi-lead ECG waveforms
-
Heart rhythm patterns (detects AFib, bradycardia, tachycardia)
-
QRS complex, P wave, T wave morphology
-
Heart rate with medical-grade precision
Best For:
-
Individuals needing a heart monitor for irregular heartbeat patterns and diagnosed arrhythmias (AFib, PVCs, SVT).
-
Post-cardiac event monitoring (heart attack, ablation, pacemaker)
-
High-risk patients requiring an FDA approved heart monitor for home use
-
Documenting irregular rhythms for physician review
FDA Clearance Levels:
- 510(k) cleared: Equivalent to predicate medical device (most consumer ECG wearables)
- De Novo cleared: Novel technology with proven safety/efficacy (some advanced algorithms). FDA regulatory summary for ECG smartwatch features
Example Devices:
- Consumer-Wearable: Apple Watch (ECG app, FDA 510(k) cleared), Withings ScanWatch. FDA regulatory summary for ECG smartwatch features
- Dedicated Medical: KardiaMobile 6L, Omron Complete, Biobeat (multi-lead)
Limitations:
Tested on limited populations; accuracy varies by electrode placement, skin moisture, and individual physiology.
Medical Review Note:
FDA clearance means the device meets medical accuracy standards, but it does NOT replace professional diagnosis. All ECG readings showing abnormalities must be reviewed by a physician. Our testing methodology includes comparison against 12-lead clinical ECG.
Most Accurate Heart Rate Monitors: Chest Straps vs Smartwatches Compared
Technology:
A chest strap heart monitor uses direct electrical sensing (similar to ECG) via conductive electrodes in contact with chest skin.
What They Measure:
-
Beat-to-beat heart rate with medical-grade accuracy (±1 bpm)
-
Heart rate variability (R-R intervals)
-
Real-time heart rate zones during exercise
Best For:
-
Athletes requiring precise heart rate data for training (intervals, threshold workouts)
-
Cyclists, runners, and triathletes (where wrist movement affects optical accuracy)
-
HRV analysis for recovery monitoring
-
Individuals with wrist conditions preventing watch wear
Advantages Over Optical Sensors:
-
Superior accuracy during high-intensity intervals
-
No motion artifact interference
-
Faster response time to heart rate changes
-
More accurate HRV measurement
Disadvantages:
-
Requires chest strap (less comfortable than wrist wearables)
-
Not continuous 24/7 monitoring (worn during exercise only)
-
Requires periodic battery replacement or charging
-
Skin contact required (gel or moisture for conductivity)
Example Devices:
Polar H10, Garmin HRM-Pro Plus, Wahoo TICKR X, Suunto Smart Sensor
Limitations:
Requires consistent chest placement and skin moisture; accuracy may vary with strap fit and movement.
Accuracy Note:
Chest straps are considered the gold standard for the best heart rate monitor accuracy during exercise
Best Home Blood Pressure Monitors: Upper Arm vs Wrist (Doctor Recommended)
Technology:
Oscillometric measurement detects blood pressure by analyzing arterial wall oscillations during cuff inflation/deflation.


What They Measure:
-
Systolic blood pressure (SBP)
-
Diastolic blood pressure (DBP)
-
Pulse rate
-
Irregular heartbeat detection (some models)
Upper Arm Monitors (Recommended):
-
Gold standard for home blood pressure monitoring. AHA guidance on home blood pressure monitoring
-
Cuff placed at heart level (brachial artery)
-
FDA-validated accuracy when used correctly
-
Preferred by American Heart Association
Wrist Monitors (Convenience, Lower Accuracy):
-
Easier to use (portable, no upper arm access needed)
-
Less accurate due to wrist position sensitivity
-
Requires strict arm positioning at heart level
-
Not recommended for individuals with circulation issues
Best For:
-
Pre-hypertensive individuals tracking blood pressure trends
-
Individuals with diagnosed hypertension monitoring treatment
-
Post-cardiac event patients requiring home BP monitoring
-
Anyone advised by physician to monitor blood pressure
Limitations:
Upper arm cuff size must match arm circumference; wrist monitors require precise positioning at heart level.
Medical Standards Reference:
All blood pressure monitors should have FDA clearance or equivalent international validation (ESH, AAMI protocols). See our blood pressure monitor testing methodology for details on accuracy validation.
Critical Usage Guidance:
-
Upper arm monitors are clinically preferred over wrist models
-
Proper cuff size is essential (measure arm circumference)
-
Take readings at same time daily (morning preferred)
-
Avoid caffeine, exercise 30 minutes before measurement
-
Sit quietly for 5 minutes before taking reading. AHA guidance on home blood pressure monitoring
Example Devices:
- Upper Arm: Omron Evolv, Withings BPM Connect, iHealth Track
- Wrist: Omron Wrist BP Monitor, Beurer BC58
Pulse Oximeters (Finger vs. Wearable)
Technology:
Pulse oximetry measures blood oxygen saturation (SpO₂) using dual-wavelength light absorption (red and infrared) through tissue.
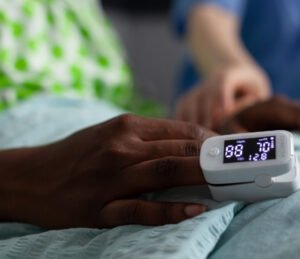


What They Measure:
-
Blood oxygen saturation (SpO₂ percentage)
-
Pulse rate
-
Perfusion index (some models)
Finger Pulse Oximeters (Medical-Grade):
-
FDA-cleared for medical accuracy
-
Spot-check measurements (not continuous)
-
Standard in clinical settings
-
Accuracy: ±2% SpO₂ typically. Clinical guidance on safe home pulse oximeter use
Wearable Pulse Oximeters (Smartwatches, Rings):
-
Continuous or on-demand SpO₂ tracking
-
Useful for sleep apnea screening (overnight trends)
-
Lower accuracy than medical finger devices
-
Not FDA-cleared for diagnostic use (most consumer models)
Best For:
- Sleep apnea monitoring (overnight SpO₂ drops)
- COPD or asthma management (tracking respiratory status)
- High-altitude exposure (altitude sickness risk)
- Post-COVID respiratory recovery monitoring
Medical Limitations:
- Consumer wearables are NOT diagnostic tools
- Accuracy decreases with poor perfusion (cold fingers, low blood flow)
- Dark nail polish, artificial nails interfere with readings
- Skin tone affects accuracy (darker skin may show lower readings)
Example Devices:
- Medical Finger: Nonin Onyx II, Masimo MightySat, Innovo Deluxe
- Wearable Consumer: Apple Watch (Series 6+), Garmin (select models), Oura Ring
Limitations:
Accuracy varies with skin tone, nail polish, finger temperature, and perfusion; wearables not validated for clinical decisions. Clinical guidance on safe home pulse oximeter use
Medical Review Note:
If you have diagnosed respiratory conditions or suspect sleep apnea, consult your physician before relying on consumer wearable SpO₂ data. Medical-grade finger oximeters are preferred for clinical decisions. Our SpO₂ testing methodology compares wearables to FDA-cleared medical devices. FDA safety communication: pulse oximeter accuracy and limitations
When to See a Doctor:
- Frequent overnight SpO₂ drops below 90%
- Excessive daytime sleepiness despite adequate sleep hours
- Loud snoring with breathing pauses
- Morning headaches or dry mouth
How Each Device Type Works
Understanding the underlying technology helps set realistic expectations for accuracy and appropriate use cases.
Optical Heart Rate Sensors (PPG)
Mechanism:
- Green LED lights illuminate skin surface
- Light absorbs into blood vessels (more absorption during pulse)
- Photodetector measures reflected light intensity
- Algorithm calculates heart rate from light variation patterns
Accuracy Factors:
- Skin contact quality (tight vs. loose band)
- Motion artifact during exercise
- Skin tone (melanin affects light absorption)
- Ambient light interference
- Tattoos or wrist hair
Limitations:
Tested on limited populations under controlled conditions; real-world accuracy varies by individual physiology and device placement.
Clinical Validation:
Consumer optical sensors show ±5-10 bpm error during exercise, improving to ±2-5 bpm at rest. Our testing data includes multi-activity validation. Clinical review of commercial wearable heart rate accuracy
Electrocardiogram (ECG) Technology
Mechanism:
- Skin contact electrodes detect electrical impulses from heart
- Signal amplification and noise filtering
- Algorithm analyzes waveform morphology
- Classification of rhythm (normal sinus, AFib, inconclusive)
Accuracy Factors:
- Electrode placement consistency
- Skin moisture and contact quality
- Body movement during recording
- Electrical interference (nearby devices)
Limitations:
Single-lead consumer ECG provides limited rhythm information compared to 12-lead clinical ECG.
FDA Clearance Standard:
Medical-grade ECG devices must demonstrate equivalence to predicate clinical ECG systems through controlled validation studies.
Oscillometric Blood Pressure Measurement
Mechanism:
- Cuff inflates above systolic pressure (occludes artery)
- Gradual deflation while monitoring arterial oscillations
- Peak oscillation = mean arterial pressure
- Algorithm calculates systolic and diastolic values
Accuracy Factors:
- Cuff size (too small → overestimate, too large → underestimate)
- Arm position (should be heart level)
- Body position (sitting, back supported, feet flat)
- Recent physical activity or stress
- Talking during measurement
Limitations:
Accuracy depends on proper cuff sizing, arm positioning, and adherence to measurement protocol.
Pulse Oximetry (SpO₂) Technology
Mechanism:
- Red and infrared LEDs emit light through tissue
- Oxygenated blood absorbs infrared light differently than deoxygenated blood
- Photodetector measures absorption ratio
- Algorithm calculates SpO₂ percentage
Accuracy Factors:
- Perfusion quality (blood flow to measurement site)
- Skin tone (melanin affects light absorption)
- Nail polish or artificial nails
- Motion artifact
- Cold extremities (vasoconstriction)
Limitations:
Tested primarily on lighter skin tones; accuracy may vary for darker skin pigmentation. FDA safety communication: pulse oximeter accuracy and limitations
⚠️ FDA Guidance on Skin Tone:
The FDA has issued safety communications about pulse oximeter accuracy differences across skin tones. Darker skin pigmentation may result in falsely elevated SpO₂ readings. See our diversity testing protocols. FDA safety communication: pulse oximeter accuracy and limitations
How to Choose a Heart Monitor: 4 Decision Factors Based on Your Health Condition
Different health goals and medical conditions require different device categories and features.
For General Fitness Tracking

📋 Medical Review Note:
If you have diagnosed heart conditions (even if mild), consult your cardiologist before beginning high-intensity training programs. Consumer fitness trackers are not designed to detect dangerous arrhythmias during exercise. See medical monitoring requirements below.
Primary Goal:
Optimize training intensity, track cardiovascular fitness trends, monitor recovery
Recommended Device Type:
Smartwatch with optical heart rate sensor OR chest strap for precision workouts
Key Features to Prioritize:
Continuous heart rate tracking (24/7)
Heart rate zone training support
VO₂ max estimation
Training load and recovery metrics
GPS integration for outdoor activities
Long battery life (5+ days for watches, 400+ hours for chest straps)
Accuracy Requirements:
For fitness tracking, ±5-10 bpm error during exercise is generally acceptable. Resting heart rate and trends matter more than beat-by-beat precision.
Best Devices for This Use:
Smartwatch: Garmin Forerunner 965, Apple Watch Series 10, Polar Vantage V3
Chest Strap: Polar H10, Garmin HRM-Pro Plus (for max accuracy during intervals)
Limitations: Consumer fitness trackers are for trend monitoring, not medical diagnosis; accuracy varies by activity intensity and individual factors.
For Diagnosed Heart Conditions

⚠️ REQUIRES PHYSICIAN APPROVAL
Device data supplements—NEVER replaces—prescribed monitoring.
Consult your cardiologist before using consumer devices.
⚠️ Critical Medical Guidance:
Consumer wearables supplement—but never replace—physician-directed monitoring for diagnosed cardiovascular disease. All abnormal readings should be reviewed by your cardiologist. Our medical review standards emphasize appropriate use limitation.
Primary Goal:
Monitor prescribed heart conditions, detect irregular rhythms, track treatment efficacy.
Recommended Device Type:
FDA-cleared ECG device OR medical-grade blood pressure monitor (depending on condition)
Condition-Specific Recommendations:
Atrial Fibrillation (AFib):
Device: Apple Watch ECG, KardiaMobile 6L, or physician-prescribed ambulatory monitor
Why: Single-lead ECG can detect AFib episodes for physician review
Limitation: Cannot replace Holter monitor or implanted loop recorder
Hypertension (High Blood Pressure):
Device: FDA-validated upper arm blood pressure monitor
Why: Home BP monitoring improves treatment adherence and control
Standard: Take 2 readings per day (morning and evening), track trends
Heart Failure:
Device: Consult cardiologist (may prescribe implantable hemodynamic monitor)
Consumer Option: Daily weight tracking + symptom logging (if approved by physician)
Limitation: Consumer wearables cannot measure ejection fraction or fluid status
Post-Heart Attack or Ablation:
Device: Physician-prescribed cardiac rehabilitation monitoring or remote telemetry
Consumer Supplement: ECG-enabled smartwatch for rhythm spot checks (with physician approval)
Limitations: Consumer devices provide screening data only; all abnormal findings require physician review and clinical confirmation.
For Sleep Apnea Monitoring
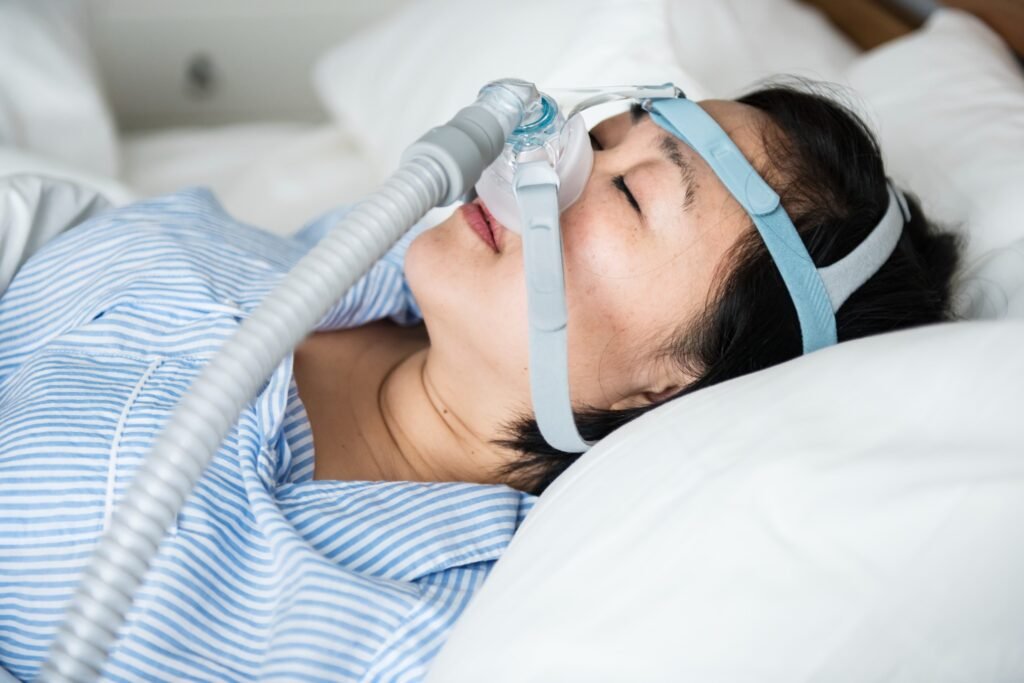
📋 Medical Standard:
Home sleep apnea testing (HSAT) devices prescribed by physicians are more comprehensive than consumer wearables. If you suspect sleep apnea (snoring, daytime fatigue, witnessed breathing pauses), seek formal diagnostic sleep study. Our sleep monitoring guide provides detailed testing protocols.
When to See a Doctor:
- Frequent overnight SpO₂ drops below 90%
- Excessive daytime sleepiness despite adequate sleep hours
- Loud snoring with breathing pauses
Morning headaches or dry mouth
Primary Goal:
Detect overnight oxygen desaturation events, track sleep-related respiratory disturbances
Recommended Device Type:
Wearable with continuous SpO₂ tracking OR dedicated sleep apnea screening device
Key Features to Prioritize:
Continuous overnight SpO₂ monitoring
Oxygen desaturation event detection (≥3% drop)
Sleep stage tracking (to correlate SpO₂ drops with sleep phases)
Respiratory rate estimation
Export data for physician review
Accuracy Requirements:
Medical-grade finger pulse oximeters are more accurate than wearable SpO₂ sensors, but wearables provide continuous overnight data that finger devices cannot.
Best Devices for This Use:
Wearable: Withings ScanWatch (medical-grade SpO₂), Garmin Fenix/Epix series
Dedicated: Wellue O2Ring (FDA-cleared overnight oximeter)
Limitations: Consumer wearables screen for patterns but do not diagnose sleep apnea; clinical sleep study required for diagnosis.
Device Decision Flowchart: Find Your Match in 60 Seconds
Device Decision Flowchart: Find Your Match in 60 Seconds
Choose your primary goal and follow the quick path to the right device.
Fitness Training & Performance
Do you do HIIT, running, cycling, or need fast HR response?
YES → Chest Strap
Most accurate heart rate (±1 bpm), instant response.
$70–140NO → Smartwatch
Good accuracy for general training and daily workouts.
$200–500Medical Heart Monitoring (ECG / Rhythm)
Diagnosed condition or doctor referral?
YES → FDA-Cleared ECG
Multi-lead, clinical-grade rhythm detection.
$80–150NO → Consumer ECG Smartwatch
Single-lead ECG for screening only.
$399–499Blood Pressure Monitoring
Upper-Arm BP Monitor (Always Choose)
Clinically validated upper-arm devices are the standard. Avoid wrist BP monitors and smartwatch BP (not yet accurate).
$80–150Sleep Apnea / SpO₂ Monitoring
Do you need continuous overnight tracking?
YES → Wearable SpO₂
Tracks overnight SpO₂ trends (not diagnostic).
$300–500NO → Finger Pulse Oximeter
More accurate single SpO₂ readings.
$50–300Accuracy Considerations
Understand how accurate are heart monitors and set realistic expectations for measurement precision across device categories.
Device Type |
Measurement |
Consumer Accuracy |
Medical-Grade Accuracy |
FDA Clearance |
|---|---|---|---|---|
Optical Smartwatch |
Heart Rate (rest) |
±2-5 bpm |
N/A |
Not required |
Optical Smartwatch |
Heart Rate (exercise) |
±5-15 bpm |
N/A |
Not required |
Chest Strap |
Heart Rate |
±1 bpm |
±1 bpm |
Not required |
Consumer ECG |
Rhythm Detection |
80-90% AFib sensitivity |
95%+ sensitivity |
510(k) required |
Medical ECG |
Rhythm Detection |
N/A |
98%+ sensitivity |
510(k) or De Novo |
Wrist BP Monitor |
Blood Pressure |
±5-10 mmHg |
N/A |
Some models |
Upper Arm BP Monitor |
Blood Pressure |
±3-5 mmHg |
±3 mmHg |
ESH/AAMI validated |
Wearable SpO₂ |
Oxygen Saturation |
±2-4% |
N/A |
Not required |
Finger Pulse Oximeter |
Oxygen Saturation |
±2% |
±2% |
FDA 510(k) |
Table Notes:
-
Accuracy ranges reflect real-world testing conditions, not ideal laboratory conditions
-
“Medical-Grade” refers to FDA-cleared or clinically validated devices
-
Consumer devices without FDA clearance are not approved for medical diagnosis
Limitations:
Tested under controlled conditions; individual results vary by skin tone, device placement, movement, and environmental factors. Clinical review of commercial wearable heart rate accuracy
📊 Testing Methodology Reference:
These accuracy ranges are based on our physician-supervised validation protocols, which compare consumer devices to medical reference equipment across diverse user populations. Learn more about our Testing Methodology.
Factors That Affect Measurement Accuracy
1
For ECG Devices:
Negatively Impact :
✗ Dry skin (poor electrical conductivity)
✗ Movement during recording
✗ Metal jewelry touching electrodes
To maintain accuracy :
✓ Moisturized skin (improves electrode contact)
✓ Still position during 30-second recording
✓ Consistent electrode placement
2
For Optical Heart Rate Sensors:
Negatively Impact :
✗ Loose wrist band (gap between sensor and skin)
✗ Vigorous arm movement during exercise
✗ Cold weather (vasoconstriction reduces blood flow)
✗ Wrist tattoos (ink blocks light penetration)
✗ Dark skin tone (may require algorithm adjustments)
To maintain accuracy :
✓ Snug fit 1-2 finger widths above wrist bone
✓ Clean, dry sensor surface
✓ Firmware updates (manufacturers improve algorithms)
3
For Blood Pressure Monitors:
Negatively Impact :
✗ Incorrect cuff size (measure arm circumference)
✗ Arm below heart level (falsely elevated reading)
✗ Talking or moving during measurement
✗ Recent caffeine or exercise (<30 minutes)
To maintain accuracy :
✓ Moisturized skin (improves electrode contact)
✓ Still position during 30-second recording
✓ Consistent electrode placement
4
For Pulse Oximeters:
Negatively Impact :
✗ Nail polish or artificial nails
✗ Cold fingers (poor blood flow)
✗ Excessive motion
To maintain accuracy :
✓ Warm hands (increase blood flow if needed)
✓ Remove nail polish before measurement
✓ Still finger position during reading
Limitations:
Accuracy affected by individual physiology, environmental conditions, and proper device use; follow manufacturer instructions.
📋 Medical Review Insight:
Understanding accuracy limitations prevents misinterpretation of readings. If device data conflicts with how you feel, trust your symptoms and consult your physician. Our testing reports document accuracy across varied real-world conditions. Learn more about our Medical Review Process
Common Purchase Concerns Answered
Before you buy, we answer the questions most readers ask:
🔒 Privacy: “Who sees my health data?”
Consumer wearables (Apple Watch, Garmin, Fitbit):
Your data, your control. All major brands encrypt heart rate, ECG, and activity data. Most offer local storage options that don’t require mandatory cloud sync.
- Apple Health: Data encrypted on-device, you control what’s shared with third-party apps
- Garmin Connect: Optional cloud sync, data exportable, can be deleted anytime
- Fitbit: Google-owned but data is not used for ads (per company policy)
Medical devices (prescribed monitors):
HIPAA-compliant when prescribed by a physician and used for medical purposes. Data shared with healthcare providers follows HIPAA protections.
Recommendation: If privacy is a concern, choose devices that work standalone without mandatory account creation (most blood pressure monitors, some chest straps).
📱 Compatibility: “Will it work with my phone?”
Quick Reference:
| Device Category | iPhone | Android | Works Standalone? |
|---|---|---|---|
| Apple Watch | ✅ Required (iOS 15+) | ❌ No | ❌ Phone required |
| Garmin devices | ✅ Yes | ✅ Yes | ⚠️ Limited features |
| Polar chest straps | ✅ Yes | ✅ Yes | ❌ Phone/watch required |
| Fitbit | ✅ Yes | ✅ Yes | ⚠️ Limited features |
| Blood pressure monitors (Omron, Withings) | ✅ Yes | ✅ Yes | ✅ Fully functional |
| KardiaMobile ECG | ✅ Yes | ✅ Yes | ❌ Phone required |
Important: Always check compatibility before purchase. Most manufacturers list requirements on product pages.
💰 Insurance/HSA: “Can I get reimbursed?”
HSA/FSA Eligible Devices:
Many heart monitors qualify for HSA/FSA reimbursement (pre-tax health savings):
- ✅ Blood pressure monitors (nearly always eligible)
- ✅ Pulse oximeters (eligible)
- ⚠️ Smartwatches (eligible only if prescribed by doctor for specific condition)
- ⚠️ Fitness trackers (generally not eligible)
Insurance Coverage:
Devices prescribed by your physician for diagnosed conditions may be partially covered by insurance:
- Blood pressure monitors: Often covered with hypertension diagnosis
- Home ECG devices: Sometimes covered with arrhythmia diagnosis (check your plan)
- Pulse oximeters: May be covered with sleep apnea or COPD diagnosis
What you need: Letter of Medical Necessity from your doctor. Ask: “Would a home monitoring device qualify for insurance coverage or HSA reimbursement for my condition?”
🤔 Validation: “Do I actually need to monitor, or is my doctor visit enough?”
Why home monitoring matters:
For blood pressure: Office readings capture one moment—often artificially high due to “white coat syndrome.” Home monitoring reveals patterns across mornings, evenings, stress, and medication timing. Studies show home BP monitoring improves hypertension control by 20% compared to office-only measurements.
For heart rate/rhythm: AFib is often intermittent. A 30-second ECG at your annual checkup might miss arrhythmias that occur weekly or monthly. Wearable monitoring over weeks/months catches events your doctor can’t see in the office.
For fitness: Resting heart rate trends predict cardiovascular fitness changes before you feel them. Heart rate variability (HRV) reveals overtraining or recovery needs.
Your doctor’s perspective: Most cardiologists welcome home monitoring data—it gives them more information to optimize your treatment. Some doctors now prescribe home monitoring for specific conditions.
When monitoring helps most:
- Newly diagnosed hypertension (finding right medication dose)
- Suspected intermittent arrhythmia (catching events)
- Medication changes (tracking response)
- Training for endurance events (preventing overtraining)
🔄 Returns & Warranties: “What if I choose the wrong device?”
Look for these purchase protections:
✅ 30-90 day return window — Essential for testing accuracy with your body. Skin tone, wrist size, and movement patterns affect device performance. You need time to evaluate.
✅ 1-year minimum warranty — Heart rate sensors can drift over time. Warranty coverage protects against accuracy degradation.
✅ Responsive customer support — Check reviews for support responsiveness. You’ll need help with setup, calibration, or troubleshooting.
✅ Firmware update history — Manufacturers improve accuracy via software updates. Active update history indicates ongoing support.
Red flags to avoid:
- ❌ No returns on opened devices (wearables must be tested worn)
- ❌ “Final sale” on health monitoring devices
- ❌ No warranty information provided
- ❌ No customer support contact visible
Pro tip: Buy from retailers with generous return policies (Amazon, REI, Apple) for first-time purchases. Return hassle is minimal compared to living with an inaccurate device.
What to Look for When Shopping
Key features and specifications to prioritize before you buy heart monitor online based on your monitoring needs.
Essential Features Checklist
For Fitness-Focused Heart Rate Monitors:
-
Continuous 24/7 heart rate tracking
-
Heart rate zone alerts (customizable thresholds)
-
HRV measurement (for recovery tracking)
-
VO₂ max estimation (cardio fitness trends)
-
Multi-sport mode support (running, cycling, swimming)
-
GPS integration (for pace/distance correlation)
-
Battery life: 5+ days (smartwatch) or 300+ hours (chest strap)
-
Water resistance: 5 ATM minimum (50m)
For Medical Heart Monitoring:
-
FDA 510(k) clearance or equivalent international validation
-
ECG waveform export (for physician review)
-
Irregular rhythm detection (AFib, bradycardia, tachycardia)
-
Data sharing with healthcare provider (PDF export, secure portal)
-
Medical disclaimer and usage instructions included
-
Clinical validation studies published (peer-reviewed)
For Blood Pressure Monitoring:
-
Upper arm cuff (preferred over wrist)
-
Cuff size range matches your arm circumference
-
FDA or ESH/AAMI validation
-
Irregular heartbeat detection
-
Memory storage (100+ readings)
-
Multi-user profiles (if shared device)
-
Average calculation (last 3 readings)
For Pulse Oximetry:
-
FDA clearance for medical use (if clinical decisions will be based on data)
-
Continuous overnight monitoring (for sleep apnea screening)
-
SpO₂ trend graphs (not just spot readings)
-
Low oxygen alerts (customizable threshold)
-
Perfusion index display (signal quality indicator)
Red Flags to Avoid
Marketing Claims That Should Raise Skepticism:
❌ “Diagnoses heart conditions” (only physicians diagnose)
❌ “Medical-grade accuracy” without FDA clearance
❌ “Replaces doctor visits” (devices supplement, not replace)
❌ “100% accurate” (no consumer device achieves perfect accuracy)
❌ “Detects all arrhythmias” (single-lead ECG has limitations)
Quality/Safety Concerns:
❌ No regulatory clearance in major markets (US FDA, EU CE, Health Canada)
❌ No published validation studies
❌ Vague accuracy claims (“clinically tested” without specifics)
❌ No medical disclaimers or usage warnings
❌ Suspiciously low price for “medical-grade” claims
Limitations:
Marketing claims may exceed validated performance; verify FDA clearance and published studies before purchase.
📋 Medical Review Note:
We test devices against their manufacturer claims and publish transparent accuracy data. See our product comparisons for head-to-head testing results. Learn more about our Medical Review Process
Budget Considerations: Investment Guide & Value Analysis
The real cost of choosing wrong: Buying an inaccurate $50 fitness tracker that your doctor dismisses wastes more than money—it wastes the 3-6 months you could have spent collecting useful health data. Meanwhile, a $400 FDA-cleared smartwatch costs less than two cardiology office visits and provides years of physician-trusted monitoring.
Value sweet spot—$150-400 devices:
Most readers get optimal value from mid-range devices because they offer:
- ✅ FDA clearance without prescription-device cost
- ✅ 3-5 year reliability (vs 1-2 years for budget models)
- ✅ Physician-trusted data that influences treatment decisions
- ✅ Lower cost than 2-3 specialist appointments
- ✅ Advanced features that prevent needing a second device later
Time savings: This 15-minute guide saves you 5-10 hours of comparing specs across retailer sites and prevents the frustration of returning incompatible devices or ones your doctor won’t trust.
[Existing price range content continues below…]
Entry-Level ($50-150):
- Basic optical heart rate tracking (fitness bands)
- Spot-check finger pulse oximeters
- Budget upper arm blood pressure monitors
Limitation: Lower sensor quality, fewer features
Mid-Range ($150-400):
- Smartwatches with validated heart rate algorithms
- FDA-cleared consumer ECG devices (KardiaMobile, Withings)
- Clinically validated blood pressure monitors
- Sweet spot for most users
Premium ($400-1000+):
- Advanced multisport smartwatches (Garmin, Apple Watch Ultra)
- Medical-grade multi-lead ECG devices
- Prescription remote cardiac monitoring
- Best for serious athletes or medical necessity
📊 Value Assessment:
Our heart monitor price comparison shows that higher price doesn’t always mean better accuracy.
Your First 30 Days: How to Use Your New Heart Monitor
You made a smart choice. Here’s how to get the most from your device:
Week 1: Setup & Baseline Establishment
Goals: Proper positioning, consistent measurement timing, identifying your baseline.
Action steps:
- Read the accuracy tips for your device type (review the “Factors That Affect Measurement Accuracy” section above)
- For blood pressure monitors: Take measurements at the same time daily (ideally morning, before coffee/medication)
- For smartwatches/chest straps: Wear consistently for 7 days to establish resting heart rate baseline
- For ECG devices: Take 2-3 readings while feeling normal to see what “normal” looks like for you
What’s normal in Week 1:
- Readings vary 5-10% daily (this is normal physiological variation)
- You’re still learning proper device positioning
- Smartwatch optical sensors may need 3-5 days to “learn” your skin/movement patterns
Week 2-3: Pattern Recognition Over Individual Readings
Goals: Stop fixating on single readings, start seeing trends.
Action steps:
- Focus on weekly averages, not daily spikes
- For blood pressure: Take 2-3 readings per session, average them, track the weekly average
- For heart rate: Note resting HR trend (should be consistent ±5 bpm)
- For ECG: Only take readings when you feel symptoms or weekly for baseline
What to watch for:
- ✅ Consistent trends (good—device is accurate)
- ⚠️ Erratic readings with no pattern (check device positioning, contact support)
- 🚨 Persistent abnormal readings (share with doctor, don’t just keep taking measurements)
Common mistake: Taking 10 blood pressure readings in a row because the first seemed “wrong.” This raises your BP from anxiety! Take 2-3 max, then wait an hour.
Week 4: Doctor Discussion Preparation
Goals: Present data your doctor will trust, get treatment adjustments if needed.
Action steps:
- Export or screenshot your trend data (most apps have “share report” function)
- Note any patterns: “BP spikes on Thursdays” or “HR elevated after medication change”
- Prepare specific questions: “My average BP is 135/85—should we adjust medication?” not “Is my device accurate?”
- Bring the device to your appointment if possible (doctor can verify positioning)
What to share with your doctor:
- ✅ Average readings over 2+ weeks
- ✅ Trends or patterns you’ve noticed
- ✅ Specific dates/times of concerning readings
- ✅ Screenshots of ECG tracings (if available)
What NOT to do:
- ❌ Bring 500 individual readings printed out
- ❌ Ask doctor to interpret every daily variation
- ❌ Expect doctor to troubleshoot device technical issues
Beyond Month 1: Sustained Monitoring Habits
For blood pressure:
- Continue daily readings if newly diagnosed or medication adjusting
- Reduce to 2-3x/week once stable (per doctor guidance)
- Always measure same time of day for comparability
For smartwatch ECG:
- Weekly baseline recordings when feeling normal
- Immediate recording during any symptoms (palpitations, dizziness)
- Don’t obsess—monthly is fine if asymptomatic
For fitness tracking:
- Let devices auto-track (no daily manual intervention needed)
- Review weekly summary reports, not daily details
- Note resting HR trends as fitness improves
For pulse oximetry:
- Use during illness (COVID, flu, respiratory symptoms)
- Nightly tracking only if screening for sleep apnea
- Not needed daily for most people
Troubleshooting: When to Contact Support vs Return
Contact device support if:
- Readings seem erratic despite correct positioning
- Device won’t sync or software issues
- Physical defects (strap breaks, screen issues)
Consider returning if:
- Device fundamentally doesn’t fit your body (cuff too small, watch too large)
- Lacks features you thought were included
- Incompatible with your phone (should have checked first!)
- Accuracy far worse than expected after 2-week trial
Give it a real try: Most devices need 7-14 days before you can judge accuracy fairly. Your body, skin tone, and movement patterns all affect readings.
Frequently Asked Questions
When comparing a heart monitor vs fitness tracker, what’s the difference between optical sensors and ECG?
Optical sensors (photoplethysmography/PPG) measure heart rate by detecting blood volume changes in capillaries using LED light reflection. They’re suitable for continuous fitness tracking and provide heart rate in beats per minute. ECG (electrocardiogram) measures the electrical activity of your heart using conductive electrodes, providing detailed rhythm analysis and waveform data. ECG is FDA-cleared for detecting arrhythmias like atrial fibrillation, while optical sensors are not diagnostic devices. See detailed technology comparison above.
Do I need a FDA-cleared heart monitor?
FDA clearance is essential if you’re monitoring a diagnosed cardiovascular condition (atrial fibrillation, hypertension, post-cardiac event) or making medical decisions based on device data. For general fitness tracking—monitoring training zones, tracking resting heart rate trends, or optimizing recovery—FDA clearance is not required, though validated accuracy is still important. Consult your cardiologist if you have diagnosed heart disease. Learn about FDA clearance standards.
Are chest strap heart monitors more accurate than smartwatches?
Yes, chest straps using direct electrical sensing achieve ±1 bpm accuracy, outperforming optical wrist sensors (±5-15 bpm during exercise). Chest straps are immune to motion artifact and provide faster response to heart rate changes, making them the gold standard for interval training and HRV analysis. However, smartwatches offer 24/7 continuous tracking that chest straps (worn during exercise only) cannot provide. See accuracy comparison table.
Can smartwatches detect heart attacks?
No. Consumer smartwatches cannot detect heart attacks (myocardial infarction). Symptoms like chest pain, shortness of breath, arm pain, or sudden severe fatigue require immediate emergency medical attention—call 911. Some smartwatches with ECG can detect irregular rhythms like atrial fibrillation, which increases stroke risk but is not a heart attack. Never rely on wearable devices for emergency cardiac symptoms. Read our medical limitations disclaimer.
How accurate are wrist blood pressure monitors?
Wrist blood pressure monitors are less accurate than upper arm monitors due to position sensitivity and distance from the brachial artery. Clinical guidelines from the American Heart Association recommend upper arm monitors as the gold standard for home blood pressure measurement. Wrist monitors require strict arm positioning at heart level and are not recommended for individuals with arterial stiffness or circulation issues. See blood pressure device comparison.
What heart rate accuracy is good enough for training?
For general fitness tracking, ±5 bpm accuracy is acceptable. For serious athletes doing interval training or threshold workouts, ±2 bpm accuracy (achievable with chest straps) is preferred. The most important factor is consistency—tracking trends and relative changes matters more than absolute precision. Resting heart rate accuracy should be ±2 bpm for meaningful trend analysis. Review our fitness accuracy standards.
Can I use consumer wearables if I have a pacemaker or ICD?
Consult your cardiologist before using any consumer heart monitoring device if you have an implanted cardiac device (pacemaker, ICD, loop recorder). Some wearables may interfere with device function or provide inaccurate readings. Your cardiologist may recommend specific FDA-cleared monitoring tools compatible with your implant. Never rely on consumer wearables as a substitute for prescribed cardiac device monitoring. See medical device safety guidelines.
Are chest straps more accurate than smartwatches for runners?
Yes, significantly. Chest straps (Polar H10, Garmin HRM-Pro) are accurate to ±1 bpm even during high-intensity intervals, while wrist-based optical sensors can show 10-20 bpm errors during activities with wrist movement (running, rowing, weightlifting). If you’re training with specific heart rate zones, chest straps are essential. For casual fitness tracking, smartwatches are adequate.
Is the Apple Watch accurate enough to replace a prescribed heart monitor?
No. The Apple Watch ECG is FDA-cleared for screening and informing your doctor, but it’s not a replacement for prescribed monitoring devices like Holter monitors (continuous 24-48 hour ECG) or ambulatory blood pressure monitors. However, Apple Watch data can supplement prescribed monitoring and help your doctor decide if more intensive monitoring is needed. Always ask your cardiologist: “Can I use my Apple Watch data alongside my prescribed monitoring?
Which heart rate monitor is most accurate: Garmin, Polar, or Fitbit?
For chest straps: Polar H10 is considered the gold standard (±1 bpm accuracy, validated against medical ECG). Garmin HRM-Pro is nearly equivalent.
For wrist-based: Garmin’s Forerunner/Fenix series with Elevate sensor typically edges out Fitbit in third-party testing, with Apple Watch Series 9/10 performing best for irregular rhythm detection. However, accuracy varies by individual—skin tone, wrist size, and tattoo presence affect all optical sensors. For critical accuracy, choose chest straps regardless of brand.
Can my employer or insurance company access my heart rate data from my smartwatch?
Not without your explicit consent. Consumer wearables (Apple Watch, Garmin, Fitbit) are governed by company privacy policies, not HIPAA, but they cannot share your data without your permission. Some employers offer wellness program incentives for sharing activity data—this is always optional. Insurance companies cannot access your data unless you voluntarily connect your device to their wellness app.
Exception: If a device is prescribed by a doctor and integrated into your medical record, that data follows HIPAA rules and could be in your health record accessible to providers.
Do I need to buy a new blood pressure monitor every few years?
No, but you should validate accuracy annually. Blood pressure monitors don’t expire, but the cuff can wear out and the sensor can drift. Bring your home monitor to your doctor appointment once a year and take a reading immediately after the doctor takes one—compare the results. If they differ by more than 5-10 mmHg consistently, consider recalibration (some models) or replacement. Most quality monitors (Omron, Withings) last 5-7 years with proper care
Are cheap $30 fitness trackers accurate enough for heart rate?
For resting heart rate, yes—usually within 3-5 bpm. For exercise heart rate, no—budget trackers often show 15-30 bpm errors during activity due to lower-quality optical sensors. Budget trackers are fine for step counting and sleep tracking, but not reliable for training zones or medical monitoring. If heart rate accuracy matters, spend at least $150 for a reputable brand (Garmin, Polar, Fitbit) or buy a $70 chest strap.
Should I get a smartwatch with ECG even if I don’t have heart problems?
It depends on your age and risk factors. ECG features are most valuable for people over 50, those with family history of AFib, or anyone with symptoms like palpitations. If you’re young (under 40), healthy, and have no symptoms or family history, the ECG feature may never get used—you’re paying for a feature you don’t need. However, Apple Watch and Samsung Galaxy Watch ECG detection has caught asymptomatic AFib in many users who then received treatment. If budget allows, it’s reasonable peace of mind for anyone over 40.
Can I trust my wrist blood pressure monitor readings?
Wrist monitors are less accurate than upper arm monitors, but they’re not useless. The challenge: small positioning errors at the wrist (not at heart level, bent wrist, tight watch band) cause large reading errors. Studies show wrist monitors can differ from upper arm readings by 10-20 mmHg.
Our recommendation: Only use wrist monitors if you cannot use an upper arm monitor (very large arm, severe pain). If you do use a wrist monitor, follow positioning instructions exactly and validate against a clinic reading
How do I know if my device’s readings are accurate?
For heart rate: Compare your device to your manual pulse count. Count your pulse for 30 seconds (at your wrist or neck), multiply by 2. Your device should be within 2-3 bpm. For chest straps, accuracy should be ±1 bpm.
For blood pressure: Bring your device to your doctor appointment, take a reading immediately after the nurse takes one. Readings should be within 5 mmHg for systolic and 3 mmHg for diastolic.
For ECG: You can’t validate ECG at home—trust FDA-cleared devices or bring tracings to your cardiologist.
What’s the difference between “medical-grade” and “clinical-grade” marketing claims?
These are often unregulated marketing terms. The only meaningful designation is “FDA-cleared” or “FDA-approved” for medical devices. “Medical-grade” or “clinical-grade” without FDA clearance is just marketing language and doesn’t guarantee accuracy or that doctors will trust the data. Always look for “FDA 510(k) cleared” or “FDA De Novo authorized” for devices you’ll use for medical decisions. Consumer wearables (even high-quality ones) can be accurate without FDA clearance, but they’re not validated for diagnosis.
References & Sources
- Fuller D, et al. Reliability and Validity of Commercially Available Wearable Devices for Measuring Steps, Energy Expenditure, and Heart Rate: Systematic Review. JMIR Mhealth Uhealth. 2020;8(9):e18694.
- U.S. Food and Drug Administration. ECG App 510(k) Summary K191521. Published 2018.
- American Heart Association. Monitoring Your Blood Pressure at Home. Updated 2024.
- Luks AM, Swenson ER. Pulse Oximetry for Monitoring Patients with COVID-19 at Home. Potential Pitfalls and Practical Guidance. Ann Am Thorac Soc. 2020;17(9):1040-1046.
- U.S. Food and Drug Administration. Pulse Oximeter Accuracy and Limitations: FDA Safety Communication. Published 2021.
Join the Community & Stay Updated
What Readers Are Saying
💬 “Finally, someone explained the difference between fitness tracking and medical monitoring. Saved me from buying the wrong device.”
— Sarah M., fitness coach and AFib patient
💬 “My cardiologist was impressed I used this guide to choose my blood pressure monitor. He said most patients buy wrist monitors that give unreliable readings.”
— James R., managing hypertension
💬 “The chest strap vs smartwatch comparison convinced me to spend the extra $40 for the Polar H10. My training zones are now accurate—worth it.”
— David L., marathon runner
📧 Get Device Updates & Price Alerts
New FDA-cleared devices launch every quarter. Stay informed:
- 📱 New device reviews within 48 hours of release
- 💰 Price drop alerts on our recommended models
- 📊 Monthly accuracy testing results
- 🆕 FDA clearance announcements for heart monitoring tech
[Subscribe to our Device Monitoring Newsletter →]
No spam. One email per month. Unsubscribe anytime.
🗣️ Join the Discussion
Ask questions, share experiences, or see what devices other people with your condition are using:
Reddit Communities:
- r/HeartHealth — Active community discussing monitors, symptoms, doctor experiences
- r/Fitness — Regular “which heart rate monitor?” threads with user testing data
- r/AppleWatch — AFib detection & ECG feature discussions
Facebook Groups:
- “Home Blood Pressure Monitoring Support” (8,500+ members, physician-moderated)
- “Heart Rate Monitor Reviews & Accuracy Testing” (12,000+ members)
Got questions about this guide?
Dr. Das occasionally responds to comments and reader questions. Leave a comment or question below.
💾 Downloadable Resources
Take this guide with you:
📥 [Download: One-Page Device Decision Checklist (PDF)]
Print this summary to bring to your doctor appointment or use while shopping online.
📥 [Download: Blood Pressure Log Template (PDF)]
Track your readings properly—includes space for time, notes, and medication timing.
📥 [Download: Comparison Spreadsheet (Excel)]
Compare specs of 50+ devices side-by-side. Filter by price, accuracy, features, and FDA clearance.
❓ Have a Specific Question?
If you’re still unsure which device is right for you, you can:
- Review our detailed FAQ section above (covers 15+ common questions)
- Check our individual device reviews (linked throughout this guide)
🔄 Keep This Guide Updated
Bookmark this page. We update this guide quarterly with:
- New device releases and FDA clearances
- Updated accuracy testing data
- Price changes and discontinued models
- Reader-submitted questions added to FAQ
Last updated: January 2025
Next update: April 2025
⭐ Found This Helpful?
Share this guide with someone managing heart health or trying to choose a monitoring device:
Your health monitoring journey starts with the right device. We’ve done the research—now you can monitor with confidence.
⚠️ QUICK SAFETY REFERENCE
EMERGENCY (Call 911):
- Heart rate >180 bpm or <40 bpm (awake)
- Blood pressure >180/120 mmHg
- SpO₂ ≤85% at rest
- Chest pain, severe shortness of breath, fainting
NON-EMERGENCY (See physician):
- Irregular rhythms, BP >140/90 consistently
- SpO₂ <90% during sleep
- Unexplained resting HR change >20 bpm
Consumer devices detect patterns—NOT diagnose. Physician review required.
Last Reviewed : January 10, 2026
Medical Reviewer : Dr. Rishav Das, M.B.B.S.
Methodology : Physician-supervised testing protocols comparing consumer devices to medical reference equipment
