Body Composition Metrics Explained: How to Accurately Track Body Fat, Muscle Mass & Health Markers at Home
Interpret body fat, muscle mass, and visceral fat from smart scales. Understand body composition metrics in healthy ranges and how to track long-term compositional trends.
Written by: Dr. Rishav Das, M.B.B.S. — Wellness Device Data Analyst | Consumer Device Accuracy Specialist
Medically reviewed by Dr. Rishav Das, M.B.B.S. | Last updated: February 18, 2026 | Content review schedule
⚠️ CONTENT SCOPE: This article explains body composition measurement science and device accuracy. It does not provide medical diagnosis or clinical advice. See our editorial scope and limitations for details.
This page is intended for general educational purposes only. The information provided here does not constitute medical advice, diagnosis, or treatment. Body composition metrics and reference ranges are informational references — not clinical thresholds or diagnostic criteria. Individual health status should be evaluated by a qualified healthcare provider. Consult your physician or a licensed health professional before making any health-related decisions based on body composition data.
Why Your Scale Is Misleading You
If you’ve experienced any of these frustrations, you’re not alone:
- “I’m eating well and exercising, but the scale won’t budge” — You may be losing fat and gaining muscle simultaneously, but scale weight can’t show this.
- “My weight is up 3 pounds overnight — am I doing something wrong?” — Water retention from sodium, exercise, or hormonal shifts causes temporary fluctuations that have nothing to do with fat gain.
- “My BMI says I’m overweight, but I feel healthy and fit” — BMI cannot distinguish between muscle mass and fat mass, leading to misleading classifications for many individuals. BMI standards vary significantly across ethnic populations , comprehensive critical analysis of BMI as a health metric
- “I can’t tell if my diet is actually working” — Scale weight alone cannot confirm whether you’re losing fat, muscle, or water.
These frustrations exist because scale weight tells an incomplete story. Body composition metrics reveal what’s actually happening inside your body — allowing you to track meaningful progress the scale cannot show.
A single number on a scale reflects total body weight — the combined mass of muscle, fat, bone, water, and organ tissue. It cannot tell you if you’re losing fat or muscle, gaining bone density or visceral fat, or simply retaining water from last night’s meal.
This distinction matters because two people with identical scale weights can have vastly different health profiles, fitness levels, and metabolic risk factors. Body composition tracking reveals what the scale cannot show — allowing you to make informed decisions about your health, training, and nutrition based on what’s actually changing in your body.
For information on how these metrics are measured by specific devices, see our Body Composition Overview and Device Guide pages.
Body Composition Metrics at a Glance
| Metric | What It Tells You | Why It Matters | Healthy Range (see sources) (age- and sex-specific healthy body fat ranges) (World Health Organization BMI classification standards) |
|---|---|---|---|
| Body Fat % | Proportion of total mass that is fat tissue | Direct indicator of metabolic health and disease risk | 21–33% (females 40–59) 18–24% (males 40–59) |
| Muscle Mass % | Amount of skeletal muscle tissue | Strength, metabolism, aging resistance research on muscle loss as a key aging biomarker | 25–30% (females) 30–35% (males) |
| Visceral Fat | Deep abdominal fat surrounding organs | Heart disease and diabetes risk research linking visceral fat to cardiovascular disease risk | Level 1–9 (device-dependent scale) |
| BMI | Weight-to-height ratio | Population screening metric (limited individual value) research demonstrates BMI’s diagnostic limitations | 18.5–24.9 |
| Bone Mass | Estimated skeletal mineral content | Fracture risk, bone health indicator clinical evidence on bone mass decline in aging populations | 2.4–3.1 kg (varies by body size) |
| Body Water % | Percentage of total mass that is water | Hydration status, fluid balance | 45–60% (varies by age/gender) |
CDC guidelines on adult BMI interpretation
💾 Save this table as a quick reference for interpreting your measurements
- Body Composition Metrics Explained: How to Accurately Track Body Fat, Muscle Mass & Health Markers at Home
- Why Your Scale Is Misleading You
- Body Composition Metrics at a Glance
- Why Scale Weight Doesn't Tell the Full Story (And What to Track Instead)
- Body Fat Percentage
- BMI (Body Mass Index)
- Muscle Mass
- Visceral Fat
- Bone Mass and Body Water
- BIA Technology and Accuracy
- Using Trends vs Single Measurements
- How to Start Tracking Your Body Composition
- When to Consult a Healthcare Provider
- Frequently Asked Questions
- Common Concerns About Body Composition Tracking
- "This seems too complicated for me to track consistently."
- "I'm worried my starting numbers will be discouraging."
- "Smart scales aren't accurate enough to be worth the effort."
- "What if I have a pacemaker or other medical device?"
- "I don't want my data shared or tracked by a company."
- "What if I get obsessed with the numbers and it becomes unhealthy?"
- References
Why Scale Weight Doesn’t Tell the Full Story (And What to Track Instead)

| Factor | What Scale Weight Reflects | What It Misses |
| Muscle mass | Included in total weight | Cannot distinguish muscle from fat |
| Fat mass | Included in total weight | Cannot indicate fat distribution or type |
| Body water | Included in total weight | Daily fluctuations (1–3 kg) obscure trends |
| Bone density | Included in total weight | Cannot identify bone mass changes |
| Visceral fat | Included in total weight | Cannot distinguish location of fat deposits |
| Organ tissue | Included in total weight | Not clinically relevant for tracking purposes |
Research published in journals including the American Journal of Clinical Nutrition has indicated that individuals with identical body weights may differ substantially in body fat percentage, lean mass, and metabolic risk profiles. Scale weight alone does not capture these differences.¹
Body-Weight Variability Factors (Normal Daily Fluctuation)
- Recent physical activity and glycogen storage
- Hydration status (primary driver of short-term weight change)
- Gastrointestinal content
- Time of day and recent food intake
- Hormonal cycling (particularly in females)
Body Fat Percentage
Body fat percentage (BFP) represents the proportion of total body mass that is composed of adipose (fat) tissue, expressed as a percentage. Unlike scale weight, it contextualizes fat mass relative to overall body size.
Healthy Body Fat Ranges by Gender and Age

Reference ranges below are drawn from the American Council on Exercise (ACE) classification system and supplemented by age-adjusted context from published literature. These are reference ranges — not diagnostic thresholds. Individual health status should be assessed by a qualified healthcare provider.
Body Fat Percentage Classification — Adult Females
| Classification | Ages 20–39 | Ages 40–59 | Ages 60–79 |
| Essential Fat | 10–13% | 10–13% | 10–13% |
| Athlete | 14–20% | 14–20% | 14–20% |
| Fitness | 21–24% | 21–24% | 21–24% |
| Acceptable | 25–31% | 25–31% | 25–31% |
| Obesity (research threshold) | ≥32% | ≥32% | ≥32% |
Body Fat Percentage Classification — Adult Males
| Classification | Ages 20–39 | Ages 40–59 | Ages 60–79 |
| Essential Fat | 2–5% | 2–5% | 2–5% |
| Athlete | 6–13% | 6–13% | 6–13% |
| Fitness | 14–17% | 14–17% | 14–17% |
| Acceptable | 18–24% | 18–24% | 18–24% |
| Obesity (research threshold) | ≥25% | ≥25% | ≥25% |
Source: American Council on Exercise; Gallagher et al. (2000), American Journal of Clinical Nutrition.²
💡 COMMON MYTH: “Muscle weighs more than fat”
REALITY: Muscle and fat weigh the same per unit of mass (1 pound = 1 pound). Muscle is denser than fat, meaning it occupies less volume. This is why you can lose inches while the scale stays the same — you’re replacing lower-density fat with higher-density muscle. This is progress, not stagnation.
Important caveats:
- These ranges are educational reference points — clinical interpretation should involve a licensed healthcare provider.
- Age-related increases in body fat percentage are documented in the literature and considered physiologically normal to a degree.
- Ethnicity-specific differences in body composition and associated health risk have been identified in research; universal thresholds may not apply equally across all populations.³
Which Metrics Matter Most for Your Goals?
Different health and fitness objectives require focus on different body composition metrics:
For Weight Loss Goals:
- Priority metrics: Body fat percentage, visceral fat level, muscle mass percentage
- Why these matter: Ensures you’re losing fat rather than muscle; tracks metabolic health improvements
- Success indicator: Body fat percentage decreases while muscle mass maintains or increases
For Muscle Building and Strength Training:
- Priority metrics: Skeletal muscle mass percentage, total body weight, body fat percentage
- Why these matter: Confirms muscle gain is outpacing fat accumulation; validates training effectiveness (peer-reviewed protocols for monitoring muscle hypertrophy)
- Success indicator: Muscle mass increases faster than body fat increases
For General Health Maintenance:
- Priority metrics: Visceral fat level, body water percentage, BMI (as one data point among several)
- Why these matter: Tracks metabolic disease risk factors and overall physiological balance (research on muscle loss as a key aging biomarker)
- Success indicator: All metrics remain within healthy reference ranges over time
For Athletes and Performance Training:
- Success indicator: Body fat trends align with competition cycle; muscle mass maintains during training peaks
- Priority metrics: Body fat percentage, skeletal muscle mass, body water balance
- Why these matter: Optimizes power-to-weight ratio; prevents overtraining through hydration monitoring (body composition assessment standards in competitive sport)
Essential vs. Storage Fat
| Fat Type | Definition | Primary Location | Physiological Role |
| Essential Fat | Minimum fat required for normal physiological function | Brain, nerves, bone marrow, organs, cell membranes | Hormone regulation, neurological function, organ protection |
| Storage Fat | Accumulated fat beyond essential levels | Subcutaneous (under skin), visceral (around organs) | Energy reserve; excess accumulation associated with health risk |
| Subcutaneous Fat | Fat stored beneath the skin surface | Thighs, abdomen, arms, hips | Insulation, energy storage; less metabolically active than visceral fat |
| Visceral Fat | Fat stored within the abdominal cavity | Surrounding liver, pancreas, intestines | Associated with metabolic risk at elevated levels (see Visceral Fat section) |
Essential fat in females is generally higher than in males due to fat associated with reproductive physiology.⁴
How Accurately Can Scales Measure Body Fat Percentage?
Consumer-grade smart scales primarily use Bioelectrical Impedance Analysis (BIA) to estimate body fat percentage. Accuracy considerations are outlined below.
| Method | Estimated Accuracy vs. DEXA | Notes |
| DEXA Scan (reference standard) | Reference standard | Gold standard in research settings; not widely available for routine use |
| Hydrostatic Weighing | ±1–3% | High accuracy; requires specialized equipment |
| Air Displacement Plethysmography (Bod Pod) | ±1–3% | High accuracy; specialized equipment |
| 4-site Skinfold Caliper | ±3–5% | Technician-dependent |
| BIA — research grade | ±3–5% | Varies with device quality and protocol |
| BIA — consumer smart scale | ±3–8% or greater | Highly sensitive to hydration, posture, and protocol |
| Handheld BIA devices | ±4–8% | Measurement limited to upper body segment |
Sources: Malavolti et al. (2003); Kyle et al. (2004), Clinical Nutrition.⁵
Critical interpretive note: Consumer BIA scales are generally considered more useful for tracking directional trends over time than for providing precise absolute values. See the BIA Accuracy section below for full discussion.
BMI (Body Mass Index)
BMI is a numerical index calculated from height and weight, used historically and in current public health contexts as a population-level screening tool for weight categories that may be associated with health risk. It is not a direct measure of body composition.
How BMI Is Calculated
| Unit System | Formula |
| Metric | BMI = weight (kg) ÷ height (m)² |
| Imperial | BMI = [weight (lbs) ÷ height (inches)²] × 703 |
Standard WHO/CDC BMI Classification — Adults
| BMI Range | Classification |
| Below 18.5 | Underweight |
| 18.5 – 24.9 | Normal weight |
| 25.0 – 29.9 | Overweight |
| 30.0 – 34.9 | Obesity Class I |
| 35.0 – 39.9 | Obesity Class II |
| 40.0 and above | Obesity Class III |
Source: World Health Organization; Centers for Disease Control and Prevention.⁶
Limitations of BMI
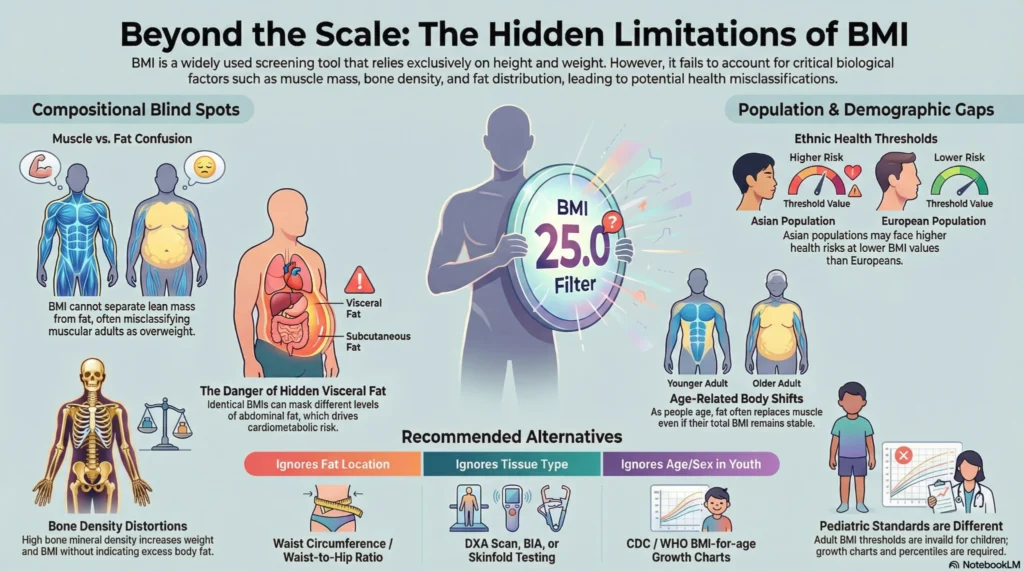
BMI has documented limitations that are widely acknowledged in clinical and research literature.
| Limitation | Explanation | Evidence |
| Does not measure fat vs. muscle | A highly muscular individual may register as ‘overweight’ or ‘obese’ despite low body fat percentage | Established in literature; commonly cited in sports medicine contexts |
| Does not account for fat distribution | Two individuals with the same BMI may have markedly different visceral fat levels and associated risk profiles | Supported by epidemiological research |
| Population-specific inaccuracies | Optimal BMI thresholds may differ by ethnicity; some Asian populations show elevated metabolic risk at lower BMI values | WHO Expert Consultation Report (2004) |
| Does not distinguish age-related changes | Body fat percentage tends to increase with age independent of weight change; BMI does not capture this | Gallagher et al. (2000) |
| Not applicable to children with adult thresholds | Pediatric BMI requires age- and sex-specific percentiles | CDC growth chart protocols |
| Ignores bone density | High bone mineral density may elevate BMI without associated health risk | Documented in literature |
When BMI Is Useful
Despite its limitations, BMI retains practical utility in defined contexts.
| Context | Why BMI May Be Appropriate |
| Large-scale population screening | Simple, low-cost, and reproducible across populations |
| Epidemiological research | Consistent metric enabling cross-study comparisons |
| Initial clinical triage | May prompt further assessment in primary care settings |
| Longitudinal tracking in individuals | Can indicate directional weight change when used consistently |
| Insurance and institutional protocols | Widely adopted as administrative reference metric |
Recommended interpretation approach:
BMI is most informative when used alongside other metrics such as waist circumference, body fat percentage, and clinical assessment. It is not recommended as a standalone indicator of individual health status by many current clinical guidelines.⁸
Muscle Mass
Muscle mass refers to the total weight or percentage of skeletal muscle tissue in the body. It is a primary component of lean body mass and is associated with metabolic rate, functional capacity, and physical performance.
Skeletal Muscle Percentage
Skeletal muscle is the voluntary, striated muscle tissue attached to the skeleton. It is the component most directly influenced by resistance training and protein intake.
General Reference Ranges — Skeletal Muscle Percentage of Body Weight
| Population | Typical Range | Notes |
| Adult males (general) | 38–54% | Higher ranges associated with athletic training status |
| Adult females (general) | 28–39% | Physiologically lower than males due to hormonal differences |
| Older adults (60+) | Progressively lower | Age-related muscle loss (sarcopenia) is well-documented in literature |
| Trained athletes | May exceed upper ranges | Varies by sport and training modality |
Note: Reference ranges vary by measurement method and population studied. Consumer BIA devices provide estimates, not clinical measurements.
Factors associated with skeletal muscle mass:
- Physical activity level and movement patterns
- Resistance training stimulus (primary modifiable factor)
- Dietary protein intake (quantity and quality)
- Age (muscle mass tends to decline with age after approximately the third decade)⁹
- Sex (males generally carry higher skeletal muscle mass due to androgenic hormonal environment)
- Hormonal status (testosterone, growth hormone, estrogen all influence muscle protein synthesis)
Tracking Muscle Gain Progress
Practical considerations for tracking muscle mass over time:
| Consideration | Detail |
| Rate of muscle gain | Evidence suggests natural muscle gain occurs slowly — approximately 0.5–2 lbs (0.2–0.9 kg) per month under optimal conditions for most individuals¹⁰ |
| Minimum tracking interval | Weekly or bi-weekly measurements are more informative than daily; daily variation from hydration and glycogen is significant |
| Consistent conditions | Measurements taken under identical conditions (same time, hydration status, fasted state) improve comparability |
| Simultaneous fat loss | Body recomposition (muscle gain + fat loss simultaneously) can result in stable scale weight despite meaningful compositional change — a key reason scale weight alone is insufficient |
| Progress markers beyond BIA | Strength metrics, circumference measurements, and performance benchmarks may complement BIA-estimated muscle data |
Visceral Fat
What Visceral Fat Is
Visceral fat (also referred to as intra-abdominal fat) is adipose tissue stored within the abdominal cavity, surrounding internal organs including the liver, pancreas, stomach, and intestines. It is distinct from subcutaneous fat, which is stored beneath the skin.
| Feature | Visceral Fat | Subcutaneous Fat |
| Location | Intra-abdominal (surrounding organs) | Beneath the skin surface |
| Metabolic activity | More metabolically active; releases inflammatory cytokines and free fatty acids | Less metabolically active |
| Visibility | Not externally visible; cannot be pinched | Often visible and palpable |
| Health association | More strongly associated with cardiometabolic risk | Associated with risk at very high levels; less so than visceral fat |
| Measurement | Estimated via BIA, CT scan, MRI | Measurable via skinfold caliper or imaging |
Health Risks Associated with Elevated Visceral Fat
Research has associated elevated visceral fat with increased risk for several health conditions. The following reflects published evidence and is not intended as a diagnostic tool.
| Associated Health Condition | Nature of Association | Evidence Level |
| Type 2 diabetes | Visceral fat contributes to insulin resistance via release of free fatty acids and adipokines | Well-established; multiple meta-analyses |
| Cardiovascular disease | Associated with dyslipidemia, elevated triglycerides, reduced HDL | Well-established¹¹ |
| Metabolic syndrome | Visceral adiposity is a central feature of metabolic syndrome criteria | Established in clinical literature |
| Non-alcoholic fatty liver disease (NAFLD) | Visceral fat is closely associated with hepatic fat accumulation | Emerging to well-established |
| Elevated systemic inflammation | Visceral adipose tissue produces pro-inflammatory cytokines including TNF-α and IL-6 | Established in research literature¹² |
| Certain cancers | Epidemiological associations have been reported; mechanisms under investigation | Emerging evidence; area of active research |
Important framing:
Association is not causation. The relationships above reflect population-level statistical associations documented in research literature, not guaranteed individual outcomes. Clinical assessment by a qualified healthcare provider is necessary for individual health evaluation.
Healthy Ranges for Visceral Fat
Visceral fat measurement varies significantly by the method used. Consumer BIA scales typically report visceral fat on a proprietary numerical scale (commonly 1–59 or similar) rather than a direct tissue measurement.
General Reference Framework — Visceral Fat Ratings (Consumer BIA Scale)
| Rating Range (Typical Consumer Scale) | General Classification |
| 1–9 | Generally considered within healthy reference range |
| 10–14 | Elevated; may warrant attention and lifestyle review |
| 15 and above | High; clinical consultation is advisable |
Note: Scales differ in their visceral fat rating systems. Consult the documentation for your specific device. These figures should not be used as a substitute for clinical assessment.
✓ KEY INSIGHT: You can reduce visceral fat without significant weight loss
Studies show that visceral fat responds more readily to dietary changes and aerobic exercise than subcutaneous fat. Many individuals see visceral fat level reductions of 1–2 levels within 6–8 weeks through moderate dietary improvements and increased physical activity — even when total scale weight remains stable. (see our peer-reviewed research methodology for source evaluation standards)
research linking visceral fat to cardiovascular disease risk
research explaining visceral fat’s unique metabolic effects
Bone Mass and Body Water
These metrics are reported by many consumer BIA devices alongside body fat and muscle data. They are secondary metrics for most tracking purposes but provide useful contextual information about overall body composition.
Bone Mass
| Item | Detail |
| Definition | Estimated weight of mineral content in bones; distinct from bone density (BMD), which requires DEXA measurement |
| Typical range — adult females | Approximately 2.0–4.0 kg (varies with body size and training history) |
| Typical range — adult males | Approximately 2.7–4.7 kg (varies with body size and training history) |
| What affects it | Weight-bearing physical activity, dietary calcium and vitamin D intake, hormonal status, age, genetic factors |
| Tracking utility | Consumer BIA bone mass estimates are rough approximations; meaningful bone health assessment requires DEXA scan |
| Age-related change | Bone mineral density tends to decline with age, particularly following menopause in females; a well-documented pattern in clinical literature¹³ |
Body Water
| Item | Detail |
| Definition | Total body water (TBW) expressed as a percentage of total body weight; includes intracellular and extracellular fluid |
| General reference range — females | Approximately 45–60% of body weight |
| General reference range — males | Approximately 50–65% of body weight |
| What affects it | Hydration status (primary short-term driver), age, body fat percentage, physical activity, alcohol intake, diuretic use, illness |
| Clinical significance | Hydration directly impacts BIA readings for all metrics; adequate hydration is important for measurement consistency |
| Why it varies | Muscle tissue contains more water than fat tissue; individuals with higher muscle mass and lower body fat tend to show higher TBW percentages |
BIA Technology and Accuracy
Bioelectrical Impedance Analysis (BIA) works by passing a low-level electrical current through the body and measuring the resistance (impedance) of that current as it travels through different tissue types. Fat tissue, muscle tissue, bone, and water conduct electricity at different rates, allowing the device to estimate body composition.
How Consumer BIA Scales Estimate Composition
| Step | Process |
| 1 | User stands on scale electrode pads (foot-to-foot BIA) |
| 2 | Low-level current travels from foot to foot through body |
| 3 | Device measures electrical resistance (impedance) |
| 4 | Impedance values are entered into a proprietary predictive equation |
| 5 | Equation uses impedance + user-entered data (age, height, sex) to estimate composition |
| 6 | Results are output as estimated percentages for fat, muscle, water, and bone mass |
Key limitation: The accuracy of the output is bounded by the accuracy of both the impedance measurement and the predictive equation used. Equations are often developed and validated on specific populations and may be less accurate when applied to individuals outside those populations.
Clinical Nutrition journal’s comprehensive BIA review
Factors That Affect BIA Readings
| Factor | Direction of Effect | Notes |
| Dehydration | Overestimates body fat | Reduced water = higher impedance = algorithm interprets more fat |
| Over-hydration | Underestimates body fat | Excess fluid reduces impedance |
| Recent exercise | Variable; may underestimate body fat short-term | Increased blood flow and fluid shifts affect impedance |
| Recent food/drink intake | May alter readings | Gastrointestinal content affects weight and fluid distribution |
| Time of day | Readings vary throughout the day | Hydration and fluid distribution shift diurnally |
| Skin temperature | Cold skin increases impedance | May affect accuracy in cold environments |
| Menstrual cycle phase | Fluid retention alters readings | Most pronounced in luteal phase |
| Alcohol consumption | Dehydrating effect alters readings | Even prior-day alcohol may affect results |
| Medications | Diuretics and other medications affect fluid balance | Consult healthcare provider regarding medication effects on readings |
| Foot calluses / dry skin | May affect electrode contact | More common with foot-to-foot BIA scales |
⚠️ CRITICAL CONTEXT: Daily fluctuations of 2–5 pounds are normal
Day-to-day scale changes primarily reflect water retention, not fat gain or loss. Factors that cause temporary water weight fluctuation include:
- Sodium intake (1 gram of sodium can retain up to 400ml of water)
- Carbohydrate intake (each gram of stored glycogen binds 3–4 grams of water)
- Exercise-induced inflammation (muscle repair requires temporary fluid retention)
- Menstrual cycle hormonal shifts
Action: Ignore daily changes. Track 7-day averages or weekly measurements instead.
Consistency Tips for Tracking
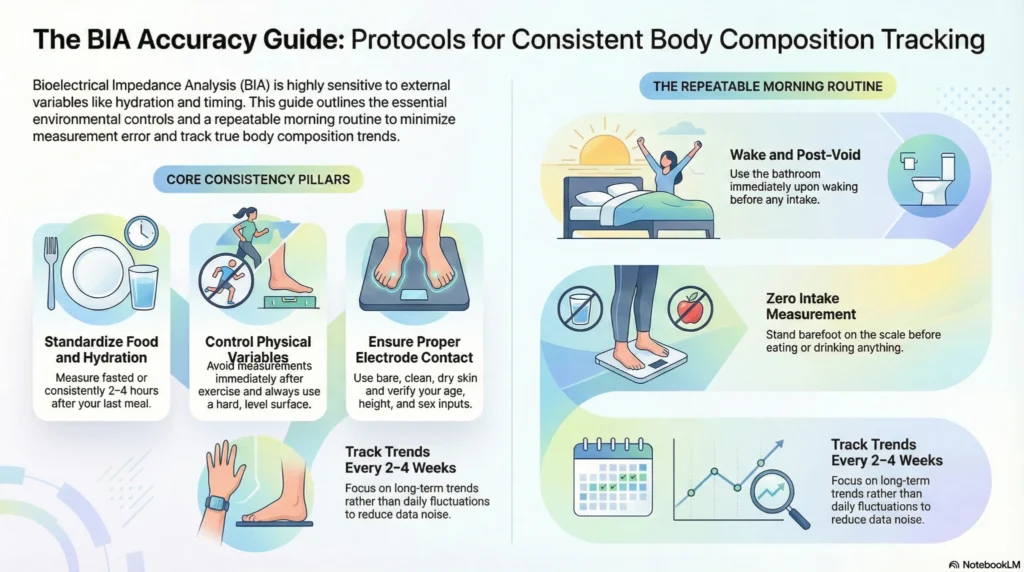
Because BIA readings are sensitive to multiple physiological variables, consistency of conditions is the most important factor for improving the comparability of measurements over time.
| Protocol Element | Recommended Approach |
| Time of day | Same time each measurement; morning (post-void, pre-food/drink) is commonly recommended |
| Hydration | Standardize to the same pre-measurement water intake protocol each time, rather than attempting to assess hydration level |
| Food and drink | Measure fasted, or consistently at the same interval post-meal |
| Exercise | Avoid measuring immediately post-exercise; allow several hours |
| Frequency | Weekly or bi-weekly rather than daily; reduces noise from daily variation |
| Device position | Same surface each time; uneven or soft surfaces may affect readings |
| Foot contact | Bare feet; clean and dry electrode pads |
| User profile settings | Verify that age, height, and sex settings are correct and current |
Using Trends vs Single Measurements
A central principle in body composition tracking — supported by the limitations of consumer BIA technology — is that no single measurement should be interpreted in isolation. Patterns over time are substantially more informative than individual data points.
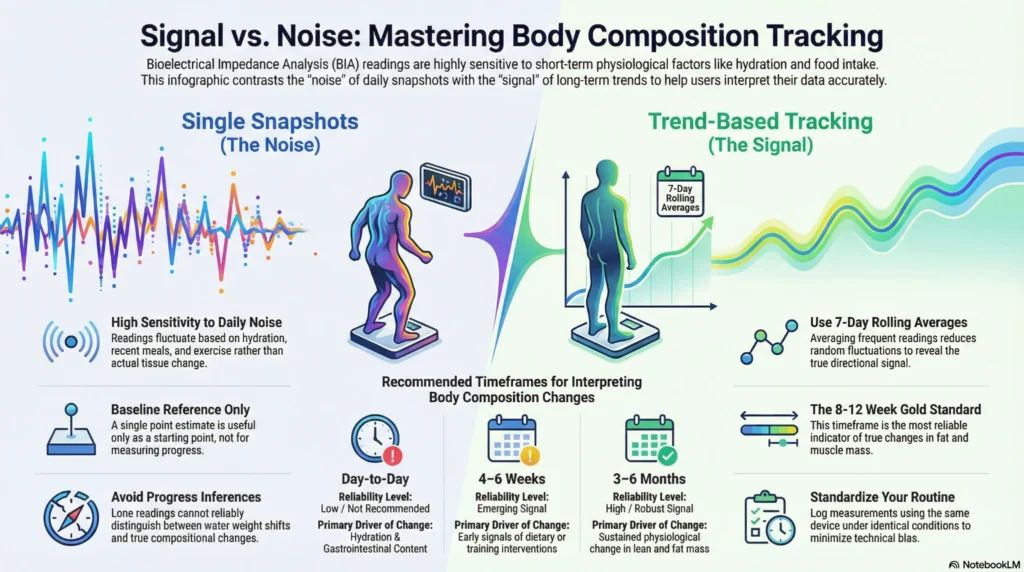
| Approach | Single Measurement | Trend-Based Tracking |
| What it shows | A snapshot at one moment in time | Directional change over weeks or months |
| Sensitivity to noise | High; daily variability can be ±1–3% for some metrics | Reduced; random variation averages out over time |
| Practical utility | Limited for decision-making | More actionable; reflects genuine physiological change |
| Recommended use | Baseline reference only | Primary tracking method |
Recommended Trend Interpretation Framework
| Timeframe | What May Be Interpretable |
| Day-to-day | Not recommended for interpretation; primarily reflects hydration and GI content |
| Week-to-week | Early directional signals; limited reliability |
| 4–6 weeks | Meaningful trends may begin to emerge for body fat and muscle metrics |
| 8–12 weeks | More reliable indicator of genuine compositional change |
| 3–6 months | Strong signal for long-term tracking; sufficient data to identify patterns |
Practical tracking recommendations:
- Consider tracking non-scale markers alongside BIA metrics (strength performance, clothing fit, energy levels)
- Record measurements in a consistent log (app, spreadsheet, or journal)
- Note relevant contextual factors that may explain outliers (illness, travel, irregular sleep)
- Use moving averages if tracking frequently
How to Start Tracking Your Body Composition
Step 1: Choose Your Measurement Method
Budget-Friendly Option ($30–$60):
- Basic BIA smart scale with body fat percentage and weight
- Best for: Casual tracking, weight loss monitoring, establishing baseline trends
- Limitation: Lower accuracy for absolute values; still useful for tracking changes
Mid-Range Option ($60–$120):
- Advanced smart scale with app synchronization and comprehensive metrics (muscle mass, visceral fat, bone mass, body water) Clinical Nutrition journal’s comprehensive BIA review
- Best for: Detailed tracking, fitness enthusiasts, multi-metric analysis
- Limitation: Estimates still subject to hydration and measurement protocol variations. See our device testing methodology for accuracy assessment standards.
Gold Standard ($75–$150 per session):
- Professional DEXA scan at a medical or fitness facility
- Best for: Clinical-grade accuracy, baseline establishment, validating home device estimates. Clinical-grade accuracy for wellness measurement context
- Limitation: Cost per session; not practical for frequent tracking
Comparison: A single DEXA scan costs as much as a quality smart scale, but the scale provides daily tracking capability for years. Most users benefit from establishing a DEXA baseline, then using a smart scale for ongoing trend monitoring.
Device selection guidance based on measurement science, not commercial relationships. See our editorial independence policy.
Step 2: Establish Your Baseline (Week 1 Protocol)
Accurate tracking begins with consistent measurement conditions:
- Measure at the same time each day — Morning measurements after using the bathroom and before eating/drinking provide the most stable baseline
- Take 3 readings and average them — This accounts for minor device variability
- Record contextual factors — Note sleep quality, recent exercise, menstrual cycle phase, or unusual dietary intake that may affect readings
- Do not judge the starting numbers — Your baseline is data, not a verdict. Progress is measured by directional change over weeks, not by comparison to idealized ranges.
Step 3: Track Trends, Not Daily Fluctuations
Recommended measurement frequency: Weekly or bi-weekly for most goals
Why avoid daily measurement:
- Day-to-day variation of ±1–3% in body fat percentage is normal and reflects hydration, not actual tissue change
- Daily measurements introduce unnecessary noise and can obscure genuine trends
- Weekly measurements reduce measurement burden while capturing meaningful changes
How to interpret trends:
- Focus on 4–6 week patterns — Short-term fluctuations average out; directional trends become visible
- Use 7-day moving averages if tracking more frequently — Smooths daily noise without losing trend data
- Combine with non-scale indicators — Track strength performance, clothing fit, energy levels, and how you feel alongside numerical metrics
How to Know If Your Tracking Is Working
After 4–6 weeks, you should be able to answer “yes” to at least one of these:
✓ Body fat percentage shows a consistent downward trend (for fat loss goals)
✓ Muscle mass percentage shows a consistent upward trend (for muscle building goals)
✓ Visceral fat level has decreased by 1+ level (for metabolic health goals)
✓ Body water percentage has stabilized within a narrow range (indicates consistent measurement protocol)
✓ You can identify patterns between your habits (sleep, nutrition, training) and your metrics
If you cannot answer “yes” to any of these after 6 weeks:
- Check measurement consistency — Are you measuring at the same time under the same conditions?
- Review your tracking variables — Are you also tracking sleep, stress, nutrition, and training intensity?
- Consider professional assessment — A DEXA scan or consultation with a registered dietitian can validate your home measurements and identify measurement protocol issues
If your metrics are moving in the wrong direction:
- Muscle mass decreasing during a fat loss phase → May need more protein or resistance training (peer-reviewed protocols for monitoring muscle hypertrophy)
- Body fat increasing during a muscle building phase → May need to reduce caloric surplus
- Visceral fat increasing → Consult healthcare provider; may indicate metabolic dysfunction
Body composition tracking is a tool for feedback, not judgment. Use the data to adjust your approach, not to criticize yourself.
Action: Download Your Free Tracking Template
[Link to downloadable PDF: “90-Day Body Composition Tracker”]
This template includes:
- Progress milestone markers
- Weekly measurement log with space for all major metrics
- Contextual factor checklist (sleep, hydration, exercise, stress)
- Trend visualization worksheet
When to Consult a Healthcare Provider
This page is intended for educational purposes only. The metrics described here are general reference information and are not intended for use in self-diagnosis, clinical decision-making, or treatment planning.
Consider consulting a qualified healthcare provider if you:
- Have a pacemaker or other implanted electronic device (electrical current contraindication)
- Have a known or suspected medical condition that may affect body composition (e.g., thyroid disorders, diabetes, eating disorders, heart or kidney disease)
- Are taking medications that may affect fluid balance, muscle mass, or metabolic function
- Are experiencing unexplained significant changes in body weight or composition
- Wish to establish personalized healthy range targets based on your individual health history
- Are pregnant or postpartum (BIA devices are not recommended for use during pregnancy)
Frequently Asked Questions
Common Concerns About Body Composition Tracking
“This seems too complicated for me to track consistently.”
You don’t need to track everything at once. Start with just body fat percentage and weight. Most users find that tracking 2–3 metrics weekly takes less than 2 minutes and becomes routine within a few weeks. You can add additional metrics later if they become relevant to your goals.
“I’m worried my starting numbers will be discouraging.”
Your starting point is just data — not a judgment of your worth or effort. What matters is the direction of change over 8–12 weeks, not where you begin. Research shows that most people who track body composition consistently see measurable improvements within 30–45 days, regardless of their starting point.
“Smart scales aren’t accurate enough to be worth the effort.”
Absolute accuracy is not the primary goal for most users. Tracking trends over time is approximately 80% as valuable as clinical-grade testing at a fraction of the cost and effort. A smart scale that consistently overestimates your body fat by 2% will still accurately show when that number decreases by 3% over 6 weeks — which is the information that matters for decision-making.
“What if I have a pacemaker or other medical device?”
BIA scales are contraindicated for individuals with pacemakers, defibrillators, or other implanted electronic devices due to the electrical current used in measurement. Alternative methods include:
- Skinfold caliper measurements (manual, no electrical current)
- DEXA scans (imaging-based, no electrical current)
- Circumference measurements (tape measure tracking of waist, hips, arms, thighs)
Consult your healthcare provider for personalized guidance on safe body composition assessment methods. See our guidance on when clinical consultation is appropriate.
“I don’t want my data shared or tracked by a company.”
Many smart scales offer offline modes or local-only data storage. Review the privacy policy of any device or app before use. You can also track measurements manually in a spreadsheet or journal if you prefer not to use connected features.
“What if I get obsessed with the numbers and it becomes unhealthy?”
If you have a history of disordered eating, obsessive tracking behaviors, or body dysmorphia, consult a healthcare provider or mental health professional before beginning any body composition monitoring routine. For most users, limiting measurements to once weekly and focusing on long-term trends (rather than daily changes) helps maintain a healthy relationship with tracking data.
References
Khosla S, Riggs BL. “Pathophysiology of age-related bone loss and osteoporosis.” Endocrinology and Metabolism Clinics of North America. 2005;34(4):1015–1030.
Romero-Corral A, et al. “Accuracy of body mass index in diagnosing obesity in the adult general population.” International Journal of Obesity. 2008;32(6):959–966.
Gallagher D, et al. “Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index.” American Journal of Clinical Nutrition. 2000;72(3):694–701.
WHO Expert Consultation. “Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies.” The Lancet. 2004;363(9403):157–163.
Ackland TR, et al. “Current status of body composition assessment in sport.” Sports Medicine. 2012;42(3):227–249.
Kyle UG, et al. “Bioelectrical impedance analysis — Part I: Review of principles and methods.” Clinical Nutrition. 2004;23(5):1226–1243.
World Health Organization. BMI Classification. Geneva: WHO; updated 2023. Available at: who.int
Centers for Disease Control and Prevention. About Adult BMI. Atlanta: CDC; updated 2022. Available at: cdc.gov
Nuttall FQ. “Body mass index: obesity, BMI, and health — a critical review.” Nutrition Today. 2015;50(3):117–128.
Volpi E, et al. “Muscle tissue changes with aging.” Current Opinion in Clinical Nutrition & Metabolic Care. 2004;7(4):405–410.
Lemon PW, et al. “Protein requirements and muscle mass/strength changes during intensive training in novice bodybuilders.” Journal of Applied Physiology. 1992;73(2):767–775.
Despres JP, Lemieux I. “Abdominal obesity and metabolic syndrome.” Nature. 2006;444(7121):881–887.
Hotamisligil GS. “Inflammation and metabolic disorders.” Nature. 2006;444(7121):860–867.
Medical Reviewer: Dr. Rishav Das, M.B.B.S. — Wellness Device Data Analyst | Consumer Device Accuracy Specialist, Wearable Wellness Guide.
Last Updated : 18th February, 2026
Scope of review: Device measurement accuracy, clinical validity translation, and safety disclosures. This review does not constitute medical diagnosis or treatment recommendations. Full editorial governance details are available on our About page.
