Stress Metrics
Explained: What HRV, EDA, Stress Scores, and Body Battery Actually Mean
Understand your stress metrics. Learn to interpret HRV, EDA, and recovery scores from wearables like Garmin and Fitbit with this expert-reviewed guide.
🩺 Written & Reviewed by Dr. Rishav Das, M.B.B.S. Medical doctor · Wearable health data specialist ·
[See full credentials and editorial standards →] Last reviewed: May,2026
Medical Review: Reviewed according to the medical standards outlined on our editorial review standards
✅ Medically reviewed by Dr. Rishav Das, M.B.B.S. · Trusted by 50,000+ wearable users · Updated May,2026
⚡ TL;DR — Short on time?
Golden rule: Track trends over days, not single readings. Your baseline matters more than population averages.
HRV = how variable your heartbeats are. Lower than your baseline = more stress or less recovery.
Stress Score = a device estimate combining HRV, heart rate, and other signals. Not a diagnosis.
EDA = skin sweat response. Spikes signal arousal — positive or negative.
Body Battery / Recovery Score = estimated energy reserve. Green = go. Red = rest.
Introduction
Your Garmin shows a stress score of 78. Your HRV dropped overnight. Your Body Battery is in the red — and it’s only 9am. Sound familiar? You’re not alone.
Wearables now generate more physiological data than most people know how to act on. This guide cuts through the noise: what each stress metric actually measures, what “normal” looks like for you, and how to use the data without turning it into another source of anxiety.
This content is educational only and does not constitute medical advice. See our About page for [authorship credentials], [editorial standards], and [medical review processes].
Modern stress trackers measure biological signals that reflect the body’s autonomic nervous system response to physical and psychological demands. Each metric captures a different dimension of that response.
| What This Page Covers | What This Page Does Not Cover |
| How individual metrics are measured | Medical diagnosis or treatment recommendations |
| General population reference ranges | Device-specific clinical validation |
| Factors that influence readings | Individualized health advice |
| How to interpret trends, not single data points | Replacement for clinical assessment |
🩺 When to Consult a Healthcare Provider If you observe persistent, unexplained changes in any of the metrics described on this page — particularly resting heart rate, HRV, or breathing rate — consult a qualified healthcare provider. These metrics are educational indicators, not diagnostic tools. Refer to our [medical oversight framework] for the standards applied to this content.
This guide is for:
💼 Professionals managing burnout — you’re using your wearable to catch stress before it catches you.
📊 Wearable owners confused by their data — you have the device; you want to understand the numbers.
🏃 Fitness enthusiasts optimising recovery — you track training load and want HRV and Body Battery to actually mean something.
Which Stress Metrics Should I Track?
Not sure where to start? Match your goal to the metrics that matter most.
| Your Goal | Focus On | Skip (for now) |
|---|---|---|
| Manage burnout or chronic stress | HRV trend + Resting Heart Rate | EDA (too context-dependent) |
| Optimise athletic recovery | Body Battery + HRV + RHR | Breathing rate (secondary) |
| Reduce anxiety | EDA + Breathing metrics + HRV | Stress score (too broad) |
| General wellness awareness | Stress Score + Body Battery | Advanced HRV metrics |
| Beginner — just getting started | Resting Heart Rate + HRV | Everything else — add later |
👉 Not sure which device tracks these best? [See our Device Comparison Guide →]
New to stress tracking? Start here.
Forget everything else for now. Track just two metrics: Resting Heart Rate and HRV. These two give you 80% of the actionable signal. Everything else adds context once you have a baseline.
- Stress MetricsExplained: What HRV, EDA, Stress Scores, and Body Battery Actually Mean
- ⚡ TL;DR — Short on time?
- Introduction
- This guide is for:
- Which Stress Metrics Should I Track?
- New to stress tracking? Start here.
- Heart Rate Variability (HRV) for Stress
- Stress Scores and Algorithms
- Electrodermal Activity (EDA)
- Breathing Metrics
- Resting Heart Rate Changes
- Body Battery and Recovery Scores
- Using Data Without Creating More Stress
- What to Read Next
- Common Concerns Before You Start Tracking
- Frequently Asked Questions
- References
Heart Rate Variability (HRV) for Stress
Heart Rate Variability (HRV) is one of the most researched non-invasive markers of autonomic nervous system function. It refers to the variation in time between consecutive heartbeats, measured in milliseconds (ms).
What HRV Indicates About Stress
HRV reflects the balance between sympathetic (“fight or flight”) and parasympathetic (“rest and digest”) branches of the autonomic nervous system (ANS).
| ANS State | Typical HRV Pattern | Associated Condition |
| Parasympathetic dominant | Higher HRV | Rest, recovery, low perceived stress |
| Sympathetic dominant | Lower HRV | Acute stress, exertion, illness |
| Balanced / mixed | Moderate HRV | Normal daily activity |
| Chronically dysregulated | Consistently low HRV | Burnout, overtraining, chronic stress (evidence-based association, not diagnostic) |
Key distinctions supported by evidence:
- HRV is not a direct measure of stress — it is a measure of autonomic flexibility
- A single low HRV reading is less meaningful than a trend over days or weeks
- HRV is influenced by both psychological and physiological stressors
- Higher HRV is generally, though not universally, associated with better cardiovascular and psychological resilience (Shaffer & Ginsberg, 2017)
⚠️ Evidence Note: The association between higher HRV and improved health outcomes is well-documented in clinical populations. Generalizing these findings to healthy consumer populations warrants caution.
What Is a Good HRV Score for Your Age? (Reference Ranges Explained)
There is no single “optimal” HRV value. Reference ranges vary significantly by:
- Age
- Biological sex
- Fitness level
- Measurement method (RMSSD, SDNN, etc.)
- Time of measurement (morning vs. during activity)
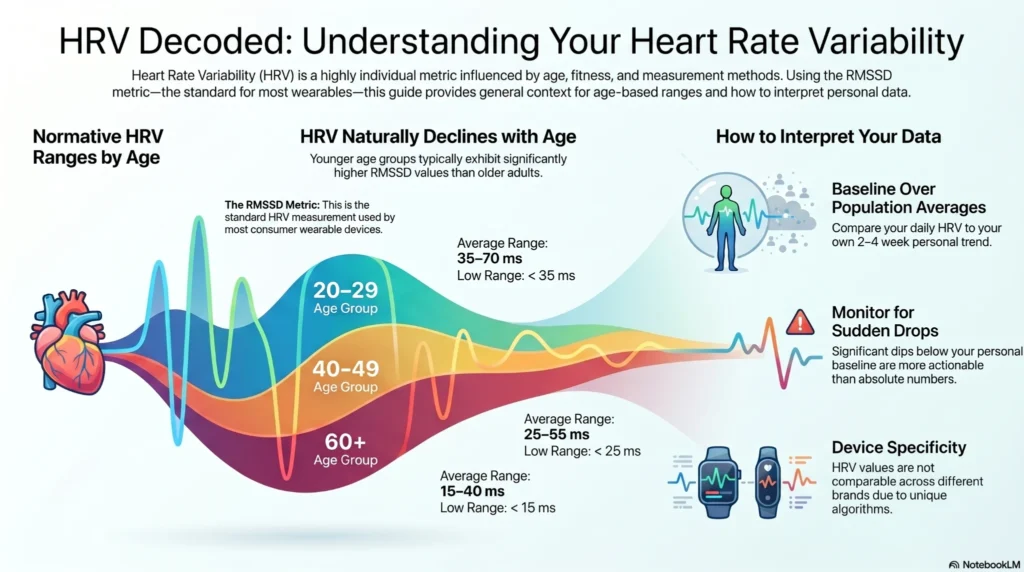
General RMSSD Reference Ranges by Age Group (RMSSD — the most common HRV number reported by consumer wearables. In plain terms: how much does the gap between your heartbeats vary? A higher number generally means your nervous system is more flexible and better recovered.)
| Age Group | Low Range (ms) | Average Range (ms) | High Range (ms) |
| 20–29 | < 35 | 35–70 | > 70 |
| 30–39 | < 30 | 30–65 | > 65 |
| 40–49 | < 25 | 25–55 | > 55 |
| 50–59 | < 20 | 20–50 | > 50 |
| 60+ | < 15 | 15–40 | > 40 |
Source: Normative data adapted from Nunan et al. (2010), published in Annals of Noninvasive Electrocardiology. Device-reported HRV values may differ from clinical ECG-derived measurements.
Important interpretation notes:
- Compare your HRV to your own baseline, not population averages
- Most devices establish a personal baseline over 2–4 weeks of consistent wear
- Sudden drops below your personal baseline are more actionable than absolute numbers
- Devices use different algorithms; values are not directly comparable across brands
📊 Did you know? Average HRV declines by roughly 15ms between ages 20–60. But your personal baseline at any age matters far more than where you sit on the population chart.
Factors That Affect HRV
HRV is highly sensitive. Many variables beyond psychological stress influence readings.
Factors Associated with Lower HRV:
| Category | Examples |
| Physical stressors | Illness, fever, overtraining, dehydration, alcohol consumption |
| Psychological stressors | Acute anxiety, work pressure, poor sleep quality |
| Environmental | High altitude, heat, air quality |
| Biological | Aging, hormonal changes (menstrual cycle phase), medication side effects |
| Measurement artifacts | Device fit, body position, movement during measurement |
Factors Associated with Higher HRV:
| Category | Examples |
| Lifestyle | Regular aerobic exercise (long-term adaptation), adequate sleep, relaxation practices |
| Behavioral | Breathing exercises, meditation (evidence varies in magnitude) |
| Physiological | Cardiovascular fitness, healthy body weight |
| Measurement | Morning, supine position, consistent measurement timing |
Sources: Thayer et al. (2012); Laborde et al. (2017)
How to Use Your HRV Data to Manage Stress: A Practical Framework
Recommended practice framework:
| Step | Action | Rationale |
| 1. Establish baseline | Wear device consistently for 2–4 weeks without behavioral changes | Personalized context is more useful than population norms |
| 2. Track morning readings | Measure at the same time daily (ideally post-sleep, pre-activity) | Reduces measurement variability |
| 3. Log context | Note sleep, exercise, stress events, alcohol, illness | Enables pattern identification |
| 4. Look for trends | Focus on 7–14 day rolling averages, not daily fluctuations | Single-point data is noisy |
| 5. Respond, don’t react | Use a sustained downward trend as a prompt for recovery, not alarm | Prevents metric-induced anxiety |
| 6. Consult a provider | If sustained low HRV accompanies symptoms (fatigue, chest discomfort, mood changes) | HRV alone is not diagnostic |
📬 Get the free 7-Day Stress Tracking Starter Guide Includes: a printable metric log template, your first-week baseline protocol, and a plain-English glossary of every metric on this page. [Enter your email → Send me the guide] No spam. Unsubscribe anytime. Sent once.
🏆 Best devices for HRV tracking
Apple users: Apple Watch Series 9 — reports raw HRV (ms) without a composite score.
Most accurate (consumer): WHOOP 4.0, Oura Ring Gen 3 — continuous overnight HRV with strong baseline algorithms.
Best value: Garmin Venu 2 / Forerunner series — reliable RMSSD measurement at a lower price point.
[→ See our full HRV Monitor Comparison — accuracy, comfort, and price tested across 8 devices]
Stress Scores and Algorithms
Consumer wearables from brands such as Garmin, Fitbit, Samsung, and others aggregate multiple physiological signals into a single “stress score.” These scores are proprietary, device-specific, and represent an estimation — not a clinical measurement.
How Devices Calculate Stress Scores

While exact algorithms are proprietary and not publicly disclosed by most manufacturers, stress scores are generally derived from a combination of:
| Input Signal | What It Captures |
| HRV (typically RMSSD or LF/HF ratio) | Autonomic nervous system balance |
| Resting heart rate deviation | Elevation above personal baseline |
| Skin temperature variation | Thermoregulatory stress response |
| Movement / accelerometry | Activity vs. sedentary state context |
| Sleep data | Recovery quality from prior night |
| Electrodermal activity (select devices) | Sympathetic arousal events |
Common score output formats:
| Device / Platform | Score Range | Low Stress | High Stress |
| Garmin (Stress Level) | 0–100 | 0–25 | 76–100 |
| Fitbit (Stress Management Score) | 1–100 | 70–100 (higher = better managed) | 1–39 |
| Samsung (Stress) | 0–100 | 0–39 | 80–100 |
| Apple (Heart Rate Variability — proxy) | No stress score; HRV reported directly | Higher ms = generally positive | Lower ms = generally lower recovery |
Note: Score scales are not standardized. Always interpret within your device’s own framework.
📊 Quick fact: A stress score of 70 on a Garmin means something completely different from a 70 on a Fitbit. These scales are not interchangeable — always read within your own device’s framework.
Interpreting Your Stress Score
Core interpretation principles:
- Stress scores reflect estimated physiological load, not psychological experience
- A high score during exercise is expected and does not indicate harmful stress
- Context is essential: the same score means different things during sleep, work, or a workout
- Most devices provide real-time and day-level stress summaries — these serve different purposes
Contextual interpretation guide:
| Scenario | Expected Score Range | Interpretation Note |
| Vigorous exercise | High (60–100 range, device-dependent) | Physiological load — expected, not harmful |
| Deep, restful sleep | Very low (0–25) | Parasympathetic recovery state |
| Sedentary but anxious | Moderate to elevated | May reflect psychological arousal without movement |
| Illness or infection | Elevated, even at rest | Immune-system physiological demand |
| Chronic elevation at rest | Consistently elevated baseline | May warrant review of sleep, recovery, lifestyle — and provider consultation if persistent |
Limitations of Stress Algorithms
| Limitation | Explanation |
| Proprietary opacity | Algorithm details are not publicly available for independent validation. (see our device testing and validation methodology for how this site approaches accuracy assessment) |
| Sensor accuracy variation | Optical heart rate sensors are less accurate during high movement or poor skin contact |
| Population generalizability | Training datasets may not represent all demographics equally (age, skin tone, fitness level) |
| No psychological input | Algorithms cannot capture emotional context, perceived stress, or cognitive load |
| Cross-device incomparability | Scores cannot be meaningfully compared across brands or even device generations |
| Not clinically validated | Consumer stress scores are not approved diagnostic tools by regulatory bodies such as the FDA |
| Feedback loop risk | Viewing a high stress score may itself increase perceived stress (nocebo-adjacent effect) |
Source: Bent et al. (2020) — accuracy assessment of consumer wearables for physiological monitoring.
⚠️ Evidence Note: Research on consumer wearable accuracy for stress scoring in free-living conditions is still emerging. Claims about accuracy should be stated conservatively.
Electrodermal Activity (EDA)
Electrodermal activity (EDA) — also called galvanic skin response (GSR) or skin conductance — measures changes in the electrical properties of the skin driven by eccrine sweat gland activity. It is controlled by the sympathetic nervous system.
Consumer devices that measure EDA include: Fitbit Sense/Sense 2, Empatica E4, and select research-grade wearables.
What Skin Conductance Measures
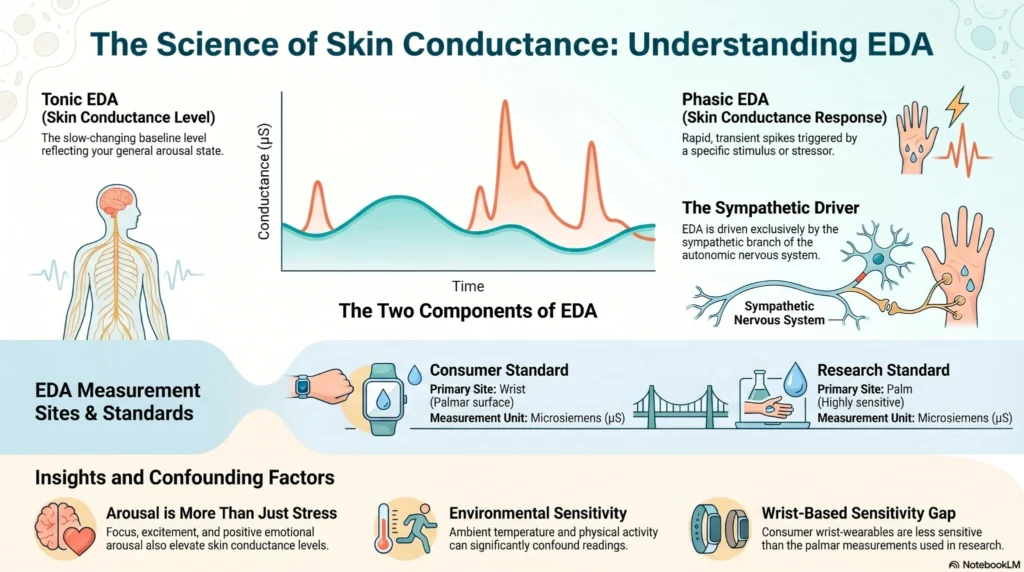
| Component | Description |
| Tonic EDA (SCL — Skin Conductance Level) | The slow-changing baseline level of skin conductance; reflects general arousal state |
| Phasic EDA (SCR — Skin Conductance Response) | Rapid, transient spikes in conductance in response to a specific stimulus or stressor |
| Unit of measurement | Microsiemens (µS) |
| Primary measurement site (consumer) | Wrist (palmar surface preferred in research but impractical for wearables) |
| What increases conductance | Greater sweat gland activity, driven by sympathetic nervous system activation |
Key physiological facts:
- EDA is driven exclusively by the sympathetic branch of the ANS
- EDA responses are not exclusively linked to negative stress — excitement, focus, and positive emotional arousal also elevate EDA
- Wrist-based EDA measurement (consumer devices) is less sensitive than palmar measurement (research standard)
- Ambient temperature and physical activity can confound readings
EDA and Emotional Arousal
EDA responses are associated with emotional and cognitive arousal, not stress specifically.
| EDA Trigger Category | Example | EDA Response |
| Psychological stressor | Difficult conversation, deadline pressure | Elevated SCL + multiple SCRs |
| Positive emotional arousal | Exciting news, anticipation | Similar pattern to stress response |
| Cognitive engagement | Problem-solving, focused attention | Moderate SCL elevation |
| Startle / sudden stimulus | Loud noise | Sharp, transient SCR |
| Physical exertion | Exercise, heat exposure | Elevated SCL (confound) |
| Calm, low-arousal state | Rest, relaxation | Low SCL, minimal SCRs |
Clinical and research context:
- EDA has been studied in the context of anxiety disorders, PTSD, and autonomic dysfunction (Critchley, 2002)
- In consumer wellness contexts, EDA is most useful as a relative indicator of arousal moments, not an absolute stress measurement
- Research-grade EDA is used in clinical biofeedback, cognitive neuroscience, and psychophysiology — consumer applications are a simplified proxy
⚠️ Evidence Note: Direct clinical extrapolation from research-grade EDA findings to consumer wrist-based EDA should be stated with caution. Wrist sensor accuracy vs. palmar measurement is an active area of device validation research.
Biofeedback Applications
EDA is one of the oldest biofeedback modalities, with a substantial research history.
How EDA biofeedback is used:
| Application | Description | Evidence Level |
| Stress awareness training | Observing real-time EDA spikes to identify personal stress triggers | Emerging evidence in consumer context |
| Anxiety management | Clinical biofeedback using EDA to train relaxation responses | Moderate evidence in clinical settings (Lehrer & Gevirtz, 2014) |
| Attention and focus training | EDA patterns used in neurofeedback-adjacent protocols | Limited; primarily research settings |
| Consumer wellness apps | Daily EDA summaries, “calm” session tracking (e.g., Fitbit EDA Scan) | Validation against clinical standards is limited |
Practical use guidance:
- Use EDA trend data to identify patterns, not to interpret individual readings
- Sessions should be taken in consistent conditions (same time, position, ambient temperature)
- EDA data is most meaningful when combined with context logging (what you were doing, thinking, or feeling)
- Consumer EDA features are not equivalent to clinical biofeedback therapy
🏆 Best devices for EDA tracking
- Consumer: Fitbit Sense 2 — most accessible wrist-based EDA with daily EDA Scan sessions.
- Research-grade: Empatica E4 — clinical standard if accuracy is critical.
[→ See our EDA Device Comparison]
Breathing Metrics
Breathing pattern is one of the most directly modifiable physiological signals. Several wearables and dedicated devices now track respiratory rate and breathing rhythm as stress-related metrics.
Respiratory Rate and Stress
Respiratory rate (RR) is the number of breaths taken per minute.
| Reference Category | Breaths Per Minute | Context |
| Normal adult resting rate | 12–20 | General adult population (NIH reference) |
| Relaxed / meditative | 4–8 | Deep, intentional breathing; below normal resting |
| Stress or anxiety response | 20–30+ | Acute psychological or physical stress |
| Clinical concern thresholds | < 8 or > 25 at rest | Requires clinical evaluation — this is not a consumer metric target |
How wearables measure respiratory rate:
| Method | Description | Common Devices |
| Photoplethysmography (PPG) variation | Detects respiratory-induced heart rate fluctuations | Fitbit, Apple Watch, Garmin |
| Accelerometry | Detects chest/wrist movement patterns during breathing | Some fitness trackers |
| Bioimpedance | Measures electrical impedance changes with breathing | Garmin (select models) |
| Dedicated chest strap | Direct respiratory movement measurement | Polar, research devices |
Stress-breathing relationship:
- Psychological stress activates the sympathetic nervous system, which is associated with faster, shallower breathing (hyperventilation tendency)
- Chronic stress may be associated with habitually elevated resting respiratory rate
- Changes in respiratory rate during sleep may reflect physiological stress load
Breathing Patterns
Different breathing patterns produce measurably different physiological effects.
| Pattern | Characteristics | Associated State | HRV Effect |
| Eupnea (normal resting) | 12–20 BPM, variable depth | Neutral, awake state | Baseline |
| Thoracic (chest) breathing | Shallow, upper-chest dominant | Common in stress, anxiety | May reduce HRV |
| Diaphragmatic breathing | Deep, abdomen-led expansion | Relaxed, intentional | May increase HRV |
| Hyperventilation | > 20 BPM, shallow | Acute anxiety, panic | Disrupts HRV |
| Hypoventilation | < 10 BPM (intentional) | Breath-retention practices | Varies by context |
| Coherent / resonance breathing | 4.5–6 BPM, rhythmic | Deliberate stress reduction | Associated with HRV increase (see below) |
Sources: Jerath et al. (2015); Telles et al. (2013)
Coherent Breathing
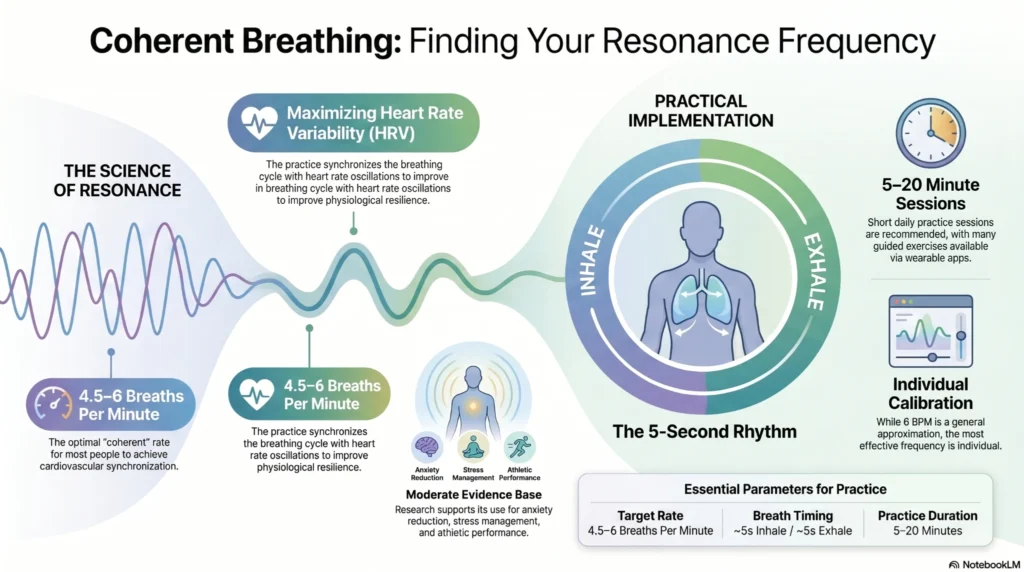
Coherent breathing (also called resonance frequency breathing or cardiac coherence) refers to breathing at a rate of approximately 4.5–6 breaths per minute in a rhythmic, even pattern.
| Parameter | Detail |
| Target rate | ~5–6 breaths per minute (approximately 5-second inhale / 5-second exhale) |
| Mechanism (proposed) | Synchronizes breathing cycle with heart rate oscillations, maximizing HRV |
| Duration studied | Sessions of 5–20 minutes in published research |
| Evidence base | Moderate — multiple RCTs; effect sizes vary (Lehrer & Gevirtz, 2014) |
| Applications | Anxiety reduction, stress management, athletic performance — research contexts |
| Consumer availability | Guided via apps (e.g., Garmin Breathing Exercises, Apple Mindfulness, dedicated apps) |
| Limitations | Optimal frequency is individual; 6 BPM is a general approximation |
Practical guidance:
- Many wearable apps include guided breathing exercises based on coherent breathing principles
- Short daily practice sessions (5–10 minutes) have been studied — evidence is promising but not conclusive for all outcomes
- Breathing exercises are a low-risk wellness practice; they are not a clinical treatment
- Users with respiratory conditions should consult a provider before beginning structured breathing protocols
⚠️ Evidence Note: The magnitude of HRV increase from coherent breathing varies significantly across studies and populations. Claims should avoid suggesting guaranteed or large effect sizes.
Resting Heart Rate Changes
Resting heart rate (RHR) is the number of heartbeats per minute when the body is at complete rest, typically measured in the morning before rising.
Reference ranges:
| Category | RHR (BPM) | Notes |
| Athletic | 40–60 | Common in highly trained endurance athletes |
| Normal adult | 60–100 | American Heart Association reference range |
| Elevated resting | > 100 | Warrants clinical evaluation (tachycardia threshold) |
| Low resting | < 40 | Warrants evaluation if symptomatic |
Source: American Heart Association (2023)
RHR as a daily stress and recovery indicator:
| Observation | Possible Association | Action |
| RHR 3–5 BPM above personal baseline | Incomplete recovery, physiological stress load | Consider additional rest; monitor trend |
| RHR consistently elevated for > 3–5 days | Overtraining, illness, chronic stress (possible) | Reduce training load; consult provider if other symptoms present |
| RHR at or below baseline | Good recovery, low physiological stress | Baseline maintained |
| Sudden large spike (> 10 BPM above baseline) | Acute illness, fever, dehydration, extreme stress | Monitor closely; consult provider if sustained or symptomatic |
Contextual variables that affect RHR:
- Hydration status
- Caffeine and alcohol consumption
- Medications (particularly beta-blockers, stimulants)
- Illness or fever
- Ambient temperature
- Emotional state at measurement time
- Time of day (RHR is lowest in early morning)
Key principle: Like HRV, individual baselines are more meaningful than population averages. Consistent morning measurement (same position, same device) is essential for trend accuracy.
Real-world example A 41-year-old project manager noticed her resting heart rate climbing 6–8 BPM above her baseline for five consecutive days — with no change in exercise or sleep duration. The pattern preceded her recognising burnout symptoms by about a week. Having an objective, trended data point gave her a concrete reason to take a rest week rather than push through. She didn’t need a doctor’s appointment to act — she needed a clear signal she could trust.
Body Battery and Recovery Scores
Body Battery (Garmin) and similar energy/recovery scores (WHOOP Recovery, Oura Readiness Score) are composite metrics designed to estimate available physiological energy and recovery status.
Energy Level Estimation
These scores integrate multiple signals to produce a single readiness indicator.
| Platform | Metric Name | Score Range | Key Inputs |
| Garmin | Body Battery | 0–100 | HRV, sleep quality, activity, stress level |
| WHOOP | Recovery Score | 0–100% | HRV, RHR, sleep performance, respiratory rate |
| Oura | Readiness Score | 0–100 | HRV, RHR, sleep, body temperature, activity balance |
| Fitbit | Daily Readiness Score | 1–100 | HRV, sleep, activity history |
| Apple Health | No composite score | — | Surfaces individual metrics (HRV, RHR, sleep) separately |
How scores are depleted and restored:
| Depletes Score | Restores Score |
| Physical exercise (intensity-dependent) | Quality sleep (deep + REM stages) |
| High stress periods | Low-intensity movement / active recovery |
| Poor sleep quality or duration | Rest and downtime |
| Illness or physiological stress | Hydration, nutrition, stress reduction |
| Alcohol consumption | Consistent recovery behaviors over time |
Recovery Tracking
Interpreting composite recovery scores:
| Score Zone | Interpretation | General Guidance |
| High (70–100 / Green) | Strong physiological recovery indicated | Suited for higher-intensity activity |
| Moderate (40–69 / Yellow) | Partial recovery | Moderate activity; monitor closely |
| Low (0–39 / Red) | Limited recovery indicated | Prioritize rest and recovery behaviors |
Important caveats:
- These scores are estimates derived from population models — individual accuracy varies
- Scores are influenced by sensor quality, device wear consistency, and individual physiology
- The absence of a high score does not mean a person is unfit to exercise — subjective feel and context matter
- Long-term trends (weekly averages) are more informative than single-day readings
- None of these scores are clinically validated diagnostic tools
🏆 Which recovery platform is right for you?
- Best for athletes: WHOOP 4.0 — strain + recovery optimised for performance tracking.
- Best for sleep + wellness: Oura Ring Gen 3 — passive wear, detailed sleep staging.
- Best all-round: Garmin (Venu / Fenix series) — broadest metric set, longest battery life.
- Already have an iPhone? Apple Health surfaces HRV and RHR without a subscription.
[→ Not sure? Take our 3-question device matcher →] (answers in 60 seconds)
Using Data Without Creating More Stress
Healthy Relationship with Metrics
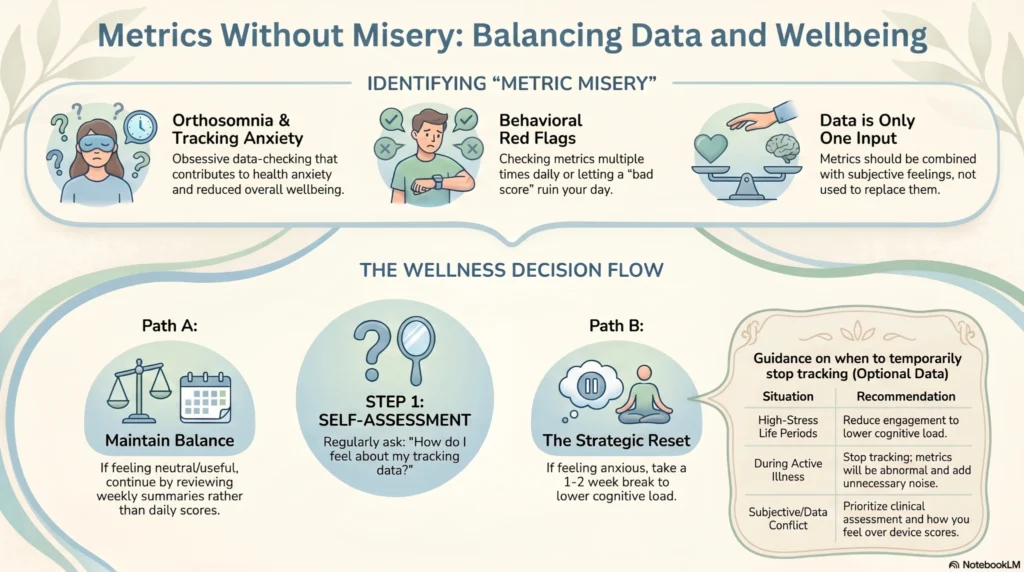
A growing body of behavioral research suggests that intensive health self-monitoring can, in some individuals, contribute to health anxiety, obsessive data-checking, and reduced wellbeing — an effect sometimes called “orthosomnia” in the context of sleep tracking.
Principles for metric-aware wellness:
| Principle | Description |
| Trends over data points | A single low HRV or elevated RHR reading carries limited standalone meaning |
| Context over scores | How you feel, your sleep, and your recent activity explain most daily metric variation |
| Action, not alarm | Data should prompt reasonable behavior adjustments, not anxiety or excessive intervention |
| Scheduled check-ins | Review weekly summaries rather than checking metrics multiple times daily |
| Data as one input | Combine metric data with subjective wellbeing — both matter |
| Recognize confounds | Know which factors temporarily affect your metrics (travel, alcohol, illness, cycle phase) |
Signs that tracking may be adding stress rather than reducing it:
- Checking metrics multiple times per day and experiencing anxiety about readings
- Adjusting behavior significantly based on a single data point
- Feeling that a “bad score” has ruined a day before it has started
- Persistent worry about metrics despite no clinical symptoms
- Difficulty feeling well without metric confirmation
🩺 Note: If engagement with health data is significantly impacting your mental health or daily functioning, speaking with a healthcare provider or mental health professional is recommended. This content is educational. See our [medical oversight framework] for the standards guiding this recommendation.
When to Take Breaks from Tracking
| Situation | Recommendation |
| Experiencing metric-induced anxiety | Consider a structured break (1–2 weeks); reassess whether tracking is adding value |
| During high-stress life periods | Reducing data engagement may lower cognitive load |
| After establishing a clear personal baseline | Less frequent review may be equally effective once patterns are understood |
| During illness | Metrics will be abnormal — tracking adds noise without useful signal |
| When subjective wellbeing and data consistently conflict | Consider consulting a provider; prioritize clinical assessment over device scores |
Returning to tracking productively:
- Set a consistent review schedule (e.g., weekly summary review only)
- Focus on 2–3 metrics most relevant to your goals, not all available data
- Use data to support decisions, not to make decisions autonomously
What to Read Next
Not sure which tracker to buy?
Our unbiased device comparison tests accuracy, comfort, battery life, and value across 8 top models — including Garmin, WHOOP, Oura, Fitbit, and Apple Watch. [→ Compare Stress Trackers Now]
Want the best HRV accuracy?
We tested HRV measurement consistency across 6 devices against a clinical ECG reference. See which wearables come closest. [→ See the Best HRV Monitors]
Not sure where to start?
Answer 3 questions and we’ll recommend the right device for your goals, budget, and lifestyle. [→ Take the Device Matcher Quiz (60 seconds)]
[← Back to Stress & Wellness Tracking Overview]
Common Concerns Before You Start Tracking
Do I need an expensive device to track my stress effectively? No. Devices in the £130–£250 range — such as the Fitbit Charge 6 or Garmin Venu Sq 2 — provide reliable HRV and resting heart rate measurement. These are the two most actionable metrics for most people. Premium devices (WHOOP, Oura Ring) add incremental accuracy and detail, but they don’t give you fundamentally different information for general stress tracking.
Is my health data private? Who can see my stress and HRV readings? Health data stays on your device and the manufacturer’s app unless you explicitly share it. Major platforms (Garmin Connect, Fitbit/Google Health, Apple Health) allow you to manage data sharing in Settings. None sell your individual biometric data to third parties under current privacy regulations (GDPR / CCPA). For full detail, check your device manufacturer’s privacy policy. Avoid syncing health apps to third-party platforms you haven’t vetted.
This all looks very technical — is it really for someone like me? Yes. You only need to watch two numbers to start: your resting heart rate and your HRV trend. If both are near your normal baseline, you’re recovered. If both are lower than usual for several days, your body is under load. Everything else on this page is context — come back to it when you’re ready.
Frequently Asked Questions
References
American Heart Association. (2023). All About Heart Rate (Pulse). https://www.heart.org/en/health-topics/high-blood-pressure/the-facts-about-high-blood-pressure/all-about-heart-rate-pulse
Shaffer, F., & Ginsberg, J. P. (2017). An overview of heart rate variability metrics and norms. Frontiers in Public Health, 5, 258. https://doi.org/10.3389/fpubh.2017.00258
Nunan, D., Sandercock, G. R. H., & Brodie, D. A. (2010). A quantitative systematic review of normal values for short‐term heart rate variability in healthy adults. Pacing and Clinical Electrophysiology, 33(11), 1407–1417. https://doi.org/10.1111/j.1540-8159.2010.02841.x
Thayer, J. F., Åhs, F., Fredrikson, M., Sollers, J. J., & Wager, T. D. (2012). A meta-analysis of heart rate variability and neuroimaging studies: Implications for heart rate variability as a marker of stress and health. Neuroscience & Biobehavioral Reviews, 36(2), 747–756. https://doi.org/10.1016/j.neubiorev.2011.11.009
Laborde, S., Mosley, E., & Thayer, J. F. (2017). Heart rate variability and cardiac vagal tone in psychophysiological research — Recommendations for experiment planning, data analysis, and data reporting. Frontiers in Psychology, 8, 213. https://doi.org/10.3389/fpsyg.2017.00213
Bent, B., Goldstein, B. A., Kibbe, W. A., & Dunn, J. P. (2020). Investigating sources of inaccuracy in wearable optical heart rate sensors. NPJ Digital Medicine, 3(1), 18. https://doi.org/10.1038/s41746-020-0226-6
Critchley, H. D. (2002). Electrodermal responses: What happens in the brain. The Neuroscientist, 8(2), 132–142. https://doi.org/10.1177/107385840200800209
Lehrer, P. M., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, 756. https://doi.org/10.3389/fpsyg.2014.00756
Jerath, R., Crawford, M. W., Barnes, V. A., & Harden, K. (2015). Self-regulation of breathing as a primary treatment for anxiety. Applied Psychophysiology and Biofeedback, 40(2), 107–115. https://doi.org/10.1007/s10484-015-9279-8
Telles, S., Singh, N., & Balkrishna, A. (2013). Heart rate variability changes during high frequency yoga breathing and breath awareness. BioPsychoSocial Medicine, 7(1), 4. https://doi.org/10.1186/1751-0759-7-4
Medical Disclaimer: The information on Wearable Wellness Guide is for educational purposes and should not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis, treatment, or medical device recommendations tailored to your individual health needs. See our [funding and conflict of interest disclosures].
Written by: Dr. Rishav Das, M.B.B.S. —See full credentials on our About page
Medical Review: Dr. Rishav Das, M.B.B.S. — reviewed according to the medical standards outlined on our About page
Last Reviewed: 10th May, 2026
