Best Stress Tracking Devices (2026): HRV Wearables, Biofeedback & Smart Ring Guide
Compare stress trackers, rings, and chest straps. Learn how HRV and EDA sensors help manage stress and improve recovery with this medically reviewed guide.
Written and medically reviewed by Dr. Rishav Das, M.B.B.S. — see About page for full credentials and editorial standards.
Medical Review Statement:
This content has been reviewed according to the medical standards and editorial oversight process outlined on our About page.
Disclaimer: All information on this page is educational in nature. It does not constitute medical diagnosis, treatment, or clinical advice. For personalized health guidance, consult a qualified healthcare provider.
Introduction
Stress is invisible until it isn’t — until it shows up in poor sleep, rising heart rate, or a crash in focus and mood. If you’re researching devices to track and manage your stress, this guide covers every category: smartwatches, smart rings, chest straps, biofeedback devices, and breathing tools.
You’ll find sensor comparisons, accuracy caveats, and structured criteria to match a device to your goals — whether you’re managing burnout, optimizing athletic recovery, or building a meditation practice. If you’re comparing stress tracking devices and don’t know where to start, begin with the Quick Picks summary below.
Who This Guide Is For
This guide is written for adults dealing with one of three situations:
- Burned-out professionals — You feel chronically stressed but can’t quantify it. You want data that confirms what your body is telling you and a tool that helps you intervene.
- Athletes and active adults — You train hard and want to monitor recovery, prevent overtraining, and understand how stress affects performance.
- Anxiety-aware individuals — You’ve been told to “manage stress” but want a structured, evidence-informed way to practice and measure progress.
Not sure which category fits you? Use the device decision guide to match your goal to a device type.
- Best Stress Tracking Devices (2026): HRV Wearables, Biofeedback & Smart Ring Guide
- Medical Review Statement:
- Introduction
- Who This Guide Is For
- Quick Picks — Skip the Research
- Device at a Glance — All Categories Compared
- Types of Stress Tracking Devices
- How Stress Tracking Sensors Work: HRV, EDA, and Skin Temperature Explained
- Biofeedback Devices vs. Passive Trackers: Which Is Right for You?
- Meditation and Breathing Tools
- Top Stress Tracking Device Picks for 2026
- Oura Ring vs. Apple Watch vs. WHOOP — Direct Comparison
- Choosing for Your Goals
- Before You Buy: 5 Questions to Ask
- When to Consult a Healthcare Provider
- References
- Explore Further
Quick Picks — Skip the Research
| Goal | Recommended Device | Price Range |
| Best overall stress + wellness | Garmin Forerunner 265 | $350–$450 |
| Best for sleep & overnight recovery | Oura Ring Gen3 | $299–$349 |
| Best budget option | Fitbit Sense 2 | $150–$200 |
| Highest HRV accuracy | Polar H10 (chest strap) + HRV4Training | $90–$110 |
| Best biofeedback (active stress training) | HeartMath Inner Balance | $129–$179 |
| Best for meditation | Muse S (EEG headband) | $349–$399 |
Prices are approximate and subject to change. See individual device retailer pages for current pricing.
Device at a Glance — All Categories Compared
| Device Type | Accuracy | Price Tier | Best For | Tracking Style | Ease of Use |
| Smartwatch | Moderate | $150–$450 | General wellness, beginners | Passive (24/7) | Beginner |
| Smart Ring | Moderate–High | $250–$350 | Sleep, recovery, discretion | Passive (overnight focus) | Beginner |
| Chest Strap (HRV) | High | $90–$130 | Athletes, accuracy-focused users | Active (session-based) | Intermediate |
| Biofeedback device | High (session) | $100–$300 | Stress reduction, anxiety management | Active (10–20 min/day) | Intermediate |
| Meditation wearable | Variable | $250–$400 | Meditation habit, mindfulness | Active (session-based) | Beginner–Intermediate |
Use this table as your entry point; detailed category breakdowns follow below.
Types of Stress Tracking Devices
TL;DR — Types of Stress Tracking Devices
Smartwatches are the most convenient starting point. Smart rings offer better sleep data. Chest straps are most accurate. Biofeedback devices are the only category designed to actively reduce stress — not just measure it.
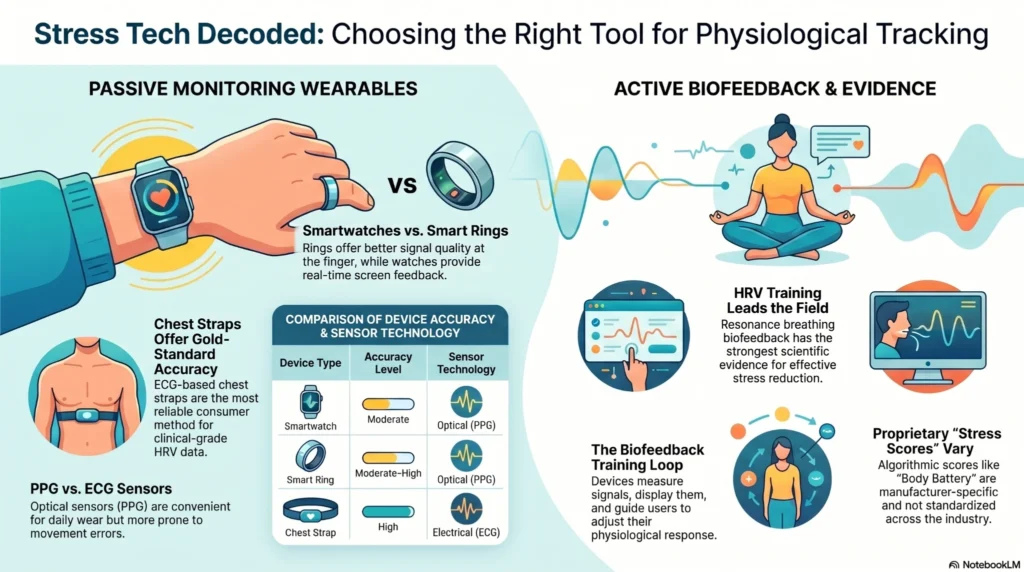
Smartwatches with Stress Features
Smartwatches are multipurpose wrist-worn devices that include stress-related metrics alongside activity, sleep, and cardiovascular monitoring. They represent the broadest consumer market entry point for stress tracking.
| Feature | What It Measures | Typical Accuracy Level | Consumer Examples |
| HRV monitoring | Autonomic nervous system balance | Moderate–High (PPG-based) | Apple Watch, Garmin, Samsung Galaxy Watch |
| EDA (Galvanic Skin Response) | Electrodermal activity as a stress proxy | Moderate | Fitbit Sense 2 |
| Stress Score / Body Battery | Composite algorithmic index | Variable (proprietary) | Garmin, Fitbit |
| Sleep stress detection | Overnight HRV and respiration trends | Moderate | Whoop, Apple Watch |
| Breathing rate | Respiratory frequency at rest or during exercise | Moderate | Most flagship smartwatches |
Key Considerations
- Battery life typically ranges from 1–7 days depending on feature usage
- Optical (PPG) sensors at the wrist may be less accurate than chest-strap measurements for HRV, particularly during movement [1]
- Proprietary stress scores are algorithmically derived and not standardized across manufacturers
Dedicated Smart Rings
Smart rings are compact, finger-worn devices that offer continuous physiological monitoring with a focus on recovery, sleep, and readiness. The finger provides a favorable site for optical sensing due to arterial proximity.
| Feature | Smart Ring Capability | Notes |
| HRV measurement | Continuous overnight; spot-checks available | Finger PPG may yield higher signal quality than wrist [2] |
| Skin temperature | Continuous nightly baseline tracking | Useful for detecting illness, cycle tracking, and recovery trends |
| Sleep stage detection | Light, deep, REM via movement + HRV | Algorithm-dependent; not clinically validated as polysomnography |
| Readiness / Recovery Score | Composite daily index | Proprietary; varies by platform |
| Form factor | Minimal; no screen | May suit users who find wrist wearables intrusive |
Limitations
- No real-time display; requires companion app review
- Ring sizing requires precise fit for accurate optical reading
- Limited active feedback features compared to smartwatches
Chest Strap HRV Monitors
Chest straps using ECG-based (electrical) rather than optical (PPG) sensors are generally regarded as the most accurate consumer method for HRV measurement [3]. They are used extensively in sports science, cardiac rehabilitation contexts, and research-grade wellness applications.
| Attribute | Chest Strap Detail |
| Sensor type | Electrical (ECG-equivalent R-R interval) |
| HRV accuracy | High — closely approximates clinical ECG [3] |
| Typical use case | Pre/post workout HRV, morning readiness, research protocols |
| Comfort | Lower during sleep; best for structured measurement sessions |
| Data output | R-R intervals exported to compatible apps (HRV4Training, Elite HRV, etc.) |
| Battery life | Typically 400–1,000 hours (replaceable coin cell) |
Key Distinction
- Chest strap HRV data is considered more reliable for research and clinical comparison purposes than wrist- or finger-based optical HRV
- Not designed for continuous passive wear; best used in deliberate measurement windows
Biofeedback Devices
Biofeedback devices provide real-time physiological information with the explicit goal of training the user to consciously influence their own stress response. This category includes clinical-grade tools used in therapeutic settings and consumer-accessible devices.
| Device Type | Physiological Signal | Feedback Mechanism | Evidence Level |
| HRV biofeedback device | Heart rate variability | Visual / auditory resonance breathing cue | Moderate–Strong [4, 5] |
| EDA biofeedback device | Skin conductance | Visual graph or alert | Moderate [6] |
| Neurofeedback headband | EEG brain activity | App-based visual/audio response | Emerging [7] |
| Respiration biofeedback belt | Breathing rate and pattern | Real-time audio or visual guide | Moderate [8] |
| Temperature biofeedback sensor | Peripheral skin temperature | Visual temperature display | Limited consumer evidence |
What the Evidence Indicates
- HRV biofeedback (using a resonance frequency breathing protocol near 0.1 Hz / ~6 breaths/min) has the strongest body of research supporting stress reduction effects [4, 5]
- EDA and EEG biofeedback show promise but require more replication in non-clinical populations [6, 7]
- Outcome quality may depend significantly on structured training protocol adherence, not device alone
For users who commit to consistent practice, multiple controlled studies show measurable reductions in perceived stress and improvements in autonomic regulation within 4–6 weeks of daily 10–20 minute HRV biofeedback sessions [4, 5]. For professionals managing high workloads, daily HRV trend tracking has revealed that poor sleep quality — not work volume itself — is frequently the primary driver of elevated stress scores. Identifying that pattern is the first step toward acting on it.
How Stress Tracking Sensors Work: HRV, EDA, and Skin Temperature Explained
TL;DR — Sensors and Technology
HRV (heart rate variability) is the most research-validated stress signal in consumer devices. EDA (skin conductance) and skin temperature are useful secondary signals but less reliable on their own. Chest-strap ECG beats wrist PPG for HRV accuracy.
Heart Rate Variability (HRV) Sensors
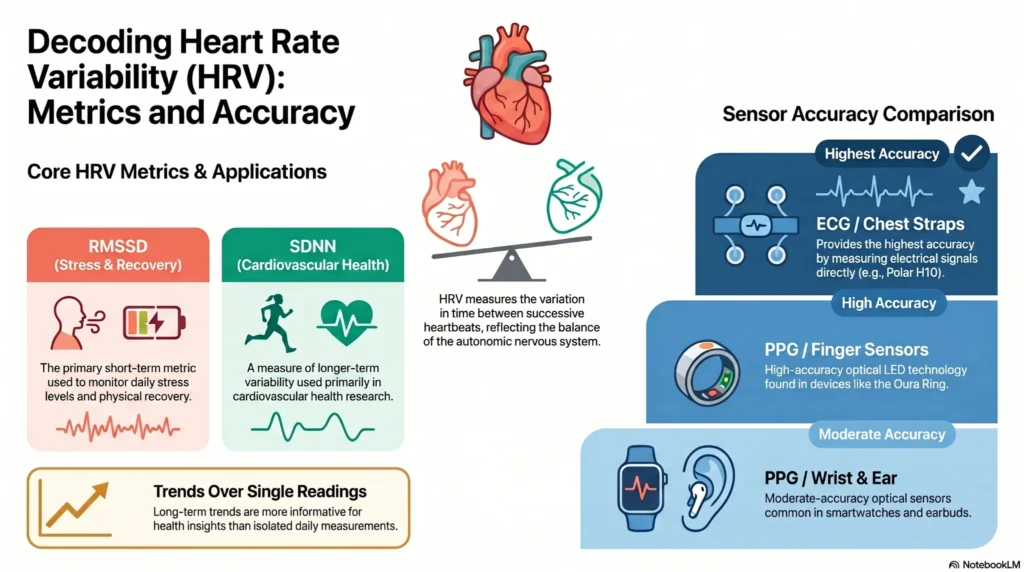
HRV refers to the variation in time intervals between successive heartbeats (R-R intervals). It is regulated by the autonomic nervous system (ANS) and reflects the balance between sympathetic (“fight-or-flight”) and parasympathetic (“rest-and-digest”) activity [9].
| HRV Metric | Definition | Typical Application |
| RMSSD | Root mean square of successive differences — primary short-term HRV metric | Stress and recovery monitoring |
| SDNN | Standard deviation of all R-R intervals — longer-term variability | Cardiovascular health research |
| LF/HF Ratio | Ratio of low-frequency to high-frequency power | Autonomic balance research (interpretation contested) [10] |
| HF Power | High-frequency band — associated with parasympathetic activity | Relaxation and recovery states |
Measurement Methods Compared
| Method | Sensor Type | Accuracy | Common Devices |
| ECG / electrical | Electrode (chest strap) | Highest | Polar H10, Garmin HRM Pro |
| Photoplethysmography (PPG) — finger | Optical LED | High | Oura Ring, Samsung Galaxy Ring |
| PPG — wrist | Optical LED | Moderate | Apple Watch, Fitbit, Garmin |
| PPG — ear | Optical LED | Moderate | Select earbuds |
Clinical Context
- HRV is used in clinical cardiology, psychiatry, and sports medicine research, though consumer device metrics are not equivalent to clinical ECG-derived HRV [11] For detail on how device accuracy is assessed and reported on this site, see our testing methodology.
- Day-to-day HRV variation is normal; trends over time are more informative than single readings [12]
Electrodermal Activity (EDA) Sensors
Electrodermal activity (also called galvanic skin response, or GSR) measures changes in the electrical conductance of the skin, which is influenced by sweat gland activity under autonomic nervous system control [13]. Higher skin conductance is associated with increased sympathetic arousal.
| EDA Concept | Explanation |
| Tonic EDA | Slow-changing baseline skin conductance level |
| Phasic EDA | Rapid, event-related responses (skin conductance responses, SCRs) |
| Stress association | Sympathetic activation increases sweat gland activity → increased conductance |
| Measurement site | Palm, fingers, wrist (wrist signal is weaker than palmar) |
Consumer Application Limitations
- Wrist-based EDA (used in some smartwatches) produces weaker and noisier signals compared to palmar or finger placement [14]
- EDA is sensitive to temperature, movement artifacts, and skin hydration — limiting real-world accuracy
- EDA is a proxy indicator of arousal, not a direct or specific measure of psychological stress [13]
Skin Temperature Sensors
Wrist and finger skin temperature sensors track peripheral body temperature, which is influenced by circadian rhythms, autonomic nervous system activity, hormonal cycles, illness, and recovery status [15].
| Use Case | How Temperature Data Is Applied |
| Overnight recovery | Elevated nighttime temperature may indicate physiological stress, illness, or insufficient recovery |
| Menstrual cycle tracking | Luteal phase is associated with a measurable temperature rise |
| Illness detection | Fever-related temperature deviations may be detected relative to personal baseline |
| Stress proxy | Peripheral vasoconstriction under sympathetic activation may alter surface temperature |
Important Caveats
- Skin temperature is not equivalent to core body temperature
- Environmental conditions (room temperature, clothing, bedding) can confound measurements
- Temperature-based stress inference is indirect and algorithmically interpreted; it should not be used diagnostically [15]
Breathing Rate Detection
Respiration rate (breaths per minute) can be derived indirectly from PPG signal variation (photoplethysmography-derived respiration, or PDR) or from accelerometer chest movement detection [16].
| Breathing Metric | Stress Relevance |
| Resting respiration rate | Elevated baseline may be associated with heightened sympathetic arousal [17] |
| Breathing rate variability | Irregular patterns may accompany acute stress episodes |
| Respiration during sleep | Elevated or irregular nocturnal breathing may correlate with poor recovery |
| Real-time breathing pace | Used in guided breathing interventions to support resonance frequency training |
Accuracy Considerations
- Breathing rate derived from wrist PPG is an estimate; it carries higher error margins than direct respiratory measurement [16]
- Real-time breathing guidance typically uses accelerometer or device-generated pacing signals rather than live measured respiration
Biofeedback Devices vs. Passive Trackers: Which Is Right for You?
TL;DR — Biofeedback vs. Passive Tracking
Passive trackers tell you how stressed you were. Biofeedback devices help you become less stressed in real time. If your goal is reduction — not just awareness — biofeedback is the category to prioritize.
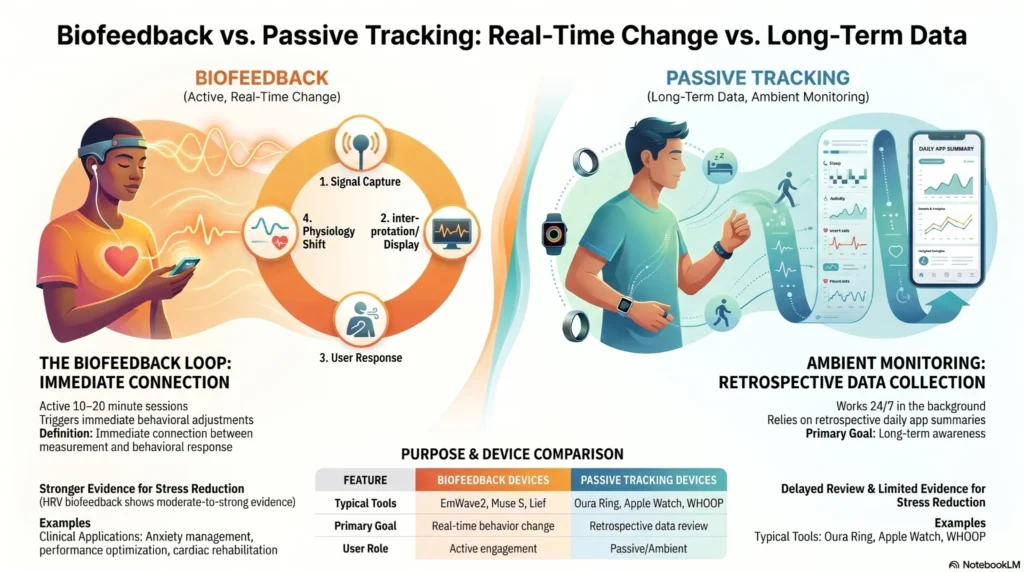
Devices in this category divide into two fundamentally different functional approaches. Understanding the distinction is essential to selecting a device aligned with your goals.
| Dimension | Biofeedback Devices | Passive Tracking Devices |
| Primary function | Real-time physiological signal → user behavior change | Continuous data collection → retrospective review |
| User engagement | Active, session-based | Passive, ambient |
| Feedback timing | Immediate (during session) | Delayed (app review, daily summary) |
| Intervention potential | Built into device workflow | Relies on user-initiated behavior change |
| Evidence for stress reduction | Moderate–Strong (HRV biofeedback protocols) [4, 5] | Limited direct evidence; supports awareness, not intervention |
| Typical session structure | 10–20 minute guided sessions | 24/7 background monitoring |
| Representative devices | EmWave2, Muse S, Lief Therapeutics | Oura Ring, Apple Watch, WHOOP |
Real-Time Feedback Devices
Biofeedback devices are designed to close the loop between physiological measurement and behavioral response during a session.
- Signal is captured → interpreted → displayed or communicated → user adjusts behavior (e.g., breathing pace, muscle relaxation) → physiological response shifts
- This loop is the operational definition of biofeedback
- Research on HRV biofeedback suggests measurable short-term reductions in perceived stress and improvements in autonomic regulation with consistent practice [4, 5]
- Clinical applications include use in anxiety management, performance optimization, and cardiac rehabilitation — consult a provider for therapeutic applications
Daily Summaries and Trends
Passive tracking devices consolidate physiological data into trend views, readiness scores, and longitudinal charts.
- Value: Pattern recognition over time — identifying correlations between lifestyle variables (sleep, activity, diet) and stress-related metrics
- Limitation: Correlation ≠ causation; proprietary scores are not clinically standardized
- Use effectively by:
- Reviewing weekly HRV trends rather than single-day readings
- Noting deviations from personal baseline (individual-relative, not population-norm comparisons)
- Pairing data review with behavioral reflection or journaling
- Sharing trend data with a healthcare provider when clinically relevant
Meditation and Breathing Tools
TL;DR — Meditation and Breathing Tools
Paced breathing at 5–6 breaths/min has the strongest controlled-study support for short-term stress reduction. Devices help with consistency, but the breathing protocol itself — not the hardware — drives the result.
Guided Breathing Devices
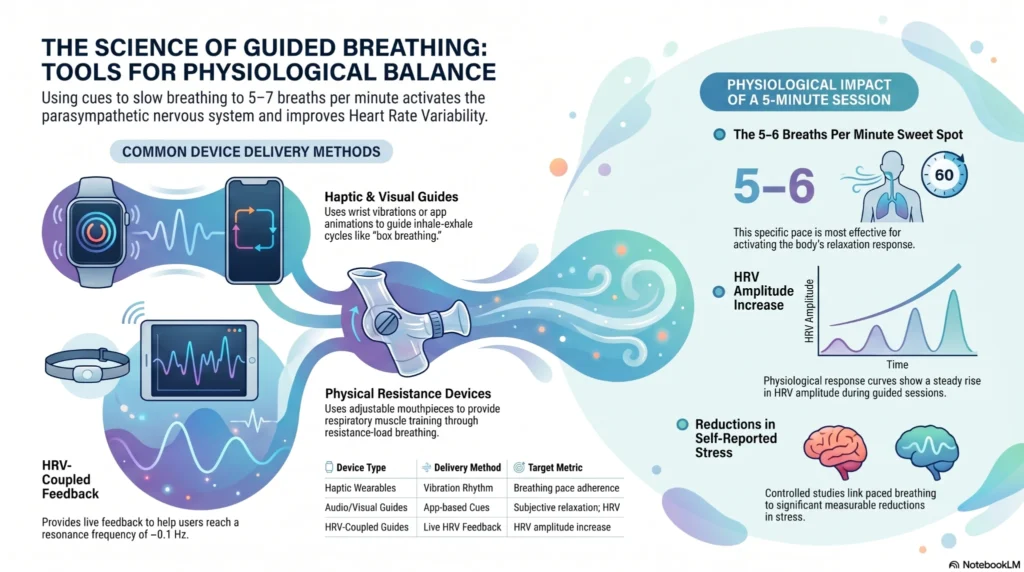
Guided breathing devices prompt users through structured respiratory exercises designed to influence the autonomic nervous system. Evidence supporting slow, paced breathing techniques (particularly at approximately 5–7 breaths per minute) for parasympathetic activation is moderate to strong [8, 18].
| Device Type | Delivery Method | Typical Protocol | Target Metric |
| Haptic vibration wearables | Wrist or chest vibration rhythm | Inhale–hold–exhale–hold cycles | Breathing pace adherence |
| Audio/visual breathing guides | App-based animation or sound cue | Box breathing, 4-7-8, coherent breathing | Subjective relaxation; HRV improvement |
| HRV-coupled breathing guides | Live HRV feedback + breathing prompt | Resonance frequency (~0.1 Hz) | HRV amplitude increase |
| Physical resistance devices | Mouthpiece with adjustable resistance | Slow, resistance-load breathing | Respiratory muscle training |
Evidence Notes
- Paced breathing at 5–6 breaths/min is associated with increases in high-frequency HRV and reductions in self-reported stress in multiple controlled studies [8, 18]
- Haptic-guided wrist devices offer portability with moderate protocol fidelity
- Device quality is not always matched by app quality — assess both independently
Meditation Wearables
Meditation wearables provide physiological feedback during or after meditation practice, supporting consistency and depth of practice through objective data.
| Device Category | Sensor Used | Feedback Type | Meditation Context |
| EEG headbands | Multi-electrode EEG | Real-time “calm/active” brain state indicators | Seated, eyes-closed meditation |
| HRV-feedback wearables | PPG or ECG | HRV trend during session | Breathing-focused meditation |
| Smart rings (sleep meditation) | PPG + accelerometer | Morning readiness + overnight recovery | Sleep-focused meditation routines |
| Multisensor smartwatch | PPG + EDA + accelerometer | Composite guided session scores | General mindfulness sessions |
Considerations
- EEG-based consumer headbands simplify complex neurological signals into binary calm/active states; clinical EEG is substantially more nuanced [7]
- Evidence that wearing a feedback device meaningfully deepens meditation practice compared to unassisted practice is limited [7]
- Devices may be most useful for beginners establishing a practice habit, or for users who benefit from objective anchoring during sessions
Breath Training Tools
Breath training tools focus specifically on developing respiratory capacity, rhythm, and control. They differ from guided breathing devices in that they typically target physiological adaptation over repeated sessions rather than acute stress response.
| Tool Type | Mechanism | Target Outcome | Evidence Strength |
| Inspiratory muscle trainers (IMT) | Resistance-load inhale | Respiratory strength, blood pressure management | Moderate–Strong [19] |
| CO₂ tolerance training tools | Breath-hold and pacing protocols | Improved hypercapnic response | Emerging |
| App-based breath training | Structured protocol progression | HRV improvement, stress resilience | Moderate [8] |
| Capnometry-guided respiration | End-tidal CO₂ monitoring | Optimal breathing rate calibration | Moderate–clinical [20] |
Evidence Context
- Inspiratory muscle training (IMT) has demonstrated blood pressure-lowering effects and some evidence for autonomic regulation improvement in published trials [19]
- Capnometry-guided respiratory intervention (CGRI) is primarily a clinical tool; limited consumer versions exist
- App-based training programs without hardware may be as effective as device-assisted protocols for otherwise healthy adults [8]
Top Stress Tracking Device Picks for 2026
| Category | Our Pick | Price Range | Why It Wins |
| Best overall | Garmin Forerunner 265 | $350–$450 | HRV trend, sleep, activity in one device; strong app ecosystem |
| Best ring | Oura Ring Gen3 | $299 + $6/mo | Finger PPG yields higher overnight HRV accuracy; no screen distraction |
| Best budget | Fitbit Sense 2 | $150–$200 | EDA + HRV + guided breathing; accessible entry point |
| Best HRV accuracy | Polar H10 + HRV4Training | $90–$120 | ECG-equivalent accuracy; preferred for athletes and research protocols |
| Best biofeedback | HeartMath Inner Balance | $129–$179 | HRV coherence training with structured protocol; strongest stress-reduction evidence alignment |
| Best for meditation | Muse S (EEG headband) | $349 | Real-time brain-state feedback; best for meditation habit formation |
Editorial selections are based on sensor accuracy, evidence alignment, and value at time of review. No affiliate relationships influence these recommendations. See About page for editorial standards.
Oura Ring vs. Apple Watch vs. WHOOP — Direct Comparison
| Feature | Oura Ring Gen3 | Apple Watch Series 9 | WHOOP 4.0 |
| HRV measurement | Overnight, finger PPG (high signal quality) | Spot-check + overnight, wrist PPG (moderate) | Continuous, wrist PPG (moderate) |
| Screen / display | None (app only) | Full display | None (app only) |
| Price | $299 device + $6/mo | $399–$499 device | Free device + $30/mo subscription |
| Battery life | 4–7 days | 18–36 hours | 4–5 days |
| Active real-time feedback | No | Yes (breathing, ECG spot-check) | No |
| Best for | Sleep quality, recovery, discretion | Broad wellness + notifications | Athletic recovery, training load |
| Subscription required | Yes | No | Yes (mandatory) |
Bottom line: Choose Oura Ring if overnight recovery data and discretion are your priority. Choose Apple Watch if you want the most versatile all-in-one device with active feedback. Choose WHOOP if you’re a serious athlete focused on training load management and are comfortable with a subscription model.
Choosing for Your Goals
TL;DR — Choosing for Your Goals
Match device type to goal before comparing brands. HRV biofeedback for stress reduction, chest strap for performance, EEG headband or HRV wearable for meditation, smartwatch or ring for general wellness.
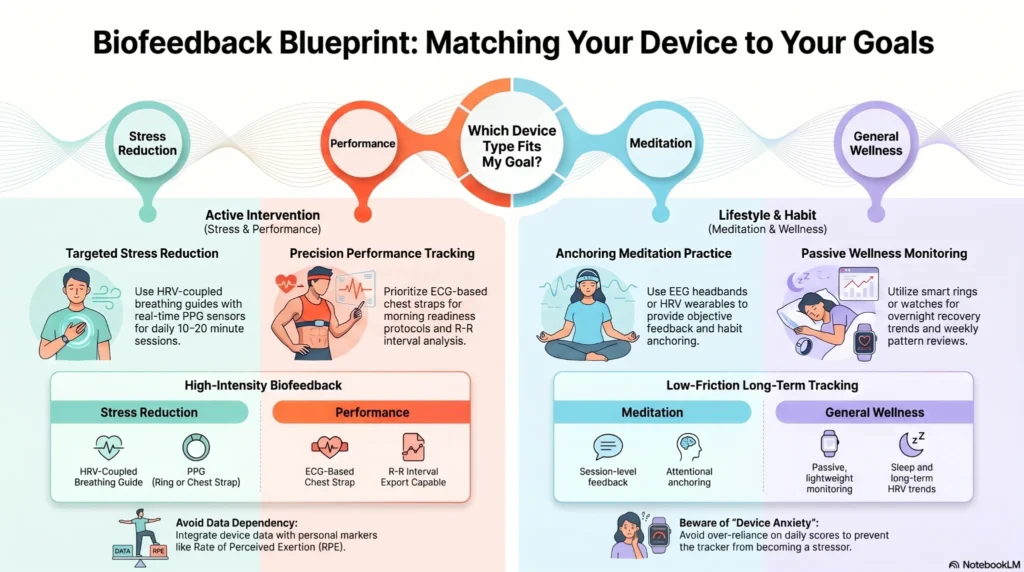
For Stress Reduction
| Criterion | Recommended Approach |
| Primary device type | HRV biofeedback device or HRV-coupled breathing guide |
| Key feature to prioritize | Real-time HRV feedback with structured breathing protocol |
| Sensor minimum | Reliable PPG (ring or chest strap preferred over wrist) |
| Session structure | Daily 10–20 minute biofeedback sessions; consistent timing |
| Evidence alignment | HRV biofeedback protocols have the strongest controlled-study support for stress symptom reduction [4, 5] |
| Secondary tool | Passive tracker (smartwatch or ring) to monitor overnight HRV trends |
| Provider guidance | Consider working with a licensed biofeedback practitioner — see About page for medical standards |
For Performance Optimization
| Criterion | Recommended Approach |
| Primary device type | Chest strap HRV monitor (ECG-based) + compatible app |
| Key feature to prioritize | Morning HRV readiness protocol; R-R interval export for trend analysis |
| Data focus | Tracking HRV trend relative to personal baseline; identifying overtraining or recovery deficit |
| Compatible apps | HRV4Training, Elite HRV, or similar research-aligned platforms |
| Secondary tool | Smart ring for overnight recovery and sleep quality monitoring |
| Caution | HRV alone is not a sufficient indicator for training load decisions; integrate with RPE and other recovery markers |
For Meditation Practice
| Criterion | Recommended Approach |
| Primary device type | EEG headband or HRV-coupled breathing wearable |
| Key feature to prioritize | Session-level feedback that supports attentional anchoring |
| Realistic expectation | Devices may support habit formation and provide objective anchoring; they do not replace practice depth |
| Session integration | Use device feedback as a post-session review, not a performance metric during meditation |
| Evidence note | Evidence for device-enhanced meditation is emerging; unassisted meditation has a substantially stronger evidence base [21] |
| App pairing | Select an app with a structured, protocol-based curriculum rather than passive mood logging |
For General Wellness
| Criterion | Recommended Approach |
| Primary device type | Smartwatch or smart ring with HRV, sleep, and activity monitoring |
| Key feature to prioritize | Sleep quality tracking; HRV trend over time; breathing and activity reminders |
| Data use | Weekly pattern review; identify correlations with lifestyle variables |
| Engagement approach | Lightweight; passive monitoring with periodic deliberate review |
| Avoid | Over-reliance on daily scores; device anxiety (“score-checking” as stressor) |
| Complement with | Behavioral strategies (sleep hygiene, regular movement, social connection) — device data supports, not replaces, these fundamentals |
Before You Buy: 5 Questions to Ask
“Will I actually use this?” Wearable abandonment is common. Start with a device category that matches your existing behavior — if you already wear a watch, upgrade to one with HRV tracking before committing to a dedicated biofeedback device. Most platforms offer 30-day free trials or return windows. Commit to one metric (HRV trend) and one month of check-ins before judging value.
“I already have an Apple Watch — do I need something else?” Not necessarily. For general stress awareness and sleep trend monitoring, Apple Watch covers most casual use cases. Consider adding a dedicated HRV tool only if you want higher accuracy (chest strap) or active biofeedback training (HeartMath Inner Balance or similar).
“Is this too complex for me?” If you’re new to wearables, start with a smartwatch — it covers 80% of general stress awareness needs with minimal setup. Chest straps and dedicated biofeedback devices require more intentional use (structured sessions, app configuration) and suit users who are ready to engage actively.
“Can I trust these scores?” Consumer device scores are trend indicators, not clinical measurements. A single HRV reading is less meaningful than your pattern over 2–4 weeks relative to your personal baseline. Use the data to notice patterns, not to make diagnostic judgments.
“Is it worth the price?” Compare device cost to the alternatives it may support or partially offset: a single session with a biofeedback therapist typically costs $100–$200. A 30-day return window eliminates the financial risk of the initial purchase. Most users find value within the first 2–4 weeks if they engage with the data consistently.
When to Consult a Healthcare Provider
TL;DR — When to Consult a Healthcare Provider
If your wearable data shows persistent abnormal patterns — not just single-day variation — and you have symptoms, that data belongs in a clinical conversation, not a wellness dashboard.
Educational framing only. This section does not constitute diagnostic or prescriptive guidance. It is provided in accordance with the medical oversight standards described on our About page.
The following situations indicate that wearable stress data should be discussed with a qualified healthcare provider rather than used as independent guidance:
| Situation | Reason for Provider Consultation |
| Persistent elevated resting heart rate or abnormal HRV patterns | May warrant cardiac or autonomic evaluation |
| Chronic, high-severity stress or anxiety symptoms | Requires clinical assessment; wearables are not a substitute for mental health care |
| Sleep disturbances beyond mild or occasional | May indicate sleep disorder requiring formal evaluation |
| Use of biofeedback devices as part of mental health or cardiac treatment | Should be overseen by licensed practitioners |
| Interpreting wearable data for any medical decision | Consumer devices are not clinically validated diagnostic tools |
| Concern about wearable data accuracy in context of known health conditions | Provider can contextualize device readings within your clinical picture |
Reminder: Stress tracking devices are consumer wellness tools. They are not medical devices approved for diagnosis, treatment, or management of any clinical condition unless explicitly stated and regulated as such.
For details on this page’s medical review process and editorial standards, see our About page.
References
- Georgiou K, et al. Can wearable devices accurately measure heart rate variability? A systematic review. Folia Medica. 2018;60(1):7–20. https://doi.org/10.2478/folmed-2018-0012
- Bent B, et al. The digital biomarker discovery pipeline: An open-source software platform for the development of digital biomarkers using mHealth and wearables data. Journal of Clinical and Translational Science. 2021;5(1):e169. https://doi.org/10.1017/cts.2021.808
- Shaffer F, Ginsberg JP. An overview of heart rate variability metrics and norms. Frontiers in Public Health. 2017;5:258. https://doi.org/10.3389/fpubh.2017.00258
- Lehrer PM, Gevirtz R. Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology. 2014;5:756. https://doi.org/10.3389/fpsyg.2014.00756
- Blase KL, van Wijk B, Zat Z, van Dijke A. HRV biofeedback as a stress management tool in occupational settings: Systematic review and narrative synthesis. Applied Psychophysiology and Biofeedback. 2021;46(2):111–130. https://doi.org/10.1007/s10484-020-09478-7
- Boucsein W. Electrodermal Activity. 2nd ed. Springer; 2012. https://doi.org/10.1007/978-1-4614-1126-0
- Lim J, et al. A systematic review of the effects of EEG neurofeedback on healthy and clinical populations. Journal of Psychiatric Research. 2019;119:48–56.
- Jerath R, Crawford MW, Barnes VA, Harden K. Self-regulation of breathing as a primary treatment for anxiety. Applied Psychophysiology and Biofeedback. 2015;40(2):107–115. https://doi.org/10.1007/s10484-015-9279-8
- Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Heart rate variability: Standards of measurement, physiological interpretation, and clinical use. Circulation. 1996;93(5):1043–1065.
- Billman GE. The LF/HF ratio does not accurately measure cardiac sympatho-vagal balance. Frontiers in Physiology. 2013;4:26. https://doi.org/10.3389/fphys.2013.00026
- Hernando D, et al. Validation of the Apple Watch for heart rate variability measurements during relax and mental stress in healthy subjects. Sensors. 2018;18(8):2619.
- Plews DJ, et al. Evaluating training adaptation with heart-rate measures: A methodological comparison. International Journal of Sports Physiology and Performance. 2013;8(6):688–691.
- Boucsein W, et al. Publication recommendations for electrodermal measurements. Psychophysiology. 2012;49(8):1017–1034. https://doi.org/10.1111/j.1469-8986.2012.01384.x
- Menghini L, et al. A standardized open-science framework for sharing and re-analyzing wrist-worn electrodermal activity data. PLOS ONE. 2020. https://doi.org/10.1371/journal.pone.0235338
- Smarr BL, Aschbacher K, Fisher SM, et al. Feasibility of continuous fever monitoring using wearable devices. Scientific Reports. 2020;10:21640. https://doi.org/10.1038/s41598-020-78481-9
- Massaroni C, et al. Contact-based methods for measuring respiratory rate. Sensors. 2019;19(4):908. https://doi.org/10.3390/s19040908
- Grossman P, Taylor EW. Toward understanding respiratory sinus arrhythmia: Relations to cardiac vagal tone, evolution and biobehavioral functions. Biological Psychology. 2007;74(2):263–285.
- Steffen PR, Austin T, DeBarros A, Brown T. The impact of resonance frequency breathing on measures of heart rate variability, blood pressure, and mood. Frontiers in Public Health. 2017;5:222. https://doi.org/10.3389/fpubh.2017.00222
- Craighead DH, et al. Time-efficient inspiratory muscle strength training lowers blood pressure and improves endothelial function. Journal of the American Heart Association. 2021;10(13):e020980. https://doi.org/10.1161/JAHA.121.020980
- Meuret AE, Ritz T. Hyperventilation in panic disorder and asthma: Empirical evidence and clinical strategies. International Journal of Psychophysiology. 2010;78(1):68–79. https://doi.org/10.1016/j.ijpsycho.2010.05.006
- Goyal M, et al. Meditation programs for psychological stress and well-being: A systematic review and meta-analysis. JAMA Internal Medicine. 2014;174(3):357–368. https://doi.org/10.1001/jamainternmed.2013.13018
Explore Further
Free resource: Download the stress tracking device comparison worksheet — a one-page decision guide you can fill in with your goals, budget, and preferences. [Download — enter email below]
Community resources for further research:
r/sleep — context for how stress tracking intersects with sleep quality improvement
r/biohacking and r/HRV on Reddit — active communities discussing real-world device experiences
HRV4Training YouTube channel — practitioner-level tutorials on interpreting HRV data
Medically reviewed by Dr. Rishav Das, M.B.B.S. — Wellness Device Data Analyst | Consumer Device Accuracy Specialist. See About page for full credentials, scope boundaries, editorial standards, and conflict of interest disclosures.
Last reviewed: 1st May, 2026 | Next scheduled review: 1st December, 2026





