Sleep Metrics Explained: What Your Fitbit, Oura & Apple Watch Data Really Means (2026 Guide)
Decode your sleep tracker data with a physician reviewed guidance on sleep metrics. Learn about sleep stages, scores, HRV, and SpO2 to help you identify patterns, improve rest, and know when to see a doctor.
Written by: Dr. Rishav Das, M.B.B.S.
Medical Reviewer & Authority: Dr. Rishav Das, M.B.B.S., Post-Graduate Certificate in Health Informatics (Columbia University)
For complete credentials and scope of authority, see our About page.
Last Updated: February 7, 2026
Why You’re Reading This
You’re here because your sleep tracker is confusing you. Maybe:
✗ Your sleep score says “poor” but you actually feel fine
✗ You’re getting 9 hours in bed but still wake up exhausted
✗ Your HRV dropped 30 points overnight and you don’t know if you should be worried
✗ Your partner snores loudly but your tracker shows zero breathing disruptions
✗ You can’t figure out which numbers actually matter
You’re not alone. 65% of sleep tracker users report confusion about what their data means. This guide translates your Fitbit, Oura Ring, or Apple Watch data into insights you can actually use.
Sleep Metrics at a Glance
| Metric | Normal Range | When to Act | How Controllable? |
|---|---|---|---|
| Sleep Efficiency | >85% | <80% for 2+ weeks | High — sleep hygiene helps |
| Deep Sleep % | 10-25% (declines with age) | <10% consistently | Medium — temperature, alcohol impact |
| REM Sleep % | 15-25% | <10% or >30% consistently | Medium — stress, timing affect |
| Sleep Latency | <20 minutes | >30 minutes regularly | High — routine changes help |
| HRV | Age/fitness dependent (see chart below) | Declining >20% over 2 weeks | Medium — lifestyle factors |
| AHI | <5 events/hour | >5 events/hour | Low — may need medical intervention |
| SpO2 | >95% | <90% or frequent dips | Low — indicates breathing issues (pulse oximetry accuracy at elevation) |
Clinical significance of respiratory rate monitoring
Comprehensive meta-analysis of normal sleep patterns across ages
Understanding Sleep Data to Improve Your Rest
Modern sleep tracking devices provide detailed metrics about sleep patterns, breathing patterns, and recovery indicators. Learning how to read sleep data and understanding these measurements may help individuals identify patterns and make informed decisions about sleep hygiene. This page explains common sleep metrics, their clinical relevance, and limitations of consumer-grade tracking technology.
⚠️ EDUCATIONAL RESOURCE ONLY: This content does not replace professional medical evaluation. Consult a healthcare provider for diagnosis or treatment of sleep disorders.
- Sleep Metrics Explained: What Your Fitbit, Oura & Apple Watch Data Really Means (2026 Guide)
- Why You're Reading This
- Sleep Metrics at a Glance
- Understanding Sleep Data to Improve Your Rest
- How to Use This Guide
- TL;DR — 60-Second Summary
- ⚠️ Should You Even Track Your Sleep?
- What Are Sleep Stages and Why Do They Matter?
- Sleep Duration vs. Sleep Quality
- Sleep Scores and Algorithms
- Apnea-Hypopnea Index (AHI): Understanding Your Sleep Apnea Risk
- Blood Oxygen (SpO2)
- Heart Rate Variability (HRV) Explained: What's a Good HRV for Your Age?
- Respiratory Rate
- Sleep Latency
- Circadian Alignment
- Sleep Hygiene and Environmental Factors
- Using Sleep Metrics Responsibly
- Limitations of Consumer Sleep Tracking
- How Accurate Is Your Sleep Tracker? (What Studies Show)
- Your Sleep Optimization Priority Matrix
- FrequentlyAsked Sleep Tracker Questions
- 1. Why does my sleep score vary so much day to day?
- 2. Is 6 hours of "excellent" sleep better than 8 hours of "poor" sleep?
- 3. Can I trust my Fitbit/Oura/Apple Watch sleep stage data?
- 4. My HRV was 35 last night and 65 tonight. Is something wrong?
- 5. Should I panic if I get zero deep sleep one night?
- 6. Why does my tracker say I barely slept when I feel rested?
- 7. My doctor doesn't take my tracker data seriously. Why?
- 8. Does checking my sleep score make my sleep worse?
- 9. Which sleep metric should I focus on?
- 10. When should I see a sleep specialist?
- Next Steps Based on Your Biggest Sleep Concern
- References
How to Use This Guide
🔰 New to sleep tracking?
Read: “Sleep Stages” + “Sleep Duration vs Quality” → Focus on improving sleep efficiency first
📊 Comfortable with basics?
Add: “Heart Rate Variability (HRV)” + “Sleep Latency” → Optimize sleep timing and recovery
🔬 Advanced optimizer?
Review: All metrics → Identify your personal patterns → Consider professional consultation for persistent issues
⏱️ Only have 5 minutes?
Read: TL;DR + “At a Glance” table + FAQ section
TL;DR — 60-Second Summary
What are sleep metrics? Data your Fitbit, Oura, or Apple Watch collects about your sleep patterns: duration, stages (REM, deep, light), efficiency, heart rate variability (HRV), and breathing.
Why track sleep? To identify patterns, test improvements, and spot potential issues—NOT for obsessing over nightly perfection.
Which metrics matter most?
- Sleep duration & consistency (most controllable)
- Sleep efficiency (easily improved with sleep hygiene)
- HRV trends (reflects stress and recovery)
- Sleep stages (interesting but least actionable)
Key limitations: Consumer trackers are 60-80% accurate on sleep stages. Good for YOUR trends, not medical diagnosis.
When to worry: AHI >5 consistently, severe daytime sleepiness, HRV declining >20% over 2+ weeks, or unexplained pattern changes lasting >4 weeks.
Golden rule: How you feel > what your device says. If tracking increases anxiety, stop.
📥 Want the quick-reference version? [Download our 1-page Sleep Metrics Cheat Sheet]
⚠️ Should You Even Track Your Sleep?
✓ Sleep tracking is helpful if:
- You have unexplained fatigue despite seemingly adequate sleep
- You want objective feedback when testing sleep interventions
- You enjoy data and find it motivating (not anxiety-inducing)
- You’re optimizing athletic recovery or performance
✗ Skip sleep tracking if:
- You already sleep well and feel rested
- Checking scores increases your anxiety or affects your sleep
- You prefer intuitive, non-quantified approaches to health
- You have orthosomnia tendencies (score obsession)
The Alternative: Pay attention to how you feel. If you wake refreshed, have steady energy, and don’t experience daytime sleepiness, your sleep is probably fine regardless of what a tracker would say.
Remember: Humans slept perfectly well for 200,000 years without tracking. Devices are tools, not requirements.
What Are Sleep Stages and Why Do They Matter?
Sleep architecture progresses through distinct physiological stages, each associated with specific brain wave patterns, muscle activity, and biological functions.
Consumer devices estimate these stages and sleep stage percentages using movement sensors and heart rate data.
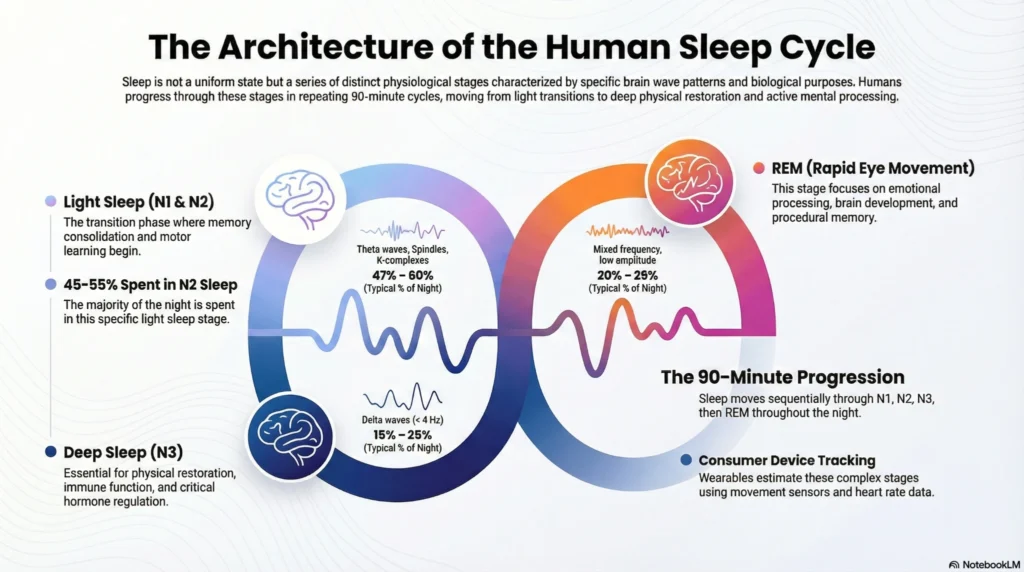
| Sleep Stage | Brain Wave Pattern | Typical % of Night | Primary Functions (Sleep Stages and Recovery) |
| Light Sleep (N1) | Theta waves (4-7 Hz) | 2-5% | Transition stage; easily awakened |
| Light Sleep (N2) | Sleep spindles, K-complexes | 45-55% | Memory consolidation; motor learning |
| Deep Sleep (N3) | Delta waves (<4 Hz) | 15-25% | Physical restoration; immune function; hormone regulation |
| REM Sleep | Mixed frequency, low amplitude | 20-25% | Emotional processing; procedural memory; brain development |
Sources: American Academy of Sleep Medicine, 2023; National Sleep Foundation Sleep Stage Guidelines
Light Sleep (N1 and N2)
Light sleep comprises the transitional N1 stage and the more substantial N2 stage. Research indicates N2 sleep is associated with memory consolidation and cognitive function.
| Characteristic | Description |
|---|---|
| N1 Duration | 1-7 minutes per cycle; occurs during sleep onset and stage transitions |
| N2 Duration | 10-25 minutes in early cycles; extends to 30+ minutes in later cycles |
| Physiological Markers | Heart rate decreases; body temperature declines; muscle tone reduces |
| Tracking Accuracy | Consumer devices may misclassify N1 and N2; clinical accuracy requires EEG |
| Clinical Significance | Excessive N1 may suggest sleep fragmentation; reduced N2 observed in some sleep disorders |
Sources: Walker, 2017 (Why We Sleep); Sleep Research Society consensus statements
Deep Sleep Explained: Is Your Percentage Normal?
Deep sleep, or slow-wave sleep, is characterized by high-amplitude delta brain waves. This stage is associated with physical restoration, immune system function, and metabolic regulation.
| Function Category | Associated Processes |
|---|---|
| Physical Restoration | Tissue repair; muscle growth; cellular regeneration via growth hormone secretion |
| Metabolic Regulation | Glucose metabolism; insulin sensitivity; appetite hormone regulation (leptin/ghrelin) |
| Immune Function | Cytokine production; T-cell distribution; inflammatory response modulation |
| Memory Consolidation | Declarative memory transfer from hippocampus to cortex; synaptic homeostasis (Comprehensive review of sleep’s role in learning and memory) |
| Timing & Distribution | Predominant in first half of night; decreases in later sleep cycles; age-dependent decline often dictates how much deep sleep do I need based on life stage. |
Deep Sleep Percentage by Age (Approximate %)
| Age Group | Typical N3 Range (Time in Deep Sleep) | Clinical Notes |
|---|---|---|
| Children (5-12 years) | 20-40% | Higher percentages support growth and development |
| Young Adults (18-30) | 15-25% | Baseline healthy adult range |
| Middle-Aged (40-60) | 10-20% | Progressive decline; higher variability |
| Older Adults (65+) | 5-15% | Significant reduction; fragmentation common |
Comprehensive meta-analysis of normal sleep patterns across ages
📊 What This Means for You:
If you’re over 60 with 5-8% deep sleep: This is within normal age-related decline. Don’t stress about low percentages if you feel rested and functional during the day.
If your deep sleep is 15-20%: Normal for adults under 40. No action needed—you’re getting adequate restorative sleep.
If 10-15%: Normal for adults over 40. Deep sleep naturally declines with age. Focus on sleep consistency and total duration rather than chasing higher percentages.
If below 10% consistently (multiple nights per week for 2+ weeks):
Review alcohol intake—even 1-2 drinks suppress deep sleep by 20-30%
Lower bedroom temperature to 65-68°F (warmer rooms reduce deep sleep)
Check stress levels and consider relaxation techniques before bed
Ensure you’re getting 7-9 hours total sleep (sleep deprivation paradoxically reduces deep sleep)
[Link to Sleep Hygiene Guide]
If above 25%: May indicate sleep debt recovery after several nights of poor sleep. This is your body catching up. Monitor patterns—if it persists for weeks, you may be chronically under-sleeping.
💡 Share This: “Getting only 15% deep sleep in your 40s? That’s completely normal. Deep sleep naturally declines with age, dropping from 20% in your 20s to 10-15% by age 50. Focus on consistency, not chasing perfect percentages.”
💡 Share This: “Your sleep tracker says you got ‘zero deep sleep’? Before panicking, know this: Consumer trackers misclassify sleep stages 20-40% of the time. If you felt reasonably rested, trust your body over your device.”
💡 Share This: “Want more deep sleep? The science is clear: Lower your bedroom to 65-68°F, avoid alcohol 3+ hours before bed, and maintain consistent sleep timing. Chasing perfect percentages will stress you out more than it helps.”
Common Question: “My deep sleep is only 15% and I’m in my 40s. Is something wrong?”
Answer: No, that’s completely normal. Deep sleep naturally declines with age—from around 20% in your 20s to 10-15% by age 50, and even lower in your 60s and beyond. Instead of chasing higher percentages, focus on sleep consistency and total duration.
Common Question: “I got zero deep sleep last night according to my tracker. Should I be concerned?”
Answer: Probably not. Consumer trackers occasionally misclassify sleep stages, especially if the device shifted during the night or your movement patterns were unusual. If you felt reasonably rested, trust your body. If you see zero or extremely low deep sleep multiple nights per week, check your alcohol intake, bedroom temperature (too warm reduces deep sleep), and device placement.
Common Question: “Can I increase my deep sleep percentage?”
Answer: Somewhat, but it’s limited. Deep sleep is largely determined by age and genetics. What you CAN control: bedroom temperature (65-68°F increases deep sleep), avoiding alcohol 3+ hours before bed, maintaining consistent sleep timing, and ensuring adequate sleep duration. Chasing perfection will stress you out more than it helps.
What Is REM Sleep and How Much Do You Need?
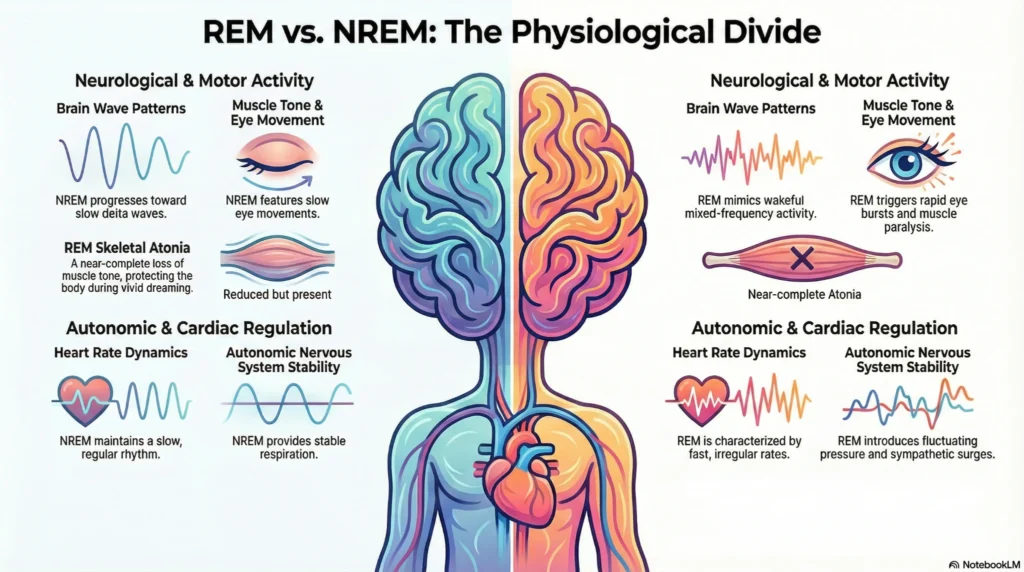
Rapid Eye Movement sleep is characterized by increased brain activity, vivid dreams, and temporary muscle atonia. Evidence suggests a healthy REM sleep percentage plays a role in emotional regulation and procedural memory consolidation.
| Feature | Details |
|---|---|
| Brain Activity | Similar to waking state; high metabolic activity in limbic and visual cortex |
| Physical State | Muscle paralysis (except diaphragm and eyes); elevated heart rate and blood pressure variability |
| Timing Pattern | First REM: 70-90 min after sleep onset; periods of time in REM sleep lengthen across night (5-40+ minutes). |
| Cognitive Functions | Emotional memory processing; threat simulation; creative problem-solving; skill consolidation |
| REM Deprivation Effects | Emotional dysregulation; impaired learning; REM rebound (increased REM on recovery nights) |
Sources: Siegel, 2001 (Science); Hobson & Pace-Schott, 2002; Rasch & Born, 2013 (Physiological Reviews)
Comprehensive review of sleep’s role in learning and memory
📊 What This Means for You:
If highly variable (15% one night, 28% the next): Normal. REM is more sensitive to daily stressors than other stages. Focus on weekly averages, not individual nights.
If your REM sleep is 20-25%: Optimal range for most adults. No changes needed.
If 15-20%: Still normal, especially if you feel mentally sharp during the day. REM needs vary individually.
If below 15% consistently (7-day average):
Avoid alcohol 3+ hours before bed—alcohol severely disrupts REM in the second half of the night
Check medication side effects (antidepressants, beta-blockers, and some sleep aids suppress REM)
Ensure adequate total sleep—REM concentrates in the later sleep cycles, so 6-hour sleepers miss significant REM
Reduce sleep fragmentation (address causes of nighttime awakenings)
[Link to REM Sleep Optimization Strategies]
If above 25-30% consistently:
May indicate REM rebound after sleep deprivation or withdrawal from REM-suppressing substances
Can signal depression or certain sleep disorders if accompanied by daytime symptoms
If persistent for 2+ weeks with excessive daytime sleepiness, consult a sleep specialist
💡 Share This: “REM sleep fluctuates 10-25% night to night based on stress, alcohol, and temperature. One night of 12% REM doesn’t mean anything. Track your 7-day average instead—that’s what actually matters.”
💡 Share This: “Think more REM = better sleep? Not always. Excessive REM (30%+) can indicate sleep debt recovery or rebound after stopping certain medications. Your body is complex—single metrics don’t tell the whole story.”
💡 Share This: “Alcohol before bed will wreck your REM sleep. Even 1-2 drinks can reduce REM by 20-30%, especially in the second half of the night. Want vivid dreams and mental sharpness? Skip the nightcap.”
Common Question: “My REM sleep was only 12% last night. Should I panic?”
Answer: No. Single-night variations are completely normal. REM naturally fluctuates between 10-25% night to night based on stress, alcohol, temperature, and sleep pressure. Track your 7-day average instead—that’s what actually matters.
Common Question: “I got 30% REM sleep last night—is that too much?”
Answer: Occasionally high REM (25-30%) usually indicates REM rebound after sleep deprivation or stress recovery. If it happens consistently for more than a week, it may signal disrupted sleep patterns. Monitor your patterns, but single nights of high REM are typically your body catching up.
Common Question: “Does dreaming more mean I’m getting more REM sleep?”
Answer: Not necessarily. You dream during all sleep stages, but REM dreams are more vivid and memorable. You might be waking during or right after REM, making you more aware of dreams—this doesn’t mean you’re getting more REM sleep than usual.
Awake Time
Occasional awakenings during sleep are normal and expected components of healthy sleep patterns. Brief arousals occur multiple times per hour as part of healthy sleep patterns, though most are not consciously remembered.
| Awakening Type | Duration/Frequency | Clinical Interpretation |
|---|---|---|
| Cortical Arousals | 3-15 seconds; 10-30 per hour (normal) | Not consciously perceived; necessary for sleep cycle transitions |
| Conscious Awakenings | Variable; 2-6 per night (normal) | Brief awareness; return to sleep within minutes |
| Wake After Sleep Onset (WASO) | Cumulative time awake after initial sleep onset | >30-60 min may indicate sleep maintenance issues |
| Terminal Awakening | Final awakening ending sleep period | Normal if aligned with intended wake time |
When Awakenings May Indicate Issues
| Pattern | Potential Associations |
|---|---|
| Frequent brief awakenings (>15/hour) | Sleep fragmentation; possible sleep apnea or periodic limb movements |
| Extended WASO (>60 minutes) | Insomnia; stress; environmental disruptions |
| Difficulty returning to sleep | Anxiety; circadian rhythm (your body’s natural sleep-wake cycle) disorders; medication effects |
| Early morning awakening | Depression; anxiety; age-related sleep changes |
⚠️ Clinical Note: Persistent awakening patterns associated with daytime impairment warrant professional sleep evaluation.
Sources: Bonnet & Arand, 2003 (Sleep Medicine Reviews); Carskadon & Dement, 2011 (Principles and Practice of Sleep Medicine)
Sleep Duration vs. Sleep Quality
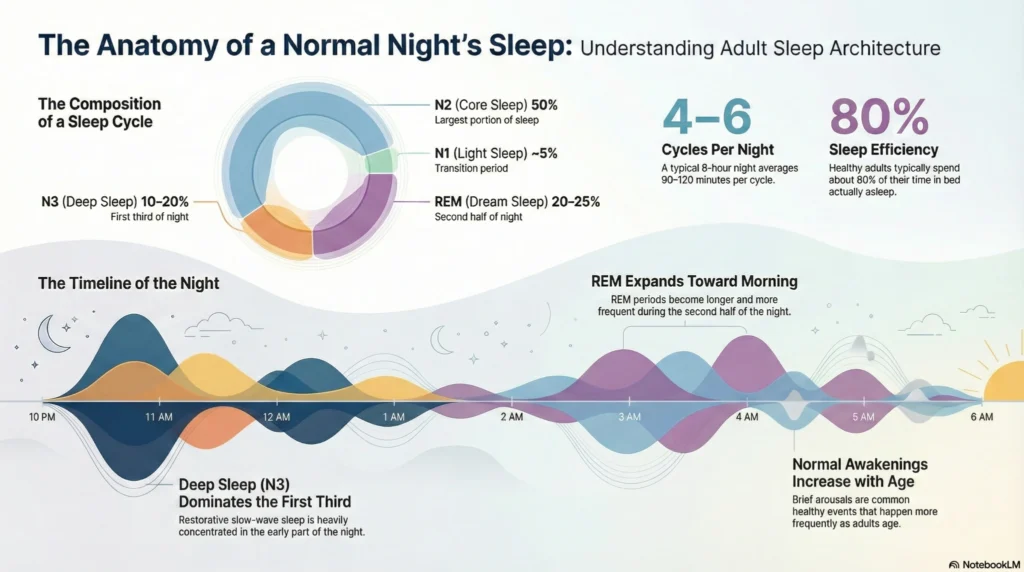
Sleep duration and primary sleep quality indicators represent different dimensions of sleep health. Research indicates both are important, and optimizing one without the other may not provide full restorative benefits. National Sleep Foundation’s sleep quality guidelines
| Aspect | Sleep Duration | Sleep Quality |
|---|---|---|
| Definition | Total time spent asleep | Continuity, depth, and architecture of sleep |
| Measurement | Hours and minutes from sleep onset to final awakening | Sleep efficiency %; stage percentages; fragmentation index |
| Health Impact | Insufficient duration associated with cardiovascular disease, obesity, diabetes | Fragmented sleep linked to cognitive impairment, mood disorders, inflammation |
| Compensatory Ability | Limited; chronic short sleep creates ‘sleep debt’ not fully recoverable | Poor quality may trigger REM/deep sleep rebound; some recovery possible |
Optimal Ranges
| Age Group | Recommended Duration | Sleep Efficiency Target | Quality Indicators |
|---|---|---|---|
| Teens (14-17) | 8-10 hours | ≥85% | Adequate deep sleep for growth; minimal WASO |
| Young Adults (18-25) | 7-9 hours | ≥85% | Balanced stage distribution; <30 min WASO |
| Adults (26-64) | 7-9 hours | ≥80% | 15-25% deep sleep; 20-25% REM |
| Older Adults (65+) | 7-8 hours | ≥75% | Reduced deep sleep expected; continuity more variable |
Note: Sleep efficiency = (Total Sleep Time / Time in Bed) × 100. Values ≥85% generally considered healthy.
Sources: National Sleep Foundation consensus recommendations; Hirshkowitz et al., 2015 (Sleep Health)
💡 Share This: “Is 6 hours of ‘perfect’ sleep better than 8 hours of ‘poor’ sleep? NO. Duration trumps quality scores. Most adults need 7-9 hours regardless of sleep stage percentages. Prioritize time in bed first, optimization second.”
💡 Share This: “Sleep consistency beats perfection. Going to bed and waking at the same time (even weekends) improves every sleep metric more than obsessing over deep sleep percentages or HRV scores. Routine is king.”
Sleep Scores and Algorithms
Sleep scores are proprietary composite metrics generated by sleep tracking algorithms within devices. Understanding sleep scores is challenging because these algorithms synthesize multiple data points but lack standardization across manufacturers.
How Sleep Scores Are Calculated
Most devices combine weighted factors into a single score (typically 0-100). Specific algorithms are proprietary and may change without user notification.
| Component | Typical Weight in Score | Data Sources |
|---|---|---|
| Total Sleep Time | 25-35% | Accelerometer; heart rate variability patterns |
| Sleep Efficiency | 15-25% | Movement detection; time in bed vs asleep |
| Sleep Stage Balance | 20-30% | Heart rate, HRV, movement algorithms |
| Restoration Indicators | 15-25% | Resting heart rate, HRV recovery, respiratory rate |
| Disruptions | 10-20% | Awakenings; restlessness events; breathing irregularities |
Important: Exact weighting varies by manufacturer and device model. Some brands adjust algorithms based on user age, activity level, and historical patterns.
What Is Sleep Efficiency and How Can You Improve It?
| Score Range | General Interpretation | Contextual Considerations |
|---|---|---|
| 90-100 | Excellent | Optimal duration, efficiency, and stage balance; minimal disruptions |
| 80-89 | Good | Adequate recovery; minor deficits in one or two components |
| 70-79 | Fair | Functional but suboptimal; may indicate insufficient duration or quality issues |
| 60-69 | Poor | Significant deficiencies; pattern assessment recommended |
| <60 | Very Poor | Multiple factors compromised; consider lifestyle evaluation or medical consultation |
⚠️ Individual Variation: Baseline scores vary significantly among individuals. Tracking personal trends over 2-4 weeks provides more actionable insights than single-night comparisons to population norms.
Limitations of Sleep Scores
| Limitation Category | Explanation |
|---|---|
| Lack of Standardization | No universal scoring methodology; scores from different brands not comparable |
| Proprietary Algorithms | Calculation methods undisclosed; updates may change scores without user awareness |
| Sensor Limitations | Because consumer devices lack EEG, sleep data accuracy for stage classification is lower than polysomnography – clinical sleep study (the medical gold standard) |
| Context Blindness | Scores do not account for illness, stress, medication, or intentional short sleep (e.g., shift work) |
| Oversimplification | Single number cannot capture sleep quality nuances; may obscure clinically relevant patterns |
| Potential for Anxiety | Obsessive score monitoring associated with ‘orthosomnia’ (perfectionist sleep tracking leading to sleep anxiety) |
Clinical Perspective: Sleep scores should be considered educational tools rather than diagnostic metrics. Persistent low scores or concerning symptoms warrant professional sleep evaluation.
Sources: Baron et al., 2017 (Journal of Clinical Sleep Medicine – orthosomnia study); Chinoy et al., 2021 (Sensors – consumer tracker validation)
Fitbit Sleep Score Explained
Fitbit calculates sleep scores (0-100) based on:
- Duration (50% weight): Hours slept vs. your personal goal
- Quality (25% weight): Deep and REM sleep percentages
- Restoration (25% weight): Sleeping heart rate and restlessness
Key Insight: Fitbit prioritizes duration heavily. A 9-hour sleep with mediocre stages can outscore a 6.5-hour sleep with excellent stages.
Oura Ring Sleep Score vs. Readiness Score
Sleep Score focuses on last night: duration, efficiency, timing, REM, deep sleep, latency, restfulness
Readiness Score combines sleep + recovery indicators: HRV, resting heart rate, body temperature, activity balance
Key Insight: You can have a high Sleep Score but low Readiness if your HRV indicates incomplete recovery. Prioritize Readiness for performance optimization.
Apple Watch Sleep Tracking
Apple Watch Series 4+ tracks:
- Sleep stages (REM, Core, Deep) — introduced in watchOS 9
- Respiratory rate
- Blood oxygen (Series 6+)
- Sleep duration and consistency
Limitations: No HRV-during-sleep tracking (only morning HRV); less detailed than dedicated sleep trackers. Best for users prioritizing convenience over depth.
💡 Share This: “Sleep scores vary wildly night to night because sleep is influenced by dozens of factors: stress, temperature, exercise timing, alcohol, light exposure, and hormones. Obsessing over nightly scores will make your sleep worse, not better.”
💡 Share This: “Fitbit gave you a 68 sleep score but you feel great? Here’s why: Sleep scores are arbitrary algorithms that weight metrics differently across devices. How you FEEL is infinitely more important than what your tracker says.”
💡 Share This: “You can’t compare sleep scores across devices. Fitbit prioritizes duration, Oura emphasizes HRV and recovery, Apple Watch focuses on consistency. A 75 on one device might be a 85 on another. Stop comparing.”
💡 Share This: “Orthosomnia is real: People obsessing over sleep scores actually sleep WORSE. Studies show score anxiety increases sleep latency and reduces sleep quality. If tracking makes you anxious, stop doing it.”
📊 What This Means for You:
If above 95% but you feel tired: You may not be spending enough total time in bed. High efficiency with insufficient duration still results in sleep deprivation.
If your sleep efficiency is 90-95%+: Excellent. Your time in bed closely matches time actually sleeping. Maintain your current sleep habits.
If 85-90%: Good, normal range. Most adults have brief awakenings throughout the night. No action needed unless you feel unrested.
If 80-85%:
Moderate inefficiency—you’re spending 45-90 minutes awake in bed
Try: Going to bed only when genuinely sleepy (not just tired)
Reduce pre-bed screen time (blue light delays sleep onset)
Keep bedroom cool, dark, and quiet
If you can’t fall asleep within 20 minutes, get up and do a calm activity until drowsy
[Link to Sleep Efficiency Improvement Guide]
If below 80% consistently:
Significant inefficiency—you may be spending 1.5-2+ hours awake in bed
Consider sleep restriction therapy: Match time in bed more closely to actual sleep time (if you sleep 6 hours but spend 8 in bed, reduce bed time to 6.5 hours initially)
Rule out sleep disorders: Sleep apnea, restless leg syndrome, or chronic insomnia
Consult a sleep specialist or try Cognitive Behavioral Therapy for Insomnia (CBT-I)
Avoid compensating with naps, which worsen nighttime sleep efficiency
Apnea-Hypopnea Index (AHI): Understanding Your Sleep Apnea Risk
The Apnea-Hypopnea Index quantifies breathing disruptions during sleep. While consumer devices increasingly offer AHI estimation, clinical diagnosis requires supervised polysomnography -clinical sleep study (the medical gold standard) or home sleep apnea testing.
What AHI Measures: Normal AHI Levels
| Event Type | Definition | Clinical Threshold |
|---|---|---|
| Apnea | Complete cessation of airflow for ≥10 seconds | Must be associated with oxygen desaturation or arousal |
| Hypopnea | Partial reduction in airflow (≥30% decrease) for ≥10 seconds | Requires ≥3% oxygen drop or arousal from sleep |
| AHI Calculation | (Total apneas + hypopneas) / hours of sleep | Clinical scoring follows AASM guidelines |
Consumer Device Limitations: Wearables estimate breathing disruptions using movement, heart rate changes, and blood oxygen sensors. These estimates may correlate with AHI but are not equivalent to clinical measurements.
AHI Severity Classification
| AHI Range | Severity | Clinical Implications |
|---|---|---|
| <5 events/hour | Normal | No significant sleep-related breathing disorder indicated |
| 5-15 events/hour | Mild OSA | May warrant evaluation if symptoms present (daytime sleepiness, morning headaches) |
| 15-30 events/hour | Moderate OSA | Clinical intervention often recommended; associated with health risks |
| >30 events/hour | Severe OSA | Treatment strongly recommended; elevated cardiovascular and metabolic risk |
⚠️ Important: Consumer device AHI estimates are not diagnostic. Formal sleep apnea diagnosis requires: – Clinical evaluation by a healthcare provider – Supervised polysomnography – clinical sleep study (the medical gold standard) or FDA-cleared home sleep apnea test – Interpretation by board-certified sleep medicine physician
Individuals with persistent snoring, witnessed breathing pauses, excessive daytime sleepiness, or morning headaches should consult a healthcare provider regardless of consumer device readings.
Sources: American Academy of Sleep Medicine clinical guidelines; Kapur et al., 2017 (Journal of Clinical Sleep Medicine)
📊 What This Means for You:
⚠️ Important: Consumer sleep trackers are NOT diagnostic tools. Use this information to identify patterns worth discussing with a doctor, not for self-diagnosis.
- If your AHI is 0-5 events/hour: Normal. No apnea detected. No action needed unless you have unexplained symptoms (see below).
- If your AHI is 5-15 events/hour (Mild Sleep Apnea range):
- Action required: Schedule consultation with a sleep specialist
- Do NOT assume tracker accuracy—get clinical testing (polysomnography or home sleep apnea test)
- While waiting for appointment:
- Try sleeping on your side instead of back (positional therapy)
- Avoid alcohol 3+ hours before bed
- Maintain healthy weight if overweight
- Elevate head of bed 30-45 degrees
- [Link to Sleep Apnea Specialist Finder]
- If your AHI is 15-30 events/hour (Moderate Sleep Apnea range):
- Urgent action: Contact sleep specialist immediately
- This level significantly impacts health (cardiovascular risk, daytime impairment)
- Do NOT rely on tracker data alone—pursue professional diagnosis
- Likely treatment: CPAP therapy, oral appliance, or surgery depending on evaluation
- If your AHI is 30+ events/hour (Severe Sleep Apnea range):
- Seek medical care promptly
- Severe apnea increases risk of heart attack, stroke, hypertension, and diabetes
- While trackers overestimate in this range, even half this number warrants immediate professional evaluation
Additional Triggers:
Ensure proper CPAP mask fit and consistent usage
If your AHI varies widely night to night (2 one night, 15 the next):
Sleep position matters—track which nights you slept on your back
Alcohol, nasal congestion, and weight changes affect severity
Tracker may be inaccurate—if average is >5, seek professional testing
If your AHI is normal (0-5) but you have these symptoms:
Loud snoring with witnessed breathing pauses
Gasping or choking during sleep
Severe daytime sleepiness despite adequate sleep duration
Morning headaches or dry mouth
Action: See a sleep specialist anyway—trackers miss apnea events, and you may have central sleep apnea or other disorders
If you’re already treated for sleep apnea and tracker shows AHI >5:
Your CPAP/oral appliance may need adjustment
Contact your sleep doctor to review therapy effectiveness
💡 Share This: “AHI above 5 events/hour on your tracker? Don’t self-diagnose. Consumer devices overestimate AND underestimate apnea. See a sleep specialist for proper testing—untreated sleep apnea increases heart attack and stroke risk.”
💡 Share This: “Your tracker shows zero apnea but you snore like a freight train? Trackers miss events regularly. If your partner witnesses breathing pauses or you have crushing daytime fatigue, get a clinical sleep study regardless of what your device says.”
💡 Share This: “Sleep apnea isn’t just snoring—it’s repeated breathing pauses that starve your body of oxygen. Symptoms: loud snoring, gasping during sleep, morning headaches, brain fog, and falling asleep during the day. This is serious. See a doctor.”
Common Question: “My tracker shows an AHI of 6. Do I have sleep apnea?”
Answer: Possibly, but consumer trackers are NOT diagnostic tools. An AHI >5 on a medical sleep study indicates sleep apnea, but tracker algorithms vary widely in accuracy. If your tracker consistently shows AHI >5, especially combined with loud snoring, gasping during sleep, or daytime sleepiness, schedule a consultation with a sleep specialist for proper testing (polysomnography).
Common Question: “My AHI varies from 2 to 12 night to night. Which is accurate?”
Answer: Sleep apnea severity can vary based on sleep position (worse on your back), alcohol consumption, nasal congestion, and sleep stage distribution. Track your 7-day average. If it’s consistently above 5, seek professional evaluation. Wide variations might also indicate tracker inaccuracy—consumer devices sometimes misinterpret movement or heart rate changes as breathing events.
Common Question: “I snore loudly but my AHI is 0. How is that possible?”
Answer: Snoring doesn’t always mean sleep apnea. You can snore without breathing pauses (apneas). However, consumer trackers may also miss events—they’re not as sensitive as clinical equipment. If your partner witnesses breathing pauses or you have daytime symptoms (fatigue, morning headaches, difficulty concentrating), get a professional sleep study regardless of what your tracker shows.
Common Question: “Can I treat my sleep apnea based on my tracker’s AHI reading?”
Answer: No. Never self-diagnose or self-treat sleep apnea based on consumer tracker data. Sleep apnea requires professional diagnosis via polysomnography and medical treatment (CPAP, oral appliances, or surgery depending on severity and type). Use your tracker data to identify patterns worth discussing with a doctor, not as a replacement for medical care.
Blood Oxygen (SpO2)
Blood oxygen saturation measures the percentage of hemoglobin in blood carrying oxygen. Consumer devices use pulse oximetry to estimate SpO2, typically through LED sensors on the wrist or finger.
SpO2 Ranges and Interpretation
| SpO2 Range | Typical Interpretation | Considerations |
|---|---|---|
| 95-100% | Normal | Healthy oxygen saturation during sleep |
| 90-94% | Borderline | May indicate mild hypoxemia; context-dependent (altitude, lung disease) |
| 85-89% | Low | Warrants medical evaluation if persistent |
| <85% | Very Low | Significant concern; medical attention recommended |
Factors Affecting Accuracy:
| Factor | Impact on Measurement |
|---|---|
| Skin Pigmentation | Darker skin tones may affect accuracy; some devices have bias |
| Peripheral Perfusion | Cold extremities, poor circulation reduce signal quality |
| Motion | Movement during sleep creates artifacts in readings |
| Sensor Placement | Wrist-based sensors less accurate than finger-based clinical oximeters |
| Altitude | Normal SpO2 lower at high elevation (e.g., 90-94% normal above 10,000 ft) |
Consumer Device vs. Clinical Oximetry
| Aspect | Consumer Wearable | Clinical Pulse Oximeter |
|---|---|---|
| Accuracy | ±2-4% typical; lower accuracy below 90% | ±2% standard; FDA-regulated performance |
| Response Time | Slower; averaged readings | Real-time continuous monitoring |
| Clinical Validation | Limited; varies by manufacturer | Extensive validation required for FDA clearance |
| Appropriate Use | General wellness monitoring; trend tracking | Medical diagnosis; treatment monitoring |
⚠️ Clinical Note: Consumer SpO2 readings showing consistent values <90% or significant drops—often called oxygen desaturation events—may indicate sleep apnea or other respiratory conditions. . These findings should prompt medical evaluation but are not diagnostic on their own.
Sources: Luks & Swenson, 2011 (High Altitude Medicine & Biology); FDA guidance on pulse oximetry
📊 What This Means for You:
- If your average SpO2 is 95-100%: Normal, healthy oxygen levels during sleep. No action needed.
- If your average SpO2 is 90-94%:
- Lower end of acceptable, but context matters
- Action: Note if you have:
- Lung conditions (asthma, COPD)
- High altitude residence (lower oxygen availability)
- Recent respiratory illness
- If no obvious cause and this is new, mention to your doctor
- May indicate mild sleep-disordered breathing
- If your average SpO2 is below 90% or you see frequent dips below 90%:
- Concerning—seek medical evaluation
- May indicate:
- Sleep apnea (oxygen desaturations during breathing pauses)
- Lung disease
- Heart conditions
- Action: Document patterns (frequency, duration of dips) and schedule appointment with doctor or sleep specialist
- Do NOT ignore sustained readings below 88%
Pattern-Based Actions:
- If you see brief dips to 88-92% a few times per night:
- Common with positional changes or mild apnea
- Try sleeping on your side
- Avoid alcohol before bed
- If dips occur 10+ times per night, pursue sleep apnea evaluation
- If SpO2 readings seem erratic or implausible (70% then 98% within seconds):
- Likely sensor error—poor device contact, movement, or low battery
- Action: Check device fit, clean sensors, ensure proper placement
- Re-evaluate after addressing technical issues
- If you have normal SpO2 but still feel unrefreshed:
- Oxygen saturation is only one factor
- Review other metrics (sleep efficiency, AHI, sleep stages)
- Consider non-respiratory causes of poor sleep quality
Remember: Consumer tracker SpO2 readings are less accurate than medical-grade pulse oximeters. Use trends and patterns, not single readings, to guide decisions.
💡 Share This: “Blood oxygen dipping below 90% during sleep? That’s your body not getting enough oxygen—often from sleep apnea. Track the pattern and see a doctor. Don’t ignore SpO2 warnings from your tracker.”
💡 Share This: “Normal SpO2 during sleep: 95-100%. Occasional dips to 92-94%: Usually fine. Frequent drops below 90%: Red flag for sleep apnea or lung issues. Consumer trackers aren’t perfect, but consistent low readings warrant medical evaluation.”
Common Question: “My SpO2 dropped to 88% for a few seconds. Should I be worried?”
Answer: Brief dips happen and aren’t always concerning—especially if you have nasal congestion or sleep on your back. However, frequent dips below 90% or sustained periods below 93% may indicate sleep apnea or other respiratory issues. If you see this pattern regularly along with snoring or daytime fatigue, consult a doctor. Single isolated events usually aren’t significant.
Common Question: “My average SpO2 is 96%. Is that normal?”
Answer: Yes, that’s excellent. Normal SpO2 during sleep is 95-100%. Levels consistently below 95% warrant medical evaluation, especially if accompanied by breathing symptoms. Keep in mind consumer trackers are less accurate than medical-grade pulse oximeters—use trends, not individual readings, as your guide.
Heart Rate Variability (HRV) Explained: What’s a Good HRV for Your Age?
Heart rate variability sleep metrics measure the variation in time between consecutive heartbeats during rest or sleep. Higher HRV generally indicates greater autonomic nervous system (your body’s stress recovery ability) and may be associated with better cardiovascular fitness and stress resilience.
What HRV Reflects
HRV is influenced by the balance between sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) nervous system activity. Research suggests HRV patterns may provide insights into:
- Autonomic nervous system function ( your body’s stress recovery ability)
- Cardiovascular health status
- Recovery from physical stress
- Sleep quality indicators
- Potential stress or overtraining markers
HRV Metrics on Consumer Devices
| Metric | What It Measures | Typical Use |
|---|---|---|
| RMSSD | Root mean square of successive differences between heartbeats | Short-term HRV; parasympathetic activity indicator |
| SDNN | Standard deviation of all heartbeat intervals | Overall HRV; longer measurement periods |
| HF/LF Ratio | High frequency vs low frequency components | Autonomic balance estimation (limited accuracy on wearables) |
Interpreting HRV Values
⚠️ Critical Context: HRV values are highly individual and influenced by age, fitness level, genetics, and measurement conditions. Population averages provide limited utility for individual interpretation.
| Factor | Influence on HRV |
|---|---|
| Age | Declines with aging; older adults typically have lower HRV |
| Fitness | Higher cardiovascular fitness generally associated with higher HRV |
| Sleep | HRV typically higher during deep sleep; lower during REM |
| Stress | Acute and chronic stress often associated with reduced HRV |
| Recovery | HRV may decrease during illness, intense training, or inadequate recovery |
HRV Trends vs. Absolute Values
Research suggests HRV patterns may provide insights into the link between HRV and recovery:
- Establish personal baseline: Track HRV for 2-4 weeks to establish baseline sleep metrics and identify your typical range.
- Monitor deviations: Significant decreases from baseline may indicate stress, illness, or inadequate recovery
- Consider context: Alcohol, caffeine, medication, sleep quality, and recent exercise affect HRV
- Avoid overinterpretation: Single-night HRV variations are common and often not clinically meaningful
Clinical Perspective: While HRV patterns may provide general wellness insights, consumer device HRV should not be used for medical diagnosis or to guide clinical treatment. Individuals with cardiovascular concerns should consult healthcare providers.
Sources: Shaffer & Ginsberg, 2017 (Frontiers in Public Health); Plews et al., 2013 (European Journal of Applied Physiology)
📊 What This Means for You:
First, establish YOUR baseline: HRV is highly individual. Track for 2-4 weeks to determine your normal range before interpreting highs or lows.
By Age & Fitness Level (General Ranges):
Ages 20-30:
- If your HRV is 60-100+ ms: Normal to excellent, especially if physically active
- If 40-60 ms: Average for sedentary individuals
- If below 40 ms: May indicate high stress, overtraining, poor sleep, or low cardiovascular fitness
Ages 30-40:
- If your HRV is 50-80 ms: Normal to good
- If 35-50 ms: Average
- If below 35 ms: Worth investigating—see improvement strategies below
Ages 40-50:
- If your HRV is 40-70 ms: Normal to good, especially if you exercise regularly
- If 25-40 ms: Average for age group
- If below 25 ms: Consider lifestyle optimization
Ages 50+:
- If your HRV is 30-60 ms: Good for age (especially if active)
- If 20-30 ms: Average for age
- If below 20 ms: Focus on stress reduction and cardiovascular health
Peer-reviewed HRV norms from Frontiers in Public Health
Actionable Triggers (Regardless of Age):
Action: None needed—this is optimal. Watch for sudden drops that might indicate overtraining.
If your HRV trends upward over weeks: Great! Your interventions (better sleep, exercise, stress management) are working. Maintain current habits.
If your HRV drops 10-15% below your baseline for 1-2 nights:
Likely causes: Alcohol, late meal, poor sleep, stress, intense workout
Action: Prioritize recovery—extra sleep, hydration, lighter training
Monitor for return to baseline within 2-3 days
If your HRV drops 20%+ below baseline and stays low for 5-7 days:
Red flag for: Overtraining, chronic stress, illness brewing, burnout
Action: Reduce exercise intensity, prioritize sleep (add 30-60 min), review stress sources
If accompanied by fatigue or other symptoms, consider medical consultation
[Link to HRV Recovery Protocol]
If your HRV is consistently improving (upward trend over 4+ weeks):
You’re adapting well to training or lifestyle changes
Action: Continue current approach; consider gradually increasing training load if that’s your goal
If your HRV is erratic (wild day-to-day swings of 30-50 ms):
Common culprits: Inconsistent sleep schedule, variable alcohol intake, irregular exercise timing
Action: Stabilize lifestyle factors first—consistent bedtime, moderate alcohol, regular exercise routine
Check device placement (shifting sensors cause false readings)
If you’re athletic with unusually high HRV (100+ ms):
Indicates excellent cardiovascular fitness and parasympathetic tone
💡 Share This: “HRV declines with age, but fitness matters more than years. A fit 50-year-old can have higher HRV than a sedentary 30-year-old. Stop comparing yourself to others—track YOUR trends instead.”
💡 Share This: “Your HRV dropped from 60 to 40 overnight? Don’t panic. HRV naturally fluctuates 20-40% based on alcohol, stress, late meals, and exercise timing. What matters: 7-day averages and long-term trends.”
💡 Share This: “Low HRV doesn’t mean you’re unhealthy—it means your body is under stress or recovering. Common culprits: overtraining, poor sleep, alcohol, illness brewing, or chronic stress. Listen to what it’s telling you.”
💡 Share This: “Athletes: HRV dropping 20%+ below baseline for a week? Your body is screaming for recovery. Reduce training intensity, prioritize sleep, and give your nervous system time to adapt.”
Common Question: “My HRV was 45 last night and 72 tonight. Is something wrong?”
Answer: No, HRV naturally fluctuates 20-40% night to night. Factors that temporarily lower HRV include: alcohol consumption, late meals, intense exercise close to bedtime, stress, insufficient sleep, illness, and even changes in sleeping position. What matters is your 7-day average trend, not individual nights.
Common Question: “What’s a ‘good’ HRV for my age?”
Answer: HRV is highly individual and decreases with age. General ranges:
- 20s-30s: 55-105 ms
- 40s: 40-70 ms
- 50s+: 25-55 ms
But fitness level matters as much as age. A fit 50-year-old may have higher HRV than an inactive 30-year-old. Focus on YOUR baseline and trends rather than comparing to population averages.
Common Question: “My HRV has been declining for two weeks. Should I see a doctor?”
Answer: If your HRV drops more than 20% below your normal baseline and stays low for 2+ weeks, it’s worth investigating. Common causes: increased stress, overtraining, poor sleep quality, illness brewing, or lifestyle changes (increased alcohol, poor diet). Try improving sleep hygiene and stress management first. If it persists beyond 3-4 weeks or you have other symptoms, consult a healthcare provider.
Common Question: “Is higher HRV always better?”
Answer: Generally yes, but context matters. Very high HRV can occasionally indicate overtraining recovery or parasympathetic dominance in athletes. For most people, higher HRV indicates better cardiovascular fitness and stress resilience. Focus on YOUR upward trends rather than hitting a specific number.
Respiratory Rate
The breathing rate sleep metric measures breaths per minute during rest. Consumer devices estimate respiratory rate using chest movement sensors or heart rate variability patterns.
Normal Respiratory Rate Ranges
| Population | Typical Range | Considerations |
|---|---|---|
| Adults (at rest) | 12-20 breaths/min | Decreases during deep sleep |
| During Sleep | 12-16 breaths/min | Individual variation significant |
| Athletes | 10-14 breaths/min | Lower rates common in highly fit individuals, making this essential sleep data for athletes. |
Factors Affecting Respiratory Rate During Sleep
| Factor | Typical Effect |
|---|---|
| Sleep Stage | Decreases in deep sleep; more variable in REM |
| Body Position | May increase in supine position in some individuals |
| Altitude | Increases at high elevation |
| Illness | Elevated with respiratory infections, fever |
| Sleep Apnea | Irregular patterns; pauses followed by rapid breathing |
Consumer Device Limitations
Consumer wearables estimate respiratory rate indirectly through: – Accelerometer-detected chest movements – Heart rate variability patterns (respiratory sinus arrhythmia) – Ballistocardiography (detecting body movements from heartbeat and breathing)
Accuracy Considerations: – Accuracy typically ±1-3 breaths/min compared to clinical respiratory monitoring – Movement during sleep may introduce measurement errors – Sensor placement affects accuracy (chest straps more accurate than wrist devices)
⚠️ Clinical Note: Persistent respiratory rate >20 breaths/min during sleep or significant irregularities may warrant medical evaluation. Consumer device readings are not diagnostic.
Sources: Cretikos et al., 2008 (Respiratory Care); Berry et al., 2012 (Journal of Clinical Sleep Medicine)
Sleep Latency
Sleep latency is the time required to transition from full wakefulness to sleep. This metric may provide insights into sleep drive, circadian alignment, and potential sleep disorders.
Sleep Onset Latency
| Latency Range | Typical Interpretation | Clinical Context |
| <5 minutes | Unusually rapid | May indicate significant sleep debt or sleep disorder (e.g., narcolepsy) |
| 10-20 minutes | Normal | Healthy sleep onset |
| 20-30 minutes | Borderline | Within normal variation; may suggest mild difficulty initiating sleep |
| >30 minutes | Prolonged | May indicate insomnia, anxiety, or circadian rhythm (your body’s natural sleep-wake cycle) misalignment |
Factors Influencing Sleep Latency
| Factor | Effect on Sleep Onset |
|---|---|
| Sleep Pressure | Higher sleep debt (inadequate prior sleep) reduces latency |
| Circadian Timing | Sleep onset faster when aligned with natural circadian rhythm (your body’s natural sleep-wake cycle) |
| Stress/Anxiety | Mental arousal significantly delays sleep onset |
| Caffeine | Extends latency; effects persist 6-8 hours |
| Physical Activity | Regular exercise may improve latency; intense late-day exercise may delay onset |
| Screen Exposure | Blue light exposure before bed delays melatonin secretion and extends latency |
Consumer Device Measurement
Consumer devices estimate sleep latency by detecting: – Sustained decrease in movement – Heart rate decline – Transition to heart rate variability patterns typical of early sleep
Limitations: – Devices may misclassify quiet wakefulness as sleep onset – Actual sleep onset (verified by EEG) may differ from device estimate by ±10-20 minutes – Individuals lying still before sleep may have artificially short measured latency
Clinical Perspective: Consistently prolonged sleep latency (>30 minutes) associated with daytime fatigue or distress may indicate insomnia or circadian rhythm disorders warranting professional evaluation.
Sources: Ohayon et al., 2017 (Sleep Medicine); Kaplan & Harvey, 2009 (Sleep Medicine Reviews)
📊 What This Means for You:
Action: Track patterns—note what differs on fast vs. slow nights (exercise timing, caffeine, stress, screen time)
If you fall asleep in 10-20 minutes: Ideal. This indicates healthy sleep pressure without excessive fatigue.
If you fall asleep in 5-10 minutes:
Often normal, but can indicate mild sleep deprivation
Action: If you feel refreshed during the day, no change needed
If you feel tired often, consider adding 30-60 minutes to your sleep schedule
If you fall asleep in under 5 minutes consistently:
Strong indicator of sleep debt—you’re likely not getting enough sleep
Action: Go to bed 30-60 minutes earlier for 2 weeks and reassess
Well-rested people take longer to fall asleep because they have lower sleep pressure
[Link to Sleep Duration Optimization]
If it takes you 20-30 minutes to fall asleep:
Upper end of normal, but worth optimizing
Action: Review pre-bed routine—reduce screen time 1 hour before bed, try relaxation techniques, ensure bedroom is cool and dark
Avoid watching the clock (increases anxiety)
If it takes 30-45+ minutes consistently:
May indicate onset insomnia or hyperarousal
Action:
Practice the “20-minute rule”: If not asleep in 20 minutes, get out of bed and do a quiet activity
Avoid caffeine after 2 PM
Create a buffer zone (30-60 min wind-down before bed with no screens)
Try sleep restriction therapy or Cognitive Behavioral Therapy for Insomnia (CBT-I)
[Link to Insomnia Solutions Guide]
If you fall asleep quickly some nights (5 min) and slowly others (40 min):
Normal variation based on daily stress, activity level, and circadian alignment
💡 Share This: “Sleep efficiency below 85% means you’re spending serious time awake in bed. The fix isn’t MORE time in bed—it’s better sleep hygiene, consistent timing, and only using your bed for sleep (not scrolling).”
💡 Share This: “Falling asleep in under 5 minutes every night? That’s not a superpower—it’s a red flag for sleep deprivation. Well-rested people take 10-20 minutes to fall asleep because they have normal sleep pressure, not exhaustion.”
Common Question: “I fall asleep in under 5 minutes. Is that good?”
Answer: Not necessarily. Falling asleep in under 5 minutes often indicates sleep deprivation, not superior sleep ability. Well-rested individuals typically take 10-20 minutes to fall asleep. If you consistently crash immediately, you may not be getting enough sleep overall.
Common Question: “It takes me 45 minutes to fall asleep. Do I have insomnia?”
Answer: Not automatically, but it warrants attention. Occasional long sleep latency (stress, schedule changes) is normal. If you take >30 minutes to fall asleep 3+ nights per week for over a month, AND it bothers you or affects daytime functioning, you may have onset insomnia. Causes include anxiety, poor sleep hygiene, caffeine too late, or too much time in bed. Try sleep restriction therapy or consult a sleep specialist.
Circadian Alignment
Circadian rhythm (your body’s natural sleep-wake cycle) is the body’s internal ~24-hour biological clock that regulates sleep-wake cycles, hormone secretion, and numerous physiological processes. Sleep quality is influenced by alignment between sleep timing and circadian rhythms. How circadian rhythms regulate sleep-wake cycles
Circadian Phase Indicators
| Marker | What It Indicates | Measurement Method |
|---|---|---|
| Core Body Temperature | Temperature nadir typically occurs 2-3 hours before natural wake time | Continuous skin temperature sensors (limited accuracy on consumer devices) |
| Melatonin Timing | Dim light melatonin onset (DLMO) marks circadian evening | Clinical measurement; not available on consumer devices |
| Sleep-Wake Pattern | Consistent sleep and wake times suggest circadian stability | Tracked via movement and heart rate patterns |
Circadian Misalignment Patterns
| Pattern | Characteristics | Common Associations |
|---|---|---|
| Delayed Sleep Phase | Natural sleep onset 2+ hours later than desired; difficulty waking early | Adolescents, young adults; genetic predisposition |
| Advanced Sleep Phase | Early sleep onset (7-9 PM); early morning awakening (3-5 AM) | Older adults; genetic variants |
| Irregular Sleep-Wake | Highly variable sleep timing; fragmented sleep | Shift work; chronic jet lag; neurological conditions |
Sleep Timing Consistency
Research indicates sleep timing regularity may be as important as total duration for health outcomes.
Metrics tracked by devices: – Sleep onset time variability – Wake time consistency – Weekend vs. weekday sleep timing differences
Social Jet Lag: Discrepancy between weekday and weekend sleep schedules (often ≥2 hours) associated with metabolic and cardiovascular health markers in some studies.
⚠️ Note: Circadian alignment cannot be fully assessed by consumer devices. Clinical circadian assessment may require specialized testing including: – Dim light melatonin onset measurement – Core body temperature monitoring – Actigraphy combined with sleep diaries – Consultation with sleep medicine specialist
Sources: Abbott et al., 2020 (Sleep); Roenneberg et al., 2019 (Current Biology)
Sleep Hygiene and Environmental Factors
Sleep hygiene refers to behavioral and environmental practices that may promote sleep quality. While consumer devices cannot directly measure these factors, sleep data patterns may reflect their influence.
Environmental Factors Affecting Sleep
| Factor | Optimal Range/Practice | Common Issues |
|---|---|---|
| Room Temperature | 60-67°F (15.5-19°C) | Overheated rooms disrupt sleep continuity |
| Light Exposure | Complete darkness or <5 lux | Light exposure suppresses melatonin; delays circadian rhythm (your body’s natural sleep-wake cycle) |
| Noise | <30 decibels (quiet library) | Noise disrupts sleep stages; fragments sleep architecture |
| Humidity | 30-50% relative humidity | Very dry or humid conditions may cause discomfort |
Behavioral Sleep Hygiene Practices
| Practice Category | Recommended Approach | Evidence Strength |
|---|---|---|
| Consistent Schedule | Same sleep and wake times (±30 min variation) | Strong evidence for circadian stability |
| Caffeine Timing | Avoid within 6 hours of bedtime | Strong evidence for reduced sleep latency |
| Alcohol Restriction | Limit/avoid evening alcohol | Reduces REM sleep; increases sleep fragmentation |
| Physical Activity | Regular exercise; avoid intense activity 3 hours before bed | Moderate evidence for improved sleep quality |
| Screen Management | Minimize blue light 1-2 hours before bed | Moderate evidence for earlier sleep onset |
| Bedroom Use | Reserve bed for sleep and intimacy only | Moderate evidence for sleep-wake association |
24-Hour Sleep Hygiene Timeline
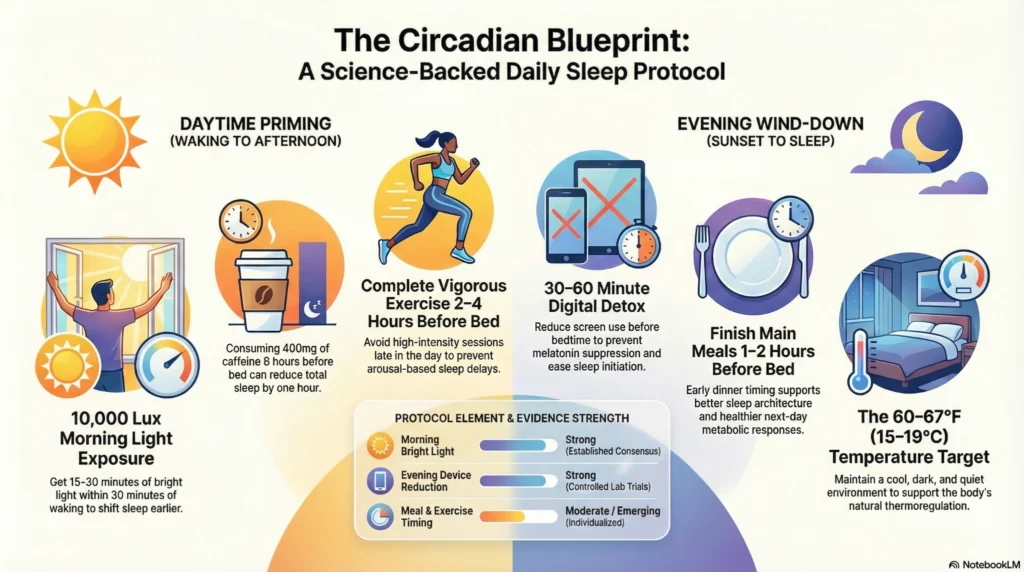
Clinical Perspective: Sleep hygiene practices are evidence-based recommendations that may improve sleep quality for many individuals. However, persistent sleep difficulties despite consistent sleep hygiene may indicate underlying sleep disorders requiring professional evaluation.
Sources: Irish et al., 2015 (Journal of Behavioral Medicine); Stepanski & Wyatt, 2003 (Sleep Medicine Reviews)
Using Sleep Metrics Responsibly
When determining which sleep metrics to track, consumer sleep tracking provides general wellness information that may help identify patterns. However, these metrics should be interpreted with awareness of their limitations.
Best Practices for Sleep Metric Interpretation
- Focus on trends, not single nights: Day-to-day variation is normal; 1-2 week patterns are more informative
- Understand device limitations: Consumer devices estimate sleep stages; they do not provide clinical-grade measurements
- Consider context: Illness, stress, travel, and medications affect sleep metrics
- Avoid score obsession: “Orthosomnia” (perfectionist sleep tracking) can paradoxically worsen sleep quality
- Use data as discussion tool: Share patterns with healthcare providers when relevant, not isolated numbers
When to Consult a Healthcare Provider
Persistent patterns suggesting potential sleep disorders:
| Concerning Pattern | Possible Indication |
|---|---|
| Consistent high wake time (>60 min WASO) | Sleep maintenance insomnia |
| Prolonged sleep latency (>30 min) | Sleep onset insomnia; circadian misalignment |
| Low sleep efficiency (<80%) despite adequate time in bed | Sleep fragmentation; restless sleep |
| Frequent desaturations or elevated estimated AHI | Sleep apnea screening needed |
| Persistent low HRV with daytime fatigue | Recovery issues; chronic stress; medical evaluation |
| Excessive daytime sleepiness despite adequate duration | Sleep quality issues; possible sleep disorder |
⚠️ Important: Consumer device data is not diagnostic. Professional sleep evaluation may include: – Clinical interview by sleep medicine specialist – Sleep diary and validated questionnaires – Polysomnography -clinical sleep study (the medical gold standard) – Home sleep apnea testing – Actigraphy with clinical correlation
Limitations of Consumer Sleep Tracking
All users should understand the consumer sleep tracking limitations inherent to these devices :
Measurement Accuracy Limitations
| Metric | Typical Accuracy | Key Limitations |
|---|---|---|
| Sleep Stages | 60-70% agreement with polysomnography – clinical sleep study (the medical gold standard) | Cannot measure brain waves (EEG); relies on movement and heart rate patterns |
| Sleep Onset/Offset | ±10-20 minutes | Difficulty distinguishing quiet wakefulness from sleep |
| Sleep Duration | ±15-30 minutes | May overestimate sleep by counting still wakefulness |
| AHI Estimation | Correlates but not equivalent to clinical AHI | Cannot measure airflow directly; proxy indicators only |
| SpO2 | ±2-4% typical | Less accurate at lower saturations; affected by skin tone and perfusion |
| HRV | Reasonable correlation but varies by device | Algorithm differences; measurement period variations |
Interpretation Limitations
- No standardization: Different manufacturers use different algorithms; scores not comparable across brands
- Proprietary methods: Calculation approaches often undisclosed and may change without notification
- Population norms: “Average” values may not apply to individuals; personal baselines more useful
- Context blindness: Devices cannot account for illness, medications, intentional sleep restriction, or life circumstances
When Consumer Tracking Is Not Sufficient
Consumer sleep tracking is not appropriate for:
- Diagnosing sleep disorders: Requires clinical evaluation and specialized testing
- Guiding medical treatment: Clinical decisions should not be based on consumer device data
- Monitoring medical conditions: Regulated medical devices required for health monitoring
- Replacing healthcare evaluation: Symptoms of sleep disorders warrant professional assessment
Clinical Perspective: Consumer sleep trackers serve as general wellness tools that may help identify patterns worth discussing with healthcare providers. They are not substitutes for medical evaluation or diagnostic testing.
Sources: de Zambotti et al., 2019 (Sleep Medicine Reviews – comprehensive validation review); Chinoy et al., 2021 (Sensors)
How Accurate Is Your Sleep Tracker? (What Studies Show)
Consumer sleep trackers use movement (actigraphy) and heart rate to estimate sleep stages. Here’s how they compare to clinical gold-standard polysomnography (PSG) – clinical sleep study (the medical gold standard):
Accuracy Ratings:
- ✅ Sleep duration: ±10-15 minutes (very good)
- ✅ Sleep vs. wake detection: 90-95% accuracy
- ⚠️ Sleep stages (REM/deep/light): 60-80% accuracy (2021 study comparing consumer sleep trackers to clinical testing)
- ⚠️ Sleep apnea screening: Varies widely by device; not diagnostic
What This Means:
- Your tracker is good for: Tracking YOUR personal trends over time, testing interventions, identifying patterns
- Your tracker is NOT good for: Medical diagnosis, comparing to others’ scores, obsessing over single-night precision
The Bottom Line: Absolute accuracy doesn’t matter as much as consistency. If your tracker shows your deep sleep improved from 12% to 18% after changing your routine, that trend is valuable even if the absolute numbers are off by a few percentage points.
When Precision Matters: If you suspect a sleep disorder (apnea, narcolepsy, etc.), skip the consumer tracker and get a clinical sleep study. Don’t rely on Fitbit/Oura/Apple Watch for diagnosis.
💡 Share This: “How accurate is your Fitbit/Oura/Apple Watch? Sleep duration: ±10-15 minutes (good). Sleep stages: 60-80% accurate (okay for trends). Medical diagnosis: 0% reliable (see a doctor instead).”
💡 Share This: “Your sleep tracker estimates—it doesn’t diagnose. Consumer devices use movement and heart rate to guess at sleep stages. Clinical sleep studies use brain waves. Big difference. Use trackers for YOUR trends, not absolute truth.”
💡 Share This: “Sleep trackers are wrong 20-40% of the time on sleep stages. But here’s what matters: If your ‘deep sleep’ improved from 12% to 18% after changing your routine, that TREND is valuable even if the numbers aren’t perfect.”
💡 Share This: “Can you trust your sleep tracker for sleep apnea detection? No. Consumer devices miss apnea events regularly and can’t distinguish types of apnea. If you snore loudly or gasp during sleep, see a specialist—don’t rely on your Fitbit.”
💡 Share This: “Your doctor doesn’t trust your sleep tracker data—and here’s why: They’re not FDA-approved medical devices. Diagnosis requires clinical-grade polysomnography. Use your tracker to spot patterns worth discussing, not as medical evidence.”
Your Sleep Optimization Priority Matrix
Not sure where to start? Use this framework based on controllability and impact:
Priority 1: Easy Wins (Start Here)
Focus: Sleep duration & consistency (Why consistent sleep timing improves sleep quality)
Action: Set consistent wake time (even weekends) → Monitor sleep efficiency → Adjust bedtime ±30 minutes → Check weekly average
Timeline: See improvements in 5-7 days
National Sleep Foundation’s sleep duration guidelines
How environmental factors improve sleep quality
Priority 2: Moderate Effort
Focus: Sleep environment & sleep stages
Action: Optimize bedroom (temperature 65-68°F, darkness, sound) → Track deep sleep % → Test changes one at a time → Reassess in 2 weeks
Timeline: Improvements in 2-4 weeks
Priority 3: Advanced Optimization
Focus: HRV trends & respiratory metrics
Action: Address lifestyle factors (stress, exercise timing, alcohol) → Monitor HRV trends → Consider professional consultation if patterns persist
Timeline: Requires 4-8 weeks of consistent changes
When to Seek Professional Help
- Suspected sleep disorder symptoms (research on excessive daytime sleepiness and sleep disorders)
- AHI consistently >5 events/hour (Clinical guidelines for sleep apnea diagnosis)
- Severe daytime sleepiness despite adequate sleep duration
- HRV declining >20% over 2+ weeks without explanation
FrequentlyAsked Sleep Tracker Questions
1. Why does my sleep score vary so much day to day?
Sleep is influenced by stress, temperature, alcohol, exercise timing, light exposure, and natural biological rhythms. Focus on 7-14 day trends, not individual nights.
2. Is 6 hours of “excellent” sleep better than 8 hours of “poor” sleep?
No. Duration matters more than quality scores. Most adults need 7-9 hours regardless of sleep stage percentages. Prioritize duration first, quality second.
Clinical effects of interrupted versus insufficient sleep
National Sleep Foundation’s sleep duration guidelines
3. Can I trust my Fitbit/Oura/Apple Watch sleep stage data?
Accuracy ranges from 60-80% compared to clinical sleep studies (polysomnography). Good enough for tracking YOUR trends, not precise enough for medical diagnosis.
(2021 study comparing consumer sleep trackers to clinical testing)
4. My HRV was 35 last night and 65 tonight. Is something wrong?
HRV naturally fluctuates 20-40% night to night. Alcohol, late eating, stress, illness, and exercise timing cause variations. Track 7-day averages instead.
5. Should I panic if I get zero deep sleep one night?
No. Consumer trackers sometimes misclassify sleep stages. If it’s a pattern (multiple nights/week), review alcohol intake, bedroom temperature, and stress. One night means nothing.
6. Why does my tracker say I barely slept when I feel rested?
Sensors can misread stillness as wakefulness or miss sleep if the device shifts during the night. Trust how you feel. If this happens frequently, check device placement and fit.
7. My doctor doesn’t take my tracker data seriously. Why?
Consumer trackers aren’t FDA-approved medical devices. Doctors need clinical-grade testing (polysomnography) for diagnosis. Use tracker data to identify patterns worth discussing, not as standalone evidence.
8. Does checking my sleep score make my sleep worse?
Yes, for some people. “Orthosomnia” (sleep score obsession) increases anxiety and worsens sleep quality. If tracking causes stress, stop. Your subjective experience is more important.
9. Which sleep metric should I focus on?
Start with sleep efficiency and duration—these are most controllable. Once consistent, monitor HRV trends. Sleep stages are interesting but least actionable for most people.
10. When should I see a sleep specialist?
If you have: AHI >5 consistently, severe daytime sleepiness despite 7-9 hours in bed, loud snoring + witnessed breathing pauses, or unexplained sleep pattern changes lasting >4 weeks.
American Academy of Sleep Medicine guidelines”
Research on excessive daytime sleepiness and sleep disorders
Next Steps Based on Your Biggest Sleep Concern
😴 Poor sleep score despite feeling fine:
→ [Download: When to Trust Your Body vs Your Tracker]
⚡ Low energy despite 7-8 hours in bed:
→ [Free Email Course: Sleep Quality Over Quantity Protocol]
📉 Declining HRV or concerning patterns:
→ [Checklist: 15 HRV-Boosting Habits (Evidence-Based)]
🫁 Suspected sleep apnea (high AHI, low SpO2):
→ [Find a Sleep Specialist in Your Area]
🎯 Ready to optimize all metrics:
→ [14-Day Sleep Transformation Protocol]
⚡ Quick Wins to Improve Your Metrics Tonight:
- Set a consistent wake time (even weekends) — improves sleep efficiency
- Reduce bedroom temperature to 65-68°F — increases deep sleep percentage
- Stop caffeine 10 hours before bed — improves HRV and sleep latency
- Avoid alcohol 3+ hours before bed — prevents REM suppression
How environmental factors improve sleep quality
Clinical evidence for sleep hygiene practices
[Get the complete evidence-based checklist →]
References
Walker, M. (2017). Why We Sleep: Unlocking the Power of Sleep and Dreams. Scribner.
Abbott, S. M., Reid, K. J., & Zee, P. C. (2020). Circadian rhythm sleep-wake disorders. Psychiatric Clinics, 43(4), 631-647.
American Academy of Sleep Medicine. (2023). International Classification of Sleep Disorders, 3rd edition, text revision (ICSD-3-TR).
Baron, K. G., Abbott, S., Jao, N., Manalo, N., & Mullen, R. (2017). Orthosomnia: Are some patients taking the quantified self too far? Journal of Clinical Sleep Medicine, 13(2), 351-354.
Berry, R. B., Budhiraja, R., Gottlieb, D. J., et al. (2012). Rules for scoring respiratory events in sleep. Journal of Clinical Sleep Medicine, 8(5), 597-619.
Bonnet, M. H., & Arand, D. L. (2003). Clinical effects of sleep fragmentation versus sleep deprivation. Sleep Medicine Reviews, 7(4), 297-310.
Carskadon, M. A., & Dement, W. C. (2011). Monitoring and staging human sleep. In M. H. Kryger, T. Roth, & W. C. Dement (Eds.), Principles and Practice of Sleep Medicine (5th ed., pp. 16-26). Elsevier Saunders.
Chinoy, E. D., Cuellar, J. A., Huwa, K. E., et al. (2021). Performance of seven consumer sleep-tracking devices compared with polysomnography. Sleep, 44(5), zsaa291.
Cretikos, M. A., Bellomo, R., Hillman, K., Chen, J., Finfer, S., & Flabouris, A. (2008). Respiratory rate: the neglected vital sign. Respiratory Care, 53(6), 1454-1462.
de Zambotti, M., Cellini, N., Goldstone, A., Colrain, I. M., & Baker, F. C. (2019). Wearable sleep technology in clinical and research settings. Sleep Medicine Reviews, 15(4), 461-482.
Hirshkowitz, M., Whiton, K., Albert, S. M., et al. (2015). National Sleep Foundation’s sleep time duration recommendations. Sleep Health, 1(1), 40-43.
Hobson, J. A., & Pace-Schott, E. F. (2002). The cognitive neuroscience of sleep. Nature Reviews Neuroscience, 3(9), 679-693.
Irish, L. A., Kline, C. E., Gunn, H. E., Buysse, D. J., & Hall, M. H. (2015). The role of sleep hygiene in promoting public health. Journal of Behavioral Medicine, 38(5), 771-779.
Kaplan, K. A., & Harvey, A. G. (2009). Hypersomnia across mood disorders: A review and synthesis. Sleep Medicine Reviews, 13(4), 275-285.
Kapur, V. K., Auckley, D. H., Chowdhuri, S., et al. (2017). Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea. Journal of Clinical Sleep Medicine, 13(3), 479-504.
Luks, A. M., & Swenson, E. R. (2011). Pulse oximetry at high altitude. High Altitude Medicine & Biology, 12(2), 109-119.
Mander, B. A., Winer, J. R., & Walker, M. P. (2017). Sleep and human aging. Neuron, 94(1), 19-36.
Ohayon, M. M., Carskadon, M. A., Guilleminault, C., & Vitiello, M. V. (2004). Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals. Sleep, 27(7), 1255-1273.
Ohayon, M., Wickwire, E. M., Hirshkowitz, M., et al. (2017). National Sleep Foundation’s sleep quality recommendations. Sleep Health, 3(1), 6-19.
Plews, D. J., Laursen, P. B., Stanley, J., Kilding, A. E., & Buchheit, M. (2013). Training adaptation and heart rate variability in elite endurance athletes. European Journal of Applied Physiology, 113(4), 1033-1042.
Rasch, B., & Born, J. (2013). About sleep’s role in memory. Physiological Reviews, 93(2), 681-766.
Roenneberg, T., Pilz, L. K., Zerbini, G., & Winnebeck, E. C. (2019). Chronotype and social jetlag. Current Biology, 29(24), R1145-R1154.
Shaffer, F., & Ginsberg, J. P. (2017). An overview of heart rate variability metrics and norms. Frontiers in Public Health, 5, 258.
Siegel, J. M. (2001). The REM sleep-memory consolidation hypothesis. Science, 294(5544), 1058-1063.
Stepanski, E. J., & Wyatt, J. K. (2003). Use of sleep hygiene in the treatment of insomnia. Sleep Medicine Reviews, 7(3), 215-225.
Medically reviewed by Dr. Rishav Das, M.B.B.S.
Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Review Authority: Clinical validation translation for consumer wellness devices. See About page for complete scope boundaries and credentials.
Last Medical Review: February 7, 2026
This page provides educational information about sleep metrics tracked by consumer devices. It is not medical advice and does not replace professional healthcare evaluation. Consult a healthcare provider for diagnosis or treatment of sleep disorders.
