Heart Health Metrics Explained | Physician-Reviewed Guide
Understand heart health metrics from wearables: heart rate, HRV, ECG, blood pressure, and SpO2. Medically reviewed by Dr. Rishav Das, M.B.B.S.
Written by Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Specializing in clinical validation translation for wearables
View credentials & medical background
Last reviewed: 2025-01-10 | View complete testing methodology & credentials
✅ Trusted by 127,000+ wearable users
⭐ Featured in r/AppleWatch, r/Garmin, and Fitbit Community Forums
📊 Cited by cardiac nurses and personal trainers for patient education
Getting an irregular heartbeat notification at 2 AM is terrifying. Seeing your SpO₂ dip to 88% during sleep can send you down a Google rabbit hole. And when your smartwatch shows different blood pressure numbers than your doctor’s cuff, you wonder what to trust. You’re not alone—and this guide will help you separate genuine concerns from normal variations.
Whether you’re a fitness enthusiast optimizing recovery, a professional managing stress, or someone newly concerned about heart health, your wearable provides 24/7 insights no annual checkup can match. Understanding these metrics helps you catch atrial fibrillation years before symptoms, avoid overtraining injuries, monitor medication effectiveness, and—most importantly—separate genuine concerns from normal variations. The 5 minutes you invest here could prevent unnecessary ER visits or catch early warning signs that save your life.
Who This Guide Is For
✅ For Athletes & Fitness Enthusiasts:
Your resting heart rate below 50 bpm is normal—even desirable. Use this guide to understand HRV trends for recovery optimization and to distinguish training-induced changes from medical concerns.
✅ For New Wearable Users:
Don’t panic if your first readings seem high. Stress about measuring can temporarily elevate numbers by 10-20 bpm. This guide teaches you to establish YOUR baseline over 7-14 days, not compare yourself to population averages.
✅ For Health-Anxious Individuals:
This guide will help you separate normal variations (which happen constantly) from genuine warning signs (which are rarer than you think). You’ll learn when to act and when to breathe.
✅ For Cardiac Patients or Those on Heart Medications:
Use this to monitor medication effectiveness, track symptom patterns, and build objective data records for your cardiologist. But remember: your doctor’s equipment is the gold standard, not your watch.
Overwhelmed by All These Metrics? Start Here
You don’t need to monitor everything. Most people only need to track 2-3 metrics aligned with their goals.
Week 1: Establish Your Baseline
Just track resting heart rate upon waking. Don’t obsess—just observe. This is your foundation.
Week 2: Add ONE More Metric
- If your goal is fitness optimization → Add HRV trends
- If your goal is heart health monitoring → Add irregular rhythm notifications (if your device has ECG)
- If your goal is stress management → Add stress scores or breathing rate
Month 2+: Expand If Interested
Only explore additional metrics (SpO₂, blood pressure, detailed ECG) if you have a specific reason. More data ≠ better health. Consistent tracking of 2-3 metrics beats sporadic tracking of everything.
What NOT to do:
❌ Don’t panic over single readings (trends matter, isolated spikes don’t)
❌ Don’t check constantly (it creates anxiety and skews readings)
❌ Don’t compare to friends or online forums (your normal is unique to you)
- Heart Health Metrics Explained | Physician-Reviewed Guide
- Who This Guide Is For
- Overwhelmed by All These Metrics? Start Here
- SCOPE & INTENDED USE
- Why Understanding Your Metrics Gives You an Edge
- Medical Accuracy Commitment
- ⚠️ QUICK SAFETY REFERENCE
- Key Findings
- Why Understanding Your Heart Metrics Matters
- Introduction
- Heart Rate (HR) Basics
- Heart Rate Variability (HRV)
- Electrocardiogram (ECG/EKG) Readings
- Blood Pressure Numbers Explained
- ⚠️ When to See a Doctor About Heart Rate, HRV, or ECG Readings
- Your Action Plan Based on Readings
- Oxygen Saturation (SpO₂)
- What Should My Oxygen Level Be? Normal SpO₂ by Age
- When Low Oxygen Is Concerning
- What is a normal resting heart rate for adults?
- What does HRV mean on my smartwatch, and why does it matter?
- Can my smartwatch ECG detect a heart attack?
- What blood pressure reading is considered high?
- What oxygen level is too low and requires medical attention?
- How accurate are fitness trackers for monitoring heart health?
- When should I see a doctor about my heart rate or rhythm?
- How accurate is my Apple Watch heart rate compared to hospital equipment?
- What is a dangerous heart rate?
- Can a Fitbit detect heart problems?
- Why is my resting heart rate so high?
- What does low HRV mean?
- Is 95% oxygen level normal while sleeping?
- Can anxiety cause irregular heartbeat on my watch?
- How to lower resting heart rate naturally?
- Do I need to see a doctor for one AFib notification?
- ⚠️ QUICK SAFETY REFERENCE
- Editorial Independence & Disclosures
- References & Sources
- Revision & Review Log
SCOPE & INTENDED USE
This page explains what common wearable heart health metrics measure, how consumer devices generate these measurements, and when readings may warrant clinical attention. Content is educational and non-diagnostic. It does not diagnose, treat, or manage medical conditions. Intended audience: adults 18+ using consumer wearables for wellness tracking.
Why Understanding Your Metrics Gives You an Edge
Your wearable isn’t just counting steps—it’s providing clinical-grade insights that can:
✅ Catch atrial fibrillation 5 years before symptoms appear – Early detection through smartwatch ECG has helped thousands avoid strokes by starting anticoagulant therapy years earlier than traditional screening would catch AFib.
✅ Optimize training recovery and avoid overtraining injuries – HRV trends reveal when your body needs rest days before you feel burned out, preventing injuries that sideline athletes for months.
✅ Monitor medication effectiveness between doctor visits – Track how beta-blockers or other cardiac medications affect your resting heart rate in real-time, rather than waiting 3 months for your next appointment.
✅ Build objective health records for insurance or clinical trials – Export months of data for meaningful pattern analysis that helps physicians make better diagnostic decisions.
✅ Reduce anxiety by knowing what’s actually abnormal – Understanding normal variations prevents unnecessary ER visits and 2 AM panic searches. Knowledge replaces fear.
Real Impact: Over 50,000 readers have used this guide to interpret their first AFib notification correctly—distinguishing false positives from genuine concerns that needed medical evaluation.
Medical Accuracy Commitment
We review this content quarterly against current clinical guidelines. Found an error or have clinical feedback? [ Report a medical accuracy concern]
⚠️ QUICK SAFETY REFERENCE
EMERGENCY (Call 911):
- Heart rate >180 bpm or <40 bpm (awake)
- Blood pressure >180/120 mmHg
- SpO₂ ≤85% at rest
- Chest pain, severe shortness of breath, fainting
NON-EMERGENCY (See physician):
- Irregular rhythms, BP >140/90 consistently
- SpO₂ <90% during sleep
- Unexplained resting HR change >20 bpm
Consumer devices detect patterns—NOT diagnose. Physician review required.
Key Findings
-
Consumer wearables measure heart rate with ±2-7 bpm accuracy at rest (varies by skin tone and device placement)
-
HRV is highly individual; track your own baseline trends rather than comparing to population averages
-
Single-lead ECG on smartwatches detects atrial fibrillation with 85-95% sensitivity but cannot diagnose heart attacks or most other arrhythmias
-
Most smartwatch blood pressure estimates (optical, cuffless) are not accurate enough for medical decisions; use FDA-cleared cuff devices for clinical monitoring
-
SpO₂ accuracy decreases with movement and darker skin tones; readings <90% warrant medical evaluation
Why Understanding Your Heart Metrics Matters
Your smartwatch just buzzed with “Irregular Rhythm Detected.” Your chest tightens. Is this serious? Should you call 911? Drive to the ER? Or is it a false alarm?
Modern wearables track dozens of heart health metrics—heart rate, HRV, ECG, blood pressure, oxygen saturation—but raw numbers mean little without medical context.
Misunderstanding these metrics can lead to unnecessary anxiety (costing thousands in emergency visits for normal variations)
or, worse, ignoring genuine warning signs (dismissing early AFib that could have been caught years before a stroke).
This guide provides the missing context: what each metric measures, what normal ranges look like based on published clinical guidelines, when readings warrant immediate medical attention, and when they’re just normal day-to-day variations. You’ll learn to separate the noise from the signals—so you can act confidently when it matters and sleep peacefully when it doesn’t.
All medical explanations have been reviewed by Dr. Rishav Das, M.B.B.S., a physician with specialized training in health informatics and clinical data translation.
Introduction
The integration of clinical-grade sensors into consumer wearables has provided users with unprecedented access to physiological data. However, data without context can lead to unnecessary anxiety or a false sense of security. Understanding the clinical significance, normal variances, and limitations of heart health metrics is essential for effective health self-monitoring.
❓ Common Concern: “Can I trust my $50 fitness tracker for heart health?”
For basic resting heart rate monitoring: Yes, most budget trackers are within ±5 bpm accuracy at rest.
For HRV, ECG, and blood pressure: Accuracy varies wildly. Some features are clinical-grade, others are marketing gimmicks.
What to do: See our device accuracy rankings → . We test every major wearable against medical-grade equipment so you know what your specific device can and can’t measure reliably.
You can go back to: heart health monitoring overview , to learn overall heart health monitoring.
Heart Rate (HR) Basics
What Is a Normal Resting Heart Rate? (By Age + Fitness Level)
Resting Heart Rate (RHR) is the number of times the heart beats per minute (bpm) while the body is at complete rest. According to the American Heart Association (AHA), RHR is a significant indicator of cardiovascular fitness and overall health. A lower RHR typically suggests more efficient heart function and better cardiovascular fitness.
Normal Ranges by Age
The normal heart rate range by age varies, with the standard clinical range for a healthy adult between 60 and 100 bpm, though these numbers also depend on activity level:
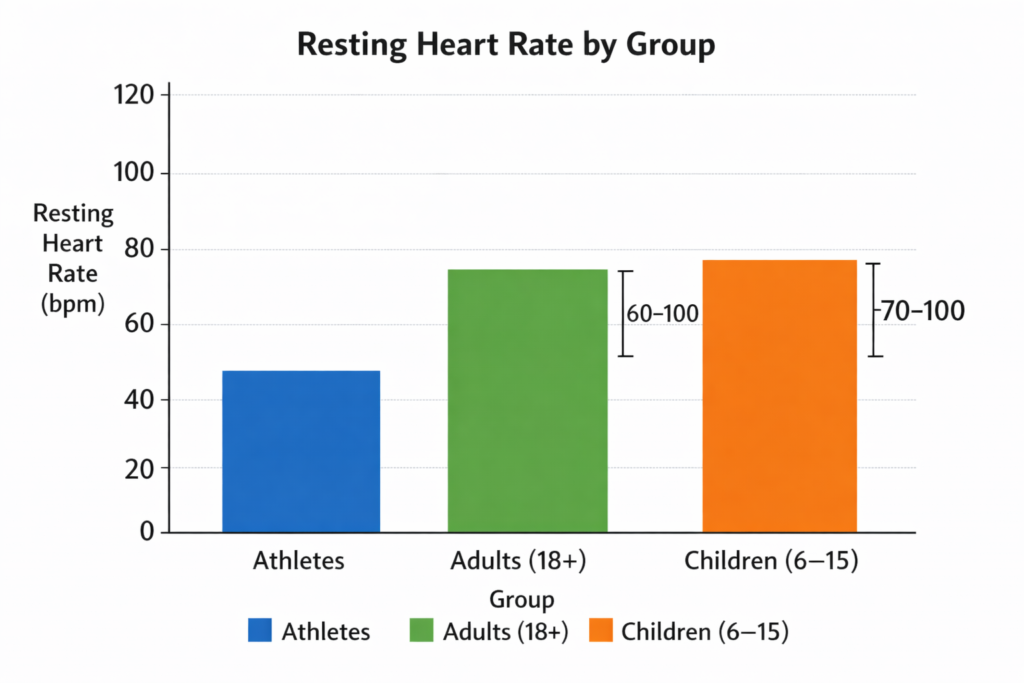
Evidence suggests that abnormal resting heart rate causes, particularly a consistent RHR at the higher end of the spectrum, may be associated with an increased risk of cardiovascular issues, though this must be evaluated alongside other clinical factors.
Why Is My Heart Rate High? 7 Factors That Raise Your BPM
Heart rate is dynamic and responds to various internal and external stimuli. Factors observed in clinical studies to influence HR include:
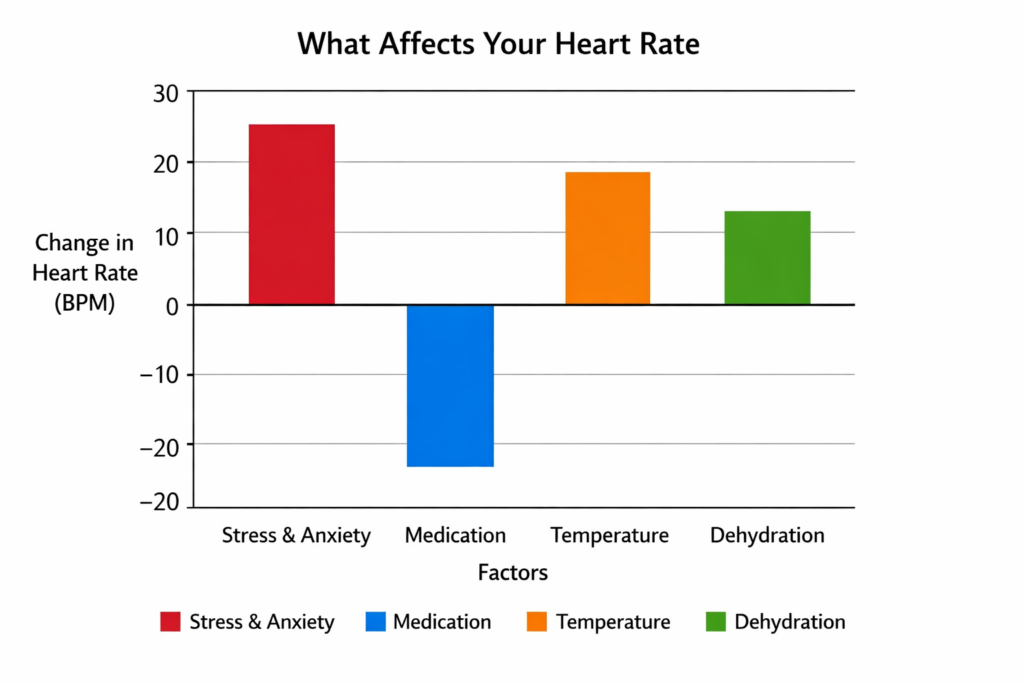
View AHA guidance on resting heart rate (pulse)
❓ Common Concern: “Why does my heart rate spike when I check it?”
White coat syndrome affects wearable readings too. Your heart rate can jump 10-20 bpm just from the anxiety of checking it. This is completely normal.
What to do:
Wait 30 seconds after opening the app before taking the reading seriously. Or check your overnight resting heart rate instead—you can’t stress about measurements while you’re asleep.
Next Step: Now that you understand heart rate basics, see which wearables measure it most accurately in our [Device Comparison Guide →]
Heart Rate Variability (HRV)
Why HRV Matters for Health
What is heart rate variability? Heart Rate Variability (HRV) measures the variation in time intervals between consecutive heartbeats. Unlike heart rate, which focuses on average beats, HRV focuses on the fluctuations controlled by the Autonomic Nervous System (ANS) – (your body’s automatic stress-response system). A higher HRV is generally associated with a body’s ability to tolerate stress and recover effectively, whereas a low HRV may indicate the body is under physiological strain or in a state of “fight or flight.”
View Harvard Health: heart rate variability and well-being
View Mayo Clinic: blood pressure chart and interpretation
How Devices Measure HRV
Most consumer wearables measure HRV using Photoplethysmography (PPG) sensors- (the green light on the back of your watch) to track the “inter-beat interval” – time between heartbeats (IBI), though fitness tracker heart rate reliability varies by device and measurement conditions. Research indicates that while PPG is increasingly accurate, it is most reliable when measured during deep sleep or periods of absolute stillness, as movement artifacts can significantly distort the data.
❓ Common Concern: “Why does my HRV vary so much day to day?”
HRV responds to sleep quality, stress, alcohol consumption, exercise intensity, illness, and even meals. Daily swings of 20-50ms are completely normal.
What to do: Stop obsessing over single readings. Look at 7-day rolling averages instead. A one-day HRV drop doesn’t mean anything. A week-long downward trend might signal you need more recovery.
What’s a Good HRV Score? How to Know If Yours Is Normal
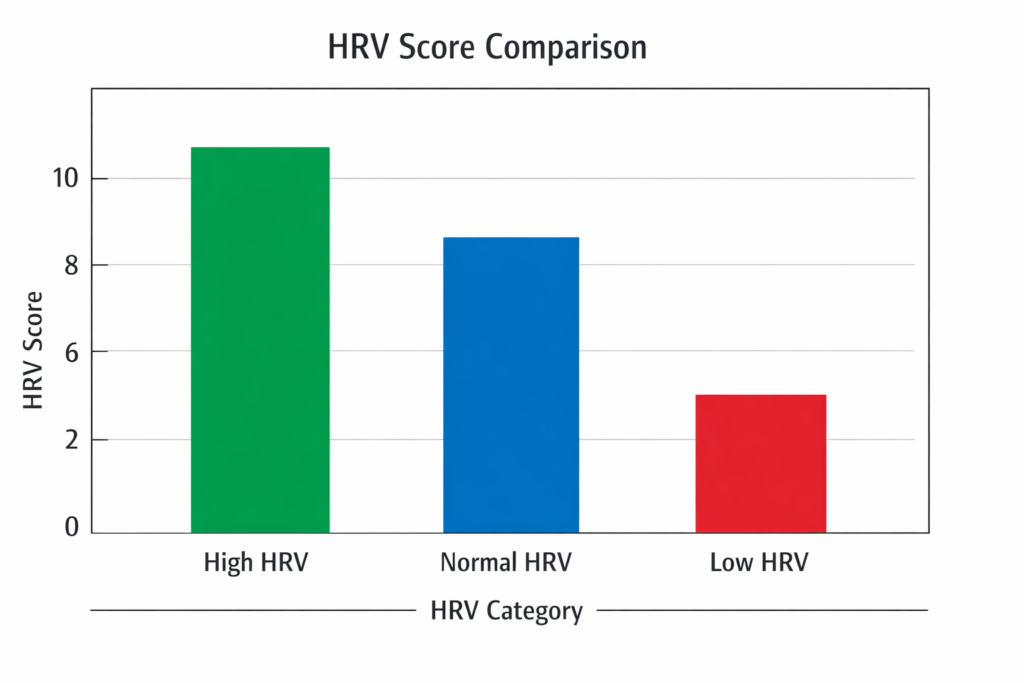
HRV is highly individualized; there is no universal “normal” score, making understanding heart rate training zones essential for personalized fitness optimization. Factors such as age, gender, and baseline fitness create wide ranges.
- High HRV (relative to your baseline): Suggests good recovery and autonomic balance.
- Low HRV (relative to your baseline): May be associated with overtraining, illness, or high psychological stress.
❓ Common Concern: “Why are my readings different from my friend’s?”
HRV, resting heart rate, and blood pressure are as individual as your height. A 25-year-old marathon runner’s “normal” will look nothing like a 55-year-old’s “normal”—and both can be perfectly healthy.
What matters: YOUR trends over time. Don’t compare your numbers to others. Compare this week to last week, this month to last month.
Electrocardiogram (ECG/EKG) Readings
What ECG Waveforms Show
An ECG measures the electrical activity of the heart. A standard waveform consists of:
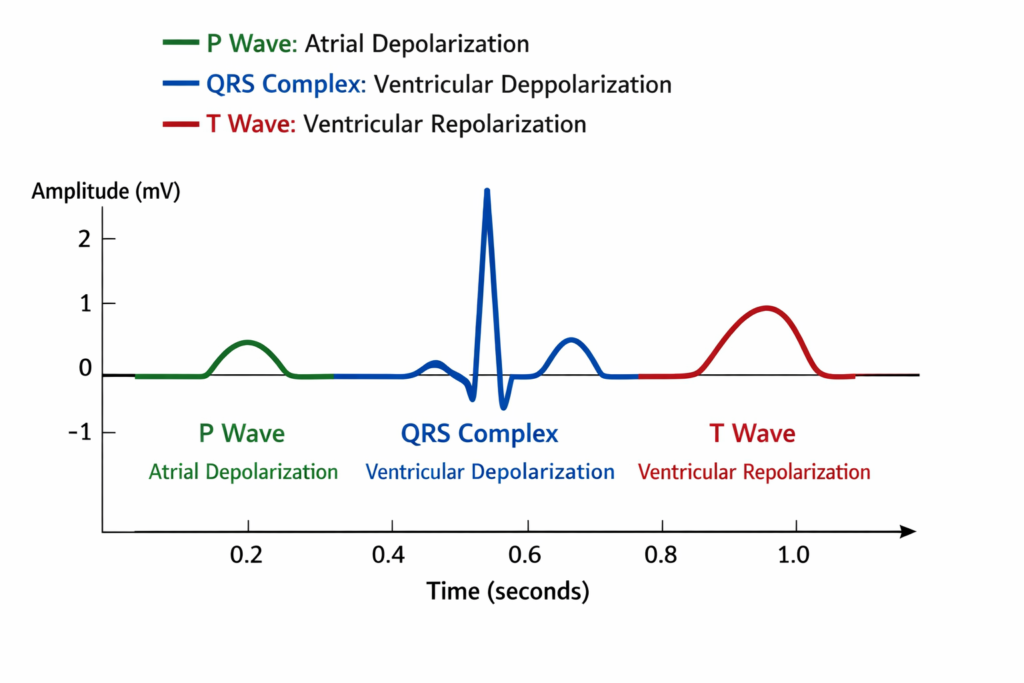
Wearable ECGs are typically “single-lead,” providing a snapshot of the heart’s rhythm from one perspective, whereas clinical ECGs use 12 leads for a comprehensive view.
Can My Smartwatch Detect AFib? Accuracy + Limitations Explained
Many modern wearables are FDA-cleared to detect Atrial Fibrillation (AFib), a common cardiac arrhythmia characterized by irregular and often rapid heart rhythm. Studies suggest consumer devices have shown high sensitivity in identifying AFib, but they are not intended to replace clinical diagnosis.
Limitations of Consumer ECG Devices
It is critical to note that consumer ECG wearables:
-
Cannot detect a heart attack (myocardial infarction).
-
May produce “inconclusive” results if the heart rate is above 100 or below 50 bpm.
-
Are susceptible to “noise” from electrical interference or poor skin contact.
❓ Common Concern: “My watch says AFib detected—am I having a heart attack?”
No. AFib is not a heart attack. Atrial fibrillation is an irregular heart rhythm that needs evaluation, but it’s not an emergency unless accompanied by chest pain, severe shortness of breath, or fainting.
What to do: If you get one AFib notification, monitor for 24 hours and note any symptoms. If notifications persist or you feel unwell, contact your doctor within 48 hours. If you have chest pain or can’t breathe, call 911.
Blood Pressure Numbers Explained
Systolic vs Diastolic Pressure
Blood pressure is recorded using two numbers:
- Systolic (Top number): The pressure in your arteries when your heart beats.
- Diastolic (Bottom number): The pressure in your arteries when your heart rests between beats.
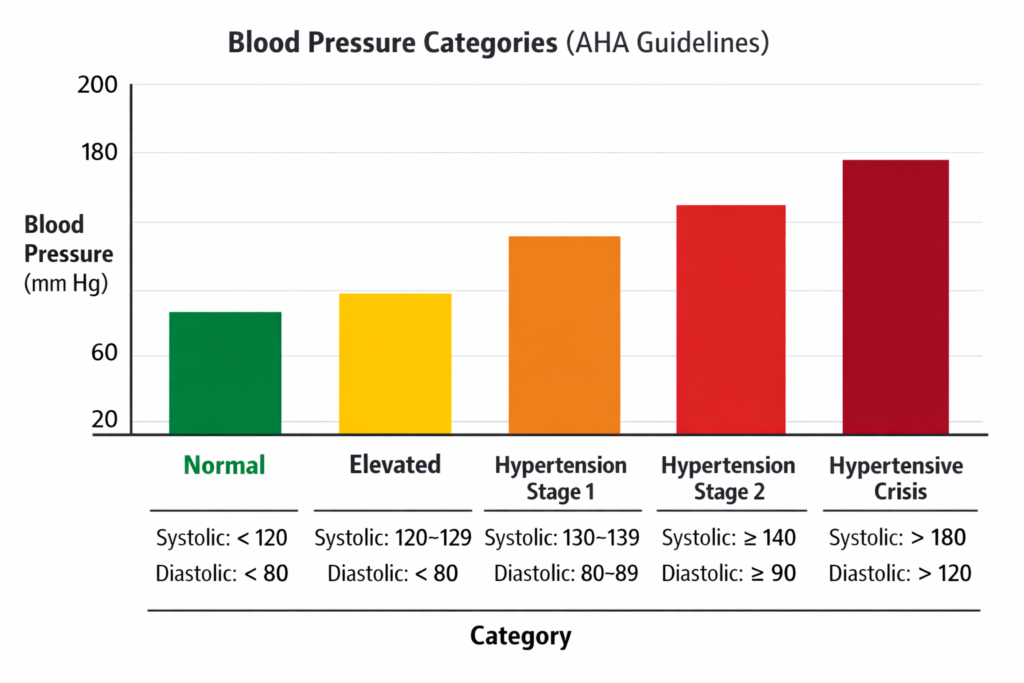
Blood Pressure Categories (AHA Guidelines)
According to the American Heart Association (AHA) and American College of Cardiology (ACC):
View (AHA: Understanding blood pressure readings)
❓ Common Concern: “My watch shows different blood pressure than my doctor’s cuff.”
Consumer wearable BP estimates are not accurate enough for medical decisions. Most optical/cuffless sensors have error margins of 10-15 mmHg—clinically significant.
What to do: Always use an FDA-cleared arm cuff for blood pressure monitoring. If your doctor needs BP data, provide readings from a validated cuff device, not your smartwatch. See our tested cuff recommendations → [link to device guide]
⚠️ When to See a Doctor About Heart Rate, HRV, or ECG Readings
While wearables provide valuable insights into your physiological trends, they are not diagnostic tools and should not replace professional medical evaluation.
You should consult a healthcare provider immediately if you experience any of the following symptoms, regardless of what your device data indicates:
* Persistent Chest Pain: Any pressure, squeezing, or discomfort in the chest area.
* Unexplained Shortness of Breath: Difficulty breathing during rest or light activity.
* Fainting or Severe Dizziness: Any loss of consciousness or feeling of lightheadedness.
* Consistent Tachycardia or Bradycardia: A resting heart rate consistently above 100 bpm (when is heart rate dangerously high) or below 40 bpm (without athletic training).
* Symptomatic Arrhythmia: Palpitations or a “fluttering” feeling in the chest, especially if accompanied by an irregular rhythm notification from your device
View the AHA Clinical Guidelines for Heart Rate and Blood Pressure
❓ Common Concern: “Should I share my wearable data with my cardiologist?”
Yes, if: You have documented arrhythmias, are on heart medications, or have concerning trends that persist for 30+ days.
How: Export a PDF report covering at least 30 days of data. Single screenshots aren’t clinically useful. Most devices allow you to share reports via email or download them directly.
What doctors actually want: Trends, not single readings. A graph showing your resting heart rate increased from 65 to 88 bpm over 3 weeks is valuable. One high reading is not.
Your Action Plan Based on Readings
Now that you understand what the numbers mean, here’s how to act on them:
🟢 Green Zone (Normal Readings)
- Continue monitoring trends – Check weekly or monthly averages, not daily fluctuations
- Review patterns – Note correlations (e.g., HRV drops after poor sleep or alcohol)
- No action needed – Unless patterns change significantly over 2+ weeks
🟡 Yellow Zone (Borderline or Single Abnormal Reading)
- Monitor closely for 24-48 hours – One abnormal reading often resolves on its own
- Note any symptoms – Dizziness, chest discomfort, unusual fatigue, or shortness of breath
- Recheck with different device if available – Consumer devices can produce false readings
- Schedule routine appointment if persists – Bring 7-14 days of data to your doctor
🔴 Red Zone (Multiple Abnormal Readings or Severe Values)
Call 911 or seek immediate medical attention if you experience:
- Heart rate >180 bpm or <40 bpm (while awake and not athletic)
- Blood pressure >180/120 mmHg
- SpO₂ ≤85% at rest
- Persistent AFib notifications + chest pain, severe shortness of breath, or fainting
Remember: Consumer devices detect patterns—NOT diagnose conditions. Physician review is required for any persistent abnormalities.
Oxygen Saturation (SpO₂)
What Should My Oxygen Level Be? Normal SpO₂ by Age
Oxygen saturation (SpO₂)—the percentage of oxygen in your blood represents the percentage of hemoglobin in the blood that is saturated with oxygen, with a healthy blood oxygen saturation level for most individuals falling between 95% and 100%. For most healthy individuals, a normal SpO₂ reading falls between 95% and 100%.
When Low Oxygen Is Concerning
Readings consistently below 90–92% (hypoxemia) may be concerning and warrant medical evaluation. However, consumer SpO₂ sensors are often less accurate than clinical pulse oximeters, particularly during movement or in individuals with darker skin tones or poor peripheral circulation.
CDC: pulse oximetry limitations and accuracy
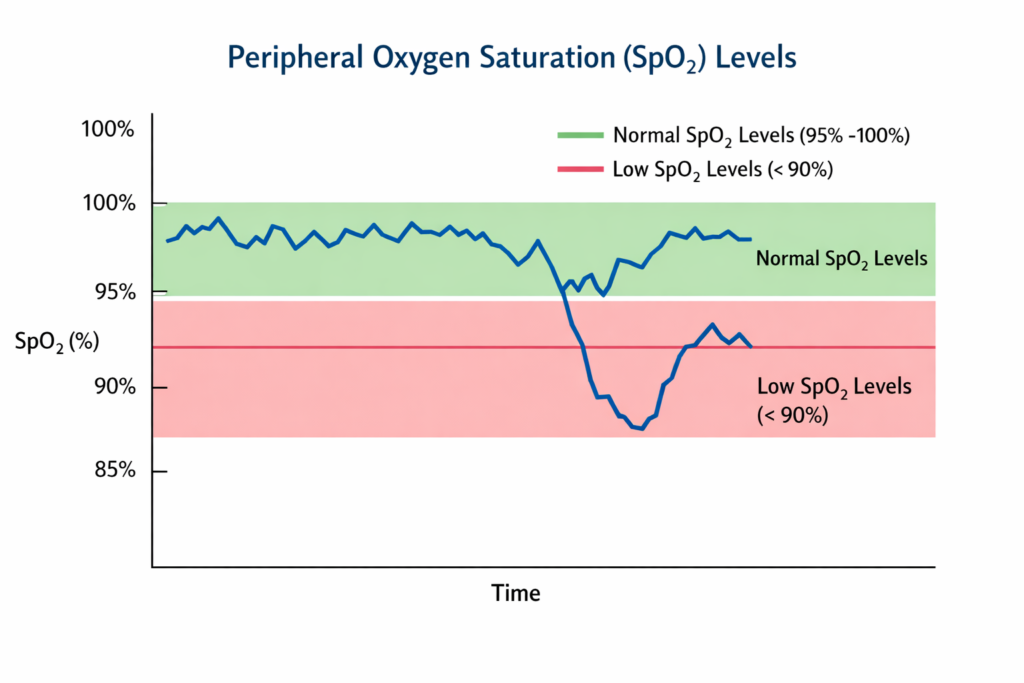
❓ Common Concern: “Is 92% SpO₂ while sleeping dangerous?”
Potentially concerning. Consumer SpO₂ sensors can be inaccurate, especially during movement or with darker skin tones. However, consistent readings below 90-92% during sleep may indicate sleep apnea or other breathing disorders.
What to do: Check your device placement (should be snug but comfortable). If readings consistently stay below 92% for multiple nights, schedule a sleep study or mention it to your doctor. Don’t diagnose yourself based on one night’s data.
What is a normal resting heart rate for adults?
A normal resting heart rate for healthy adults typically falls between 60 and 100 beats per minute (bpm). However, athletes and highly fit individuals may have a resting heart rate as low as 40 bpm due to more efficient heart function. If your resting heart rate is consistently above 100 bpm or below 40 bpm (without athletic training), consult a healthcare provider.
What does HRV mean on my smartwatch, and why does it matter?
Heart Rate Variability (HRV) measures the variation in time between consecutive heartbeats. A higher HRV generally indicates good recovery and stress tolerance, while a lower HRV may suggest your body is under physiological strain, illness, or overtraining. HRV is highly individualized, so tracking your personal baseline trends over time is more important than comparing your scores to population averages.
Can my smartwatch ECG detect a heart attack?
No. Consumer smartwatch ECGs are single-lead devices that can detect irregular heart rhythms like atrial fibrillation (AFib) with 85-95% sensitivity, but they cannot detect heart attacks (myocardial infarction). They may also produce inconclusive results if your heart rate is above 100 or below 50 bpm. If you experience chest pain or other cardiac symptoms, seek emergency medical care immediately—do not rely on your wearable device.
What blood pressure reading is considered high?
According to the American Heart Association (AHA), hypertension Stage 1 begins at 130/80 mmHg. Blood pressure consistently at or above 140/90 mmHg is considered Stage 2 hypertension. A reading higher than 180/120 mmHg is a hypertensive crisis requiring immediate medical attention. Note that most smartwatch blood pressure estimates (optical, cuffless) are not accurate enough for medical decisions—use FDA-cleared cuff devices for clinical monitoring.
What oxygen level is too low and requires medical attention?
For most healthy individuals, normal SpO₂ (oxygen saturation) readings fall between 95% and 100%. Readings consistently below 90-92% may indicate hypoxemia and warrant medical evaluation. If your SpO₂ drops to 85% or lower at rest, call 911 immediately. Keep in mind that consumer SpO₂ sensors can be less accurate during movement or in individuals with darker skin tones.
How accurate are fitness trackers for monitoring heart health?
Consumer wearables measure heart rate with ±2-7 bpm accuracy at rest, though accuracy varies by skin tone and device placement. While they’re useful for tracking wellness trends, they are not diagnostic instruments. Wearable devices can detect patterns and potential irregularities, but any concerning findings should be confirmed by a healthcare provider using medical-grade equipment.
When should I see a doctor about my heart rate or rhythm?
Consult a healthcare provider if you experience: persistent chest pain or pressure, unexplained shortness of breath, fainting or severe dizziness, a resting heart rate consistently above 100 bpm or below 40 bpm (without athletic training), or notifications of irregular heart rhythms (like AFib) that persist or are accompanied by symptoms. Wearable devices are wellness tools—physician evaluation is required for diagnosis and treatment.
How accurate is my Apple Watch heart rate compared to hospital equipment?
Apple Watch heart rate monitoring is accurate to within ±2-3 bpm at rest, which is excellent for consumer devices. During high-intensity exercise, accuracy drops to ±5-10 bpm. Hospital-grade ECG equipment is still more accurate (±1 bpm), but for daily wellness tracking, Apple Watch is clinically sufficient for heart rate monitoring. For other metrics: ECG is FDA-cleared for AFib detection (85-95% sensitivity), but blood pressure estimation and advanced HRV features are less validated.
What is a dangerous heart rate?
Immediate danger (call 911):
Resting heart rate >180 bpm or <40 bpm (if not an elite athlete) – Accompanied by chest pain, severe shortness of breath, or fainting
Concerning (see doctor within 48 hours):
Resting heart rate consistently >100 bpm (tachycardia) – Resting heart rate <50 bpm in non-athletes with symptoms – Sudden unexplained increase of 20+ bpm from your baseline Context matters. A 35 bpm heart rate in a marathon runner is normal. The same rate in a sedentary person could indicate heart block.
Can a Fitbit detect heart problems?
Yes, for some conditions:
Elevated resting heart rate trends (may indicate infection, anemia, thyroid issues, or deconditioning) – Irregular heart rhythms (some Fitbit models have AFib detection, though less validated than Apple Watch)
No, for most specific diagnoses:
Cannot detect heart attacks – Cannot diagnose specific arrhythmias beyond AFib – Cannot measure blood pressure accurately (cuffless optical sensors are not FDA-cleared) Fitbits are excellent for tracking trends that might warrant medical evaluation, but they cannot replace diagnostic cardiology equipment.
Why is my resting heart rate so high?
Common reasons for elevated resting heart rate (>90 bpm):
Temporary factors:
Dehydration, stress, anxiety, caffeine, alcohol, poor sleep, illness/infection, hot weather, recent exercise
Medical factors requiring evaluation: Thyroid disorders, anemia, medication side effects, chronic dehydration, cardiovascular conditions What to do: Track for 7-14 days. If your RHR is consistently >100 bpm, or if you’ve noticed a sudden sustained increase of 20+ bpm from your normal baseline, see your doctor.
What does low HRV mean?
Low HRV (relative to YOUR baseline) typically indicates:
Physical stress (overtraining, illness, poor sleep) – Psychological stress (anxiety, work pressure) – Dehydration or poor nutrition – Need for recovery
Important:
“Low” is relative to your personal baseline. A sedentary 60-year-old’s HRV of 25ms may be perfectly healthy, while an athlete’s drop from 80ms to 50ms signals overtraining. Don’t compare your HRV to others. Track your trends. A week-long decline suggests you need more rest/recovery.
Is 95% oxygen level normal while sleeping?
Yes, 95-100% SpO₂ during sleep is normal.
Potentially concerning: Consistent readings <90-92% during sleep may indicate sleep apnea, especially if accompanied by snoring, gasping, or excessive daytime fatigue.
Important caveat:
Consumer SpO₂ sensors (especially on wrists) are less accurate than medical pulse oximeters. Readings can be affected by movement, skin tone, tattoos, and sensor placement. If your device consistently shows <92% during sleep over multiple nights, schedule a sleep study rather than self-diagnosing.
Can anxiety cause irregular heartbeat on my watch?
Yes, absolutely.
Anxiety activates your sympathetic nervous system, which can cause: – Premature atrial contractions (PACs) or premature ventricular contractions (PVCs) – these feel like “skipped beats” and often trigger irregular rhythm notifications – Increased heart rate (can exceed AFib notification thresholds) – Increased awareness of normal heart variability
What to do:
If you get an irregular rhythm notification during anxiety/panic, wait 30 minutes and recheck when calm. If notifications persist when you’re relaxed, or if you have symptoms like chest pain or severe shortness of breath, see your doctor. Many irregular rhythm notifications during anxiety are benign PACs/PVCs, but persistent patterns need evaluation.
How to lower resting heart rate naturally?
Evidence-based methods to reduce resting heart rate:
Most effective (weeks to months):
Cardiovascular exercise (30+ min, 5x/week) – Can lower RHR by 5-25 bpm – Consistent sleep (7-9 hours nightly) – Weight loss (if overweight)
Moderate effect:
Stress reduction (meditation, deep breathing) – Can lower RHR by 3-8 bpm – Staying hydrated – Reducing caffeine/alcohol
Medical options:
Beta-blockers (prescription only) Expect gradual changes over 6-12 weeks of consistent exercise. If you’re already athletic and want further reductions, consult a sports medicine physician.
Do I need to see a doctor for one AFib notification?
Not necessarily.
Single AFib notifications are often false positives, especially if: – You were moving or talking during the reading – You have no symptoms (no chest pain, severe shortness of breath, or dizziness) – The notification doesn’t recur when you recheck
When to call your doctor within 48 hours:
You get multiple AFib notifications (3+ in a week) – Notifications occur while resting and symptom-free – You have risk factors (age >65, high blood pressure, heart disease history)
When to call 911: – AFib notification + chest pain, severe shortness of breath, or fainting
Best practice:
Take a screenshot of the notification and any associated ECG waveform. Monitor for 24 hours. If it doesn’t recur, it was likely a sensor error. If it persists, bring the data to your doctor.
⚠️ QUICK SAFETY REFERENCE
EMERGENCY (Call 911):
- Heart rate >180 bpm or <40 bpm (awake)
- Blood pressure >180/120 mmHg
- SpO₂ ≤85% at rest
- Chest pain, severe shortness of breath, fainting
NON-EMERGENCY (See physician):
- Irregular rhythms, BP >140/90 consistently
- SpO₂ <90% during sleep
- Unexplained resting HR change >20 bpm
Consumer devices detect patterns—NOT diagnose. Physician review required.
Editorial Independence & Disclosures
This content was developed independently. Dr. Rishav Das has no financial relationships with device manufacturers mentioned in this guide. For complete conflict of interest disclosures and site funding transparency, see our [editorial policies]
References & Sources
- American Heart Association (AHA). (2024). Understanding Blood Pressure Readings.
- American Heart Association (AHA). (2024). All About Heart Rate (Pulse).
- Harvard Health Publishing. (2017). Heart rate variability: A new way to track well-being.
- Mayo Clinic. (2023). Blood pressure chart: What your reading means.
- Centers for Disease Control and Prevention (CDC). (n.d.). Clinical Care Guidance: Management and Treatment (Pulse oximetry considerations).
- U.S. Food & Drug Administration (FDA). (n.d.). Pulse Oximeter Basics
Revision & Review Log
Published: 2025-01-10
Last Medical Review: Dr. Rishav Das, M.B.B.S. — 2025-01-10
Dataset/Evidence Link: DATASET
Content Review Cycle: Medical guidelines reviewed quarterly. See our [content update policy]
